Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
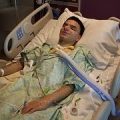
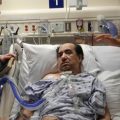
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Julie as part of my 1:1 consulting and advocacy service! Julie’s mother is in the ICU for Pneumonia and is asking if the next step for bowel ischemia is surgery or antibiotics.
My Mom is in the ICU for Pneumonia. Conservative Management or Surgery? Help! Time is running Out.

“You can also check out previous 1:1 consulting and advocacy sessions with me and Julie here.”
Art: Hello?
Patrik: Hello. It’s Patrik here. How are you?
Art: Okay. Good, give me one second-
Patrik: You let me know.
Julie: Okay, can you hear us?
Recommended:
Patrik: I can hear you, can you hear me?
Julie: Yeah.
Patrik: Okay. So, I don’t know whether you could hear some of the conversation that I had with Mel?
Julie: Yes.
Patrik: Right. So, he was really. He wasn’t trying to avoid any of my questions, which is always a good sign. Basically, what’s happening is the problem has shifted from the pneumonia to potentially having a bowel perforation, okay? They are not 100% sure whether she does have bowel perforation, they’ve done two CT scans in the last 48 hours. They think there is bowel perforation, but they are not 100% sure. Is that something that they brought up with you? Are you aware of that?
Julie: No.
Patrik: Right. So, nobody told you about the potential for bowel perforation?
Julie: They said that the blood supply had been shut off and the intestine has started to die.
Patrik: Right. So …
Julie: What causes the perforation?
Patrik: Say that again.
Julie: What causes the perforation?
Patrik: They’re not sure. What happens is …
Julie: Does that …
Patrik: What happens is when somebody is in a coma, their bowel motion is slowing down. Their bowel motions are slowing down when they are in an induced coma and with that, stools can push to the edge of the bowels and then there could be a perforation. Has your mother ever had issues with bowel motions?
Julie: A bit of constipation at the nursing home, but then they would use a thing to get it moving. She’s had a little constipation in the past.
Patrik: Okay.
Julie: But going in here, we did not see her for seven days, and they knew she wasn’t having a bowel movement for over how long now, now? They didn’t start treating the fact that she hadn’t had a bowel movement in days until about three, four days ago.
Patrik: Right. So, what they’ve done is they consulted the bowl surgeon, so at the moment she’s not a candidate for surgery, just simply she’s too unstable. It looks like she’s going into septic shock. Have you heard of that?
Julie: Septic shock you said? And why?
Recommended:
Patrik: So, it looks like she’s going into a septic shock at the moment. What’s happening is she’s basically battling two infections at the moment. She’s battling the pneumonia, even though Mel said that the pneumonia is a lot better, but she’s now battling the next infection, which is she’s got some bacteria in her gut. One way or another, she would have some bacteria in her gut from not opening bowels or potentially having a bowel perforation.
If that happens, patients get severely infected, and they often go in what’s being called a septic shock. What happens during septic shock is blood pressure drops significantly, temperature goes up, and your mother is showing both signs at the moment. So, her blood pressure has dropped, and her temperature is going up, and her white cell count, the white cell count is the marker in the blood for an infection, has doubled in the last 24 hours.
Julie: Okay.
Patrik: Are you following me?
Julie: I am, I’m just wondering, how do we fix it.
Patrik: What they’re doing at the moment is they’re stabilising her blood pressure. They’re stabilising her blood pressure with medication. But, before I go on, what’s important to know, I have no concerns at the moment that they’re not trying everything within their power. I have no concerns that they’re not trying everything.
Julie: Okay.
Patrik: Because I was trying to find out, what are they doing? Are they potentially withholding some options for treatment? And, clearly, they’re not. So that was really important for me to find out. Are they doing everything within their power, or are they potentially withdrawing or withholding life support, but that’s not the case?
Julie: Okay. So, can they treat that perforated bowel before it’s too late?
Patrik: This is the problem. I’ll tell you where the problem is. In a more stable scenario, let’s just say another patient would have a bowel perforation outside of hospital, you would operate on them fairly quickly. The reason why they can’t operate on your mom at the moment is she’s too unstable. Now, what do I mean by that? She’s on two forms of life support at the moment. One form of life support is the ventilation, and the other form of life support is what’s called Vasopressors.
She is currently on Norepinephrine and Phenylephrine, and those are life support drugs. They are basically stabilising the blood pressure, and she’s on high doses of that. Very high doses of that. Now, if she was to go for surgery to get the bowels fixed, it would be unlikely that she would survive that, because she’s so critically unstable at the moment. Even though the surgeon might say, “Yes, the bowels are perforated, and we need to surgically operate on them,” the reality is she’s way too unstable to go into surgery at this point in time.
Recommended:
What do they need to do? They need to give her antibiotics, which they are giving, and see whether they can get the infection under control that way and get her more stable. And once she’s more stable, then there is a chance that they might be able to do surgery.
Julie: Okay, and I heard him say that she is … they are going to treat with the GI. What does that mean?
