Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
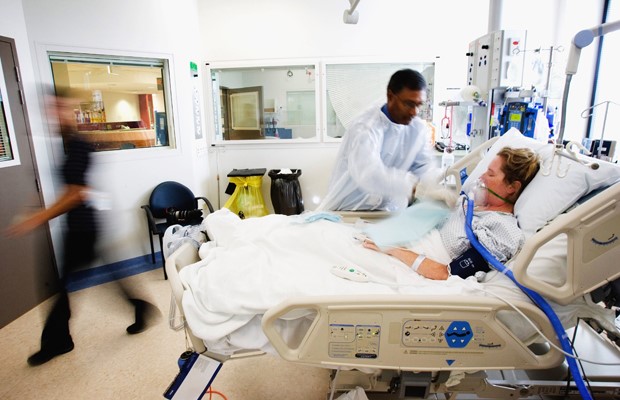
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU with sepsis, extubated but struggling to breathe. She is asking if she should take the risk of pushing her mom for another 24 hours of BIPAP to prevent re-intubation.
My Mom is Critically ill in the ICU and Extubated. Should I Take the Risk of Pushing my Mom for Another 24 hours of BiPAP to Avoid Re-intubation?
Patrik: To find the extubate. Right? If you’re choosing the wrong time, things like that can happen. By the same token, because it’s been 19 days, I argue they had to try. Right? Because otherwise 19 days is overstayed. She’s overstayed the 14 day mark, you know. And I’m glad they haven’t done a tracheostomy yet because you know, you always want to try first.
Julie: Yes. So, will they continue to try? Because after she gave me the speech… But you’re saying, Hey, you know the speech is because she’s giving me worst-case scenario again, right?
Patrik: Yeah, absolutely. She will give you the worst-case scenario. Let me ask you this. With the bowel, with the ischemic bowels and the ischemic gut last week, has she been fed? Has she been getting nutrition?
Julie: So, they… She they were starting with Total Parental Nutrition (TPN)
Patrik: She was getting TPN?
Julie: Yes. And then recently, like three days ago, she had a large bowel movement. They said like a very hard stool that was kind of like a flood came out, and then she continued to have very, very large bowel movements after that. And so they said that it was no longer an ischemic bowel and that it’s been resolved.
Patrik: Okay, well I’m glad. I’m glad to hear that she’s getting TPN. Right?
Julie: Yeah. And then, well after the bowel happened, they started giving her 10 ml of the food again.
Patrik: 10 ml of?
Julie: Of the, you know, the vital care stuff through the intubation.
Patrik: Yeah. Yeah. Understood.
Julie: So very light feeding. They started very light feedings because of the stool. So, she was getting TPN and 10 ml of food.
Patrik: Okay, excellent. That’s good. That’s good. That’s excellent. So, you know, there’s two things there, Julie. Number one, a critical illness and an induced coma obviously is weakening a patient severely. So your mom would have been severely weakened by, you know, just the critical illness. Then, number two, you’ve got the added on issue of probably not getting adequate nutrition for a few days? Right. I don’t know whether they started the TPN straight away. Do you remember? Do you know?
Julie: She’s been been on the TPN, yeah, for quite a while. So they waited two days for the septic shock and for her to move a little bit. And then they instantly started the BiPAP, or I mean the… Sorry, the TPN. Because they said they were trying to see if they could get her on regular nutrition.
RECOMMENDED:
Patrik: Yeah, yeah. So, you understand the mechanics then, and as I said, without having seen the chest X-ray, if you are telling me, if they turned her on her side and she basically decompensated. Right? There is a very high chance that one side of the lungs is worse than the other.
Julie: Okay.
Patrik: Right? So she might have a pneumonia, and the left side might be worse than the right side. So, let’s just say for argument’s sake, the left side is having a pneumonia and the right side is clear. Okay? And if they turn your mother on her right side and that’s the better side, that’s less air entry because of just because of, you know, mechanics. Okay? And then you’ve got the left side that’s got a pneumonia. No air’s going in.
