Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Can They Safely Wean My Wife Off The Ventilator In LTAC?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Mon, as part of my 1:1 consulting and advocacy service! Max’s mother is in ICU with a breathing tube and Max is asking if it is legal for the ICU team to decide not to resuscitate his mom without their consent.
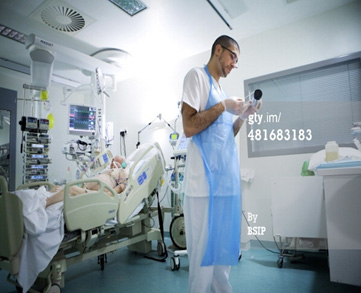
Is It Legal for the ICU Team To Decide Not To Resuscitate My Mom Without Our Consent?
Patrik: I can hear you fine. Thank you. I know it’s very late for you.
Max: It’s totally cool. Don’t even worry I’ve been up for the last couple of days, you know it’s been really hard to get some sleep, but thank you.
Patrik: Yeah. Now I’ve just reached out since I read what put in the email. So it’s been since five weeks when she went into hospital.
RECOMMENDED:
Max: Yes.
Patrik: The first thing that I want to highlight from your email is you are saying that the doctors told you they’ve made a medical decision not to resuscitate her?
Max: Yeah.
Recommended links:
Patrik: Now, let me be very clear there, that is totally brutal, excuse my language. They can’t do that.
Max: Okay.
Patrik: They are at the complete mercy of you or your family to sign a document if you would agree on that. Are you in agreeance with that or…
Max: Well, they told us this morning that they’ve made the medical decision to do that.
Patrik: Let me explain this to you. I’ve worked in the environment for over 20 years. I’ve seen this so many times myself, that the boxes are ticked not for CPR. That is murder, right?
Max: Yeah.
Patrik: Hospitals are very good to pretend they can operate in a vacuum and nothing could be further from the truth. For such a life or death decision, which it is, such a life or death decision, they need 100% your or your dad’s consent whoever is the medical power of attorney.
Max: Okay.
Patrik: Okay. The reason I know this area so well is, number one, I’m having conversations like with yourself every day. When I still practiced in the environment I came to a bedside, to a patient and I looked through the records and I could see exactly that document tick not for CPR. My first question to the medical team was, “Have you discussed this with the family? Where’s the signature of the family?” And I get silence. And then I said, “Well, I’m not looking after this patient today because my registration is at stake. If I follow your wishes, the family might sue me. If I don’t give CPR to this patient because you are instructing me not to, but I don’t see a signature from the family I could end up in jail.” This is how serious this is. But hospitals are very good to pretend, “Oh, we’ll just make this medical decision.” It’s complete and utter nonsense.
Max: And why do they do that?
Patrik: Yeah. Great question. They need the beds. That’s number one. They need the beds, especially at the moment with COVID.
Recommended:
Max: Yeah, that could do that.
Patrik: I guess COVID is running complete rampant. ICU’s are running out of beds, running out of staff. So I mean, the situation is probably, has never been more critical. At the same time, this was common practice even outside of COVID. So it’s nothing new, I guess the COVID just made it worse. So unfortunately it’s common practice. And also there’s this element of ICU doctors in particular thinking even if your mom survives-
Max: Yeah, that she’s going to be worse.
Patrik: Correct. Well, who are they to judge?
Max: Exactly. Yeah.
Patrik: Who are they to judge? Who am I to judge what is acceptable for you as a family? What is acceptable for your mom, who am I to judge? So that is probably the most important thing that I wanted to get out of the way, because the risk of the heart stopping in a situation like that, it’s there.
Max: Yes.
Patrik: And if your mom’s heart was to stop God forbid they would just let her go.
Max: Yeah.
Patrik: So that I believe is the very first thing you and your family need to challenge. I give you a simple tip there, ask them for their hospital policy about CPR and ask, wait for an answer. If they have nothing to hide, if the policy says, “Oh, well, we can just make that medical decision.” They will present that policy to you in no time. And I bet they won’t.
Max: Yeah, noted.
Recommended:
Patrik: Also, it’s not only that.
Patrik: Yeah. So I’m talking to people every day in the US, UK, Canada, and Australia. There is a state law in black and white that they can’t make a decision about withholding CPR without your consent. So it’s not only hospital policies. It’s also state law.
Max: Okay.
Patrik: That’s that. Let’s move on to your other questions. Sorry, I just quickly bring up your email. So survival chances, very hard to predict. What I can tell you is this, the research is out there that 90%, roughly 90% of patients in ICU survive. That’s one in 10 that doesn’t survive. So the odds are in a patient’s favor. Now there are no statistics at the moment as far as I’m aware about the survivor rate for COVID. I do believe the survival rate for COVID is lower. Meaning that if you have 10 COVID patients, maybe only four survive. But I couldn’t tell you exactly. And I still believe the jury is out there. It’s still all new. Right?
Max: Yeah.
Recommended:
Patrik: In a couple of years, they’ll probably have better treatment, they’ll probably have a much better idea how many COVID patients survive. If they do survive, what does their quality of life look like? All of that. So pre COVID, 90% of ICU patients survive. Now, bear in mind, that doesn’t talk about quality of life six months down the line, it just talks about nine in 10 patients leave intensive care alive. Nobody tells you what that looks like in terms of quality of life, functionality, where do they end up, pure survival. What is definitely in your mom’s favor is age, 52. There’s no reason why your mom can’t survive. The bottom line is this though, the longer someone stays on a ventilator, the higher chances they don’t survive. Let me ask you this, do you know, have they proned her? Do you know when I talk about prone position?
