Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
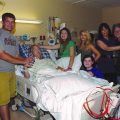
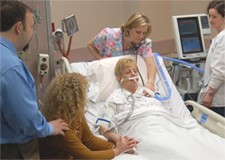
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my client Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU with sepsis and has a breathing tube. Julie is planning to move her to another hospital and she is asking if it will be risky for her mom to be transferred.
My Mom is in the ICU and Has a Breathing Tube in Place. Is it Risky to Transfer Her to Another Hospital While in Critical Condition?
Julie: So, it says… These are the things I think she’s on. It says A is P-H-E-N-Y-L-E-P-H-R-I-N-E. That’s at 80.
Patrik: Epinephrine
Julie: Okay. That’s at 80 mcg.
Patrik: Okay, yep.
Julie: Then she’s on IV maintenance, and she’s Vasopressin at 0.04. And, then she’s on Total Parenteral Nutrition (TPN)
Patrik: TPN yeah.
Julie: And then she’s on D-E-X-M-E-D-E-T-O-M-I-D-I-N-E
Patrik: Can you say that last one again. V?
Julie: D as in dog, and then E-X-M-E, D as in dog, E-T-O-M-I-D-I-N-E.
Patrik: Oh, that’s Precedex. That’s Precedex.
Julie: Okay. She’s on 0.6 of the Precedex.
Patrik: Okay, so they… And she would probably be on a little bit of Fentanyl as well. Do you know that?
Julie: This is everything she’s on I think.
Patrik: She’s on, okay.
Julie: Let me just ask if she’s on the Fentanyl. Fentanyl, let’s see. Let’s see, Fentanyl. Okay, and then he also sent me the arterial blood gases, so let’s look at that. So today is … So they took it on January 22nd, January 23rd and January 11th. How do you know?
Patrik: It’s probably right on-
Julie: It says 7.36 and 7.34. Does that sound right?
RECOMMENDED:
Patrik: It does, but it’s irrelevant because it’s so long back. If it was in January, it’s really irrelevant. I would like to see a blood gas-
Julie: Can you?
Patrik: I would like to see a blood gas from today or from yesterday. What happened in January is, as far as the blood gases are concerned, it’s irrelevant what they looked like in January.
Julie: Well, this is February. The February 11th, 2019. So, it’s 7.36 and then they did it again a couple of hours later and it was … Well, 23:00. So, what would that be? Minus 12 right? Is that how you do that?
Patrik: Yeah, roughly.
Julie: Or you add?
Patrik: Yep, that’s okay.
Julie: The last one they took was 7.34 and that was on the 11th.
Patrik: Yep, that doesn’t mean anything. That’s just the pH. You get from a blood gas, you get what… The most important numbers to look at in a blood gas is the PO2 the oxygen and the CO2 the carbon dioxide. They’re the most important numbers. Only with those numbers does the pH make sense. The number with the seven, 7.36 is the pH. It only makes sense if I have the PO2 and the CO2.
Julie: Well, there’s more numbers under it. There’s…
Patrik: Keep reading them out.
Julie: The PCO2, 41 last night and 44 today, the PO2, wait PC02, was 41, and the PO2 was 65 and 95.
Patrik: Okay, now we can stop there. That’s all I need. That’s all I need.
Julie: Okay.
Patrik: So, PCO2 is normal, just about. The normal range for PCO2 is 35 to 45. So, that’s normal. The PO2 is normal too. 65 is just about the lower limit, so it’s just about border line, but 95 is fine.
Julie: Okay.
RECOMMENDED:
Patrik: Okay. Do you know whether the first numbers, the CO2 41 and the PO2 65, do you know whether that was before intubation? Do you know that?
Julie: I believe one of them was after, one was before. So she got extubated and they took one, and then she got re-intubated and they took one.
Patrik: So that means the first one would be on extubation and that’s just about all right. But then the next one looks good, but that’s on a ventilator.
Julie: Yeah. So, it has a whole breakdown, and I can send you that screen too. She is on Fentanyl. She’s on 10 mcg of Fentanyl.
Patrik: Okay, that’s minimal. That’s minimal.
Julie: Okay.
Patrik: You talked about your mom earlier, you talked about your mom being overweight. What are we looking at in terms of weight, roughly?
Julie: Oh, 113 kg, so what is that?
Patrik: I like kilogram. I know what that means. I know what that means. I would struggle with any other measure. I’m good with kilogram. That is overweight, but it’s not like … It’s probably a little bit too much but… And what height, what height are we looking at roughly?
