Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
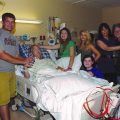
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU for four (4) weeks with sepsis and Julie is asking if she needs to push her mom to be transferred to another hospital because the doctor keeps on delaying surgery for her.
My Mom is in the ICU for 4 weeks with Sepsis.
Should I Push for a Transfer as They Keep on Delaying Surgery For My Mom?
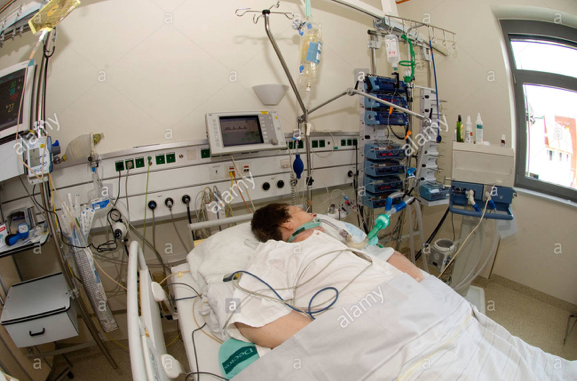
Patrik: Absolutely. Every day is a waste of time, and it’s putting your mom in a worse position. You know?
Julie: Yeah. Do you think there’s still a chance? I mean there’s always a chance, because they won’t even say that my mom could eventually go back and talk again and stuff. I mean…
Patrik: That to me is too far out. Yes. There is a chance, but I’m not even thinking about that at the moment, because she needs to have the tracheostomy, you know? It’s not even… it’s too far out. So, the other thing that I’m wondering is will they tell you that they want do to tracheostomy, want to take her off sedation, and then send her to LTAC. So, that could be another reason why they want to meet. So, if they did that, again, your response to that needs to be that you wanted to have her closer to home first in another ICU. Okay? And the reason to-
Julie: You would say that?
Patrik: Yeah. So, if they went back to you and they say, “Hey. We do the tracheostomy and then we want to send her to LTAC as quickly as possible.” Okay? That could well happen. That could well happen. Your response to that needs to be that you want her in an ICU closer to home first.
Julie: Okay. Should I say that now? Because-
Patrik: No, no, no.
Julie: I’m worried that’s going to trigger them wanting to transfer her before the surgery’s done.
Patrik: They won’t transfer her before the surgery’s done. No, no, no, no, no. Unless… I’ll tell you what I would do if I was you. If for whatever reason the surgery is going to be delayed for another week, let’s just say that, I don’t know what they’re going to talk about, but let’s just say for whatever reason there’s further delays with the surgery. Number one, they wouldn’t send her to LTAC, because she can only go to LTAC with a tracheostomy. But if there were further delays, I would look for plan B which is get her out there as quickly as possible. This place is a shocker.
Julie: Okay. So if they try to say, “Well, we don’t know when we’re going to schedule. We’re going to try to get her in there A-S-A-P.” Should I be like, “I need a date.” Because this is starting to get ridiculous. It’s a waste of time and every day she’s getting weaker and the outcome’s getting less favourable. And just say…
RECOMMENDED:
Patrik: Put the pressure on.
Julie: Okay. I will try my best. I’m not very confrontational, but I will try to just put the pressure on.
Patrik: Do you want me to be there over the phone?
Julie: I don’t know. I don’t know how chaotic it could get, because of my aunt. My aunt is already very confrontational.
Patrik: Yeah. Sure. That’s good.
Julie: And my uncle’s going to be there. Yeah. So, but if you tell me my main goal, I will let the family know on my arrival.
Patrik: Yes.
Julie: I think my aunt does want you on the phone, though. So, I don’t know what you want to do.
Patrik: Look, I. .
Julie: We think that should be on the phone to explain things to us.
Patrik: Well, I think, it’s sort of bad timing. It would’ve been better if you had let me know yesterday, so I could sort of… it’s 1 o’clock now. I sort of have to drop everything.
Julie: Yeah.
Patrik: It might be okay. The question is how chaotic is this going to be. We don’t know. You know the main point.
Julie: Yes.
Patrik: You know the main point.
RECOMMENDED:
Julie: But basically push for the surgery. Push for the surgery and if they’re like, “Well, we can’t get together.” Then I say, “Well, should we have our transfer to get it done sooner?” I feel like they’re trying to get us to request a transfer. I think they’re ready to wash their hands clean of us and my mom. I feel like he’s kind of like, “Let us out. If a transfer’s what you want, a transfer’s what you’ll get.” So, I’m afraid to even throw that around lightly, because I’m afraid that Dr. Smith going to be like I’m done. I’m done arguing with you guys. And then, we’re going to be 24 hours to 48 hours plus delay. So, do you think I should throw that out there?
