What is a Heart Transplant?
A heart transplant, or a cardiac transplant, is surgery to remove a person’s diseased heart and replace it with a healthy heart from a deceased donor. It is a surgical transplant procedure performed on Patients with end-stage heart failure or severe coronary artery disease. As of 2008 the most common procedure was to take a working heart from a recently deceased organ donor(allograft)and implant it into a receiving Patient. The receiving Patient’s own heart is either removed (orthotopic procedure) or, less commonly, left in place to support the donor heart (heterotopic procedure); both were controversial solutions to an enduring human ailment. Post-operation survival periods averaged 15 years.
Worldwide, about 3,500 heart transplants were performed annually. The vast majority of these are performed in the United States (2,000-2,300 annually). About 800,000 people have a Class IV heart defect indicating a new organ. This disparity spurred research into the transplantation of non-human hearts into humans after 1993. Xenografts from other species and man-made artificial hearts are two less successful alternatives to allografts.
Because donor hearts are in short supply, Patients who need heart transplants go through a careful selection process. They must be sick enough to need a new heart, yet healthy enough to receive it.
Survival rates for people receiving heart transplants have improved, especially in the first year after the transplant.
About 88 percent of Patients survive the first year after transplant surgery, and 75 percent survive for 5 years. The 10-year survival rate is about 56 percent.
After the surgery, most heart transplant patients can return to their normal levels of activity. However, less than 30 percent return to work for many different reasons.
- Indications for heart transplant
- What does the Cardiovascular System do?
- What happens during surgery?
- What happens in the Intensive Care Unit?
- Immunosuppressants
- Complications
- How long is my loved one going to stay in Intensive Care?
- Links
Indications for heart transplant
The primary indications for heart transplantation for adult patients have been nonischemic cardiomyopathy (53%) and ischemic cardiomyopathy (38%). Other indications include: valvular heart disease (3%), retransplantation (3%) and others (<1%)
-
Refractory cardiogenic shock requiring intra-aortic balloon pump counterpulsation or left ventricular assist device (LVAD);
-
Cardiogenic shock requiring continuous intravenous inotropic therapy (i.e., dobutamine, milrinone, etc.);
-
Peak VO2 (VO2max) less than 10 mL/kg per min;
-
NYHA class of III or IV despite maximized medical and resynchronization therapy;
-
Recurrent life-threatening left ventricular arrhythmias despite an implantable cardiac defibrillator, antiarrhythmic therapy, or catheter-based ablation;
-
End-stage congenital HF with no evidence of pulmonary hypertension;
-
Refractory angina without potential medical or surgical therapeutic options.
Similarly, the European Society of Cardiology describes a series of features that must be met before consideration for heart transplant which are more specific and include, functional, structural and symptoms parameters;
-
Severe symptoms, with dyspnea at rest or with minimal exertion (NYHA class III or IV);
-
Episodes of fluid retention (pulmonary or systemic congestion, peripheral edema) or of reduced cardiac output at rest (peripheral hypoperfusion);
-
Objective evidence of severe cardiac dysfunction (at least one of the following): left ventricular ejection fraction less than 30%, pseudonormal or restrictive mitral inflow pattern on Doppler echocardiography, high left and/or right ventricular filling pressure severely impaired functional capacity demonstrated by one of the following: inability to exercise, 6-minute walk test distance less than 300 m (or less in women or patients who are age 75 and older), or peak oxygen intake less than 12 to 14 mL/kg/min;
-
One or more hospitalizations for HF in the past 6 months.
What does the cardiovascular system do?
The essential components of the human cardiovascular system are the heart, lungs, blood, and blood vessels. It includes: the pulmonary circulation, a “loop” through the lungs where blood is oxygenated and the systemic circulation, a “loop” through the rest of the body to provide oxygenated blood. An average adult contains five to six quarts (roughly 4.7 to 5.7 liters) of blood, accounting for approximately 7% of their total body weight. Blood consists of plasma, red blood cells, white blood cells, and platelets. Also, the digestive system works with the circulatory system to provide the nutrients the system needs to keep the heart pumping.
The heart is at the centre, basically distributing blood from the ‘central pump’ with the blood vessels the pipes of the body, trying to reach every corner of the body. The cardiovascular system also passes nutrients (such as amino acids, electrolytes and lymph), gases(Oxygen and Carbon Dioxide), hormones, blood cells, etc. to and from cells in the body to help fight diseases, stabilize body temperature and pH, and to maintain blood pressure.