Julie: 5’6″.
Patrik: Okay. So it’s not… She’s not like… That’s not too bad I mean there’s other … You know, overweight would be 150 kilos.
Julie: Yeah. No, she’s at 113, and they just weighed her so that was her most recent was weight was 113.
RECOMMENDED:
Patrik: Did you see the text that I sent you yesterday about ventilator associated pneumonia? Did you read that?
Julie: I did.
Patrik: So, you would have seen that the longer you’re on a ventilator, the higher the risk for ventilator associated pneumonia and also a tracheostomy, it’s a safer option for ventilation. It’s just safer.
Julie: Okay.
Patrik: The next step I believe is, they need to find … I tell you what I think needs to happen. They need to find out why she decompensated. They need to find out why she couldn’t stay off the ventilator. So, if she’s on 65% of oxygen … Yeah, go on.
Julie: No, I didn’t say anything.
Patrik: Oh, okay. There’s a very good chance that she’s developing some sort of pneumonia again, otherwise she wouldn’t have gone up to 65%, right? So, hopefully they send a sputum sample. I really hope that’s happened. Right?
Julie: Okay.
Patrik: The blood results will be important because the white cell count might show a picture, especially if she’s got a temperature. Right?
Julie: Yes.
Patrik: But they also would have to do a… Have you heard of blood cultures? Have you heard of that?
Julie: No.
Patrik: Yeah. So, they need to send blood cultures. Basically what it means is they need to take a sample of blood from the central line. Because she’s on the Vasopressin and the Phenylephrine, she would have a central line. So, they can take blood from the central line, and they need to test the blood for any blood stream infection. They need to do that.
Julie: They might, they did do that when she developed sepsis for sure, and they also did it in both arms.
Patrik: Yes. Do you know whether that’s happened in the last 24 hours?
Julie: I don’t. Let me ask. So, it’s called a blood culture, right?
Patrik: Blood culture, yeah.
RECOMMENDED:
Julie: I feel like they’re kind of at a standstill right now because of how weak she is. So they don’t feel that because they took an x-ray this morning and it shows minimal pneumonia, they feel as though everything that is happening is a product of her weakness, her overall big picture, and they’ve almost stopped treating her. Could the blood infection or the blood clot … Could a blood clot cause fevers and the things, kind of stuff to?
Patrik: It could, it could. It’s less likely compared to a simple infection causing a temperature. You know, it’s less likely.
Julie: Okay. She is getting fed again. They’re back to giving her the 10 mL in the feed and the TPN. We talked to the Infection Disease doctor today. That they don’t do blood cultures regularly after they have taken a culture that showed no growth unless signs present again that she is fighting an infection, which is elevated white cell count.
Patrik: Yeah, which is what I said. We need the white cell count.
Julie: Let me ask about that.
Patrik: Yes.
Julie: Let me ask what that is. So, what are your thoughts going forward? I mean, what kind of demands should I be putting in place? Should I be moving her? Should I say, “Hey, stop the…” Because how serious it of a blood clot in your arm, if you’ve just come off the blood clot medications to do the surgery. Heal from the surgery and go back on the blood… Is a blood clot in your arm, is that pretty severe?
Patrik: I wouldn’t say it’s severe. It’s a concern, but I wouldn’t say it’s severe. It’s definitely a concern and it’s showing that whatever they’ve done, they haven’t prevented it. Right? That’s simply not good enough. It’s their job to prevent things like that. The minute somebody becomes immobile the risks for a blood clot is huge.
Julie: We have been telling them since Saturday that her hand is swollen and that the blood pressure cuff was too tight. Could that cause it, the blood pressure cuff?
RECOMMENDED:
Patrik: Definitely, definitely. And here is the thing, Julie. If she had an arterial line, she wouldn’t need a blood pressure cuff. Because, I’ll tell you why. With an arterial line, you’re doing two things with an arterial line. Number one is you are able to check arterial blood gases and number two, you are able to get the blood pressure from the arterial line.
Julie: Wow. Wow.
Patrik: Right. So, the first pictures you sent me last week, she had an arterial line, right? I could see it in the monitor. Hang on.
Julie: We asked them-
Patrik: Hang on, hang on, hang on. Just give me one second. Hang on. Hang on. Just give me one sec that I’m telling you the right thing. Don’t want to make up things that are not accurate. No, no she didn’t have an arterial line. No, no. She didn’t.
