Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mom is Critically Ill in the ICU. How Long Can She Safely Be Intubated Before Risking Everything?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU, currently on BIPAP ventilation and she is asking why does the ICU team give three (3) sedatives at the same time for her mom.
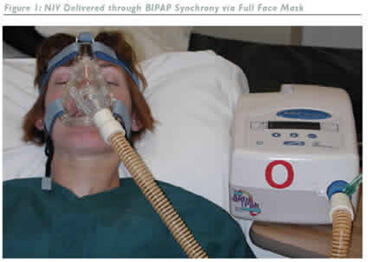
My Mom Has Sepsis in ICU and is Currently on BIPAP Ventilation. Why Does the ICU Team Give Three Sedatives All At the Same Time For My Mom?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Julie here.”
Julie: My argument is, is this something we should be getting rid of, because I think it gives her heart rate a fighting chance, and why is there all these different opinions on, well, as long as the numbers are reading right, we’ll keep her on that, even though we know that it drops her blood pressure down significantly.
Patrik: Mm-hmm (affirmative). I’ll give you my thoughts on that. When I spoke to the nurse yesterday, I was very surprised because I asked him what medications is she on? Yesterday, she was on Precedex. She was on fentanyl and propofol. Now, you know enough about Precedex by now. Do you know anything about propofol and fentanyl?
Julie: I know about, fentanyl is a pain reliever, and I know propofol is what they give you to sedate you for endoscopies and colonoscopies, which is quick acting, take it off and the person comes back up with just little side effects, and it’s just like a medication to take you under a little bit.Then I know the fentanyl is a pain, and then I’m not quite sure. The Precedex they said that the other benefit of it is keeping anxiety down, and it’s also a sedative medicine
Recommended:
Patrik: Yeah, very much so. So I’ll tell you the background there, and what I think about it. Precedex has been around now for about 15 years, it’s a reasonably new drug in ICU. Right, it only came in about 15 years ago. Initially it was designed to replace propofol and fentanyl. I was very surprised yesterday when he said that she’s on all three, fentanyl, propofol, and Precedex. Normally it’s one or another. If you give Precedex, you should take fentanyl and propofol off, right? Fentanyl and propofol have been sort of the standard drug for an induced coma for decades in ICU. Okay? The Precedex sort of tried to replace that starting about 10, 15 years ago.
Patrik: Now, I believe the Precedex has failed. That’s my personal opinion and also experience. It only works in 1 out of 10 patients from my experience. I do believe it shouldn’t be a mainstream drug used in ICU. That’s my personal opinion, and my professional opinion, because I have seen it not work on most patients. I’m very much in favour of propofol and fentanyl. As you said, the propofol is very good in terms of you can sedate somebody quickly, and you can also wake somebody up very quickly. The Precedex has the main side effect of bringing the heart rate down. Having said that, yesterday when your fiance sent me a picture of the ventilator, your mom’s heart rate was 92. What is it at the moment?
Julie: So, her heart rate, 68.
Patrik: That’s very low. The other side effect of Precedex, and you see, this is another issue. Another side effect of Precedex, as well as propofol, is hypotension. Hypotension means low blood pressure. Now, your mom would have a low pressure from the infection. But the Precedex and the propofol potentially contribute to that. Okay. So that’s why I feel like you either give the Precedex or you give the propofol and the fentanyl, but not both. That doesn’t make any sense to me.
Recommended:
Julie: Can we ask the ICU consultant for that?
Patrik: Yes, yes, I think we should. If I can speak to the ICU consultant, I would ask that question, or you could even ask that question to the nurse. I would also try and find some literature around that so that we have evidence. There is some literature around that. Right, because as I said-
Julie: Okay.
Patrik: It was initially designed to reduce propofol and fentanyl, and as I said, for some patients it works beautifully. But I would argue it’s only 1 out of 10.
Julie: So because they’ve continued to use it, is she that 1 out of 10?
Patrik: Say again?
Julie: If they’ve continued to use it, is she that one out of 10?
