What is liver failure?
Liver failure is a severe decline in liver function and the inability of the liver to perform its normal synthetic and metabolic function as part of normal physiology. Two forms are recognised, acute and chronic.
Acute Liver Failure is defined as “the rapid development of hepatocellular dysfunction, specifically coagulopathy and mental status changes (encephalopathy= disease or disorder of the brain) in a Patient without known prior liver disease”.The diagnosis of acute liver failure is based on physical exam, laboratory findings, Patient history, and past medical history to establish mental status changes, coagulopathy, rapidity of onset, and absence of known prior liver disease respectively.
Chronic liver failure usually occurs in the context of liver cirrhosis, itself potentially the result of many possible causes, such as excessive alcohol intake, hepatitis B or C, autoimmune, hereditary and metabolic causes (such as iron or copper overload, Steatohepatitis or non-alcoholic fatty liver disease).
The symptoms and signs of liver failure include tiredness, loss of appetite, nausea, bruising and excessive bleeding, confusion, abdominal pain and swelling, and a yellow tinge to the whites of the eyeballs and skin (jaundice). If the condition becomes worse and the liver continues to fail, other symptoms may develop such as muscle wasting, marked fluid retention(edema), and increased confusion that may progress to a coma. The build up of toxins in the body, contributes to increased confusion(encephalopathy) and swelling of the brain tissue. This is a sign of end stage liver disease.
- What does the Liver do?
- What Happens in Intensive Care?
- How long will your loved one remain in Intensive Care?
- Weblinks
What does the Liver do?
The liver is the second largest organ in the body, sitting under the diaphragm and lungs. There are two lobes or sections of the liver, the right and the left lobe. The right lobe is six times larger than the left. The liver is made up of many liver cells called hepatocytes. The liver is an important organ in the body and is responsible for a number of essential functions.
The liver
- Filters the blood and breaks down toxins such as drugs and alcohol.
- Processes old blood cells and stores iron.
- Helps to maintain normal blood sugar level.
- Produces the majority of clotting factors.
- Produces and maintains normal levels of protein in the blood.
- Assists in resisting infections by producing immune factors and removing bacteria from the blood.
- Plays a central role in fat and protein metabolism.
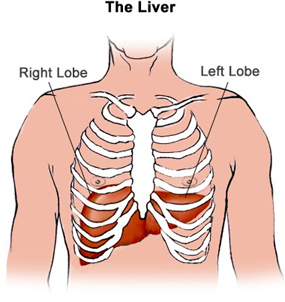
This image was found at Medicinenet
What Happens in Intensive Care?
Often people with liver failure can be treated in hospital without coming to an Intensive Care environment. However if the symptoms of reduced level of consciousness and or bleeding become worse they will be admitted to the Intensive Care Unit (ICU) for close monitoring and organ support.
If your loved one requires Intensive Care for Liver failure he or she
- will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Initially oxygen and respiratory support might be commenced via an oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required to improve and maintain the oxygen delivery
- Sedation may be used if your loved one is in an induced coma
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- Liver failure may also lead to kidney failure (renal failure) and the heart and lungs may also require support. Your loved ones neurological state and conscious levels are closely monitored to gauge how bad the brain swelling is. Supportive therapy includes the use of drugs to support blood pressure, and a dialysis machine to support and do the work of the kidneys. The liver has a capacity to regenerate itself and the plan of care is often to support your loved one until this can occur.Sometimes the supportive therapy will be unsuccessful and your loved one will be assessed for liver transplantation. If a liver is unavailable for transplantation or if your loved one is not suitable for transplantation then it is possible that your loved one may not recover.
Treatment for liver failure
If detected early enough, acute liver failure caused by an overdose of acetaminophen can sometimes be treated and its effects reversed. Likewise, if a virus causes liver failure, supportive care can be given at a hospital to treat the symptoms until the virus runs its course. In these cases, the liver will sometimes recover on its own.
For liver failure that is the result of long-term deterioration, the initial treatment goal may be to save whatever part of the liver is still functioning. If this is not possible, then a Liver transplant is required. Fortunately, liver transplant is a common procedure that is often successful.
How long will your loved one remain in Intensive Care?
The time spent in Intensive Care differs from Patient to Patient and can vary from a few days to a few months.
Weblinks
- Liver Foundation USA http://www.liverfoundation.org/
- British Liver Trust http://www.britishlivertrust.org.uk/
- Liver Transplantation January 2002 NSW Government Action Plan for Health
- NSWHealth Fact Sheets: Infectious diseases
- Better Health Victoria – the Liver explained
- Health Insite – Liver diseases , Australian Government
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related Articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


