Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
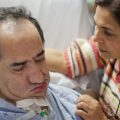
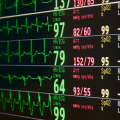
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in ICU with sepsis. Julie is asking on what are the advantages and disadvantages of an arterial line over a non-invasive blood pressure monitoring device.
My Mom is in Critical Condition in the ICU without an Arterial Line. Can I Consider it as Medical Negligence?
Patrik: How are you?
Julie: Good. How are you?
Patrik: Very good. Thank you.
Julie: So, I just wanted to talk to you for a little bit. I’m on my way to one of those meetings. I know you said not to go, but the only reason I want to go this one is because supposedly there’s going to be a surgeon. So, they’re going to be doing the tracheostomy on my mom.
Patrik: Right.
Julie: And they’re going to be in this meeting.
Patrik: Right. So, they haven’t done the tracheostomy yet?
Julie: They haven’t done it, because they refuse to do it until she got off blood pressure medication
Patrik: Right.
Julie: And she got off the blood- huh?
Patrik: Yeah, no, no. I’m just trying to make sense out of what you’re telling me. That’s okay. Just carry on.
Julie: So, I do think it’s a little weird that she hadn’t gone off blood pressure medication a little faster, because she wasn’t on them prior to the extubation trial. And then afterwards, they were kind of giving her these long weaning trial after they re-intubated her, and I think it was kind of stressing her body out.
RECOMMENDED:
Patrik: Right. Right. Can I just ask so she has not had another extubation trial since we last talked?
Julie: No.
Patrik: Okay. Okay.
Julie: Since then they’ve all been weaning trials. So, they did it for three days. They were leaving her on a weaning, the CPAP weaning trial for all day long. And we went up there about four days ago and well I’ve been there ever since, but four days ago they did something really alarming. We went up there and the lady had the blood pressure cuff and readings would go on every hour. And we said, well someone in her condition should probably be reading it every 10 to 15 minutes. She said, “Well no, because she’s in homeostasis.” And she goes, “And I’m trying to get her off blood pressure medication so that she’s a candidate for surgery.” And she goes, “So, I’m going to go ahead and try to step it down right now.”
Patrik: Right.
Julie: And then she left it. So, she stepped down her blood pressure medication and she leaves the settings for over an hour and my fiancée said, “Well, since she just stepped down the blood pressure medication. Shouldn’t you recheck right away or?” She goes, “No. It’ll be fine in an hour.” Well 30 minutes later, my mom starts turning purplish red and just sweating profusely. I’ve never seen her like that before. And so, I went out and then said, “Ma’am, I think something’s going on with my mom.” I say, “Can you please?” And she took her sweet time and comes over, over read the machine and my mom was in like cardiac arrest.
RECOMMENDED:
Patrik: Sorry. Your mom went into cardiac arrest?
Julie: Well, kind of. Because remember that day where she was starting pass away because her blood pressure…
Patrik: Yeah.
Julie: Was all the way to like 43 in those white parentheses? That’s what happened this day, too. And that day, she opened her eyes and they started rolling back in her head even though she was on high levels of blood pressure medication.
Patrik: Yeah. Yeah.
Julie: And that’s when they started jumping up. Well, the same thing happened and she goes, “Oh my gosh. She really loves her blood pressure medication.” And she tried to play it off. Another nurse comes running in, because now that she over read the machine, the sirens started going off. And so, it was kind of like what in the heck. That wasn’t very safe. And now, instead of doing the arterial line that we requested, it’s like now he’s doing that as a power play. And now, he put the blood pressure cuff on the other arm.
Patrik: Okay. When you mom had this episode, did they start CPR? Do you know what I mean by CPR?
Julie: They did not. They did instantly took her off the wean trial. They had respiratory come up and get her off the wean trial and then they just increased her dose of blood pressure medication even higher than it was when she was like, “I’m going to go ahead and step it down.” She had bumped it up really high just to bring my mom back to normal numbers.
Patrik: Okay. You see, you remember the last conversation we had when the doctor was there. As you may remember, I was very adamant about the arterial line and to me, it sounds like it hasn’t changed. To me…
Julie: It hasn’t.