Max: Yeah. I made sure that they were proning her and I constantly ask if they’re keeping her in that position, and if they push her like back and forth, back and forth from the back to her stomach. And I just constantly ask what position is in, letting them know that I know that proning is like the best option. But yeah, they do that.
Patrik: Okay. All right. And do you know how many days she’s been proned for?
Max: So she gets proned for about 16 hours and then she’ll come back, turned back and then she’ll get proned again for another…
Patrik: And for how many days have they done that for?
Max: I actually haven’t asked. But consistently every day that they call me, I ask what position she’s in. So consistently every day she’s basically in proning position.
Patrik: Look, it is the best option if you have no other treatment available. Now, the alternative to proning is ECMO. It’s a machine, its life support, especially at the moment. Pretty much all COVID patients in ICU are proned as the first-line treatment. And that may or may not work. With some patients it works wonders, other patients not so much. If proning doesn’t work, the next step should be ECMO. Now ECMO is a very scarce resource. Not every ICU has it. If ICUs have it, they need to have trained staff, because it’s a… Basically what happens is, in proning the ECMO machine does what the lungs should be doing. It’s basically bypassing the lungs. It’s exchanging oxygen and carbon dioxide and the lungs get a break. The lungs don’t get a break at the moment even though with proning. With ECMO the lungs get a break and they can heal.
Recommended:
Max: Okay. What’s the difference between the ECMO and the ventilator?
Patrik: Yeah. Great question. So at the moment, the ventilator is pumping oxygen into the lungs, which is why the lungs don’t get a break.
Max: I see. Because they are still working.
Patrik: Right. So the gas exchange, oxygen exchange, oxygen intake, and carbon dioxide exhalation is done through the ventilator, which means the lungs are still in action. With ECMO, you do the gas exchange outside of the body.
Max: I see.
Patrik: And therefore the lungs get a break.
Max: Yeah. I read about ECMO.
Patrik: Yeah. But it’s a very scarce resource. I would argue that out of, let’s just say I would argue 500 ICU beds, there would be 20 ECMO beds. So I don’t know how many ICU beds there are in your place. Probably more than 500, probably a 1,000, probably even more. Let’s just say for simplicity, there’s a 1,000 ICU beds. I would argue there would be 50 ECMO beds at the most. And they, I argue, are all occupied at the moment with COVID.
Max: Yeah. I’ll definitely bring it up with the doctors see if it’s an option.
Patrik: Yeah, absolutely. So the proning might work but it’s they… How many days has she been intubated now?
Max: It’s going to be two weeks tomorrow.
Patrik: Okay. All right. To answer your other question. Was it legal to intubate your mom without consent? Yes. In that instance it was legal because probably if they hadn’t intubated her, she probably would have died. So at the end of the day you only find out if you look at the medical records, but I have not seen people being intubated without saving their lives. You wouldn’t intubate someone unless there is a very valid reason for it. So she’s on dialysis at the moment?
Max: Yeah. She’s on dialysis because her kidneys were failing and needed that extra support.
Recommended:
Patrik: Right. Okay. Have they talked about ECMO? Not ECMO, sorry. ECMO we talked about. Have they talked about the tracheostomy?
Max: They haven’t. No, they haven’t brought it up.
Patrik: Right. Do you know what a tracheotomy is?
Max: Yeah. I believe it’s when they do it through the neck. It’s another form of ventilation, I believe.
Patrik: Yeah. Basically what happens is, so she’s got the breathing tube in the mouth, which is very uncomfortable.
Recommended:
Max: Oh, when she wants to wake up, something like that?
Patrik: Yeah. Because they have to sedate her, because it’s so uncomfortable. So a tracheostomy would help her to wake up but only if, for example, if they did a tracheostomy and they would still prone her, she would still need a lot of sedation. Because the proning in and off itself is uncomfortable. But if your mom wasn’t proned, and they should definitely do a tracheostomy just for comfort, getting off sedation trying to wake her up.
Max: What is that?
Patrik: Are you seeing her? Can you see her by a Face Time?
Max: Well, she’s completely sedated so we haven’t actually Face Timed. We just kind of have a speaker and then we talk to her, but we don’t see her or anything. But even if we did she wouldn’t be able to see us either. We just talk to her, my sisters and me, my dad and me, given what works.
Patrik: Okay. What are they saying are the next steps for them?
Max: They’re saying that they’re just going to keep doing the dialysis on her and hope that her kidneys get better. And because she choked on her nutrition I believed in the morning, her lungs got another hit and so the lungs are damaged and scarred. And so they’re going to hope that it gets better. But there are no other steps that they’re probably taking.
RECOMMENDED:
Patrik: All right. I’m hearing this at the moment all the time with COVID in particular, that the lungs are scarred, hearing it every day. Do you know how much oxygen she is on?
Max: Yeah. Yesterday, it was the first good news that we got from the doctors from the whole situation, is that she was on 60, and so she was breathing a little better. But because of her gagging on her nutrition in the morning today, she went back to getting on 100%.
Patrik: So she aspirated? Do you know what I mean?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!