Patrik: I think so. I think… So, when you’re saying they’re going to push for a transfer, you mean they will push for a transfer to go to LTAC not to another ICU.
Julie: No, I think another ICU. I think Dr. Smith. .
Patrik: Okay. I would take that, because what they’re doing there I think is ridiculous. I mean one delay after another. Still not having an arterial line potentially… because of not having arterial line, almost jeopardising her wellbeing, it’s just getting ridiculous. You know? Why…
Julie: Yeah. From the beginning now with the arterial gas line has caused all of this in my opinion. Because I think it’s able to put that in to her as soon as she went in to the ICU, she would’ve never been intubated.
Patrik: Right. Right. There’s too much… and issues like she’s on high doses of inotropes or vasopressors and she’s still not having an arterial line, I mean that’s ridiculous. Absolutely ridiculous.
RECOMMENDED:
Julie: Yeah, I agree.
Patrik: It sounds very old-fashioned. It sounds like, correct me if I’m wrong there, it sounds to me like this Dr. Smith is the big shot there and there’s nobody else. Is he sort of running the whole show?
Julie: Dr. Smith? He’s never there. He has nurses that don’t even know my mom. Every time they go in, it’s a new nurse. So, they read her chart and they treat her off… So, if they all went back to the beginning, these nurses, then they would’ve known my mom doesn’t do good on the Precedex and the Precedex is one of the things that causes her blood pressure to drop really low. Well, they keep spiking up the Precedex and doing all these crazy things and I’m like okay, one or two or three nurses needs to be following the whole time, and Dr. Smith is never there. All he does is read charts and tell the nurses what to do.
Patrik: So, there is no other doctor in between Dr. Smith and the nurses? There’s not a junior doctor managing while he’s away.
Julie: There’s a regular doctor, just not a pulmonologist.
Patrik: Okay.
Julie: And I’ve never seen her.
Patrik: Right. How many patients are in there? Roughly.
Julie: I’d say in this hospital, there’s like 10 or less. So, Dr. Smith transferred. He goes back and forth between two hospitals.
Patrik: Right. Right, because I’m still trying to work out, and I didn’t have a response to that question last week from him. I sort of said to him like one of the reasons why they haven’t done an arterial line is maybe he doesn’t have the skills on the ground. Right? And that sounds to me like it’s part of the issue. If he disappears, right? And he leaves it up to the nurses, there is no one in between him and the nurses if there might be another doctor, but they’re probably too busy to put in an arterial line, or they are too junior to have that skill. So…
Julie: Probably. Last night, he said the reason why is because he thinks that the reason is he truly does not believe in the arterial gas line. I can’t say it.
Patrik: Yeah, yeah.
Julie: He doesn’t believe in it.
Patrik: Yeah, it sounds like… Look. They’ve probably done this for years. He probably doesn’t know any better, but that’s why I’m also wondering who’s sort of keeping an eye on him? He can do whatever he likes by the sound of things. There’s nobody keeping an eye on him.
RECOMMENDED:
Julie: Yeah, and you can tell because every time a doctor comes in, a specialist, like a gastrointestinal specialist, they’re the only ones that make any difference in her getting better. Every time they’ve ever touched her or when they’re like, “Whoa, this needs to be addressed now,” Or, “Why wasn’t thing this being done?” And all of a sudden things start getting better. It’s almost like he’s overwhelmed and he’s always like… I think he’s too pressed for time. He even shows up late. He’ll tell us he’ll be here at 11, he didn’t show up until 5 PM the other day.
Patrik: Yeah.
Julie: I’m like you’re ridiculous. Even the extubation thing. He showed up in jeans and a T shirt to re-intubate my mom and she showed up to that late.
Patrik: That sounds very unprofessional to me.
Julie: Yeah. It is, but at this point, I feel like our hands are tied and I feel like every day that I’ve come down here and said, “Why haven’t we done the surgery?” And they’re like, “Oh, you know, we’re trying to get in today. As soon as we can get her off vasopressors for one day, we’re able to do the surgery.” Well now, she’s been off the vasopressors for two days. Oh now we’re going to get a transfer? Because I’m scared. I’m scared more and more and more and more time’s going by.
