Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is critically ill in the ICU and she is asking if the ICU team has a timeline for patients in the Intensive care.
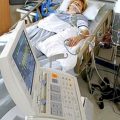
My Mom is Critically Ill in the ICU. Why Does the ICU Team Want Me to Just Pull the Plug on my Mom’s Life Support? Help!
Patrik: I’m Patrik speaking. How can I help?
Julie: I was wondering, what is this hotline for? Is this for an advocate to come and let you know what’s going on with your loved-one?
Patrik: Yeah. We help families who have a loved one in Intensive Care. Yes, we are consultants and advocates for that situation. Do you have a family member-?
Julie: So you can say … you can look at- ?
Patrik: Do you have a family member in Intensive Care?
Recommended:
Julie: Yes, I do. And so, you can look at their files and see if everything’s being done that needs to be done?
Patrik: Absolutely. Absolutely.
Julie: He said, “Absolutely.” Okay. ‘Cause we need … this is a stat decision. What should I say?
Patrik: A “stat” … What do you mean with “stat decision”? Are you- ?
Julie: They are trying to-
Patrik: What are they trying to do?
Julie: What’d you say?
Patrik: No, no. What are they trying to do?
Julie: They’re trying to tell us that we can either pull her off the life support and make her comfortable and watch her go. Or we can keep going at this path, but she’s gradually getting worse.
Patrik: Okay. We can definitely help you with getting best care and treatment for your … is it your mother or …?
Julie: Yes, my mom.
Patrik: Right. Are you the medical power of attorney for your mom?
Julie: Yes.
Patrik: Right. Okay. So, you have decision-making authority?
Julie: Yes.
Patrik: Okay. Yeah, we can definitely help you with that. Tell me a little bit more, why is your mom in ICU?
Julie: She got pneumonia and she was at a nursing home. She was at a nursing home because she’s bedridden.
Patrik: Right.
Julie: She’s 56, and she got pneumonia. And they kinda did wait for her to get a little bit purple before bringing her in to here. There wasn’t a rush on it. And they did get her in here, and they got her on oxygen, and her saturation level was good. And then they got her into the ICU, and they got her on the BiPAP machine, because they wanted her to breathe a little better, to keep her oxygen levels up.
But then she kept being defiant and wanting to rip the mask off so she could talk, and she didn’t want the blood oxygen level light on her finger. And so, then they decided … so Friday, Saturday, Sunday … about three days later that they would start her on … What’s that P-word?
Recommended:
Mike: Oh, Precedex.
Julie: Precedex, which … upon arriving at the hospital, they gave her Precedex, and it dropped her blood pressure down really low. And so, they said “No more of that,” because that dropped her to scary levels, and so they took her off. Well, then three days later a nurse decided to put her on low levels ’cause she was watching her numbers and said she felt safe, and she put her on it so that my mom would behave basically.
Patrik: Right.
Julie: And not rip off the BiPAP machine. Well, then what happened was they were watching the machine, the saturation levels. But the next two days she slept and slipped into a coma, because the CO2 levels went through the roof, and she actually became … her blood became acidic.
Patrik: Right. Okay. Is she still on BiPAP or is she … how is she breathing at the moment? Is she on a ventilator?
Julie: Yeah. So, they found out two days later, and she almost lost her life last Tuesday at 2:00, and they had to intubate to save her life.
Patrik: I see. How many days-
Julie: But she did not flatline. She did not flatline. What did you say?
Patrik: How many days had she been in ICU in total?
Julie: Total, 16 days.
Patrik: 16 days. And basically, since last Tuesday she’d been on the breathing tube and in an induced coma?
Julie: Yes. Yes. Well, she kinda went into an induced coma from the CO2 levels on the BiPAP, and then they couldn’t get her to wake up. And then they found out that she was acidic, and she had high CO2 levels. So, then they put her on the intubation, and now she’s been in that induced coma.
Jane: She also has air in the abdominal area.
Julie: And then recently, as of this morning, they found out that she has air in her abdominal. Because they said that her blood supply is shutting off to her intestines or something like that.
Recommended:
Patrik: Okay. Okay. So, have you heard of lactate levels? Have you heard of lactate levels?