In the heart there is one atrium and one ventricle for each circulation, and with both a systemic and a pulmonary circulation there are four chambers in total: left atrium, left ventricle, right atrium and right ventricle. The right atrium is the upper chamber of the right side of the heart. The blood that is returned to the right atrium is de-oxygenated (poor in oxygen) and passed into the right ventricle to be pumped through the pulmonary artery to the lungs for re-oxygenation(inhalation) and removal of carbon dioxide(exhalation). The left atrium receives newly oxygenated blood from the lungs as well as the pulmonary vein which is passed into the strong left ventricle to be pumped through the aorta to the different organs of the body.The left side of the heart then receives oxygen rich blood from the lungs and pumps this blood into the Aorta and arteries of the body. This pumping action is a complex well-coordinated activity that cannot be fully explained here. The heart itself, receives oxygenated blood supply via the left and right coronary arteries.
Poor or abnormal function of the cardiovascular system
May be a result of:
- Insufficient blood supply due to dehydration, bleeding or swelling;
- Insufficient blood supply to the heart due to ‘clotted’ arteries
- A poor blood supply to the heart, where there is not enough oxygen and other nutrients for its work;
- Poor lung function or obstruction to blood flow in the lungs, which places a strain on the heart muscle;
- Too many or too few electrolytes (eg. potassium, magnesium) that cause irregular heartbeats or dangerous rhythms in the heart.
- Weakness of blood vessel walls
- Heart muscle weakness Cardiomyopathy
- unhealthy lifestyle such as alcohol consumption, smoking, obesity
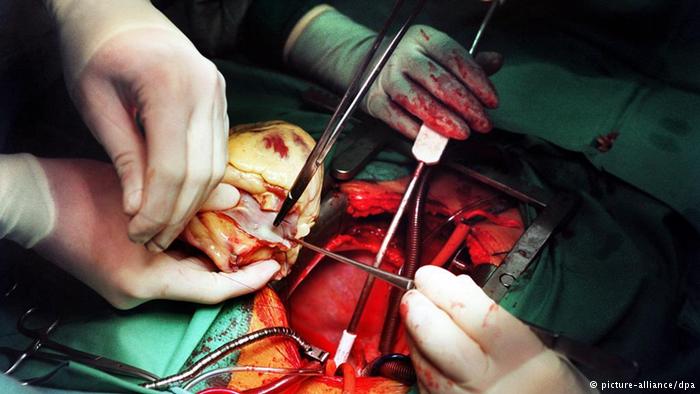
What happens during surgery?
Pre-operative
A typical heart transplantation begins when a suitable donor heart is identified. The heart comes from a recently deceased or brain dead(Brain Death) donor. The receiving Patient is contacted by a nurse coordinator and instructed to come to the hospital for evaluation and pre-surgical medication. At the same time, the heart is removed from the donor and inspected by a team of surgeons to see if it is in suitable condition. Learning that a potential organ is unsuitable can induce distress in an already fragile Patient, who usually requires emotional support before returning home.
The Patient must also undergo emotional, psychological, and physical tests to verify mental health and ability to make good use of a new heart. The patient is also given immunosuppressant medication so that the patient’s immune system does not reject the new heart.
Operative
Once the donor heart passes inspection, the Patient is taken into the operating room and given a general anaesthetic. Either an orthotopic or a heterotopic procedure follows, depending on the conditions of the Patient and the donor heart.
Orthotopic procedure
The orthotopic procedure begins with a median sternotomy, opening the chest and exposing the mediastinum. The pericardium is opened, the great vessels are dissected and the Patient is attached to cardiopulmonary bypass. The donor’s heart is injected with potassium chloride (KCl). Potassium chloride stops the heart beating before the heart is removed from the donor’s body and packed in ice. Ice can usually keep the heart usable four to six hours depending on preservation and starting condition. The failing heart is removed by transecting the great vessels and a portion of the left atrium. The Patient’s pulmonary veins are not transected; rather a circular portion of the left atrium containing the pulmonary veins is left in place. The donor heart is trimmed to fit onto the Patient’s remaining left atrium and the great vessels are sutured in place. The new heart is restarted, the Patient is weaned from cardiopulmonary bypass and the chest cavity is closed.
Heterotopic procedure
In the heterotopic procedure, the Patient’s own heart is not removed. The new heart is positioned so that the chambers and blood vessels of both hearts can be connected to form what is effectively a ‘double heart’. The procedure can give the Patient’s original heart a chance to recover, and if the donor’s heart fails (e.g., through rejection), it can later be removed, leaving the Patient’s original heart. Heterotopic procedures are used only in cases where the donor heart is not strong enough to function by itself (because either the Patient’s body is considerably larger than the donor’s, the donor’s heart is itself weak, or the patient suffers from pulmonary hypertension).
