Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
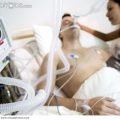
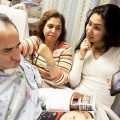
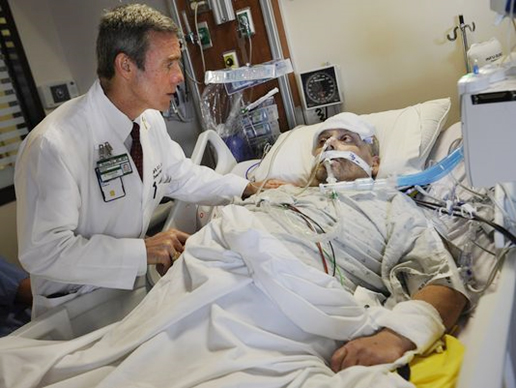
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Isabel as part of my 1:1 consulting and advocacy service! Isabel has concerns about the tracheostomy procedure that her husband needs in ICU and she asking about the risks and benefits of having it and how will it help her husband recover.
I Am Afraid About The Tracheostomy Procedure For My Husband In ICU. What Are The Risks And How Will It Help Him With His Condition?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isabel here.”
Helga: I remember you saying that, “that’s usually how you start weaning”, but because he was on ECMO, it was kind of too late for that.
Patrik: Now, now, yes. I don’t think I would have mentioned that it’s too late, it’s really never too late for a tracheostomy, but the risk of him having a tracheostomy while he was on a lot of heparin.
Helga: Yes, that’s what I meant with the ECMO, he didn’t need it because he was on ECMO at the time.
Patrik: Yeah. Look, generally speaking, if someone goes above two weeks of ventilation, patients should have a tracheostomy, generally speaking. Right. Now that he’s more or less taking the next step in his recovery, I do believe they need to look at a tracheostomy. Sorry, what’s your brother’s first name again, Noel?
Helga: Noel.
Isabel: Noel.
Patrik: Noel, sorry.
Helga: We called him Noel before, so that’s right, actually.
RECOMMENDED:
Patrik: Okay. Have you seen him in a video while he’s in ICU? Have you seen him at all?
Isabel: Yes, we do Zoom visits with him.
Patrik: Yeah. Have you seen the tube in the mouth, you’ve seen that?
Isabel: Yes.
Patrik: It’s very uncomfortable, it’s very uncomfortable. Tracheostomy is so much more comfortable.
Isabel: No, no. I’m still in the meeting.
Helga: Okay.
Isabel: He’s been like that for a while now, 30 days.
Helga: And one week off of pain medicine.
Patrik: Yeah. A breathing tube should be shorter. Right. And if you can avoid the tracheostomy that’s great, but on 55% of oxygen, unless he really can be weaned off the ventilator in the next few days, I believe they definitely should review him having a tracheostomy. It’s just so much more comfortable. It’s easier to wean patients off the ventilator, it’s just easier, for a number of reasons. Tracheostomy will be sitting in the neck.
Isabel: Yes.
Helga: Versus going down this road. Yeah.
Patrik: Yeah.
Helga: What did she say, she did say that, because he’s still considered unresponsive, but she said that, “it’s not consistent, but sometimes he’ll flinch a little bit to pain,” to some painful stimuli not consistent enough and they talked about some of the things that they do that sounds like it hurts, but I didn’t know I just wanted to tell you that she mentioned that his feet will flinch sometimes.
Patrik: So, the biggest concern really is, if he’s got the Glasgow Coma Scale of four or five, that’s certainly concerning. From what I remember, he’s been off sedation since Sunday, the 12th. You recall that?
Helga: Yeah, that sounds right. When the tests results first came in.
Isabel: Yeah, that’s accurate.
Patrik: So, he’s been off sedation since Sunday the 12th. So, here’s my take on this, when patients come out of an induced coma, and don’t have a brain injury, they may not wake up for that period of time. I have seen this, okay. It’s just people are critically ill, they just need time to recover. However, in the light of the code the likelihood of him not waking up because of a brain injury is definitely there. If he didn’t have the code, I would say, “Okay, sometimes people take a long time to wake up after an induced coma even without a brain injury, but now we are day nine, day 10.” You should show more signs of waking up. The question is, have you heard from a neurologist?
RECOMMENDED:
Isabel: No, they were supposed to do that today.
Patrik: After the MRI?
Isabel: Right.
Patrik: And there has been no neurologist involvement since Friday.
Isabel: Right.
Helga: I have a question, Isabel, because Dr. Dy, the one that was a little bit more negative on our first meeting, I could have sworn when he was referencing the first EEG saying that it was consistent with the anoxic brain injury. When we asked him more questions, he mentioned he needed to refer to neurology, but today Dr. Abril said that he was a neurology specialty. Wasn’t that correct?
Isabel: No. Dr. Abril isn’t neurology, he’s ECMO. Dr. Abril’s ECMO.
Helga: I’m sorry.
Isabel: She said Dr. Lim, was the neurology.
