Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about,
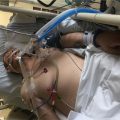
My Dad Needs Dialysis in Intensive Care After Sepsis! What are His Chances of Survival? Live Stream!
Welcome to another intensivecarehotline.com livestream. We are live now, and today’s topic is “My dad needs dialysis in intensive care after sepsis. What are his chances of survival?” So, this is today’s topic. I want to welcome you all.
I do these live streams every week around the same time. It’s usually 8:00, 8:30 Eastern Standard Time in the U.S., which is 5:00, 5:30 PM Pacific Time in the U.S., and you can work out Central Time, Mountain Time in the U.S., what times they are. 7:30 Central Time. 6:30 Mountain Time. It’s 10:30 AM in Sydney and in Melbourne. Unfortunately, this is in the middle of the night for our U.K. audience, for our U.K. viewers, but this live stream is recorded, and it will go live once the video has been uploaded, which is usually within less than 24 hours after the live stream.
So, please type your questions into the chat pad. Try and keep them to today’s topic. But if you have any other questions, please type them in, and I will get to them at the end of the presentation.
If you like this video, give it a thumbs up. If you find value in it, share it with everybody else that can benefit from this video. Click the notification bell and subscribe to my YouTube channel for updates and live streams for families in intensive care.
Now, a little bit of housekeeping. That’s the housekeeping out of the way. So, before I go into today’s topic, you might wonder what makes me qualified talking about this topic. So, I have worked in intensive care as a critical care nurse for over 20 years in three different countries, and out of those 20 years, I’ve worked as a nurse unit manager for over five years. I have founded several businesses in the intensive care space. One of them is Intensive Care Hotline, which is a consulting and advocacy service for families in intensive care. I also own and operate a business called Intensive Care at Home where we provide services for long-term intensive care patients in the home with critical care nurses, 24 hours a day.
So, with today’s topic about dialysis or hemofiltration in intensive care, I’ve looked after hundreds, potentially even thousands of patients in intensive care on dialysis, or I have overseen their care as a nurse manager or charge nurse, whichever way you want to call it.
So, let’s dive into today’s topic, “My dad needs dialysis in intensive care after sepsis. What are his chances of survival?” So, this is a question we get quite frequently. Whether it’s my mom, my dad, my sister, my brother, my spouse, my child, my grandparent, this is a question we get quite frequently almost every day, and that’s why I thought it’s valuable making a live stream about this. So, let’s break this down.
RECOMMENDED:
Many patients in intensive care end up on the haemodialysis machine for acute kidney injury temporarily, most of the time. Most of the time, it’s temporarily for an acute kidney injury or acute kidney failure, also known as Acute Kidney Injury (AKI) in medical terms. So why do people need that, what’s also referred to in medical terms as renal replacement therapy?
So, when someone comes into intensive care, they are at a high risk of an infection. If they do get an infection, they are at high risk of potentially ending up in sepsis or septic shock. If sepsis or septic shock happens, blood pressure goes down for prolonged periods. Patients in intensive care are incredibly unstable. They need life support not only with ventilation, tracheostomy, breathing tube/endotracheal tube. They also need vasopressors or inotropes to sustain a physiological blood pressure or a blood pressure that’s compatible with life.
During the periods of time of sustained low blood pressure, the kidneys and other organs may not be perfused as much as they need to be perfused to sustain organ function. Therefore, prolonged periods of the kidneys not getting the adequate perfusion with blood puts them in the position where they shut down. If the kidneys shut down, urine output goes down. Urea and creatinine go up. Urea and creatinine are kidney markers in the blood, which then confirms a kidney dysfunctional or an acute kidney injury.
Now, the terms “urea” or “blood urea nitrogen” are interchangeable predominantly in the U.K. and Australia. We measure urea. Whereas in the U.S., you more refer to BUN (blood, urea, nitrogen) levels, but at the end of the day, it’s the same. So, if that happens, if an acute kidney injury happens as part of someone going into intensive care, as part of a trauma, as part of an infection, as part of post-operative complications, as part of, at the moment, COVID complications, at the end of the day, all tracks lead to sepsis no matter why someone went into ICU. A lot of patients in Intensive Care Unit (ICU) go into sepsis or septic shock because of their primary condition that got them into ICU in the first place. So, those are reasons why someone can end up on dialysis or hemofiltration.