Patrik: If they are giving propofol and fentanyl on top of Precedex, I argue she’s not the 1 out of 10. I’m pretty sure the doctor there will argue that’s not accurate, that it’s not 1 out of 10, that it works for most patients. As I said, I do not agree with that. What I will do is I will find some literature around Precedex is meant to replace propofol and fentanyl, and giving all three drugs to me is overkill. At the moment, your mom, go on.
Julie: So they tried, what was the other one instead of the Precedex? The one that starts with an A? They tried Ativan, and that’s why they went to the Precedex, because she didn’t respond well to the Ativan.
Patrik: Interesting, interesting. Have they tried Versed or midazolam? Have you heard of that?
Julie: Versed, I haven’t. It does sound kind of familiar, but do you think that’s necessary on top of the propofol and fentanyl?
Patrik: No, no, no. Not at all. Not at all. Not at all. Versed is good for some patients, but one of the main side effects of Versed is it’s a benzodiazepine, and it can make people addicted. They can go through withdrawals of it. So it’s a good sedative, but if you can use the propofol, I would prefer the propofol just simply because it’s not an addictive drug.
Recommended:
Julie: Okay. Okay, perfect.
Patrik: Neither is the Precedex. Neither is the Precedex. The Precedex isn’t an addictive drug either.
Julie: But could potentially, one of the side effects of it is, and the necessity of it, is not dire.
Patrik: I do not see the necessity for it. I will, as I said, my next step is… I’ll tell you what my next steps are. Will send you some questions that you should ask on a daily basis, or even twice a day, morning and night. I will find some literature around the Precedex and what it should be used for. I’ll tell you another reason why they may not have gone away from the Precedex. One advantages of the Precedex is, your mom on BiPAP, is that right?
Julie: Yes.
Patrik: Right, right. Because she was on BiPAP, and she needed a little bit of sedation, the Precedex is good for that if it works. Okay. Now-
Julie: Okay.
Patrik: When somebody is on BiPAP, and they need a little bit of sedation, you can’t give propofol, you can’t really give fentanyl, and you certainly shouldn’t give the Ativan or the Versed that I spoke about. It would knock people out completely. Right?
Julie: That’s what the Precedex did to her. It literally… Oh, yeah, it knocked her out for 48 hours, and that’s when the decline kind of happened because they tried to wake her up the next day, and they found out that her CO2 levels were through the roof, and that her blood became acidic. So they found out that on the BiPAP, the air wasn’t, the CO2 wasn’t being released, and she was knocked out so she wasn’t kind of moving herself around and getting that release of air.
Patrik: Sure, sure. So if that’s the case, then I’d say, if it knocked her out, then I’d say it’s not the right drug for her. It also depends on how much they gave her, for example, did they start on a high dose or on a low dose? You know?
Recommended:
Julie: Yeah. Even though it knocked it out, it did make her so that she wasn’t going to be ripping the IV out and the stuff out. It still, the fact that she was sleeping is still, that’s okay, then?
Patrik: Well, it’s a fine line. When somebody’s on BiPAP, it’s a fine line between tolerating the BiPAP, but not being overly sedated so you can avoid the breathing tube. It’s a very fine line. Because the BiPAP, as you would have seen, can be fairly uncomfortable, right?
Julie: Yes.
Patrik: So you probably need a little bit of sedation, especially if you’re very sick. But at the same time, you don’t want to over sedate because if it knocks you out, you need a breathing tube. That’s a very fine line.
Julie: That’s exactly what happened. That is why we-
Patrik: Right.
Julie: So you think as of now, because we were thinking that the other day. My aunt is actually the one that said, “I don’t want to do the Precedex anymore.” Until we actually got the doctor’s okay. Huh?
Recommended:
Patrik: I feel that way too. I feel that way too.
Julie: Yeah, and the doctor got the okay, but he said that taking her off the Precedex could increase the discomfort, and so we got nervous about that.
Patrik: I don’t think so. I strongly feel that the discomfort can be managed very well on the propofol and the fentanyl.
Julie: Okay.
Patrik: How many days has she been on the Precedex now? For many days?
Julie: Since Sunday, where the nurse put her back on that. So it was last, not this Sunday. So she got admitted on the 16th, and she started getting the Precedex, I think, on Sunday
Patrik: Can you see how much Precedex she’s on at the moment? Can you see that?
Julie: Can you see how much Precedex she’s on? One mic.