Julie: They did. Yesterday it was 1. This morning it’s a 2.2.
Patrik: Yeah, it would go up. If blood supply to the abdomen is dying, it’s closing off, the lactate would be going up. What’s your biggest challenge? And, sorry, what was your name again?
Julie: Julie.
Patrik: Julie. I’m sorry, Julie. What? At the moment, you’ve basically been given two options, which number one is to stop life support, let her pass away. Or number two, keep going, but she will deteriorate anyway. That’s pretty much what they’ve told you.
Jane: Yes, that’s what they’re saying.
Julie: Yes. I mean, they’re not saying they won’t give us 100%. So, they did not say, “If you continue forward …” They said, “We think she might not get better, but no one knows.”
Patrik: Of course. And the doctors who are saying that, they’re the Intensive Care doctors, they’re not pulmonologists, because she came with a pneumonia. What’s the doctor’s qualification who’s saying all of this?
Julie: He is a pulmonologist.
Patrik: Okay. Okay. And how has that been communicated? Have you been asked to attend family meetings? How has that been communicated to you?
Julie: Today was a family meeting, was our first family meeting.
Patrik: Okay. Did you … when you went into the family meeting, did you see that coming or were you completely surprised by what they told you?
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Julie: I would say mostly surprised. We knew that she … Well no, I’m going to say surprised, because we’ve kind of been told that her … on the intubation she’s going from … she could be at 100, but no, she goes to 60, then she goes to 50. And then they said, “We’re trying to lower the oxygen, but she can’t tolerate that at that time. The pneumonia’s gone, the sepsis septic is gone, her UTI is gone, things are showing improvement.” So, to me, I felt as though things are getting better.
Patrik: Okay. And when you went to the meeting, who was there? There would have been the pulmonologist, there probably would have been a nursing charge or … Who was there in the meeting?
Julie: A nurse that saw her for the first time today, and a doctor we had never met. The doctor that we were with, was on her case, wasn’t there. They put another doctor they said was her colleague or something. And then the pulmonologist and then an advocate for my mom and for us supposedly. But she was more kind of leaning towards you just need to let her go.
Patrik: Did the advocate … Is the advocate an employee of the hospital?
Julie: Yeah, we think so.
Jane: Yes, she’s definitely.
Patrik: Okay. Okay. All right. Look, we can definitely help you. I mean we are highly specialised in that area, the way we can help you is-
Julie: Now, which way are we getting help here? Is this help in “There’s still a fight for my mom” kind of help? Or are we … is this help like we’re trying to pin … say “Something was done wrong way” help?
Patrik: Yeah. So, let me explain how I can help you. So, we are highly specialised in knowing about patients’ and families’ rights, okay? And not only that, but also, we are clinicians. For example, I have worked in Intensive Care for 20 years.
I believe … I argue I’ve seen it all, right? I’m well aware of patients’ and families’ rights. We can provide a second opinion for you. Right? But more importantly, things like … look, I’ll give you an example, right? If you had come to me 24 hours ago, and you would’ve told me, “Hey, we’ve got this family meeting tomorrow,” I would’ve said to you, “Don’t go.” Because I could’ve told you what’s going to come.
Family meetings are designed to deliver bad news. That’s the only reason family meetings are being held. Okay? And if you do go to a family meeting, you need to be prepared. Because otherwise they will walk all over you, and that’s what’s happened in this situation. You know, they’re bringing an advocate in, a quote-unquote advocate in. That’s not really an advocate, because they’re not independent.
Recommended:
Julie: Okay.
Patrik: So, for example, what I would like to do as the next step is, I would really like to talk to the doctor with you. We would have to set up a call with you and the doctor, and then find out what’s exactly happening and really asking all the clinical questions. You see, your biggest challenge at the moment is that you don’t know what you don’t know. Right?
Julie: Exactly. Yes.
Patrik: That is your biggest challenge. Right? You don’t know what you don’t know, and that’s exactly where I can help you with. You know, after having worked in Intensive Care for 20 years, we leave no stone unturned. Right? And I would really like to speak to the doctor to ask some clinical questions and ask him why-
Jane: How quickly can you see it happens. They’re trying to tell us that she could pass away at any second.
