Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I shared an interview on a podcast from one of my clients and the interview in last episode was
Interview with Ileana whose mother passed away in LTAC after ICU stay!
You can check out last week’s interview by clicking on the link here.
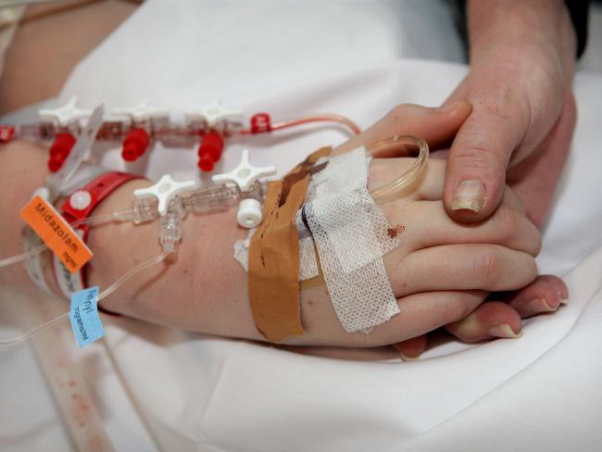
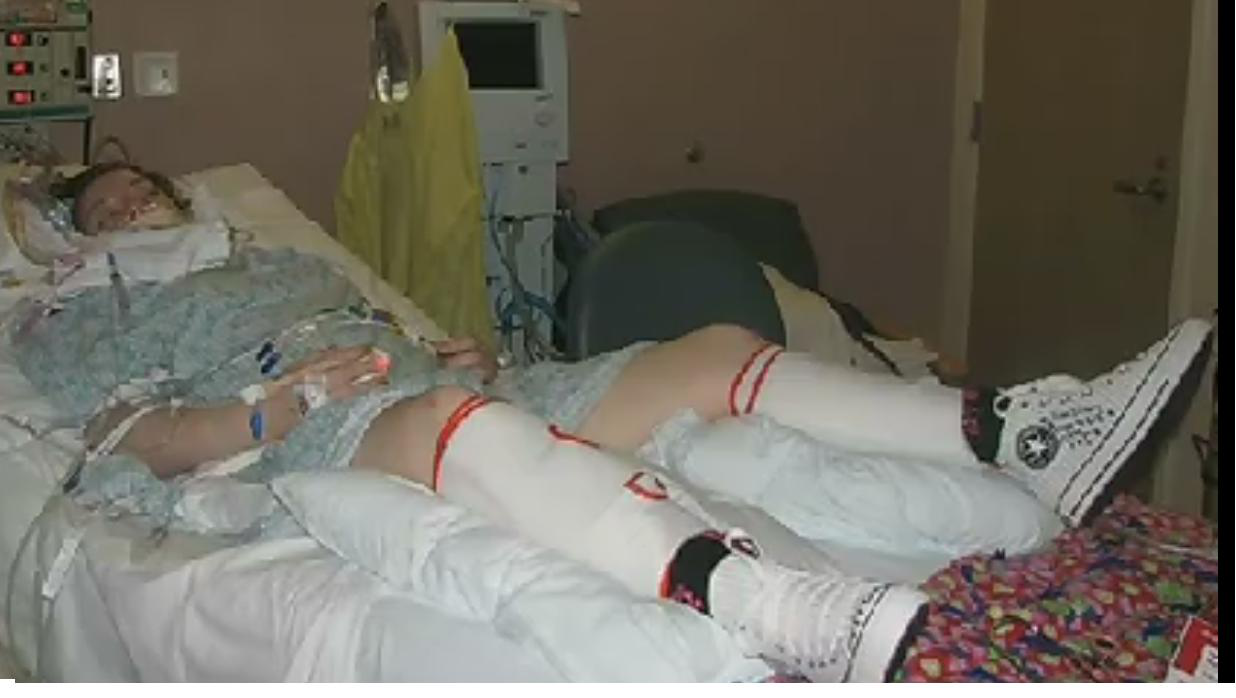
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one my clients Sheralee who has her daughter transferred in the Intensive Care due severe brain injury leading to alteration in mental function and state that needs to undergo tracheostomy.
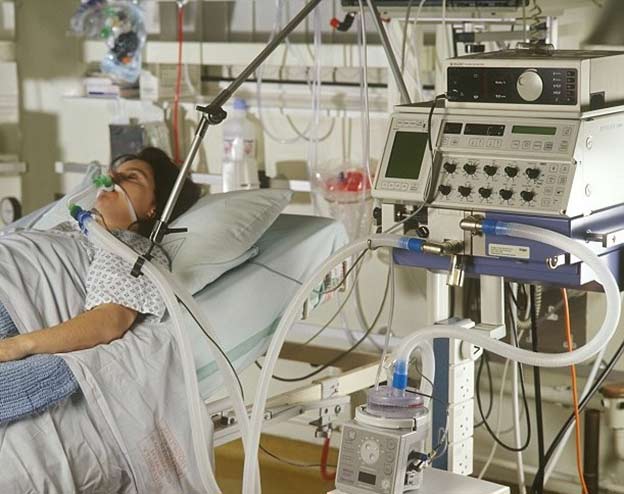
My daughter stops breathing frequently in ICU! Does she need a tracheostomy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Sharon here.”
