Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
In the last blog I talked about
You can check out the last blog by clicking on the link here.
In this week’s blog I want to talk about
The difference between “real” and “perceived” futile medical treatment!
Before I get into today’s topic I want to share a quote with you that I wrote on today’s topic and the quote says
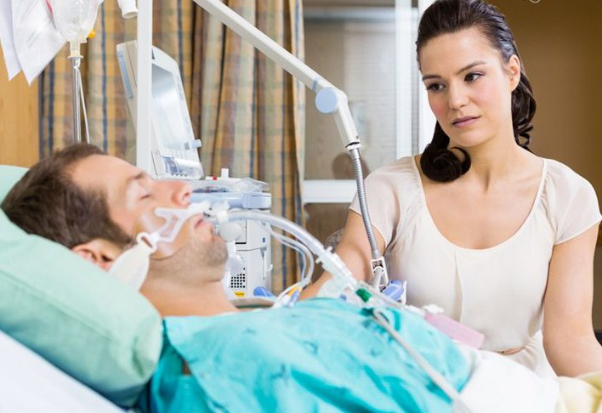
Families of critically ill Patients in Intensive Care are often surprised when they first hear about medical treatment being “futile”.
They are often wondering what the term “futile” really means in the context of Intensive Care treatment and therapy for their critically ill loved one and they are often wondering why the Intensive Care team is using the term “futile medical treatment”.
Futility of medical treatment is nothing more and nothing less than a perception and it may or may not reflect reality.
The perception whether medical treatment is futile or not often depends on one’s point of view as well as the agenda one is pursuing.
Intensive Care teams often have “hidden agendas” where many moving and hidden parts impact on how Intensive Care teams position your critically ill loved one’s diagnosis, their prognosis, as well as their care and treatment.
Families of critically ill Patients in Intensive Care often have no idea whether the positioning of their loved one’s diagnosis, their prognosis, as well as their care and treatment is accurate and they often need urgent re-education about Intensive Care and the dynamics in order to make informed decisions, get peace of mind, control, power and influence!
So let’s get into today’s topic
Here’s the definition about “futile medical care” from Wikipedia:
“Futile medical care is the continued provision of medical care or treatment to a patient when there is no reasonable hope of a cure or benefit.”
Let’s put this in context in Intensive Care.
If you have followed my blog for any reasonable length of time you’d know by now that the majority of the things the Intensive Care does in order to position your critically ill loved one’s diagnosis, their prognosis, as well as their care and treatment is driven by the “hidden agenda” of the Intensive Care team and it’s driven by what’s happening “BEHIND THE SCENES” in Intensive Care.
Especially the last part of the definition of “futile medical care” needs to be looked at in more detail.
“when there is no reasonable hope of cure or benefit”
What does “no reasonable hope of cure or benefit” mean?
In Intensive Care terms the interpretation and the positioning of Intensive Care teams often means
“We don’t think that it’s ‘in the best interest” for your critically ill loved one to continue treatment, because your loved one wouldn’t have any quality of life in the future if they do survive…”
It’s like a catch phrase in Intensive Care, especially a catch phrase the Intensive Care team is using quite regularly to cement their positioning, cement their “perceived power” and cement their “perceived authority” in order to get what they want.
This is particularly important if your critically ill loved one is either
The fact of the matter is that Intensive Care teams have no idea what’s happening to a critically ill Patient outside of Intensive Care in 6 months time if a Patient has survived Intensive Care, because it’s not their area of expertise.
The fact of the matter is that “no reasonable hope of cure or benefit” could mean a variety of things. Let’s look at some of them in more detail.
1) If Intensive Care teams continue treating a critically ill Patient in Intensive Care where they perceive there is no “benefit” or “cure” to a critically ill Patient they often only speak in medical terms, they don’t speak in emotional terms.
2) Therefore one of the “benefits” to continue treating a critically ill Patient in Intensive Care could be non-medical “benefits” like giving a family more time to come to terms with the situation they are currently facing. It could also mean to have more time in a “real” end of life situation where a family is waiting for other family members to be with their critically ill loved one. Situations like that tend to be very complex, therefore it’s important that you chose what needs to happen so that it makes sense to you and your family!

3) A “benefit” to continue treating a critically ill Patient in Intensive Care could also be to give families the opportunity to have an end of life situation on their terms. What do I mean by that?
The rather bleak reality in Intensive Care is that when Intensive Care teams want to decide to “withdraw treatment” or “withdraw life support”, they want to do so as quickly as possible and they want to do so in a time frame that is convenient for them and the Hospital.
After all the pressure in Intensive Care, where a bed costs around $5,000-$6,000 per bed day is huge.
Furthermore, Intensive Care beds are in ever increasing demand and those beds are precious and expensive. Therefore it’s a limited and precious resource.
What it really means that once the Intensive Care team wants to “sell” you and your family that a “withdrawal of treatment” is “in the best interest” for your critically ill loved one, it means they often want to rush things because of the things that I mentioned above.
What about giving you, your family and your critically ill loved one choice?
For example if “withdrawing treatment” might be perceived as “in the best interest” for your critically ill loved one, why not giving you, your family and your critically ill loved one the opportunity to do so at home?