Julie: How quickly can you talk to him?
Patrik: Do you think you can get the doctor on the phone in the next two hours? I mean, it’s the middle of the night for you.
Julie: He’s gone for the night.
Patrik: Okay.
Mike: He’s on call though.
Patrik: Okay. Okay. Yeah, we can … If he’s available, I’m available.
Julie: Okay. So, can we ask your opinion on the whole starting the … the P-word.
Mike: Precedex.
Recommended:
Julie: … the Precedex and taking her into a coma? Could that very well be what is the leading cause of all of this? And if we take her off the Precedex, could she possibly start to do better? ‘Cause they’re continuing to give that to her.
Jane: Is there a possibility she’s allergic to the Precedex, and it’s just a matter of taking her off of that? And if they need to keep her sedated, give her a different sedation that would help with the anxiety and all of that, but not it be the Precedex, ’cause that was the finger we can point to that started the downhill decline.
Patrik: Right. Look, I would need to know what … it’s often not simply you give one drug and then everything goes downhill from there. I would need to know more, which is why I would appreciate if we could talk to the doctor. The Precedex has certain mechanisms and all that, certain side effects, but I would not provide an opinion on that without knowing what else has happened. I get the bigger picture with, you know, pneumonia, BiPAP, CO2 is rising. I get the bigger picture, and I know the Precedex … I’m well aware of what Precedex is doing, and I’m aware of the side effects. However, I would want to know more in terms of what else is happening before I-
Jane: Now that being said, I just worry because they’re throwing out diagnoses that have not ever really been …
Mike: There’s no evidence.
Jane: I don’t know.
Mike: There’s no evidence.
Jane: Yeah, there’s no evidence. So, they found a diagnosis from the nursing home, and I worry, you talking to them, that they can convince you “Oh, her quality of life prior to this was bad.” Or “Oh, her diagnoses of this certain disease is why she’s leading to this.” But that is not the case from knowing her and her family. We know what her quality of life was before, and we know that where we are right now is not because of this diagnoses that came out of nowhere.
Recommended:
Patrik: Look, I can get you … We constantly argue that quality of life is not a determining factor of treating somebody in ICU or not. I’m not … I can tell you … I don’t know how much research you’ve done on our website. You know, I don’t know how much research you’ve done. We would … Quality of life is a subjective measure, and it’s never in my mind a determining factor whether you should, or you shouldn’t treat somebody in Intensive Care. Right?
Jane: Well, thank God, because they keep saying that.
Patrik: I wouldn’t even go … Yeah, it doesn’t matter what they say. I would tell them exactly what I tell you now that quality … that perceived, perceived quality of life should not be a determining factor whether you treat somebody in ICU or not. And that’s the end of story. And again, after 20 years in ICU, I believe I can make a credible argument to the doctor in terms of saying “This is all bullshit,” because quality, perceived quality of life in the future. It’s not a determining factor what you’re doing today. It’s a perception.
Jane: And then what about them throwing this diagnosis around? Because I assure you the diagnosis did not disintegrate all of the sudden. She’s had this diagnosis supposedly for- how long?
Mike: Like four years?
Patrik: What is the diagnosis? What is it?
Jane: It’s PML.
Patrik: PML.
Jane: So, it’s like … Yeah, do you know what that is? It’s a … Can we look it up, so we can tell him what it is? It’s like multifocal …
Mike: Progressive Multifocal Leukoen-
Patrik: I’m just browsing on net. Right, right. Yeah, I’ve just found it. It’s a very rare disease. I haven’t come across-
Recommended:
Jane: Yeah. And the thing is she’s not … you most likely pass away. And then you also degenerate over time, but a short amount of time. I mean we’re going on … this has been going on her whole life. So, if she did have the PML … yeah, she recently lost her ability to walk. That was about three years ago, but they found out two years ago she had a split disc. And she complained and complained about this pain in her back and she kept falling. I don’t say slipped disc or whatever it is right, but a slipped disc.
Patrik: Look, the … I do-
Jane: She has a slipped disc.
