Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU and Julie is asking how come that the ICU team diagnosed her mom with irreversible respiratory failure without any scientific evidence?
The ICU Team Says Mom has Irreversible Respiratory Failure but Without Proof. What Should I Do?
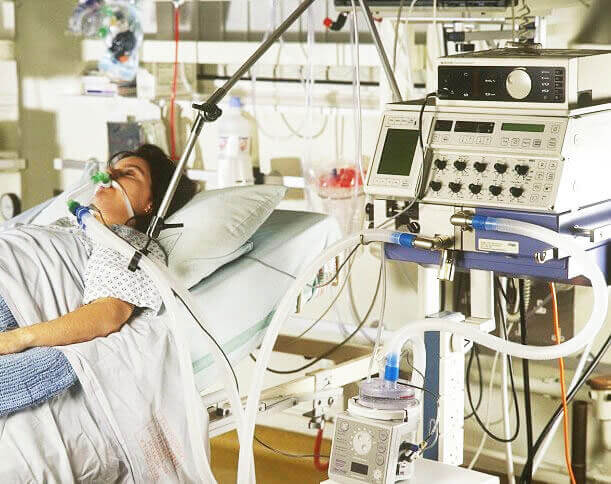
Julie: And then, I think he comes in every now and then, and kind of says something. And, I don’t know. You don’t really see a doctor. You never see the on-scene doctor. That one lady, I’ve only seen her in the meetings. I’ve never seen her face in that ICU.
Marvin: Oh yeah, me either.
Julie: So, you never see the doctors. And, you never catch the pulmonologist unless he’s at a meeting, or he’s there to extubate or intubate.
Patrik: That’s worrying. That’s very worrying. That’s very worrying.
Julie: So, we just need to get to this ethical meeting ASAP, I feel like.
Patrik: I think so.
RECOMMENDED:
Julie: I feel like we’re …
Patrik: I think so. What I would also do, Julie, is I would text you some links to a couple of interviews for you to get perspective. Because at the moment, all you hear is the doom and gloom. That’s all you hear. You know?
Julie: Yeah, you’re right.
Patrik: I will send you some interviews that you can listen to, that will give you perspective.
Julie: Because …
Patrik: Okay, because people have been in those situations. The other thing that I think I haven’t mentioned to you is, 90 percent of ICU patients survive. Ninety percent, roughly, give or take.
Julie: Yeah.
Patrik: So, the question you need to ask them is, why should your mom be one out of 10? Why? Why would she not be in the majority of patients?
RECOMMENDED:
Julie: They said it’s because of how ill she is.
Patrik: Yeah, yeah, understand. Understand that. But, I understand what they said. But again, at this point in time, we have no evidence that she is in respiratory failure. Yes, she’s ventilated, and she is in some type of respiratory failure. The question is, is it reversible respiratory failure? That’s the question.
Julie: And, that’s what they’re claiming, is not. They said it is not reversible.
Patrik: Yeah.
Julie: It’s the first time they said that today. But, there’s no proof of that.
Patrik: Yeah, exactly.
Julie: And even when I told her, I said, “Well, that’s funny, because my mom just finished three days of being on the ventilator, off the ventilator all day long.” And, they didn’t really have anything to say to that.
Patrik: So, that’s happened?
Julie: Yeah. My mom … Two days ago, they stopped it. So, for Friday since we left … So, which was Thursday, Friday, Saturday … No, Saturday, Sunday and Monday, she was on the ventilator, but she was on the weaning, so all day long. And, she was staying stable. No blood pressure medication. Nothing. And, she was doing like, 12 hour weans on the ventilator and still remaining very strong and very positive.
Patrik: So, that’s adding onto the ethical dilemma. Right? I mean, they’re telling you one thing, and if she was off the ventilator in the last few days, that’s painting a very different picture.
RECOMMENDED:
Julie: They say at night, she has to go back on.
Patrik: The ethical dilemma is thickening.
Julie: What did you say?