Other reasons why someone can go on dialysis or hemofiltration is for rhabdomyolysis, which means if someone in ICU has trauma and multiple fractures, they often have what’s called rhabdomyolysis, and they need dialysis as well. I’ll break that down in a minute. So, that’s just to set the scene why people need dialysis, and as I said, it’s often temporarily when someone needs dialysis in intensive care.
So, rhabdomyolysis. It’s a breakdown of muscle tissue that releases damaging protein into the blood. The muscle tissue breakdown results in the release of protein myoglobin into the blood. Myoglobin can damage the kidneys. If someone goes on dialysis for rhabdomyolysis, it’s often prophylactically before patients actually go into kidney failure. Whereas if someone goes on dialysis or hemofiltration because of high urea, and high creatinine, and urine output going down, it’s often when the acute kidney injury actually happened already.
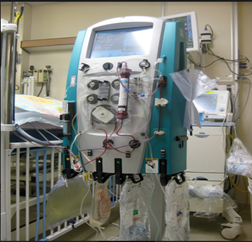
Now, when someone does go on dialysis, it’s often they need what’s called a vascular catheter. The medical term is a vascath. It’s a double-lumen line that goes into the neck, into the shoulder, or into the groin, and the dialysis machine will be connected to that. Blood will be extracted and run through the dialysis machine. Fluids will be removed. The other term for dialysis is RRT, Renal Replacement Therapy, which basically means the dialysis machine is replacing the kidney function.
Suggested Links:
So, when someone goes on dialysis, there are several things that need to be considered. Often, they need to be started on a local heparin. Heparin is a blood thinner. It runs through the dialysis machine. It prevents the dialysis machine from clotting or prevents the blood from clotting. Often, when someone is in sepsis and has a low blood pressure, and they’ll be started on dialysis, blood pressure goes down even further. It goes about 300 mls of blood are extracted from the body and are running through the machine, are basically extracorporeal outside of the body, and that usually lets blood pressure go down, making the need for inotropes or vasopressors such as noradrenaline, adrenaline, or norepinephrine, epinephrine, even higher.
Other side effects from the dialysis are that often, hemoglobin drops because, again, you’ve got fresh blood going through a filter, and that might filter out some of the red blood cells. Also, if for whatever reason the dialysis filter clots and you’re not in a position to return the blood into the body because the blood has clotted, you’d be losing around 300 mls off your own blood, and that drops hemoglobin, and it might trigger the need for blood transfusions.
Now, I mentioned heparin as a local therapy going through the hemofilter to prevent the filter from clotting. Another alternative for that is a citrate infusion. It also prevents the hemofilter or dialysis machine from clotting. Now, for both heparin, you need to check activated partial thromboplastin time (aPTT) frequently, and for the citrate, you need to check the calcium levels frequently, making sure that the citrate and heparin that you’re giving are therapeutic within therapeutic range.
Other things that are important are to check electrolytes quite closely when your loved one is on a hemofilter or a dialysis machine. Electrolytes such as magnesium and potassium are very important. For example, when you run the blood through the dialysis machine, potassium and magnesium can drop quite quickly. Especially when potassium drops quite quickly, you need to replace fairly quickly because if your potassium drops below 4, 4.0, 3.5 millimoles per liter, it could trigger atrial fibrillation (AF), or other irregular heart rhythms in the heart, and that is obviously quite dangerous. Many patients on a dialysis machine end up on a potassium infusion. Again, these are the type of questions you can ask. Magnesium usually needs to be replaced once a day when someone is on a dialysis machine.
Now, what’s next? Very important. When someone goes on a dialysis machine, it doesn’t always mean that they are anuric. Anuria means, basically, no urine output. It means that they might be making some urine. Before someone goes on a dialysis machine, they often started on diuretics when they are in acute kidney failure or having an acute kidney injury. They often end up with an infusion such as… not necessarily with an infusion, but they often end up with furosemide or Lasix intravenously to see whether that’s doing the trick, but Lasix or furosemide, again, can only be a temporary fix as well. At the end of the day, the kidneys need to start working independently, and that is also always the goal when someone goes on a hemofilter or a dialysis machine in ICU. The goal is always to have it as a temporary therapy or temporary treatment.