What happens in the Intensive Care Unit?
- After Heart Transplant surgery your loved one is admitted to the Intensive Care Unit
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required for 24-48 hours after surgery to improve and maintain the oxygen delivery, as your loved one is usually unable to breath for themselves immediately after surgery. The ventilator is usually “weaned off” over the next 12-24 hours, sometimes even quicker, after ensuring haemodynamic stability of your loved one is achieved. The process of weaning somebody off the ventilator my take longer in a Patient with lung disease and may sometimes stretch over a few days or weeks. If ventilator dependency continues for a few weeks, it is likely that your loved one will require a Tracheostomy
- Sedation may be used for ventilator tolerance and if your loved one is in an induced coma. Common sedation used is Propofol and Morphine or Fentanyl. If your loved one is unstable and/o is showing signs of bleeding, sedation may be increased, in order to minimise further risk of bleeding and also to focus on haemodynamic stability first
- Your loved one will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs), testing the effectiveness of the ventilation
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- Use of a Pulmonary Artery Catheters or a PICCO catheter to closely monitor cardiac function is not uncommon.
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- An oxygen saturation probe attached to the your loved ones finger monitors the oxygen level in the blood continuously
- Monitoring of the drains(chest drains) coming out of your loved ones chest, to drain any excess fluids of the surgery site and also to monitor any bleeding
- Abnormalities in heart rhythm usually require treatment
- Strict blood pressure control is achieved by medications infused via rate-controlled pumps. Fluid is also given intravenously at first to treat low blood pressure
- Body temperature is monitored. A blanket filled with warm air may be used to bring the body temperature back to normal
If you are visiting your loved one in the Intensive Care Unit at this stage you should expect to see many lines, tubes, and drains attached to your loved one.
Immunosuppresants
Your loved one remains on immunosuppressant medication to avoid the possibility of rejecting the new heart.
Common immunosuppresants are
- Corticosteroids (Steroids). Steroid therapy is a standard component of induction, maintenance, and antirejection therapy in heart transplant recipients. High-dose steroids are generally administered intraoperatively and postoperatively with gradual weaning of doses over months
- Azathioprine (AZA) and Mycophenolate mofetil (MMF) are the antiproliferative agents used commonly after heart transplantation. Azathioprine is used alone or in combination with other immunosuppressive therapy to prevent rejection following organ transplantation. Mycophenolate is a less toxic alternative to azathioprine.
- Cyclosporine is an immunosuppressant drug widely used in organ transplantation to prevent rejection
- Tacrolimus is an immunosuppressive drug that is mainly used after allogeneic organ transplant to reduce the activity of the patient’s immune system and so lower the risk of organ rejection
- Everolimus is currently used as an immunosuppressant to prevent rejection of organ transplants and treatment of renal cell cancer and other tumours
Complications
Post-operative complications include infection, sepsis, organ rejection, as well as the side-effects of the immunosuppressive medication. Since the transplanted heart originates from another organism, the recipient’s immune system typically attempts to reject it. The risk of rejection never fully goes away, and your loved one will be on immunosuppressive drugs for the rest of his or her life, but these may cause unwanted side effects, such as increased likelihood of infections, like fevers, unusual pains, or any new feelings. Recipients can get kidney disease from a heart transplant. Many recent advances in reducing complications due to tissue rejection stem from mouse heart transplant procedures. It is also a possibility post-operatively that the new heart is not working to its full capacity as yet and therefore VA-ECMO(ECMO(Extracorporeal Membrane Oxygenation) may be necessary.
How long does my loved one need to stay in Intensive Care?
The length of sty for your loved one after heart transplantation can vary, depending on factors such as Haemodynamic stability, acceptance of your loved ones body of the new heart, ventilator dependency, Inotrope dependency etc… Every Patient is different and therefore the length of stay in Intensive Care therefore may vary from a few days to a few weeks.
Links
http://www.transplant.org.au/Why-people-need-transplants.html Transplant Australia
http://www.ahlta.com.au/site/index.cfm Australian Heart/Lung Transplants association
http://www.organdonor.gov U.S. Government Information on Organ and Tissue Donation and Transplantation
http://www.heart-transplant.co.uk/ Heart transplant in the United Kingdom
http://www.organdonation.nhs.uk/ Organ donation in the United Kingdom
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long does a cardiac arrest patient stay in Intensive Care
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better…
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


