Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
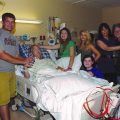
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU with a breathing tube in place and on blood pressure medications. Marvin (Julie’s husband) is asking regarding the importance of arterial line for their mom.
My Mom is Critically Ill in the ICU with Sepsis. How Can My Mom Be in the ICU Ventilated and on Vasopressors for Three (3) Weeks Without an Arterial Line?
Patrik: Patrik speaking. How can I help?
Marvin: Hi Patrik, it’s Marvin. How are you doing, buddy?
Patrik: Very good, thank you. How are you?
Marvin: Oh, pretty good. I’m walking into the hospital right now. I just wanted to get down the line. It’s a little easier to put him on the spot that way, I feel like.
Patrik: Yes.
Marvin: Instead of, hold on, let me call him.
Patrik: Yeah. Yeah. Are you expecting him to be there now?
Marvin: Yes, they called me and told me he was here.
Patrik: Oh, I see, I see. Okay. And what is… He’s the pulmonologist. Is this the guy that I spoke to a while back?
Marvin: Yes.
Patrik: Right. What was his name again?
Marvin: Dr. Smith
Patrik: Yes, that’s right. That’s right. And he’s the pulmonologist and he’s basically in charge of Julie’s mom’s care. What’s her name, by the way?
Marvin: Yeah, she’s… The patient’s name?
Patrik: Yeah, the patient’s name, so I can refer back to him as well with the patient’s name.
Marvin: It’s Roselyn Jefferson.
Patrik: How do you say the first name?
RECOMMENDED:
Marvin: Roselyn.
Patrik: Oh, Roselyn.
Marvin: Like the flower.
Patrik: Okay. Yeah. Yeah. Okay. Okay. Yep. Okay. And what has happened? Has anything happened? So I spoke to Julie yesterday. What has happened between now and when I last spoke to Julie? Do you know whether there have been any changes?
Marvin: They wouldn’t speak to us over the phone about it.
Patrik: That’s really inappropriate.
Marvin: And said that the doctor wanted to speak to us himself. Kind of like in person.
Patrik: Okay. Okay. So when you’re going up there now, are you the only family member who’s there or are there other family members there as well?
Marvin: Right now it’s just me.
Patrik: Okay. And since I last spoke to Julie, there haven’t been any other family members around in the hospital?
Marvin: Not that I’m aware of.
Patrik: Okay. So you are basically now getting the first update. It would be really good when I talk to him if it was on loudspeaker so you can actually hear what I’m saying. I don’t know whether that’s an option or not, but I think the more you can hear what I’m saying the better it is.
Marvin: Oh, like if I put you on speaker?
RECOMMENDED:
Patrik: Yeah, absolutely. Or what I can do, if you want that, when I talk to him, I can also record the chat. I mean, he doesn’t need to know, I can record that and then I can email it to you.
Marvin: I was looking into that as well. Downloading something on my phone to be able to do that.
Patrik: Yeah, I can do that from my end. It’s not a problem. Sometimes one side disappears, the recording, but nine times out of 10 it’s fine. So that’s what I would suggest. If you’re okay with that, he doesn’t need to know but… Especially if you’re…
Marvin: For our information.
Patrik: Exactly. Exactly. Especially if you can’t hear what I’m saying.
Marvin: Okay. Yeah, I like that.
Patrik: I think that’s a good idea.
Marvin: Me too.
Patrik: And just to summarise, so they re-intubated her yesterday morning?
Marvin: Hold on. No, it was Monday night.
Patrik: Okay. So they re-intubated her Monday night. From what I understand, they had to call the senior doctor in. They didn’t have anybody there who was able to re-intubate her. Is that correct?
Marvin: They called in the same doctor. Dr. Smith. He did the intubation
Patrik: Right. You see, here is a concern in my mind. If they have to call a senior doctor in to re-intubate, it’s telling me that the skill level on the ground is pretty skim. Do you know what I mean by that?
Marvin: They are understaffed.
RECOMMENDED:
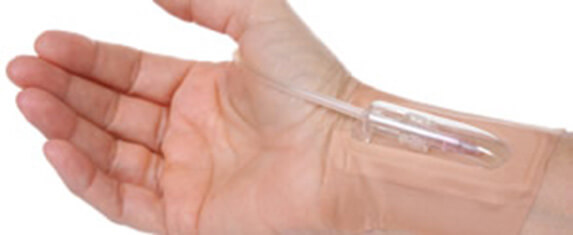
Patrik: That’s right. There should be somebody there who can intubate at any time. Right? That’s number one. Number two, yesterday when Julie reiterated that she hasn’t had an arterial line basically since admission, it makes me wonder, again, it comes back to a skill level. Do they not have anyone who can put in an arterial line?
Patrik: Right?
Marvin: I would think they would.
Patrik: Yeah. Yeah. That’s what I would think too. They’re in ICU. But given those two issues, I am wondering who are the people on the ground when he’s not around?
Marvin: Oh yeah. I asked that question last night.
Patrik: Right. What was the answer-
Marvin: And when he’s not here they don’t have a doctor on the floor in the ICU, but they have what they call a hospitalist.
Patrik: Oh my goodness.
Marvin: That is in the hospital at all times that they could call, that’s what their answer was.
Patrik: Yeah, so that’s the problem. So that’s the problem. As soon as he leaves, that’s it. He’s the big player there and he’s got no backup.
Marvin: Oh yeah. At that’s point it’s just-
Patrik: That’s the problem.
Marvin: The nurses often make all the decisions or a call.
Patrik: That’s right. That’s right. Okay. That sheds more light on it and it also then cements almost the argument that she needs to go somewhere else.
Patrik: Do you want me-
Marvin: That would be cool.