Patrik: Yeah, the ethical dilemma is sort of getting worse in terms of, well, if she’s had that time off the ventilator and now, they’re talking about respiratory failure, I say, you know, if she’s had time off … I know, I’ve seen patients who go into respiratory failure who died. They don’t die if they have time off the ventilator.
Julie: They don’t die if what? Oh, yeah, yeah. I see what you’re saying. If somebody’s in real true respiratory failure, that you wouldn’t be able to do wean trials, right?
Patrik: No, the minute, not for a minute.
Julie: Not for even a minute, you’re saying.
Julie: And, the only reason they cut back her trying for the last three days is because they said it was putting in an ideal amount of stress on her body, and they wanted to keep her relaxed so that she could … And, be a candidate for the surgery.
Patrik: Okay.
Julie: But now, she’s not a candidate because they determined as a staff that it’s not going to help her get better. And, she cannot even safely go with the procedure.
Patrik: Yeah, sure, sure. So, they changed their minds fairly quickly. You know, they probably realized, okay, well, your mom might as well get a tracheostomy, but then she could be in there for a long time to come. And, that’s what they’re trying to avoid. You know, so, if she had time off the ventilator in the last few days, I argue that claiming that she’s in respiratory failure is a false claim. Or, that she’s in irreversible respiratory failure, could be a bold claim.
Julie: That’s a bold claim. He said, he argues that she’s not. She wouldn’t have been able to do that.
Patrik: That’s right.
Julie: Well, you know, the blood pressure medications go up right before the talk with the surgeon, or they turn down the surgeon.
Patrik: Yeah, exactly. Exactly.
RECOMMENDED:
Julie: Everything is very … Yeah, and I don’t know that they really are going to contact another surgeon. Because, you know, they’re probably afraid that the outcome might get better. And, I’ll be quite honest with you. My mom asked for a lawyer prior to being intubated.
Patrik: Right. Okay. Does your mom have an advanced care directive? Is there something documented about her wishes?
Julie: Well, she whispered really quickly before the last time they put it on her, “Get me a lawyer.” And, my mom’s never asked for a lawyer. Never at the nursing home, never. She’s never felt so threatened that she’d need a lawyer. I thought that was a really interesting comment from her.
Patrik: Right. But, prior to going to hospital, she didn’t put down an advanced care directive where she documents something along the lines of, “Well, if I go to ICU, I want to have this, this, and this, and I don’t want to have this, this, and this.” There’s none of that.
Julie: No.
Patrik: Did you ever have a discussion with her about that. Did you and her, or anybody else within your family, have that discussion with her about her wishes if a situation like that came up?
Julie: No. But, I know that she’s very much pro life.
Patrik: Okay, okay.
Julie: And, very religious. And, also afraid to die.
Patrik: Okay. So, okay, good point. Good point, adding onto the ethical dilemma. Your mom is religious. She’s pro life. So, here’s another thing that they haven’t mentioned. If somebody moves towards comfort care, I would argue it could be perceived as euthanasia.
RECOMMENDED:
Julie: I agree.
Patrik: Right, right, because you’re potentially hastening death. Right? If people are in agreement with that, fair enough. If people are not in agreement with that, it’s euthanasia. Euthanasia is illegal in most countries, in most states. Right? So, you could argue they’re potentially moving towards an illegal action.
Julie: Okay, and we did said, “Well, you turning down the tracheostomy, the alternative is killing my mom.”
Patrik: And, what was their response?
Marvin: They didn’t like that.
Julie: Yeah, they didn’t like that. She said we’re not killing your mom. What did she say? I don’t even remember at that point. I don’t even remember what she said. She said, “It’s not … ” What’d she say?
Marvin: Something about it would happen either way is what I remember.
Julie: Yeah, she said, “Let me plant this little seed.” She said that comfort care is going to come up, or something like that. That’s what she said.
Patrik: Right, okay.
Julie: They’re like, “We’re trying to keep her comfortable, because the outcome is poor.”
Patrik: Yeah, yeah, yeah, I’ve heard it all before. Basically, what they are saying is, you know, they’re saying it’s in your mom’s best interest not to proceed with the tracheostomy. That’s what they’re basically saying.
