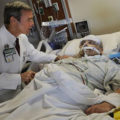
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Do I Stay Positive Whilst My Daughter is Critically Ill in the ICU?
You can check out last week’s question by clicking on the link here.
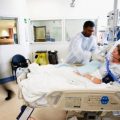
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy service! Tess’s daughter is on a ventilator and her Glasgow Coma Scale (GCS) is 3. Tess is asking why does the ICU team want to do a tracheostomy on her daughter.
Why Does the ICU Team Want to Do a Tracheostomy on My Ventilated Daughter?
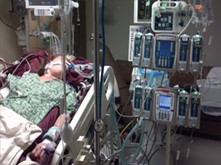
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Patrik: That’s okay. It’s probably either Keppra or phenytoin, one or the other, most likely. So the way I’d like to approach this now is more or less from head to toe, To get a better understanding. You’ve shared a lot already GCS or Glasgow Coma Scale 3, pupils reacting to light but probably not equal, no sedation, only on Panadol. Do you think she’s in pain?
Tess: They say she can’t feel pain, but I don’t believe that because why would they give her paracetamol?
Patrik: I’m not interested in their opinion with this question, I’m interested in your opinion.
Tess: I haven’t actually done any pain tests for 10 seconds or more, so I wouldn’t know. All I’ve done is try to console and communicate with her as best I can.
Patrik Hutzel: Sure. When you look at her, do you think she’s in pain?
Tess: Her face actually is quite calm.
RECOMMENDED:
Patrik Hutzel: Okay.
Tess: I’m not sure, it’s very difficult to tell you.
Patrik Hutzel: Right, do you think that she’s suffering?
Tess: I think that she is actually consciously aware but can’t at the moment express herself.
Patrik Hutzel: Right, do you think that the tube in her mouth is uncomfortable for her?
Tess: I would imagine it would be.
Patrik Hutzel: Right, but she’s not showing signs of discomfort when you look at her?
Tess: Not when I’m present.
Patrik Hutzel: Yeah, okay.
Tess: She was actually dribbling, yeah. She is fighting the ventilator.
Patrik Hutzel: She is, okay.
Tess: Yep, she has been fighting the ventilator. And another point that I thought was a bit curious was that on Friday or the day before, she was dribbling profusely. A frothy dribble from the side of her mouth.
Patrik Hutzel: Right.
Tess: And then the day before yesterday when I saw her, and I noted that in all of the time that I was with her, there was absolutely no suction, necessity to suck from the side of her mouth. Which suggests to me either they’ve dehydrated her to the point where they’re stopping the dribbles or she’s actually swallowing her own saliva.
Patrik Hutzel: Right, okay.
Tess: And I pointed that out and asked, I’ve made that observation and I asked about it and they pooh-poohed it again, they’re pooh-poohing it as not of significance, as not a big deal. But if somebody is profusely salivating, where they have to wipe her up on a relatively routine basis and only the most recent time I saw her, which was a couple of days ago, there’s nothing going on, I don’t understand, it doesn’t equate for me.
Patrik Hutzel: Right. Right, okay. Okay.
Tess: They’ve communicated with her brain and her brain stem’s intact.
Patrik Hutzel: Her brain stem is intact, okay, good. Oh yeah, that’s a very good question, have they ever mentioned to you that she might be brain dead?
Tess: No.
Patrik Hutzel: Good. That’s good, that’s good.
Tess: They’re talking of a perfuse brain injury.
Patrik Hutzel: Yeah, sure.
Tess: I don’t know what perfuse means.
Patrik Hutzel: Sure, have you spoken to a neurologist?
Tess: Yeah, it was yesterday for the first time, and she wasn’t very friendly really. How would I describe it? It’s very difficult when you’re basically communicating with somebody with a mask, so all of the visual cues are basically marred but her attitude was quite reticent and also, they were quite empathic that in a sense, we had to come to terms with the state that Sara’s in and that’s that kind of attitude.
Patrik Hutzel: Right, so she was very negative, was she?
Tess: I would say she was, yeah.
Suggested Links:
Patrik Hutzel: And who’s suggesting the tracheostomy, that’s ICU?