Patrik: Sure, sure. I do believe that the most important part here is that, irrespective of the diagnosis they have made, that they will continue treating her. I do believe that is the most important part. Why do I say this? I say this because patients in ICU are sick. They are often diagnosed with really rare or critical illnesses, but nevertheless, as long as there’s life, people need to be treated. Right? And with this PML, have they got a neurologist involved?
Jane: No, they’re going off of a neurologist from two years ago that was like, “Okay, I think this is what we have, because it’s the best thing I can explain that,” I guess. We were never told about it. Until we came to the hospital and they said, “What’s the PML diagnosis?” We’ve been asking the nursing home the results of that visit to get the MRI for the longest time. And then they said something about … Yeah, so basically, from just what you read about it and just how long she’s had it, I don’t believe that. I think we’re playing with a little bit of maybe long-term mental illness mixed with a slipped disc. And we didn’t ever get the surgery needed, and so it broke her down to where she couldn’t walk ’cause of the pain, and then she atrophied. And so, they’re just using … they’re basically being like, “Well, that matches up with this. We’re going with PML.” And now they’re trying to use PML as the main reason as to why she is falling apart. And it’s not, because she went in-
Recommended:
- What if you could reverse the Intensive Care team wanting to “pull the plug” or “withdraw treatment”
Patrik: So, this is not a new diagnosis. It’s not a diagnosis that was made in the last week?
Jane: No.
Patrik: Okay. Okay. So, then I wouldn’t really worry too much about it. Look, I know, I tell you what I can do for you. Right? I would never claim that I can save a life, right? That would be foolish of me. But what I can confidently claim, and we’ve got hundreds of case studies on our website, right? I can buy you all the time that your mother needs to get the best care and treatment in there. Because again, basically what they’re telling you is that you have no rights, and they make the decisions, and she’s probably going to die. That’s what they’re saying. Right?
Julie: Yeah, but they’re saying that we have the MRI results.
Patrik: Okay. You have the MRI. Well, that’s good. But on the other hand, it sounds to me like it can’t be … it sounds to me like they can’t have the diagnosis. They can’t be like they are leaning towards stopping treatment. Most ICUs are leaning towards stopping treatment as soon as things get difficult, you know? But again-
Jane: Yes, they definitely are leaning towards stopping.
Patrik: Right, right. And that’s where I can help.
Jane: Can I ask you this question? So, we’ve laid out how ill she is and everything. We’re at a smaller hospital, and not too far away from here there’s a much, much larger hospital. Do we have the right, would it be safe to transport her to a different facility? What are our-
Patrik: Yeah, let me talk to the doctor, and then I can tell you whether it’s safe or not. Again, I would need to know more clinical information. I would need to speak to a clinician to find out is this a situation where your mother can be transferred to another hospital. So again, I would need more clinical information before I can guide you there.
Jane: Okay. Do you think that would be beneficial if she could, though? Like second opinions? Or just a second opinion coming here? Or are you that second opinion? Are you a doctor?
Patrik: No, I’m not a doctor. I’m an Intensive Care nurse with 20 years’ experience.
Jane: Okay.
Patrik: But again, I believe I’ve seen it all. And what we’re really special- And we are a team of nurses here. We’re not a team of doctors, because doctors usually protect each other. And we are real patient advocates. We don’t have … we’re not affiliated with the doctors or with any of … Our service run by Intensive Care nurses. Right?
Jane: Okay.
Recommended:
Patrik: We believe that nurses are real advocates and don’t have … like a lot of the doctors have interests that go way beyond treating a patient. They have interests that … you know if you’ve done a little bit of research, they have interests in medical research, they have interest in getting money through medical research, but don’t necessarily have the interest in treating patients appropriately. Whereas as we, as nurses, we are genuine advocates. And again, I don’t know how much research you’ve done. You can listen to some interviews on our website, on our podcast. Where we interviewed some of our clients, how we help them to get outcomes. Because we don’t really care what the doctors think. We are advocates. Whereas, if you have another doctor coming in, they’re often protecting each other.
Jane: That sounds like what Julie needs. So, let’s get down to brass tacks, and first, what’s your name?
Patrik: Patrik.
Jane: Patrik?
Patrik: Yeah.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recording and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!