Next, when someone goes on the dialysis machine, measuring fluid balance is very important. I mean, measuring fluid balance in ICU is important one way or another. What that means is you got to measure over a 24-hour period what’s going into the body and what’s coming out. For many patients in ICU, you want what’s being referred to as a negative fluid balance. Why do you want a negative fluid balance? Simply because most patients in ICU that are on a ventilator, and you want to wean them off a ventilator, you need a negative fluid balance to keep the lungs dry. That’s number one.

Number two, you don’t want to fluid overload kidneys that are already failing. If the kidneys are failing, if there’s fluid accumulation in the lungs, also known as pulmonary edema, combined with sometimes heart failure, you absolutely need to keep a patient on the dry side. Meaning, you need to have a negative fluid balance. More fluids should be coming out than going in, and you got to take into account urine output, of course. If there is no urine output, you got to take into account how much fluids are you removing from the dialysis machine or from the hemofilter. You got to take things into account such as bowel motions. You got to take things into account if someone has an abdominal drain, a chest tube. What’s coming out there? So, you got to take everything into account that’s coming out of someone’s body in order to have an accurate fluid balance.
Also, a fluid balance is not something you just measure over one day. You measure it over many days. Ideally, for someone with an acute kidney injury, you have a total fluid balance over many days because if you have someone, for example, with an acute kidney injury that is five liters positive, where the fluid balance is five liters positive over the last three days, you’re putting a patient potentially into harm’s way by increasing the risk of pulmonary edema, or fluid accumulation in the tissues. So, it’s very important to look at fluid balance. It’s also very delicate to manage a fluid balance, and many factors have to be taken into consideration.
Now, here is another question we get quite frequently, “Is dialysis or hemofiltration something that is permanent, or is it something that is intermittent? What are the outcomes?” Most patients in intensive care that end up on dialysis or on the hemofilter have dialysis or hemofiltration temporarily. Now, are there many patients that will never come off the dialysis machine after they’ve been started in intensive care on the dialysis machine for the very first time? Yes, that happens too, but from my experience, the overwhelming majority of patients that leave intensive care after they have dialysis treatment or hemofiltration treatment in intensive care, by the time they’re leaving intensive care, they’re liberated from the renal replacement therapy, and their kidneys have kicked back in again.
So then, what happens in ICU quite frequently is that a filter, a dialysis filter, or hemofiltration clots. That means there’s a clot in the hemofilter, and the dialysis machine stops. Now, if that’s the case, ideally, you return the blood into the body. Ideally, you disconnect the hemofilter, and you start all over again. Now, sometimes the intensive care team might decide that depending on fluid balances on electrolytes, depending on urea and creatinine, that you might give it a break for 24, 48 hours, and you might want to see other kidneys kicking back in again. Is the patient making urine? Then, there is no need to continue the dialysis machine or the hemofiltration. But in other instances, you might have a patient that’s heavily fluid overloaded. The kidneys have stopped working. The filter clots, you stopped the filter. You return the blood, ideally. You prime a new filter, and you restart dialysis as quickly as possible because it’s simply a therapy that is needed urgently for this particular patient that’s fluid overloaded and go from there.
Recommended:
Now, other things that you need to consider if your loved one needs hemofiltration or dialysis in ICU for an acute kidney injury or for acute kidney failure is that they might look very swollen. One of the reasons for the swelling is that they’re immobile, which means because they’re immobile and they don’t move, that fluids are not being shifted around. Then, how do you deal with that? (A), you can deal with that with physical therapy or physiotherapy. Physiotherapy should ideally start doing some passive range of motions. That’s one way to deal with it. You can elevate limbs, you can elevate the arm, you can elevate legs so that actually tissue is being pulled back or moving backwards to the body, going back into the blood.