Julie: Yeah, she didn’t.
Patrik: Yeah. So, you mentioned that there’s the potential for going to a hospital up the road. The hospital up the road, is in that a teaching hospital? A big teaching hospital?
RECOMMENDED:
Julie: I don’t know if it’s a teaching hospital. Let me ask.
Patrik: Because I think that’s important.
Julie: Did you see, when you looked up West Valley Hospital. Is it a teaching hospital?
Patrik: Not that I can see. Not that I can see. I don’t think it’s a teaching hospital. I can’t see any indication that it’s a teaching hospital.
Julie: So, do you think… I mean, how invasive is it to move somebody on intubation that’s this critical and wait that 24 to 48 hours? Are we looking at, you know, yes it is necessary because the help we could get at a bigger, teaching hospital is going to be a make it or break it situation?
Patrik: Yeah. I’ll tell you my thoughts around this. If the other hospital is less than half an hour away, it’s not a big deal. Right? At the same token, it’s like, you don’t want to take a risk either if it’s not necessary. However, given what’s happening there it might be the best thing to do. And as you said, a fresh pair of eyes can help. Your mom is young. Your mom is, did you say 56?
Julie: 55, yeah.
Patrik: Oh my goodness, she’s very young.
Julie: Yeah, she is. She is young and she’s actually very strong. And I’m telling you right now, her being bed-ridden, she only went to a nursing home, I don’t even think it’s been two years. It’s almost two years. But, prior to her going to the nursing home, she was changing herself, you know. Using a bed-side toilet. You know, when she arrived at the nursing home she was using a stand assist, which they said they have to be able to use 80% of your legs to do the stand assist. So, her weakness is coming from her saying, “No, I’d rather be in my bed and being stubborn.” Maybe a little bit of depression.
Julie: So when she arrived there, we’re not talking like somebody who’s just… I mean she was able pull herself up in a wheelchair; push herself in a wheelchair, you know, feed herself still. She’s still very capable of these things. I don’t know why they keep saying, “Well your mom was weak upon arrival and she’s been very weak because she allowed herself to gain all this weight and not get out of her bed for so long.”
Patrik: They’re saying that in order to cement the idea of that it’s the worst case scenario. You really need to ignore that because your mom. They don’t know your mom. They just look at her and think, “Oh she’s been in a nursing home prior to that, it’s probably pretty bad.” That’s the way they would look at it. You’ve got to turn a blind eye on that for now. It’s not going to help.
Julie: Okay, okay.
Patrik: With this other hospital that you’re thinking about. What’s the hospital’s name?
Julie: West Valley Hospital
Patrik: West Valley?
Julie: Yeah.
Patrik: Yeah, yeah.
Julie: So they said that that arterial line goes into a femoral artery in the leg and goes all the way up to her heart.
Patrik: What?
RECOMMENDED:
Julie: They said that the gas, that the arterial gas line goes into her femoral artery in her leg and goes all the way up to her heart.
Patrik: Okay, so she does have an arterial line.
Julie: Huh?
Patrik: So she does have an arterial line.
Julie: No. No, she does not. He is down there telling them that we would like to have one.
Patrik: Good.
Julie: And they said it’s super invasive because it’s going to be going through an artery in her leg all the way up to her heart.
Patrik: What I’ll do as well, Julie, is I’ll send you some information around arterial lines. Yes, it is correct that they might do the arterial line in her femoral artery, that is correct. That’s one of the locations where they can do it. I mean you’ve seen the wrist. They can put an arterial line into the wrist, or they can put it into the femoral artery in her thigh, sort of up her thigh. Those two options you have, generally speaking.
Julie: Okay.
Patrik: But it’s not even a here or there. I mean, as I said, look, I’ve worked around the world and I’ve worked in at least seven or eight ICU’s over the years. I’ve never worked anywhere where you ventilate a patient without an arterial line. I just haven’t seen that. I just haven’t.
Julie: Now, does it go up to her heart or it just…
RECOMMENDED:
Patrik: No, no, no, no. It just sticks in the artery, that’s all. That’s all it does. I will send you some information, I mean this is just … I would be very happy to talk to them because this is just-
Julie: I’m not there.
Patrik: Yeah, yeah. Sure. This is just ridiculous.
Julie: Yeah. I’m just saying you could call him. You could call him, he is there. But her white blood cell count is 7.2.
Patrik: That’s normal. That’s normal. But then, in the early stages of infection not all the lights are on, you know?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recording and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!