Patrik: Right. And that to me is dangerous. I believe it’s medical negligence. I feel that way.
Julie: And what I just told you is medical negligence, too. To be having her blood pressure set on hourly readings? It’s ridiculous.
Patrik: Totally. And not only that, it’s not only setting it on hourly is dangerous. It’s also with the last time we had the issue of the thrombosis. Right? And you may remember, we discussed that the blood pressure cuff might have contributed to the… you know.
RECOMMENDED:
Julie: Yes.
Patrik: This to me is ridiculous, you know. I mean has that thrombosis been managed? Has that disappeared? Do you know?
Julie: I don’t believe so, because they told me it take a lot of time. So, they said put her on a blood pressure or on the blood clot thinner that could be removed out of the system right away if she needs to go to surgery. They said that that blood clot is going to take a lot of time to remove. But now, I’m so afraid for the speech we’re getting ready to get. So, I just wanted your opinion, because a number of it will be good. My mom had another bowel movement, which was really good. She’s been able to stay on 40% oxygen every day, even after the long all day wean trial, but then recently they shifted her, and she couldn’t breathe and they went up to 50% again. But still, 50% is not 65, 75, you know.
Patrik: Exactly.
Julie: And now, she’s been off blood pressure medication for two days and we’re meeting with the two surgeons that I have a feeling this meeting’s going to go very bad. And I’m missing work. I’m really nervous that I just wanted to hear from you from our time.
Patrik: Sorry, you’re dropping out. Are you there?
Julie: Her other organs are great.
Patrik: Yeah.
Julie: Can you hear me?
Patrik: Yes, I can hear you now. Yeah, Yeah. Uh-huh.
Julie: Okay. So, I have a feeling what they’re going to try to scare us straight back into trying to unplug her.
Patrik: Yeah.
Julie: How do you unplug someone when they’re fighting so hard? Even the nurses are like, “Your mom is very strong.”
RECOMMENDED:
Patrik: Yeah. Yeah. Let me ask-
Julie: Yeah. Go ahead.
Patrik: Let me ask you this. So, I do remember when we spoke last time. Your mom wasn’t on vasopressors from I remember, or if she was on vasopressors, it would’ve been very minimal amount. What changed? Do you know why she’s back on high doses of vasopressors? Do you…
Julie: She’s not now. She hasn’t been for two days, but she was doing fine and they went to go turn her again. And sometimes, these turns really upset her. So, they had to go… yeah.
Patrik: Okay.
Julie: But right now, she hasn’t been on blood pressure medication for two days. Basically, what happened was they extubated her. She failed. They left her tube out for four to five hours. And so, when they put her back, intubated her again, her body was just like, “Uh-uh (negative). I’m done.” And so, her blood pressure medication had to go one then, and they’ve been on ever since until two days ago.
Patrik: Okay. Okay.
Julie: I should say today is day two.
Patrik: Okay. Let me ask you this. When we last spoke, there was discussion obviously about doing the tracheostomy and then sending her somewhere else. Right? So, do you believe to a degree that not following through on the tracheostomy quick enough. Do you think they want to keep her, not send her out? Do you think that’s delaying tactics?
Julie: I don’t know, because we never really told them we were going to do the tracheostomy and send her out. All we said was we were going to think on whether we wanted to get a transfer going forward or not. And so then I called the morning after, because you had recommended, “No. Let’s do the tracheostomy. It needs to get done ASAP.”
RECOMMENDED:
Patrik: Yes. Yes.
Julie: And so I called the very next morning and I said, “Hey, we’re going to go ahead and go with the tracheostomy.” That’s all I said and then because of her blood pressure medication, it’s delayed it until today. We don’t even have an appointment set up because to do the tracheostomy- because they said both surgeons want to be there. So, I’m like the whip. I mean look at how long this is going on. It’s ridiculous.
Patrik: Yes. Absolutely. From my perspective with the blood pressure medication, unless she is on copious amounts, it’s not a reason not to do a tracheostomy.