Patrik: Yeah, absolutely. Every day is critical. So, you know what to look for. You know how to conduct yourself. You will need to walk if it’s not heading the right direction, but with everything’s that happened, there is a very good chance Dr. Smith wants her out. And the safest way to get her out is to do to a tracheostomy. A transport would be much safer with a tracheostomy, would be less risky. Maybe he just wants to have that chat with you, but you have to wait and see. But you have to be prepared to walk. Have you spoken to another hospital again in the mean time?
Julie: They won’t talk to me. So, I called St. Mary’s Hospital and the case manager who was there before isn’t there now. And they said they do not talk to patients advocates. The only persons that they will talk to is going to be the case manager from the hospital who sends over a referral, and she said and at that time, we will let that case manager know if we have beds and if our team is willing to take on the case or not.
Patrik: Okay.
Julie: So, that was a dead end route.
RECOMMENDED:
Patrik: Right. Okay, and that’s the hospital where she’s known as a patient.
Julie: Yes. I called St. Mary’s Hospital and I said my mom has been there before, and they said, “Yeah, on different circumstances.” And she said, “Unfortunately, you have to have a case manager.” So, I just kind of gave up on that.
Patrik: Look. You got to go to the meeting and find out what’s happening, and I agree that generally speaking, if the referral is going to be made by a case manager or a doctor, the doors tend to open. Okay? At the same time, let’s just look at the worst case scenario for a moment. They wouldn’t refer. You could always try again, but you need to go to the meeting to find out what’s happening. You know how to push back. You know that your goal is to get the tracheostomy done as quickly as possible. Your goal is to avoid LTAC and your goal is to get her to another ICU to begin with.
Julie: Okay. So, I’m just going to tell them… should I start bringing up the LTAC in a different, I mean bringing up another ICU once the surgery’s done just to stay on the safe route?
Patrik: Absolutely. Absolutely. That’s what I’m saying. That’s what I’m saying. Your goal needs to be get the tracheostomy done and get her to another ICU as quickly as possible.
RECOMMENDED:
Julie: Okay, and if they just won’t let go of the badness the surgery’s going to be, then I say, “Okay, I’m done. I want the surgery to be done as soon as possible. If you guys don’t have the capability of doing the tracheostomy right here, we need to transfer her to a place that does and to do it ASAP.”
Patrik: Absolutely. Look. The reality is she could’ve been transferred with a breathing tube and with a vasopressor. She could’ve been transferred, right? However, the risk is higher to do that. Not that she’s off the vasopressors and hopefully have a tracheotomy before the weekend, that’s eliminating not all of the risks, but it’s much less risky.
Julie: Okay. In all honesty, with a specialist surgeon and all the technology we have now, I just don’t understand how crazy this neck of my mom’s could be because I feel we’re only talking two to three inches of tubing here. How can that be harder to do than intubation?
Patrik: Yeah, look. I haven’t seen your mom’s anatomy, but if her short neck is an issue, look. It is a bit risky, but as I said to you, if the anatomy was fine, Dr. Smith might have done the tracheostomy himself in the unit. That’s nine times out of ten. That’s what happens these days. Okay? They do the tracheostomy in the ICU. It’s half an hour. It’s very quick. Done. Right?
Julie: Yeah, yeah. I know. I know. I totally understand. I’m going to send you a picture today before I leave of her neck. And if you’re okay, I probably will call you tonight to just tell you what happened.
Patrik: Yeah. Please. Please. I would be very interested. Please. And yeah.
Julie: And you don’t think it’s unreasonable for me no matter what the risks are to want to move forward with the tracheostomy, right? You don’t think I’m torturing my mom or being unreasonable.
Patrik: I don’t think so, because the tracheostomy should have happened two weeks ago. Yes, I know there were the issues with the bowels, but again, time has passed. I can’t see why they wouldn’t do the surgery… why would they have the surgeons there? Unless the surgeons are going to tell you, “Oh, we can’t do it at all,” Or the reason, but why would they bring the surgeons? I would hope they bring the surgeons to tell you about the risks and the benefits, but also somebody needs to sign consent. I would imagine.
Julie: Okay. All right. So, I guess I’m going to go in there and sign the consent, and I will give you a call back later. Is there a time that’s better than another?
RECOMMENDED:
Patrik: Probably any time… It’s just really the next couple of hours where I’m busy, next hour or so. But, any time after that should be fine.
Julie: Okay. Perfect. Thank you so much for all your time.
Patrik: You’re very welcome.
Julie: What did you say?
Patrik: I said you’re very welcome.
Julie: Oh, okay. Thank you.
Patrik: All the best. Take care.
Julie: Thanks, you too. Bye.
Patrik: Thanks. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!