Julie: Okay.
Patrik: Right? So that, I can almost say, as I said to you, you know, because that’s what happens. That’s what happens.
Julie: Okay. So, but they turned her back and they started giving her a nebulizer treatment, saturation was 90% but the heart rate still stayed up.
Patrik: Yeah, but the heart rate… Look. The heart rate is like, you know, she’s probably finding it hard to breathe. Right? And the heart is trying to-
Julie: Yes.
Patrik: The heart is trying to compensate with a higher heart rate to pump oxygen around the body. It’s just a compensation mechanism.
Julie: So what’s her best interests right now then? Because we don’t want her to aspirate, but should we let her get reintubated so she can get weaker and weaker and weaker?
Patrik: Look, I feel that way because that will save her life in the short run. Okay? It’s a very fine line. You know, if we knew that another 24 hour of BiPAP would help her to get through this, I would say, “Yup, let’s do the BiPAP for another 24 hours.” You’ve got the risk of aspiration. You know, you’ve got the risk of discomfort. You know that’s-
RECOMMENDED:
Julie: If she’s able to keep her oxygen saturated at 90 or above, is it still a risk to leave her up at the high heart rate for the aspiration and the… throwing up?
Patrik: Definitely, definitely. However, there is another thing, Julie. Her oxygen levels might be okay. Okay? Her oxygen levels might be okay. However, her the carbon dioxide levels might not be okay.
Julie: Okay. Well they did test that. They just tested that. Prior to, I don’t know when they tested it, actually. I’m going to find out though.
Patrik: I’ll tell you. I tell you when they tested it, they would have tested it with an arterial blood gas. It’s the part of the test. That’s why I said to you earlier, do you know the blood gas results?
Julie: I will in just a little bit when I arrive. Is there anything else I should know so… So you don’t think I should be too worried about the intubation, because that’s scaring me the most right now.
Patrik: It’s scaring me too, you know. Every time you’re extubating a patient and it fails, there’s two reasons for failing. Right? The first one is they didn’t choose the right time. Okay, that’s number one. So, that that judgement is potentially, you know, not correct. That’s number one. Or, number two, she just won’t be ready and they needed to try it anyway to get a feel for what, what she’s up to.
Patrik: Okay? And then determine the next steps and also give her the chance on the BiPAP. I think it’s good that they’re doing that, you know, because she stayed 19 day, 20… It’s time that, you know, they wanted to see what she’s doing. And I agree with that, generally speaking. But you see, if she’s potentially not a candidate for a tracheostomy, let’s just say that’s the case. Okay? Let’s just say she can’t have a tracheostomy for the reasons they told you. Then I’m almost bound to say let’s push on with the BiPAP for another 24 hours with all the risks that we know. Right? And in order to give her a chance to stay off that ventilator, you know. To stay off the breathing tube. It’s a very fine line, Julie. It’s a very fine line.
RECOMMENDED:
Julie: So, but let me ask you this. For the last five days they’ve been doing breathing trials. In the breathing trials my mom has been off all sedation, all pain meds and she’s been doing four hours plus with nothing, with no help. Breathing through a little tiny straw, coughing. And she did very, very well.
Patrik: Yep. So…
Julie: So why now that you pull the tiny little straw she was breathing out of, without oxygen… Why…. I don’t understand.
Patrik: Yep. So, here is what I would want to know. So let’s just say… Let’s pretend I was the bedside nurse looking after your mom. Okay? Let’s just say I was the bedside nurse looking after your mom and I could see she was doing that. You know, she was doing all the breathing trials. She was doing well. You know, there’s a number of things that I would still want to know. Number one, I would want to know what are the arterial blood gas on the breathing trial. Okay? I assume they must have been good, otherwise they wouldn’t have decided for extubation. Okay?