Tess: No, the tracheostomy was… Yeah, the ICU, they wish to put in a tracheostomy and they’ve said, “Because you’re the next of kin, Tess…” The nurse turned to me, he was really on my case and quite forceful, at the Critical Care Unit, he was quite forceful with me, “We’re only prepared to talk to you,” kind of thing.
Patrik Hutzel: Right.
Tess: And I haven’t really have said very much, really as much as I could, I’m just observing how they’re behaving.
Patrik Hutzel: Right. And sorry, I might have asked that question before but when was the first time they mentioned the tracheostomy?
Tess: The other day.
Patrik Hutzel: The other day, okay.
Tess: But no, previously, there was an option. It was a suggestion, a suggestion to a question over the past week.
Patrik Hutzel: Right.
Tess: At some point. Whether it would be Tanya who was overlooking at that time or Rachel. Rachel, who was the last doctor that we saw before she got transferred over back to her present hospital on Sunday of last week.
Patrik Hutzel: Right, okay. And before they mentioned the tracheostomy the other day, did you know anything about tracheostomy or did that come out of the blue?
Tess: It came out of the blue, as far as they’re concerned we were not really informed of it, we weren’t given any intelligence as to the consequences, the benefits or risks. They were doubting whether she needed one prior to that.
Patrik Hutzel: Right, but it’s not that you pushed for a tracheostomy, they did that themselves?
Tess: No, not at all.
Patrik Hutzel: Okay. Okay, that’s good. That’s a good sign. Okay. With her heart condition or with the cardiac arrest, so you mentioned she’s off the norepinephrine or noradrenaline?
Tess: Yeah, both she was on at one point.
Patrik Hutzel: Okay. Is she having an intravenous access, do you know?
Tess: Well, she would have had when she was having the blood transfusions but at the moment, I don’t know because I didn’t get to see her yesterday.
Patrik Hutzel: Right.
Tess: I knew that there was only one… You know where they basically have a little screen in the ICU where you can tell that something’s being input? There was only one and I’m not quite sure what because I couldn’t see the writing on it but I assume she’s still being ventilated. I don’t know whether they’re attempting to move her off but I can well imagine that given what her situation is now, if she was closed down effectively in communication, she’ll find herself in a very worrisome position, she may well be confused. It’s quite evident she’d be confused but if they’re actually giving a far worse prognosis, it doesn’t make sense that they would do an MRI (magnetic resonance imaging). Maybe they’re trying to find other things and establish other things, pretext.
Patrik Hutzel: Is this the first MRI in three weeks since admission?
Tess: We don’t know, we don’t know.
Patrik Hutzel: Right.
Tess: They already said they did one at her previous hospital. Yeah, they would have had to ask us back then but we weren’t asked.
Recommended:
Patrik Hutzel: Right, okay. I would be surprised if it was the first MRI, I would be surprised. Okay. Does she have a fever?
Tess: No, she was 37.2 about five days ago but as of a couple of days ago when I saw her going back, she was basically all right in her temperature, I felt her forehead and everything.
Patrik Hutzel: Yeah, okay.
Tess: 36 something.
Patrik Hutzel: Right, and with the pneumonia, that’s been cleared now or is she still on antibiotics?
Tess: She’s completed a round of antibiotics. They did blitzkrieg on her first time round and did three, they didn’t know what they were dealing with. And then they’ve tried to hone it down to doing one, one antibiotic which I don’t know the name of.
Patrik Hutzel: Right, okay. Is she coughing?
Tess: No, but she was initially. The weird thing is that they said that she could have potentially had food particles going into her trachea, into her esophagus, yeah?
Patrik Hutzel: Right.
Tess: In the sense of going into the lung cavity, and that indeed may have been the major clue as to why she developed an infection, on top of the fact that she was underweight. But she’s not been around anybody other than ourselves and so it didn’t make logical sense. And I said it was most probably an opportunistic bacteria that got the better of her because she was simply in an underweight state. And also, she’d been furloughed and then it had all come to an end, so she would have had internal sadness about that and stress because of being let off her work and all that as of October the 29th, that would have been a blow to her anyway.
Tess: And all of the uncertainty revolving around that and the fact that she hadn’t really been getting out because she was having gait issues at that time, non-confidence in walking, even in the house. Although she would readily go to the bathroom of her own accord and walk around the house, except for the last four days. But she would cough very slightly, almost like a little bit of regurgitation coughing upon eating and swallowing, so it’s a good possibility that they detected something that may have actually caused the problem in the first place, which was an introduction of food particles into the lung cavity.