Sheralee: Hello.
Patrik: Good morning. It’s Patrik from Intensive Care Hotline. How are you?
Sheralee: Yeah, I’m okay.
Patrik: I’m very sorry to hear that you have been in such a difficult situation, especially if you found your daughter in this situation.
Sheralee: Yep.
Patrik: What are they telling you?
Sheralee: They’re talking of giving us the option of doing a tracheostomy or not doing a tracheostomy.
Patrik: Mm-hmm (affirmative)
Sheralee: But the other night, she had a couple of apneic episodes, so I am starting to lean towards a tracheostomy. My family don’t really want to, but.
Patrik: Right, right.
RELATED INFORMATION:
Sheralee: The buck stops with me so. I believe she’s still there. There is just something, I just feel she is still there.
Patrik: Any seizures?
Sheralee: No, no seizures.
Patrik: And, are they, what’s their outlook like? Are they positive, are they negative?
Sheralee: Basically, they’ve become negative in the last 48 hours.
Recommended:
Patrik: Mm-hmm (affirmative) But they’re still happy to do a trach, or.
Sheralee: Yeah, they’re still happy to do a trach.
Patrik: Well, you probably haven’t read through the article yet. I guess from my experience you know, with anything that’s related to the brain, whether it’s a traumatic brain injury, or whether it’s a hypoxic brain injury, time is often what helps, right?
Sheralee: Mm-hmm (affirmative)
Patrik: And by time, I mean sometimes weeks and months. I guess, the goal is to get your daughter out of intensive care. That would be the goal.
Sheralee: That’s what they’re wanting to do. They’re wanting to do a tracheostomy and get her into a ward.
Patrik: Mm-hmm (affirmative) Well, if they do a tracheostomy, I mean, the question is can she come off the ventilator straight away? Have they looked into that?
Sheralee: I think they thought she could, but then she had these episodes last night.
RELATED INFORMATION:
Patrik: Right.
Sheralee: So, I’m not sure if she will. She’s only having a little bit of assistance from time to time.
Patrik: Okay. Okay.
Sheralee: She’s been breathing on her own quite a lot.
Patrik: Right.
Sheralee: She’s not being able to control her temperature or her heart rate very effectively, and her blood pressure is not being monitored because of the area of the brain that is damaged obviously.
Patrik: Mm-hmm (affirmative) mm-hmm (affirmative)
Sheralee: But, I mean, they tried to tell us that all the swelling will be down by now, which is not what I have researched and found out. What I’m understanding is the swelling will still be going down at this stage.
RELATED ARTICLE:
Patrik: When have they done the last CT scan?
Sheralee: I don’t think they’ve done a CT scan for a while. Because of where we are, they had to take her to the PA hospital for an EEG
Patrik: Oohhh.
Sheralee: That was done last Friday. That’s the last real test that they’ve done on her.
Patrik: Mm-hmm (affirmative) Because they can only really talk about swelling going down if they do a CT scan.
Sheralee: Right. Okay.
Patrik: Right. So, anything else is speculation really.
Sheralee: Yeah.
Patrik: Have there been any, there haven’t been any discussions about NFR (Not for resuscitation) or any of that, do you know what I mean.
Sheralee: They haven’t said it outright, but I know it’s what they’re planning, cuz he said if we take out the breathing tube, we’ve got to be clear on the fact that we won’t be putting it back in. Which to me means they’re planning to do a DNR (Do not resuscitate).
MORE INFO REGARDING DNR:
Patrik: Mm-hmm (affirmative) That’s right. And I guess if they are doing a tracheostomy, I guess that would be off the table to a degree. I guess the other thing you might want to think about is have they asked you that if her heart was to stop whether you want them to do CPR. Have they talked about that?
Sheralee: They haven’t asked me that yet. I know that will be coming. In some ways, I guess I am fortunate I’ve been through a similar situation, not hypoxic, but I watched my first husband pass away from a brain tumour many, many years ago. So, I’ve seen some of it, and I did sign a DNR then because I knew that it was hopeless.
Patrik: Sure.
Sheralee: But this time, I know it’s not.
Patrik: Mm-hmm (affirmative) Good. Good. And you’ve got to be very clear on that because they wanna make their own decisions.
Sheralee: Yes, I know. And they’re having a bit of an issue with us because they keep on telling us these things and we keep looking at her and saying Francisca, we know you’re still there, and I think they are having a bit of an issue with us.
Patrik: Yeah.
Sheralee: They are acting like we are in denial, but fortunately my family has not given up hope.
RELATED ARTICLES:
Patrik: Yeah. Yeah. And you know the reality is for whatever reason your daughter is not waking up, there’s still time to talk about that.
Sheralee: Yeah.
Patrik: You know, it’s probably way too early to look at all of those decisions.