Patrik: One mic, so not a lot. Not a lot. But see, the other thing with Precedex is, Precedex is clonidine. I don’t know whether you’ve heard of clonidine, and again, I don’t want to get too medical here. But the issue with clonidine is, again, it needs to be weaned. It should be weaned slowly. So they shouldn’t just take it off. They should probably half it, and then tomorrow take it… If she’s on one mic now, they should probably put it down to .5 for 24 hours, and then tomorrow switch it off.
Julie: Okay.
Patrik: Right.
Julie: Okay, so can I request that?
Patrik: I tell you when you can request it. Let me get you some literature first. Right? I will send you a couple of links to websites where you have it documented that it should be either/or, but not both. It shouldn’t be propofol, fentanyl, and Precedex. It should be either Precedex or fentanyl and propofol. Either/or.
Julie: Okay, perfect. One more question. Yeah, no, I totally agree with you. One more question. She’s on some psych meds that have never worked for her, which we question if she was ever diagnosed right. We believe she was diagnosed because her mother was diagnosed with bipolar schizophrenia that when she started signs of hallucinations and things at age 27 that they kind of followed suit. But the problem was, my grandma, when she took the psych meds, you saw a huge difference. My mom has never showed a difference on psych meds. Never. All it has ever done for her is allow her to sleep at night, so the next day she’s not as erratic.
Julie: So they have her on three different psych meds. They have her on a psych med that can cause seizures, then they have her on a medication that stops the seizures that the psych med causes, then they have her on what? What’s the third one? We don’t know that third one, but my question is, how necessary do we keep her on psych meds that really the only benefit that they ever give her is keep her from getting super upset and not sleeping at night when we’re getting plenty of sleep now, and they all have side effects, and now the infectionist disease doctor came in, and we had to do different options of medications.
Recommended:
Julie: We couldn’t do her preferred one because the psych meds interact with it, and you can’t just stop the psych meds today because the psych meds stay in her blood stream for a while, so therefore we’re not getting some of the antibiotics that may have been the best for the treatment. So I’m just wondering, how necessary is it to stay on these psych meds, and if maybe getting rid of some of this medicine, could her body start to also do better, and the side effects start to get better?
Patrik: So, I’ll tell you my thoughts on that. When patients have psychiatric drugs, and they come into ICU, they are also being continued for a while. Let’s just say your mom, God forbid, was in ICU for the next eight weeks, they would probably be stopped at some point and restarted when somebody’s coming out of the induced coma, right? The question to me is it comes back again to the specialist. Has the psychiatrist been consulted, do you know? Since she’s been in ICU.
Julie: No, I don’t believe so. No, because she hasn’t really been able to speak for herself. The last day she was able to speak for herself was Saturday. Yeah.
Patrik: Okay. Because again, I don’t believe that ICU should be making the decision on whether to continue or not to continue with her psychiatric drugs. That should be up to the specialist. Right, so-
Julie: So should I ask for a mental specialist?
Patrik: I believe so. I believe so. Because those drugs might well interact with everything else.
Julie: Okay.
Patrik: Right? Do you know whether there are any Depo drugs. You know what I mean by that?
Julie: No.
Patrik: I’m not the expert on psychiatric illnesses or diseases, but one thing that I do and is some psychiatric patients have Depo drugs, which means every month they get an injection, and then they get the next injection the next month. Which means there is a drug in the system anyway, and you can’t get rid of it. Right?
Julie: No, she’s not on anything like that. Now that you say that, I’m trying to remember what it was called. Yeah, I do believe she was on one of those at one time. Actually, if you want to know the truth, I felt like that was the one time that we ever seen an improvement, but it was also at the very beginning of her break. So it was her very first break, and they gave her a shot that lasted three months, and she literally was completely normal. I didn’t see anything that I was like, whoa!
Julie: Whatever was in that helped her. It might not have been Depo, or it might have been… He believes a lot of it was depression and stress because she was moved with a brand new baby really far away from home. They moved out of state. She had no family and friends, and she started showing a lot of depression. So I know the shot had something in it that took down her being super depressed and up and down, and she just did wonderful with it. Then we moved. We moved back right away. We were only there a year. Ever since we’ve been here in Wisconsin I feel like the psych meds have had one thing after the other that’s went wrong with them. But I don’t think she’s been on that shot one for a long time.