RECOMMENDED:
Julie: Yeah.
Patrik: So, the ethical dilemma argument needs to be around your mom wants to fight until the end. That’s her belief. You know, and they have to be in a position to provide that, and that includes talking to other hospitals.
Julie: Yeah. Or, providing us some sort of proof that she’s in respiratory failure, and it will not get better.
Patrik: Correct, correct. But, if that … Okay, let’s put it that way. If that’s accurate, and they continue treating her, she will die. If their prediction is accurate, it means that no amount of treatment would reverse this condition, and she would die. That’s the bottom line. Because, that’s what they’re saying.
RECOMMENDED:
Julie: Religious.
Marvin: Oh, they’re medical then?
Julie: Oh, okay. So, right now, we have what was the most recent …
Marvin: This is the chest X-Ray.
Julie: So, the findings … Okay. Here’s the findings on the chest X-Ray. Life support tubes and lines are stable. Heart shows interval stability. There’s no significant pneumothorax, soft tissues and structures are unchanged.
Patrik: Okay. There is no talk about …There is no talk about end stage something, you know. If you can send me the image of that, that would be good, as well.
Julie: Yes, let me send you a picture, because I think that’s going to help. What was 10 days ago? So, they haven’t done the blood gas in 10 days.
Patrik: Yeah, that’s ridiculous. That’s ridiculous. The other thing that you need to do, as well, is because if you want to move down the track towards ethical issues, ethical dilemma, you will need to mention things like medical negligence. You will need to use stronger language.
RECOMMENDED:
Julie: What did you … I’m sorry, someone decided to come over here and play the piano, so we might need to move just a little. What did … Let me just … Did you get that picture there?
Patrik: No, not yet. Not yet. That’s okay.
Julie: This is today’s?
Marvin: Yeah, February 11th,
Julie: Okay, yeah. So, what were you saying?
Patrik: You will need to use stronger language. You will need to use words like medical negligence. You will need to continue …
Julie: Medical what?
Patrik: Medical negligence.
Julie: Medical negligence, okay.
Patrik: You will need to use things like, that if they stop treating your mom, that they’re killing her. Okay, you might even say that they’re murdering your mom. As I said, you will have to use stronger language. They need to get the message that you’re not giving up.
Julie: Okay. Well, we did say if the alternative is killing Mom, then we want a transfer, because we believe that she needs a tracheostomy in order to get better. We did say that today.
Patrik: Good, good, and you will need to be repetitive here, Julie. You will need to sound like broken records, okay? Because, they are used to people giving in. They’re used to that. You will need to be repetitive until they understand you will not give up.
RECOMMENDED:
Julie: Okay.
Patrik: You will need to …
Julie: So, who do I say this to? Do I go back in and tell the nurse right now that we are not going to give up, and how can I get evidence that you guys have called another doctor office? How do I say it? Do I just say that right to the nurse? Or, who do I say that to? The case manager?
Patrik: Well, so start with the nurse. But then, I would go to the case manager. I would go to Dr. Smith. Make sure you are very non … there can’t be any ambiguity around this. You need to be very clear in your expectations.
Julie: I don’t feel like we’re clear in … I mean, for the most part, we are very clear that we are not giving up. We did say that very clearly.
Patrik: Yeah.
Julie: We said, “Okay, if you feel that you have reached the point where you will not give her a tracheostomy, we need a transfer.” That’s what we said.
Patrik: Yeah. But, you got to go through that door of the ethical dilemma. You’ve got to use that.
Julie: Did you say go through the door, you said?
Patrik: Yeah, you need to use the ethical dilemma as an argument.
Julie: Okay. So, maybe my next thing is, I need to talk with the case manager on the phone and just say that, you know, we do not want to give up on her. And, I feel as though ethically, there’s a lot of things going on here that concern me, and I need evidence that you are working on the transfer.
RECOMMENDED:
Patrik: Yeah, absolutely. And, ask her how she will give you that evidence. Keep them accountable. Keep them accountable.
Julie: He said they have to be accountable.
Patrik: You have to …
Julie: Okay.
Patrik: You have to hold them accountable.