Julie: Yeah. She was doing… She was at 40% and at 5 PEEP.
Patrik: Okay. So she was on 40% of oxygen?
Julie: Yeah, on the ventilator it was 40% was what the ventilator was doing and five PEEP.
Patrik: Okay. I tell you that if she was on 40% of oxygen, that’s too high. That’s too high for extubation.
Julie: Oh.
Patrik: It should be 35% or less. You can extubate on 40% but it’s tricky. Borderline. Borderline. The other thing Julie, that could have simply happened is, the numbers looked good. You know the numbers looked good, and the breathing trials were going fine and for whatever reason overnight she might have had, she might have had, an abnormal aspirate, or she might have had… No, she might’ve developed another pneumonia. You know?
Julie: So you can get, you can get another pneumonia on top of a pneumonia?
Patrik: Have you heard of ventilator-associated pneumonia (VAP)? Have you heard of that?
Julie: No.
Patrik: No, that’s okay. I’ll tell you what I’ll do when we come off this call. I’ve got some articles on my website that I’ll send you a link to, that talks about ventilator-associated pneumonia. It also talks about when a patient is ready for extubation. So I’ll send you some articles today. You can have a… You know, that gives you just a little bit more explanation to what we already spoke about. Right?
Patrik: It’s a tricky one. Julie, your mom, you know, is sort of sitting on the cusp in terms of, you know… So, but yeah, if she’s not a candidate for a tracheostomy and I doubt that. As long as an ENT specialist hasn’t given their opinion, I doubt it. Okay?
RECOMMENDED:
Julie: Okay.
Patrik: I believe you would want to see an opinion from an ENT, from an ear, nose and throat specialist. They would be the specialist to determine whether your mom could have a tracheostomy or not. But let’s just look at the worst-case scenario. Let’s just say your mom isn’t a candidate at all for a tracheostomy. Okay? I would almost be in favour of taking the risk and pushing for another 24 hours of BiPAP., if she could tolerate it. Right? To avoid reintubation. If your mom can have a tracheostomy, I would say let’s intubate and not take a risk.
Julie: Now, if you intubate, the next step is tracheostomy. There is no…
Patrik: Look. No, no. Look, there could be. But I’d say after 20 days of ventilation with a breathing tube, chances are slimmer and slimmer.
Julie: Okay.
Patrik: Right?
Julie: Yeah. So then with the extubation, we’re putting her on a ventilator for the rest of her life?
Patrik: Say that again, please?
Julie: With the extubation, we’re planning on a stomach tube to feed her, and a ventilator for the rest of her life?
Patrik: The ventilator for the rest of her life would only be an option if she can tolerate a tracheostomy. Ventilation for the rest of her life with a breathing tube is not an option. Not an option.
Julie: No. No. And I don’t even want that as an option. I don’t even want the tracheostomy then ventilation as an option. So, there’s no way that how good she was doing that we could possibly do a tracheotomy that’s temporary?
RECOMMENDED:
Patrik: Oh. A tracheostomy should always be temporary. Should always be temporary.
Julie: Because the way they’re saying it… So, they were talking about a tracheostomy on a ventilator for the rest of her life.
Patrik: Yeah. Remember, remember Julie, worst-case scenario, they’re always painting the worst-case scenario. Always.
Julie: So, if she is a candidate, she does intubation tonight, she gets the GI specialist, they put in a tracheotomy that is buying us time to rebuild strength. Are we actually rebuilding strength at that time.
Patrik: You’d hope so. You would hope so. You see one, one of the main advantages with the tracheostomy is, so you remember when you have a breathing tube, most of the time you need to go into an induced coma. Okay? That’s… one of the reasons you’re going in an induced coma with a breathing tube is simply because you can’t really tolerate a breathing tube. It’s so uncomfortable. Okay? So, that’s the main reason why people go into an induced coma with a breathing tube.