Patrik: Yeah. Yeah, okay. So on the ventilation side, do you know what ventilation settings she’s on?
Tess: Well, the last time I saw her, I was told by the nurse that she was on about 30.
Patrik: Sorry, you’re dropping out a little bit.
Tess: 30%. Sorry, 30%. Did you catch that?
Patrik: Yes, 30%. That doesn’t mean anything. Do you think you could take a picture when you go back there?
Tess: No, I can’t, I can’t photograph apparently or anything like that.
Patrik: Look, I’ll leave that to you. I’ll leave that to you.
Tess: Okay.
Patrik: But it would certainly be helpful.
Tess: Okay. What, a photograph of the whole setup?
Patrik: Look, if you can, it would be great, that gives me so much information.
Tess: Okay.
Patrik: It gives me so much information.
Tess: Well, I will try.
Patrik: I know, I know you will try and I know they will tell you what they think you can and you can’t do, in a situation like that I would never ask for permission.
Tess: Okay.
Patrik: Who’s going to stop you to take pictures of your daughter?
Tess: Yeah, right.
Suggested Links:
Patrik: That’s the way I look at it. Okay. So do you know if they’re doing arterial blood gases?
Tess: I don’t know, I’m not quite sure of that.
Patrik Hutzel: Getting quieter and quieter, I can barely hear you anymore, Tess.
Tess: But they did mention an ABG test.
Patrik Hutzel: Yep, ABG.
Tess: Yeah, upon entry to the hospital on the day of her transfer of recent times and they were doing a whole procedure apparently in the ward which prevented me from seeing her, as I mentioned previously.
Patrik Hutzel: Right.
Tess: Obviously, probably an intake of another patient, I don’t know.
Patrik Hutzel: Right, right. Because ventilator settings and the blood gas would give me very good information about what she’s up to from a ventilation point of view.
Tess: Okay. And did you say blood settings?
Patrik Hutzel: No, no, arterial blood gas.
Tess: Okay.
Patrik Hutzel: I’ll send it to you, how it’s spelled.
Tess: Okay.
Patrik Hutzel: Okay, so we talked about feeds, she’s absorbing, she’s getting 40 mls an hour, so we’ve gone through that. Kidneys are working as far as you’re aware?
Tess: Yes, they’re all right, they basically didn’t say… Only this Dan doctor said that potentially… They’re trying to reason why it could have happened and they think… They basically mentioned the possibility that she was a diabetic anyway.
Patrik Hutzel: Right, okay, okay. So there’s no issue there. Okay, that’s good.
Tess: I don’t think there is, myself.
Patrik Hutzel: That’s good, that’s good. So there’s a couple of questions that are remaining, one is, is there a DNR (Do Not Resuscitate)? I would not trust them not to issue a DNR. Given that they’re moving towards a tracheostomy, I would suggest there isn’t one but I do believe it’s a question you should be asking. How do you get updates? How does that happen?
Tess: Very sporadically and I wasn’t expecting the update from the specialist yesterday, I think that they basically jumped on the opportunity because they were preventing me from seeing her and I just wanted to find out from somebody. They could have easily called through potentially from the reception and found out that she was all right but it happened the way it did.
Patrik Hutzel: Right, okay. And have there been any meetings?
Tess: I didn’t catch that. Sorry, Patrik, what did you say?
Patrik Hutzel: I said has there been any meetings?
Tess: Meetings with whom? With them?
Patrik Hutzel: Yeah, with the doctors.
Tess: Only yesterday and previously, yeah, there was a meeting with Dan, the doctor, on Sunday.
Patrik Hutzel: Okay.
Recommended:
Tess: With another nurse, Tam.
Patrik Hutzel: Right.
Tess: They won’t see me today because they want me to grant my permission in writing to let the tracheostomy to go ahead.
Patrik Hutzel: I think given that her Glasgow Coma Scale is 3 and given that it’s been 20 days, I think it’s a good idea to do a tracheostomy.
RECOMMENDED:
Tess: Okay.
Patrik Hutzel: I think it’s a good idea.
Tess: My instinct is it’s the right thing to do too.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!