Patrik: Mm-hmm (affirmative). Okay. Okay. As I said, I am not the expert on psychiatric drugs in ICU. What I do know is in the beginning when patients come to ICU, they’re usually given for a while. Where it might get tricky is once your mother can hopefully wake up, and she’s not on those psychiatric drugs… Let me say this differently. When patients wake up in ICU, 9 times out of 10 they’re confused. Right? That’s patients without a psychiatric history. But if you’ve been in an induced coma for a period of time, and you wake up, you have no idea what’s happened. You wake up in a strange environment, and people are most of the time very, very confused. So for anybody waking up after an induced coma, plus having potentially a mental illness, the situation could get worse. Right?
Recommended:
Julie: Okay. That makes sense, yes.
Patrik: That’s why I can’t answer the question what they should be doing with those drugs. that’s why, again, I believe it needs the specialist.
Julie: Okay, so the next steps is I’ll get an email from you with questions I should ask daily. Some literature on why it should propofol and fentanyl versus the other one, and also them possibly asking them to talk to a specialist for her psych.
Patrik: Also, you see, one other issue is like what I mentioned before, but it’s also important to understand and to probably reiterate that the septic shock causes hypotension. Hypotension is low blood pressure. Okay? The main side effects of Precedex and propofol are hypotension as well. Right?
Recommended:
Julie: Right.
Patrik: Right. Just giving propofol without the Precedex can cause hypotension. Why would you give Precedex on top of that? It doesn’t make any sense to me. This is also why, just again to educate you on this, I mentioned the Versed earlier. Versed is midazolam, and it’s often replaces the propofol for longterm sedation. It’s a benzodiazepine, and it can make people addicted. It has a less hypotensive effect. Right? So the Versed has a time and a place if patients are very hypotensive, and they could be in a coma for a long time to come, because you don’t want hypotension. Most patients are septic, they’re hypotensive already, and then you’ve got propofol and Precedex, that’s often when you change to potentially midazolam or Versed. Just to keep the hypotension at bay.
Julie: Right, and we don’t need anything adding to-
Patrik: No, no, we don’t.
Julie: The situation.
Patrik: No, no, we don’t. If the Precedex works, great, use it. But if it doesn’t, get rid of it.
Julie: Okay.
Patrik: Right?
Julie: Okay, definitely.
Patrik: Right? So if the doctor comes and he’s happy to talk to me, just call me back. Also you mentioned in your text earlier, he didn’t want to talk to me. Ask him what he has to hide.
Julie: Okay, they said something about you coming in on this case out of nowhere when you are employed here, and things like that. I said, he’s just a family friend that knows and has a way of saying things to us that we relate to. So.
Patrik: Ask him what he has to hide. That would be my response if I was you.
Julie: Okay. I’m going to as the nurse too.
Patrik: Ask him what he has to hide, and ask him what’s his problem? Why can’t he talk to me for five minutes. I’m not asking him to talk to me for an hour.
Recommended:
Julie: I will tell him. It wasn’t him that had the problem, it was actually that side nurse today that said that there could be a problem with that. She’s the one that said that we just don’t want to be doing that kind of stuff. I said, “Well, as power of attorney, I feel as though if I give him the code and I would like the doctor to fill him in, and he is a friend of the family, that has a way of explaining things to us and making us more comfortable with the situation, then I don’t see any harm in that.” She said, “Well, I will talk to him, and we will see where it’s going to go.”
Patrik: Okay, and again-
Julie: She said, “But I feel as though everything that was said in the meeting yesterday, nothing more needs to be said.” And that she feels comfortable with it. I said, well, we don’t feel comfortable with it, and I think that’s what matters.
Patrik: Yeah. Your response to that really needs to be, and what do you have to hide? Why can’t you talk to another health professional? That’s not employed. That would be my response to that. The next thing you could do is, you estimated the power of attorney. You have every right to bring somebody in. You could even go to another doctor, and you could say, “Hey, I want a second opinion.” You could do that too. The question really is what do they have to hide? That’s the question.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE quickly when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!