Patrik: It’s up to you. Do you want me, when I talk to him, do you want me to mention to him that’s what we’re thinking about or do you want me to leave that out for now? What do you think?
Marvin: No, we are thinking about that. We actually, we’re leaning pretty heavily towards wanting to be able to do that.
RECOMMENDED:
Patrik: Okay. Do you want me to mention that to him or not?
Marvin: Yes.
Patrik: I think so. I think so too, because he needs to know that we’re watching. He needs to know that we’re watching.
Marvin: Yeah. I agree.
Patrik: So basically he’s the big guy there, there’s no back up. What happens? He can’t be there 24 hours a day. I mean, there must be a rotating roster. There must be somebody else when he has the day off or something like that.
Marvin: Yeah, I think they have a couple doctors that rotate through but the big one that’s been on her case was him.
Patrik: Sure, sure. Okay. Okay. And things like, when I spoke to Julie yesterday, do you know whether the assessment was happening?
Marvin: I don’t know. They wouldn’t give us any information today over the phone and said that he wanted to talk to us.
RECOMMENDED:
Patrik: That’s ridiculous.
Marvin: To tell us everything that’s going on.
Patrik: Right, right. Look, from my perspective, there are three top questions that we need to ask today. Three top questions. Number one is, what’s the current status, of course. The next, and I’ll just make a note there. The next, I want to get an idea about what she’s up to. The next question to me is, how can she be in ICU ventilated for three weeks without an arterial line. But it’s not only the ventilation side of things, it’s also the blood pressure medications like, she’s been on the phenylephrine and the vasopressin and in the past she’s also been on norepinephrine.
Patrik: It’s imperative that whenever somebody is ventilated and has the vasopressors, needs to have an arterial line. I have never seen that. I’ve never seen that. I might’ve seen it for 24 hours.
Marvin: It’s kind of crazy.
Patrik: That’s crazy. I might’ve seen it for 24 hours, if it’s really busy, but not for three weeks.
Marvin: Yeah, I agree.
Patrik: The other thing is-
Marvin: And I’ve mentioned it multiple times and they always kind of…
Patrik: Yeah, and it’s time that-
Marvin: They baulk at it.
Patrik: Yeah. And it’s fine that he has become a clinician, right, because I will have all the right questions for him and then I want to hear what he says. I want to hear what he says when I tell him, look, in 20 years ICU, I’ve never seen this. I want to hear what he has to say.
Patrik: And also the-
Marvin: I do too.
Patrik: Right, exactly. The other issue is, they extubated her on 40% of oxygen, from what I understand from Julie. Now extubation on 40% of oxygen is really risky. I have rarely seen it succeed. I do believe sort of 40% of oxygen is… Usually extubation is done on 35% or less.
RECOMMENDED:
Marvin: And I would say here probably less because we’re also at altitude.
Patrik: Right. Well, what do you…
Marvin: We’re 6,000 feet above sea level here.
Patrik: Oh.
Marvin: So we’re not dealing with normal oxygen levels to start with.
Patrik: Right. Whereabouts are you, in South Carolina?
Marvin: Yes.
Patrik: Right.
Marvin: We’re actually in Williamsburg at this hospital, but it’s part of the South Carolina area and I think it is 6,000 feet, so.
Patrik: Yeah, right. I see. Okay. Yeah, sure, sure. But then, that would only impact on room air, really. Room air is 21% and you would be not having 21%, but if you’re giving 40% with via oxygen, via the ventilator, you should get 40% oxygen. But anyway, I hear what you’re saying.
Marvin: Well, no, no. I mean when you pull off, it’s an even bigger jump at that point. That’s my point.
Patrik: Sure, sure. No, no, that’s a valid point. And then obviously I want to know about the ENT assessment, because it sounded to me like that was taken off the… That was not an option 24 hours ago and then I believe it is now an option again and it needs to be an option.
Marvin: Well they had contacted an ENT yesterday to come in and consult and he had never made it down yesterday. I guess he was supposed to come in this morning.
Patrik: Right. Okay.
Marvin: And what Julie heard from them was that the ENT and Dr. Smith spoke and then they didn’t elaborate any further. And that Dr. Smith wanted to speak to us.
Patrik: Right.
Marvin: That’s basically where we got on everything. So pretty much everything is status from last night when we talked to Julie.
RECOMMENDED:
Patrik: Yeah, no, not that is-
Marvin: The status is pretty much status quo.
Patrik: Yeah. Okay. No, no, that’s good. And that’s what I needed to know because when I do talk to him, obviously one needed to know whether anything has changed, and if anything has changed he might fill me in hopefully.
Marvin: Yeah, anything changed or did happen. We are completely in the dark on right now until he gives us an update.
Patrik: That’s so inappropriate. I mean, basically what you’re saying is you can’t even ring the bedside nurse and get an update there.
Marvin: Not today.
Patrik: That’s inappropriate.
Marvin: Usually yes.
Patrik: But not-
Marvin: But today, no.
Patrik: I’m very wary of that, very wary of that.
Marvin: Yeah, me too. Because usually when they do that kind of stuff, they’re not coming to you with anything good.
Patrik: That’s right. What do they have to hide? What do they have to hide that they can’t discuss over the phone?
Marvin: Yeah, exactly.
Patrik: So, okay. So yeah, look, I think that’s enough information for now.
Marvin: Okay.
Patrik: If you can get him on the phone, get him on the phone.
RECOMMENDED:
Marvin: Okay. Yeah. Do you want me to keep you on the phone or just give you a call back in a minute?
Patrik: Just give me a call back.
Marvin: Okay, I will. Because I’m in the waiting room.
Patrik: Yeah.
Marvin: So I’m going to wash my hands and get back there.
Patrik: Yeah. Just give me a call.
Marvin: Will do.
Patrik: Thanks. Thank you.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!