Sheralee: Yeah, I think so. I want to give it some time. I don’t know when the right time is, but I do, there are just little signs to me. There was a time I was sitting there holding her hand about a week ago, and I said FRancisca, if you’re there, can you just give me a sign, can you move your hand. And her thumb moved slightly, and I thought what? And my son looked at me said “what is it?” and I said “I asked her to move her hand and her thumb moved slightly.” He lifted up the blanket and I said “Francisca, can you do that again?” and she did, and he saw it. So, I truly, truly believe she’s there. They’re acting like we’re just wanting the best, but there have been little signs to me. We’ve got a new, great Occupational Therapist, who is coming and is giving her some great therapy. She has sort of been saying to us one sense at a time. Only hold her, or talk to her. Don’t do both. And she’s really trying to bring her back. She started cocooning her with pillows to try and help her feel safe. So we’ve got some positive things happening.
Patrik: Yeah. Yeah. And that’s what you’ve got to keep looking for. The main message that I think I want to give you is really don’t give up hope, and number two, and you’ve gotta keep in mind, they are looking for a solution for their ICU, you are looking for a solution for your daughter.
Sheralee: Yep. Well, it’s a nightmare that they are only funded for seven beds.
Patrik: Yeah. They have a bed problem.
Sheralee: Yes they do have a bed problem. They’re full up. I know they’re full up. And she’s been there for two weeks.
Patrik: Yup. Yup. Absolutely. And, their worst nightmare is that she will be there for another four weeks. That’s their worst nightmare.
Sheralee: Yeah.
Patrik: Right and you’ve got to keep that in mind at all times, and you’ve got to position it, you know, you’ve got to spell it out because they are probably only telling you half of the truth. You know they’re telling you the swelling hasn’t gone down. Well, if they haven’t done a CT scan, where’s the evidence?
Sheralee: Yeah, well they are saying that the swelling has gone down and this is as good as it is gonna get. And that’s the problem. I don’t believe that at all.
RELATED INFORMATION:
Patrik: No. No. No. No. They’ve gotta do more CT scans. It’s a bit unfortunate that they have to go to PA to do the CT scans.
Sheralee: Oh, CT scans can be done at Logan. It’s the EEG that they couldn’t.
Patrik: Okay. But that’s interesting because an EEG, you don’t need to go into a scanner for an EEG. You just hook up at the beside with a machine.
Sheralee: Well, for some reason in order to do the EEG they wanted to, they took her to PA.
Patrik: That doesn’t make any sense to me because again, for an EEG, you gotta have a machine, you hook it up to the person’s head.
Sheralee: Yeah they did that. We had one of those and in there for a while and you could see there was brain activity. And you could also see she does respond to stimuli. If they’re giving her a blood test or something, she reacts.
Patrik: Good. Good
Sheralee: She is definitely responding to stimuli. They’ve admitted that.
Patrik: Right. Do you know whether her pupils are reacting to light.
Sheralee: Yes, they are reacting to light.
Patrik: Okay. When they put pain stimuli on her fingers or on her toes, what is she doing?
Sheralee: Mmmmm.
Patrik: Have you seen that?
Sheralee: No, I haven’t seen that. Oh, actually, she reacts on the fingers because they’re doing blood glucose tests, and she doesn’t like it.
Patrik: Okay. She’s grimacing, or is she opening eyes?
Sheralee: Yes, she’s grimacing, and she’s not opening her eyes, but she’s grimacing, and trying to pull away.
Patrik: Yeah. Yeah. And you’re certain that she hasn’t been on any sedation for days now? You’re certain about that?
Sheralee: Not for days no. She hasn’t been for days.
Patrik: Okay. Do you know?
Sheralee: They put her on a little bit of sedation for one time when they were doing something to her, but it was only for a short period of time.
Patrik: Right. Do you know what sedation they’ve given?
RELATED ARTICLES:
Sheralee: No, I don’t. I can find out.
Patrik: Okay. You should find out, and the reason I’m saying that is there is a difference between long-acting and short-acting sedation.
Sheralee: They’re only giving her short acting I know.
Patrik: Propofol.
Sheralee: Yeah. That would be right.
Patrik: Yeah. Okay. So if they’ve given her Propofol, you know, that’s short acting, it basically means as soon as Propofol is coming off, people wake up relatively quickly.
Sheralee: Yeah, that’s what they’ve been telling me.
RECOMMENDED:
Patrik: Right, right, they don’t have to. People wake up quicker compared to the long-acting one which is Midazolam and she would have had some Fentanyl or some Morphine as well for pain.
Sheralee: Probably, yeah. Probably. I don’t think she’s on anything anymore.
Patrik: Yep good, good. But what I’m saying is the Fentanyl or the Morphine are long acting so that means even though Propofol is short acting, if she had Morphine or Fentanyl, that might still be hanging around, and it might stop her from waking up as much as she can at this point in time.
Sheralee: It wouldn’t have been in the last five days or so.
Patrik: Okay, okay. So yeah, so then, I’d say five days if her kidneys are working, she should slowly wake up. She should. But then that is dependent obviously on what’s going on in the brain.
Sheralee: Yes. I’m positive.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!