Julie: Okay. So, what is the … So, the nurse just said that they feel ethically that they would not be doing right to my mom if they put her through the surgery.
Patrik: Hang on, say that again, please.
Julie: So, they’re throwing the ethically, they don’t feel as though they would be doing right by my mom to put her through the surgery. They’re ethically saying that …
Patrik: Okay, yeah, yeah. Okay, yeah, and you will argue well, ethically, you are … Ethically, they are … What’s the word? They need to keep treating your mom, because it’s your wish. Okay, It’s your wish.
Julie: Okay.
Patrik: Right, you just got to keep pushing back for now. That’s all you got to do.
Julie: Okay. All right, so do I just call the case manager every day and just say, “What, how, who did you talk to at St. Mary’s Hospital?”
Patrik: I would approach this like who have you spoken to, today? Can she go tomorrow? I would just … You got to change your approach. You know, you got to, you need to set expectations.
RECOMMENDED:
Julie: So, who have you spoken to?
Patrik: You know, you need to go back to them and say, “Hey, who have you spoken to, today? Where’s the evidence? Can she leave tomorrow? Have you found a place so she can go tomorrow?” Take that expectation.
Julie: Okay. Okay. All right, so, and do that to the case manager?
Patrik: I would do it to all of them. Keep them on their toes. Keep them on their toes.
Julie: Okay, okay.
Patrik: And, if you can send me some pictures, that would be great.
Julie: Okay, I’ll send them again. Will you let me know if you get them? Because, I just sent the gas line?
Patrik: I haven’t received them yet. I haven’t received them yet.
Julie: Okay, so, I wonder if you’ll receive them once we get off the phone here.
Patrik: Could be, could be.
Julie: And, I’ll resend them.
Patrik: Yeah, please. Yeah.
Julie: And, I’ll have the monitor, the IV lines, and the ventilator. And then, I sent you the CAT Scan, and I sent you the gas line.
Patrik: Please, please, yeah. That would be great.
Julie: Okay, and then, if you want to send me those videos on the perspectives.
Patrik: Yeah, yeah, yeah.
Julie: And then, anything that you feel is important for me to say directly to the case manager. Like, I’m definitely going to go in there, so set my expectations in talking to everybody, instructing what we want for her.
RECOMMENDED:
Patrik: Yeah. And, you know, if she wanted me to talk to … You know, you need to touch base with this ethics department in this other hospital.
Julie: In the ethics departments, okay.
Patrik: You know, and you can, whatever you need, let me know and I can help you with that. Put in, to talk to them. You know, but touch base with them first.
Julie: Okay.
Patrik: And then, let me know what’s next.
Julie: Okay. Okay. So, and then, when do you recommend that I give you a call back?
Patrik: When you think it’s necessary.
Julie: Okay. Okay, and if they don’t get her … When does it become illegal if they haven’t been able to get the transfer going and everything? Because sadly, she’s not going to get better if they’re ethically keeping her on the vasopressors, you know. If they’re actively keeping her on the vasopressors.
Patrik: Agreed, agreed.
Julie: And so, you know, and there’s no way to prove any of that.
Patrik: No. Well, there could be. I mean, what we could start doing is, maybe not right now, I’ve got enough information for now. But, maybe tomorrow, I could talk to the nurse, just getting an update. Getting a better understanding of what’s exactly happening. Getting an understanding which information they’re potentially withholding from you.
Julie: Okay.
RECOMMENDED:
Patrik: Because, that would be …
Julie: So maybe, if you could talk to the nurse tomorrow?
Patrik: Yes, I think so. Because, let me talk to them. Let me get, like, a handover, almost. Because, you know, I want to talk to them and find out where’s the respiratory failure? Where is it? Show me?
Julie: Okay. Okay, yeah. Okay, all right.
Patrik: And so, and send me the pictures. I will send you some links to some interviews. And then, you give me a call when you need me next.
Julie: Okay, all right. Thank you.
Patrik: Okay, thank you so much. All the best for now. Thank you, bye.
Julie: Thank you very much.
Patrik: Thank you, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!