Julie: And that’s just to get the tube?
Patrik: Pardon?
Julie: That’s just to get the tube?
Patrik: That is not so. In other words-
Julie: She came off of all…
Patrik: Yeah, yeah, I know, I understand.
Julie: She’s been off of all-
Patrik: Yeah, I understand. And that’s normal because, before you extubate, you need to be able to be off everything. But, in the beginning you need to be in an induced coma. Where I’m going with this, Julie, is have you seen as tracheostomy, do you know what it looks like?
RECOMMENDED:
Julie: I’ve seen it on the scary commercials where the guy that had been smoking had it and kind of talks funny or whatever.
Patrik: Sure, I’m sure.
Julie: And is in a wheelchair and it’s like, don’t smoke. That’s all I’ve ever seen or even know of it.
Patrik: Fair enough. Fair enough. So the good news, besides the scary part that you’ve seen, you know, on TV commercials or whatever the good news about a tracheostomy is, as soon as you have a tracheostomy you can be off sedation. It doesn’t, you know, it’s not painful. It’s easy to tolerate compared to a breathing tube, it’s a walk in the park.
Julie: Oh wow. Okay. So that’s great.
Patrik: Okay? So that’s good. Right? So compared to a breathing tube, they can switch off sedation straightaway, once a tracheostomy has been done.
Julie: And then can they also, can they also feed you or how does that work?
Patrik: Yeah, they can feed you. They can feed you. At the moment your mom would still have a nasogastric tube?
Julie: At the moment?
Patrik: Yes.
Julie: At the moment she had a tube in through the intubation. I don’t know… since they did extubation I don’t know what else she would have.
Patrik: She would have. She would have another tube through her nose, for feeding. She would have that. She would have that. So she could be fed-
Julie: Okay and so when they say that that they would have to go through her stomach if they do a tracheotomy. Is that worst-case scenario too, because they don’t do through the nose.
Patrik: That is worst-case scenario and I’ll tell you why. It’s very much also a thing in your country that when they do a tracheostomy that they also do a PEG tube, which is the tube through the stomach for feeding, it goes hand in hand. Whereas in other countries it doesn’t go hand in hand. My preferred option is not to do a PEG and just continue with a feeding tube through the nose.
RECOMMENDED:
Julie: Okay. Because she said something about the mucus membranes are really sensitive and they can’t tolerate it or something like that. I don’t know. So, I’m here at the hospital now. What, what, what can I get you to… or what do you want pictures of anything? Or…
Patrik: Yes please. Please send me a picture of the ventilator. Please send me a picture of the monitor. Please send me an arterial blood gas. If you send me anything please send me an arterial blood gas. If you send me anything, please send me an arterial blood gas.
Julie: And the result of the chest X-ray and I’ll see if they’ve taken one since then.
Patrik: Yeah. Yeah. And I’m very happy when you’re there. I will, I’m very happy to get on the phone with whoever is there.
Julie: Okay. Because my… Okay, so I think the nurse is going to be in there. Maybe they can just kind of give you an update. Hopefully she’s not intubated and a miracle happened on my way up here. But, I will send you pictures of everything in the blood gas and the results of the X-ray and give you an update via a text message in just a second here.
Patrik: Please.
Julie: Okay. Thank you so much.
Patrik: You’re very welcome. You’re very welcome. I’ll wait to hear from you. Thanks. Bye.
Julie: Oh, and you’re going to send me some stuff, you know, right?
RECOMMENDED:
Patrik: I’ll send you some links to articles that are relevant. I’ll text them to you.
Julie: Okay. For the pneumonia.
Patrik: For the ventilator-associated pneumonia (VAP). And I’ll also send you a text about when a patient is ready for extubation.
Julie: Okay. I appreciate it. Thank you so much.
Patrik: You’re very welcome. All the best for now. Thanks.
Julie: Okay. Thanks. Bye-bye
Patrik: Thanks. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!