Julie: No, and she’s only been on like 20 mcg of the Norepinephrine, and then she’s only been on the regular dose of the vasopressin, but not every day. They were able to keep her to 20 to 40 mcg of the Norepinephrine and then they would take the vasopressin away. Then, they would turn her and she might need a little bit of vasopressin again. Yeah, but like I said, today is like day two of she’s had two nights where she hasn’t had any need of blood pressure medication or all day the next day. So, I mean I was like why didn’t they do the surgery yesterday?
Patrik: Yeah. Yeah. I mean 20 to 40 of norepinephrine is a fair amount. Okay?
Julie: Okay.
Patrik: It’s not a low dose, but if she was off it for a number of days or on really low doses, there’s no reason why they couldn’t have performed the surgery I believe. Now remind me with your mom, there was the issue of having a short neck. Is that correct?
Julie: Yes, and the obesity. So, the anatomy of her neck is why they’re doing it surgically.
Patrik: That’s right. That’s right. So with that in mind, she has been reviewed by a surgeon and obviously, the surgeon said, “Yep. That’s okay.” They can perform the surgery. So that box has been ticked.
Julie: Kind of. We’re meeting with the surgeons today and they want two surgeons, and so they said the scheduling has to be an appointment where both surgeons could be there. So, we’ve never really heard from the surgeons mouth or met the surgeons that said, “Yes, we are going to go ahead and do the surgery.” So, we’ve been told by nurses that yes, they got a call. Dr. Smith says yes. They looked at it. They think it’s doable, but there are a lot of risks and your mom is very weak. The anatomy of her neck and the obesity is very critical. None of them are going into surgery lightly.
I just want to know… Of course, it’s a fight. I mean, right? No matter what they say to us today about losing her on the surgery table and putting her through all this, because he had the nerve to pop off he wouldn’t do this to his mom. And I’m like well the other alternative is to let my mom die? So, I don’t know how that’s better.
RECOMMENDED:
Patrik: Yeah. Absolutely. I need to ask a couple of other questions to get clarity on the situation. So, one of the reasons your mom might be back on the vasopressors like the norepinephrine and the vasopressors and because she still has the breathing tube, does she still need sedation? Do you know?
Julie: Yes, and this is the highest they’ve ever kept her on sedation.
Patrik: Right.
Julie: Not Propodol, not Propofol or whatever. Propofol they just recently added yesterday, and it was because she was really struggling during her med trial. They only did a three hour med trial yesterday, but she struggled so hard that they came in and put her on 10 mcg of Proponol, but she’s been on the Fentanyl pretty high levels and they’ve been keeping her on the Precedex at 1 point something mcg.
Patrik: Okay, and how much Fentanyl is she on? Do you know?
Julie: How much what?
Patrik: How much Fentanyl?
Julie: Last night was either supposed to say 12.5 or 125? Does that answer?
Patrik: Yes. Yes. Okay. So, you may remember that the tracheostomy is supposed to have the main advantage of once it’s done, sedation can be taken away. Okay? Precedex. One of the side effects of Precedex and Propofol is hypotension. Hypotension means low blood pressure. Okay? With low blood pressure, well you need the vasopressors. You need the norepinephrine and the vasopressors. That’s one thing. Okay? The other thing to be looked at, especially with the vasopressor, is fluid balance. What do I mean by that? There’s a high chance your mom’s fluid balance would be negative, which means more fluids going out than in. That could also contribute to low blood pressure and the requirement of the vasopressors. The next thing is infection. Do you know whether she’s still battling an infection? Do you know?
RECOMMENDED:
Julie: She’s been getting a little bit of fever and they’ve been giving her Tylenol, because they’ve been taking chest X-rays and checking the white blood cell count, and everything’s been good. So, they told me they think the fever is from the long wean trials putting a lot of stress on her body. Another thing, she’s so swollen like you wouldn’t believe. I’ve never seen her this swollen.
Patrik: Okay. Okay. Now, we’re probably coming closer to what’s happening. Okay. Are the kidneys working?
Julie: Are what?
Patrik: Are the kidneys working? You know what I mean?
Julie: No.
Patrik: Okay. The kidneys. Is she making…
Julie: Oh, kidneys. Yes, yes. I thought you said T-P. I was all the TPN?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!