This would help you and your family as well as the Intensive Care team.
Related articles/videos:
Let’s look at this in more detail.
a) It helps you and your family to spend more time with your critically ill loved one, which is most likely what you want and it helps families in Intensive Care to have an end of life situation on their terms rather than on the Intensive Care team’s terms. With a shift to more and more home care anyways, even high acuity areas like Intensive Care can now outsource more and more work into the community with services like INTENSIVE CARE AT HOME.
b) This leads me to my next point. Intensive Care teams and Intensive Care Units want to save money, they want to have their beds available and they often don’t want to invest the physical as well as the emotional resources that are necessary to get a critically ill Patient and their family where there is a chance of a meaningful recovery and/or meaningful end of life. They prefer treating Patients that have a shorter stay in Intensive Care.
The good news is that with services like INTENSIVE CARE AT HOME everybody is winning.
INTENSIVE CARE AT HOME is offering Patients, their families as well as Intensive Care Units the choice to meet their goals.
For families it’s often choice and peace of mind to have the opportunity to have their loved ones at home and for Intensive Care Units it’s a matter of emptying their beds and saving money. INTENSIVE CARE AT HOME costs around 50% of an Intensive Care bed and can still provide similar quality services in a much more Patient and family friendly environment.
Therefore the term “futility” and “Futile medical care” needs to be looked at in context and not in isolation of services available as well as the emotional needs of Patients and their families.
How do I know the difference?
After nearly 20 years Intensive Care nursing in three different countries where I literally worked with thousands of critically ill Patients and their families and where I have been actively involved in hundreds of “real” and “perceived” “futility of treatment” situations in Intensive Care, I think I have a real duty to share with you the lessons that I have learned!
I have also worked as a Nurse Unit Manager in Intensive Care for more than five years and I have been managing again many “real” and “perceived” end of life situations/medical futility situations in this role.
I’m also now managing many “real” and “perceived” “futile medical care” situations in my 1:1 counselling and consultancy practice here at INTENSIVECAREHOTLINE.COM and help my Clients to make informed decisions, get peace of mind, control, power and influence in those situations!
And I also have experience with INTENSIVE CARE AT HOME services and I know first-hand what’s possible at home for Intensive Care Patients and their families!
The bottom line here always is that you and your family need to ask yourself the questions around what the Intensive Care team’s “hidden agenda” is whenever they are referring to potential “futile medical care” or “futile medical treatment”.
The fact of the matter is that real “futile medical care” or real “futile medical treatment” is based on a perception of a situation and not necessarily on reality.
It’s the Intensive Care team’s interpretation of a reality.
Recommended:
Having a holistic perspective!
The most important question in this is what is your reality? Do you believe that continued medical treatment is futile and of no benefit to your critically ill loved one and your family?
Would ongoing medical treatment be of benefit for you, for your family and for your critically ill loved one? You and your family are most likely looking at it from a holistic perspective. Chances are that Intensive Care teams are only looking at it from their limited perspective which is biased by issues like the financial management in Intensive Care, the availability of beds and staff in Intensive Care, as well as the competition for limited resources in Intensive Care.
Intensive Care should be all around Patients, their families and making meaning out of the situation.
Positioning your critically ill loved one’s treatment as being “futile” will probably not make much meaning to you and your family.
Positioning your critically ill loved one’s care and treatment in a meaningful way that makes sense to you, your family and your critically ill loved one is a much more beneficial approach to those often heartbreaking, challenging and difficult situations.
Offering you, your family and your critically ill loved one choice during “real” or “perceived” “futile medical treatment” situations is a much more Patient and family friendly approach.
Therefore a “real” “futility of treatment” situation is only ever “real” if no fancy treatment, no fancy type of surgery, no life support equipment can save or preserve your critically ill loved one’s life.
On the other hand given with everything that you know now, with the empowerment you get, the chances that whenever the Intensive Care team is using the term “futile medical care” they are trying to limit the options for you, for your family and for your critically ill loved one, without looking at what’s possible and without looking at would be meaningful to you and your family.
Once you have looked at several options available for you and your family, such as extending life for your critically ill loved one in or outside of Intensive Care to give meaning to the situation for you and your family you will come to the conclusion that most “futility of treatment” situations in Intensive Care are “perceived” and not “real”.
It all depends on the context of the situation.
Once you know and understand that “what you see is not always what you get” in Intensive Care and once you know how you can powerfully position your critically ill loved one’s diagnosis, their prognosis, their care and their treatment as well as the meaning you want to attribute to it, you will find that there are options available to you in order to make informed decisions, get peace of mind, control, power and influence!
Therefore don’t let the things happening “BEHIND THE SCENES” in Intensive Care dictate if your critically ill loved one is in a “real” or a “perceived” medical futility situations.
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get PEACE OF MIND, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s BLOG and I’ll see you again in another update next week!
Make sure you also check out our “YOUR QUESTIONS ANSWERED” section where I answer your questions or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling with me via Skype or over the phone and via email by clicking on the email and phone counselling tabs on the top of the website!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!