Now, what sometimes triggers swelling as well besides the patient being immobile is that the albumin levels are low. If albumin levels are low and albumin transfusion is required, albumin increases the oncotic pressure in the artery and the veins, which means more fluids are being drawn back into the vessels, and that brings swelling down as well over time. So, albumin levels are very important, or again, as I mentioned before, hemoglobin might drop when someone is on the dialysis machine. If hemoglobin drops, there can also be some swelling because when someone gets a unit of red blood cells or blood transfusion, albumin being administered as well.
Next, when someone does go on the hemofilter, their body temperature, most of the time, drops. So, if that is the case, if someone has spikes of fever, 39.5, 39.5 Celsius, if you run them through the filter, the temperature drops. Now, they might even go down as cold as 34 now, 34 Celsius. Now, you need to warm them up on the other end. On the odd occasion, I have seen the filter being used just to get the temperature down because all other measures to get the temperature down failed. So, I’ve seen that on the odd occasion that the filter has been used to manage someone’s temperature. The dialysis machine often runs through a warmer, so that the temperature doesn’t drop too low.
Next, while someone is on a hemofilter or on the dialysis machine, they might take out the urinary catheter. Then, you got to check with a bladder scan whether the patient is still producing urine, whether you need to put in another catheter, because most patients in ICU can’t manage their bladder, their bladder function. If they do have a catheter in still, you definitely need to check urine output. You need to check that hourly to see whether dialysis might become obsolete, whether the kidneys have recovered.
Helene, nice to see you again, and your question is, “Can dehydration come from overdose Lasix?” Yes, absolutely. Absolutely. Dehydration can also cause acute renal failure. Patients that are dehydrated. Absolutely. Secondary to that can be kidney failure, for sure. Is that what you experienced with one of your family members, Helene, that they were overdosed with Lasix, and they ended up in kidney failure because of that? Is that what you think has happened? While I’m waiting for your answer, let’s just quickly carry on about dialysis and hemofiltration.
Suggested Links:
Now, sometimes what can also happen is you don’t necessarily want to remove fluids, but you want to remove toxins, which is basically what dialysis is all about. You want to remove the toxins that the kidneys normally get rid of. Sometimes you may not even want to focus on fluid removal. Sometimes you may just want to focus on getting rid of toxins such as urea, creatinine, and muscle tissue in case of rhabdomyolysis. They are all very important things to consider when someone is on dialysis. What’s the purpose of it? What is the purpose of the dialysis?
Next, when someone is connected and disconnected from the dialysis machine, it needs to be done sterile. The lines need to be flushed sterile. They’re often flushed with Hep-Lock to have a little bit of heparin in the lines to prevent the lines from clotting. Those lines often need to be changed every seven days because otherwise, there’s too much of an infection risk. If someone can’t come off dialysis in the long run, they need a permanent dialysis catheter/ vascular catheter. That is what often happens outside of ICU. It’s not something that happens inside of ICU.
So, that’s it in a nutshell, why patients end up on dialysis, what needs to be considered when patients end up on dialysis. Fluid balance is an important one and most… I realize when I talk to families in intensive care, they don’t have any idea about fluid balances in ICU and how important it is. Also, last but not least, when someone does go on dialysis and they’re hemodynamically unstable already, there’s a high risk of them needing inotropes or vasopressors. I think I briefly mentioned it earlier, but there are situations, especially when it comes to end of life in intensive care. Blood pressure is very low. Patients are in need of dialysis because their organs are failing, and you can’t get them on dialysis because they’re already having a blood pressure of 80 over 40. They’re already on maximum inotropes or vasopressors. If you would start them on dialysis, even though they need it, they would crash. They would crash. So, there needs to be a certain level of hemodynamic stability before someone can go on dialysis.
Just as a side note. many patients on extracorporeal membrane oxygenation (ECMO) need dialysis, and then dialysis is being connected to the ECMO machine as well. What’s important when someone is on dialysis is also, as I mentioned, you got to measure daily urea or BUN. You got to measure daily creatinine. You might also see that if someone does go into kidney failure, that they might be getting confused because toxins are not being cleared out of the body. Therefore, dialysis needs to be started as quickly as possible, and you will see that patients often clear up.