Helga: Lim. Okay. Got it. Okay. Just making sure, because I thought whoa, whoa, whoa. He just told us he didn’t know, and now they’re referring to him. Okay. Got it. So, it’s a different doctor. Okay.
Patrik: Have they mentioned anything else?
Isabel: No. No.
Patrik: Okay.
Isabel: Other than, their focal point being the brain injury, the level of brain injury. I mean, what is the MRI tell us, what is it going to tell us.
Patrik: The MRI will show them if A, if there is brain damage, and B, where it’s located. That’s what the MRI will show you Are they talking about Was there any more talk about?
Isabel: Oh okay.
Patrik: Are they talking about… was there anymore talk about… he told me ventilator settings 55% of oxygen, have they talked about whether he’s taking any breaths himself?
Isabel: Whether he’s taking breaths?
Patrik: Yeah. Or is the machine doing everything?
Isabel: No, they didn’t mention that.
Helga: Not today, but on ECMO with Dr. Charles , he did mention that Noel would sometimes take a breath and sometimes even cough.
Patrik: Yes, no, he did mention that. Yeah, he did mention that. Yeah, no. Okay.
Helga: But we haven’t asked anything since then.
Patrik: Okay. All right. Because if he’s taking breaths himself, that’s a sign that the brain is doing something, that’s definitely a sign.
Isabel: What about the coughing?
Patrik: Oh, coughing is a good sign for sure. That’s a good sign. Is he coughing?
Isabel: That’s what he said. I remember him saying that “He coughs.” Didn’t he say that?
Helga: Yeah. He said that, “Sometimes he’ll cough,” yeah. I don’t know if that’s when they’re clearing out stuff, but that was surprising, yeah, that he was coughing.
Patrik: No, that’s good. I mean, those are the first signs of getting more awake, coughing, taking breaths. Do you know if he’s opening eyes?
Isabel: He’s opening his eyes, but it’s a blank stare. He’s not blinking, he’s not responding to threat like they said.
Patrik: Yeah.
Isabel: But what does that mean?
Patrik: It means that potentially brain activity is minimal. But again, I have seen this with patients that don’t have a brain injury, that come out of a prolonged induced coma, and it takes sometimes up to two weeks for them to wake up. So, but I guess in this situation, where they’ve done the EEG, and the EEG suggests there is an anoxic brain injury, I guess the MRI today will tell you more information about where it’s heading.
Helga: Okay.
Patrik: You got to wait for the MRI. But I’ll tell you something else, and that’s one of the challenges of not being able to visit. One way to wake up a patient is, have they started some physical therapy? Have they started moving his arms, moving his legs? Have they started that?
Helga: Isabel?
Isabel: No, no.
Helga: We haven’t been told anything about that. We haven’t even asked about it either.
Patrik: Got to ask, got to ask. It’s so important. One of the challenges for a critically ill patient is that deconditioning is rapid. Right. Because it’s been 30 days now, he’s been in a coma for most of the time. So, the deconditioning goes rapidly. And they need to turn it up, and that starts with simple arm movement, leg movement.
Isabel: Yeah.
Helga: That makes sense.
Patrik: It’s critical and it also helps generally speaking with waking up. If you don’t stimulate someone, I think it needs to happen. You need to ask.
Helga: Okay.
Patrik: And then, taking it a step further, taking it a step further. As soon as he’s off the epinephrine or the norepinephrine, the vasopressors that we spoke about earlier, he needs to get out of bed. I know that sounds almost unachievable at the moment, but he needs to get out of bed even if it’s only sitting up to begin with. Head up, legs down, they can do that in the bed. Things like that need to be the next step to stimulating. So, he’s not waking up if they’re not stimulating him.
Helga: Okay.
Patrik: Do you think, it’s probably hard for you to say from a distance, but they probably not stimulating him enough?
Helga: When Isabel asked if they have, I think you were on the call with us when Isabel’s sister had asked if they were touching his hand and things like that. And they said that they would, I think they were just doing the assessment like the fingernail poking. That’s not necessarily. That’s just responding to pain. That’s not stimulation is what you’re saying.
Patrik: Very much no.
Helga: So, we need to ask them if they specifically do that. Okay.
Patrik: Yes, very much so.
Isabel: So, that’s called stimulation therapy.
Patrik: No.
Helga: Physical therapy.
Patrik: Physical Therapy, this is a therapy. Right. So, and that leads me back to the tracheostomy and I’ll tell you why. So, if they can gradually stimulate him, and if they can gradually start with things like sitting up, head up, legs down. And then the next step is to get him in a recliner chair, I know that almost sounds unachievable at the moment, but I know a good ICU, we’ll do that. But that’s much easier once he’s got a tracheostomy, so much easier. Because the risk of the breathing tube coming out is so much higher. When you mobilize a patient whilst once you have a tracheostomy, it’s so much more stable, so much more safe to get somebody in a recliner chair, for example.
RECOMMENDED:
Isabel: Yeah.