Now, also important. When someone is in kidney failure, and they have been in an induced coma for prolonged periods on maybe a combination of fentanyl and propofol, morphine and propofol, combination of morphine and midazolam or Versed, fentanyl and midazolam or Versed. If they’re not waking up, even though sedation has been switched off for many days, and they’re not waking up, but they are in kidney or liver failure, someone might start dialysis again to clear toxins to get rid of any medications that are still in the system, and that might also help to wake them up. Very important for you to know and understand that if toxins are floating around in the body, if sedation is floating around in the body, it can’t be cleared with the liver or with the kidneys. That’s what you can do about it.

Helene, you’re asking the doctors. Yes, this happened to your mom. “Doctors in ICU intentionally ordered hold off water and adversely prescribed two large bottles of Lasix. Nurse only documented one bottle but witnessed the two bottles given through the central line.” It’s probably important, Helene, whether… whatever has been given in terms of Lasix, it would be important to get a dosage. So, in order to increase someone’s urine output, you often start with 20 milligrams of Lasix intravenously. If that doesn’t work, you might go up to 40 milligrams of Lasix IV. Maybe you have a result after that.
Then, you would start and giving it maybe twice daily until you’ve got your fluid balance corrected, but you got to keep an eye on the fluid balance. You got to keep an eye on the electrolytes. You got to keep an eye on urea and creatinine, and you need to titrate it accordingly. You also have to look at fluid input, fluid output. There are several things you need to look at. Once they’re saying one bottle versus two bottles of Lasix, I would want to know the dosage. Was it 20 milligrams? Was it 40 milligrams? Was it 100 milligrams? So, it would be important to know.
RECOMMENDED:
Anyway, so I think I want to wrap this up today. If you have any other questions, please type them into the chat pad. You can also type them in under this video once it’s uploaded. So, last chance of answering questions if you have any. You can ask your questions that are off topic. You don’t need to keep them to the topic. I’ve given my presentation, I pretty much said everything that I wanted to say about dialysis and hemofiltration, and if you have any questions now…
“They’re also giving her excessive IV fluids overloaded.” Helene, I don’t know what you mean. I know what you mean by that, but to a degree, that’s contradicting what you said earlier. You said they were dehydrating her by giving too much furosemide, and now you’re saying they have fluid overloaded her. So, was that on two separate occasions? How did that happen? How can they fluid overload her and dehydrate her at the same time, or did that happen on two separate occasions?
Anyway, so if you have any other questions, please type them into the chat, but as I said, you can type them below after the video has been uploaded after… If you’re watching this video, once it’s been uploaded, type your questions away, or if you have any other questions, just send them to [email protected], and we’ll get back to you. You can also call us.
If you go to intensivecarehotline.com, call us on one of the numbers on the top of the website. You will also find the numbers below this live stream on YouTube.
We also have a membership for families in intensive care. You will find that at intensivecaresupport.org. I also provide one-on-one consulting and advocacy for families in intensive care.
If you like this video, subscribe to my YouTube channel, give it a thumbs up, click the notification bell, and leave your comments below.
Now, Helene, you’ve got another question. It says, “Yes, hold on water for three days.” Wow. That sounds like medical negligence to me, Helene. It sounds like medical negligence to me, “Hold off water for three days.” Do you know why?
Now, also, while I’m waiting for your answer, I will do another live stream next Saturday night, 8:30 PM Eastern Standard Time in the U.S., 7:30 Central Time, 6:30 Mountain Time, and 5:30 Pacific Time. That will be 10:30 Sydney/Melbourne time, and unfortunately, it’s in the middle of the night for our friends in the U.K.
Please note that next week, I will be doing a live stream about, “Someone not waking up after an induced coma. Should sedation and medication be changed?” So, watch out for that live stream for next Saturday night in the U.S., Sunday morning here in Australia. Watch out for that.
Now, if there are no other questions or comments, I do want to wrap this up. I will be publishing any quick tips this week on YouTube.
Again, go to intensivecarehotline.com if you have a loved one in intensive care and call us on one of the numbers on the top of the website. I wish you and your families all the best.
Have a wonderful Saturday or Sunday. Have a wonderful weekend and a great week ahead.
Take care.
Thank you.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!