Patrik: So, those are the next steps, I believe.
Helga: I have a question.
Patrik: Yeah, please, please.
Helga: Go ahead, go ahead.
Patrik: That’s going to be the next steps irrespective of what the MRI shows, because they need to stimulate him one way or another.
Helga: Okay. Now, I was going to ask as far as, so it sounds like we need to be asking him regardless of the results of the MRI, we need to ask them what the plan is to wean him off the ventilator, and see if they mention tracheostomy. If not, then we can bring it up. And if they were to suggest that it was too risky, like they did last time, do we now, what is our counter to that of saying, justifying it, other than it just being easier or safer? What?
Patrik: In terms of weaning him off the ventilator?
Helga: Right. if we were to say, when we ask them what’s their plan to wean him off, and if they don’t mention tracheostomy and we bring it up, and they were to say that’s not a good idea for whatever reason. How do we counter that? That’s why we want to move forward with it.
Patrik: Yep. No, that’s a great question. So, there’s two arguments at the moment that the sort of ICU community is making. Prior to COVID, the standards were sort of two weeks breathing tube at the most, then you would be looking at a tracheostomy if somebody can’t be weaned. Now, with COVID, that approach has changed from what I understand. When somebody is having a tracheostomy at the moment, the risk of COVID spreading in the air is pretty high. Right. So, that’s one of the reasons why they probably delayed. Right. But I also know people with COVID do have tracheostomy, it’s just more risky at the moment, because of airway will be open, and it’s coming from the lungs directly, which means it’s a fairly high risk for the staff and the environment to have COVID spread in the air.
Patrik: That could be one of their arguments. But the other argument is clearly, I think he mentioned that on the weekend as well, it could damage the vocal cords. You remember that? He mentioned that.
Isabel: The tracheostomy or?
Patrik: No, the breathing tube?
Isabel: Oh yeah. Yeah. I mentioned that. Yeah.
Patrik: Could damage the vocal cords. The tracheostomy, to a degree as well, but the risk, generally speaking, of a breathing tube damaging the vocal cords is higher.
Helga: Now question is, since he’s not on any type of pain medication, if they were to move forward with that, would we expect them to give him anything for that procedure or not at all?
Patrik: He would have a general anesthetic for the procedure, but it would be a short one.
Helga: Okay. So, it would wear off and wouldn’t affect the assessment, okay. Just because-
Patrik: Look, temporarily, temporarily.
Helga: I know that on Tuesday night when we spoke to the night nurse she, she kind of said that she thought that he could feel stuff, and it kind of scared Isabel and I, because she was just saying he’s on nothing, and he has everything on him, all these tubes, tubes. And if he could feel it would be very, very painful. And now we’re just, I think, he’s just, I’m hoping, he’s just asleep and can’t feel anything. So, I was curious if he had it, would we expect them to give him something just in case?
Patrik: No, he will definitely have something for sure. And it will be temporarily.
Helga: Okay. Their argument was that they didn’t want him on anything because the neurological assessment took precedence right now, since he wasn’t showing anything, any signs of feeling pain.
Patrik: Yep, agree with all of that. The only thing, a tracheostomy is, it’s almost like having surgery. It’s quick, and reasonably easy nowadays, but it’s still surgery and it requires a brief general anesthetic.
RECOMMENDED:
Helga: Okay. So, when does that start to happen. You said the next few days if he’s stable on the ventilator, is that something that we would ask for next?
Patrik: I think so. I think, as soon as soon as you’ve got an answer with the MRI, I feel, “Okay, what’s the point?” Now, if he’s is off ECMO, you will have an answer about the MRI. Someone like the neurologist, I believe, should advocate for a tracheostomy as well. Because the neurologist job is really, if there is a brain injury, to look at, “Okay, how can we treat this, how can we move forward treating the brain, can we look at rehabilitation down the line.” And if you look at rehabilitation down the line, one way to get into that point smoothly, I believe is a tracheostomy.
Helga: Okay.
Patrik: Because the tracheostomy just gives people time to maintain an unstable airway. And that’s what it is at the moment, he’s got an unstable airway. Tracheostomy is just to say a device to manage an unstable airway for longer periods of time.
Helga: Right. Because the ventilator is just shorter term.
Patrik: And the ventilator could be longer term, with the tracheostomy as well. But then you’ve got, with a tracheostomy, you can take it on and off, yeah you can do that at the moment as well, but it’s just higher risk.
Helga: Isabel, do you have anything, any concerns or worries about that? You want to ask? Because I know when they first mentioned it before he was on, where he’s at now a few weeks ago. It was a scary thing. I want to make sure your questions are answered about it.
RECOMMENDED:
Isabel: Yeah I had concern about it all, because they cut the throat and put the tube that way, but at the same time I was more uncomfortable with him having damaged his vocal cords. So, I’m okay, I mean, if it’s something that needs to be done, but my concern is the MRI results. Honestly, it really is going to determine which direction we’re going to go, to be honest with you.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!