Patrik: GI stands for gastrointestinal tract. Anything, basically, from the stomach to the rectum is referred to as the GI area. Anything stomach and bowels is referred to as the GI area. So, what that means is they made a referral to a GI surgeon. The GI surgeon had a look at the CT scans, but they’re not 100% sure whether the bowels are perforated or not. They’re still undecided about that. Having said that, the signs she’s showing, which is a septic shock, makes it highly likely that the bowels are perforated. Makes it more likely than not.
Julie: Okay.
Patrik: I am …
Julie: So, can we treat her for sepsis, and she can get stronger enough for the surgery that’s realistic the timeframe, or could we possibly lose her?
Patrik: She’s definitely critical. I’ll tell you what I believe needs to happen next. I’m surprised that you are not … So, you didn’t know about the possibility of bowel perforation. Nobody told you about that.
Julie: No. They said that they thought there might be a blockage, but they have confirmed that there’s, in the blood vessels, they’ve confirmed that there’s not blood getting to the outside of the intestines, and that the intestines had died. That’s what they said.
Patrik: I see. And if the intestines have died, that also makes it more likely that the bowels are perforated. Makes it more likely.
Julie: Is that from not doing an enema sooner? Is that from how long she went constipated? Is that … because that’s clearly just a recent thing that happened, and they’ve been recently trying to get her to have a bowel movement. Is that from feeding her too fast? Why?
Recommended:
Patrik: What happens is when somebody’s in a coma, in ICU … Or, not even in a coma, but when somebody is in ICU, and is immobile, basically bed-bound, it makes it all the more likely that there is bowel obstruction. So, the question to me is … definitely goes into the direction of why they have not tried to manage the constipation earlier, and, normally, the deadline is if you haven’t had your bowels open for three days in ICU, you need to get an enema. So, I don’t know … The question needs to be asked: has she had an enema after three days of not opening bowels.
Julie: I don’t know the protocol for ICU but we know she’s had an enema in the last two days.
Patrik: Yeah. He told me that. Mel told me that.
Julie: They hadn’t done anything for her at that time. They weren’t feeding her, either.
Patrik: They weren’t feeding her, were they?
Julie: They stopped feeding her. They didn’t feed her until she got on the intubation. When she was on the intubation, they started a protein feeding tube through the stomach. I mean, down her throat into her stomach.
Patrik: Through the nose.
Julie: Yeah.
Patrik: Yeah. I’ll tell you what I …
Julie: And is-
Patrik: Go on.
Julie: Is that normal? It’s actually through her throat, the feeding tube.
Patrik: Yeah. In the beginning, it’s normal. If it’s ongoing, they might do what’s called a gastrostomy, or a PEG. But, that’s not … It wouldn’t be urgent. I’ll tell you why they only started feeding her when she was intubated. I’ll tell you why. It’s probably important to understand. If she was on BiPAP before intubation, and they would have fed her, the risk for aspiration would have been fairly high. Do you know what I mean by aspiration?
Julie: Yes. That’s a lot of reason why they say she’s in here is that she aspirated at the nursing home.
Patrik: Oh, I see. That’s where the pneumonia came from.
Recommended:
Julie: Yes.
Patrik: Right. Okay.
Julie: The pulmonologist told us that the pneumonia was completely cured up now.
Patrik: Right. Okay. And then, when somebody’s intubated, it’s much easier to feed them, because the risk for aspiration is much lower.
Julie: Okay. And then, they should have immediately started doing an enema after starting to feed her, correct?
Patrik: Well, no, they should’ve started an enema after three days of not opening bowel. But, even prior to that, they should have given her some aperient.
Julie: The what?
Patrik: Aperient, or laxatives.
Julie: Okay, until way later. They didn’t give her laxatives until … I mean, Wednesday, Thursday, Friday, Saturday, Sunday, Monday, Tuesday. We’re looking at day eight, nine before we got laxatives on deck.
Patrik: Right. That should be standard medication from day one in ICU, to give a laxative. Should be standard.
Julie: We’ll have to check more on that, to make sure that they didn’t … Maybe they just didn’t tell us.
Patrik: Look, I would be surprised, frankly, if they didn’t give your mom any laxatives on day one. I would be very surprised.
Julie: Okay. So maybe we need to get to the bottom of that. And then, so you’re saying that there is a possibility that she could be on these antibiotics and possibly be a candidate for surgery.
Recommended:
Patrik: If they get the infection under control. So, I’ll give you … This is some examples there, so you can see the deterioration in the last 24 hours. The white cell count in the blood is the indicator for an infection. The white cell count in the blood went from 20 to 40, and normal is four to 11.
Julie: Wow. So …
Patrik: It’s basically doubled in the last 24 hours.
Julie: She’s also on steroids, too, which can cause that, right?
Patrik: Very much so. Is she on steroids when she’s not in hospital as well?
Julie: Yes. No, when she was in the hospital, no. When she was in the nursing home, she was not on steroids.
Patrik: Right. So, this is a new thing.
Julie: Yes. So, could that cause the white blood cell to go from 20 to 40?
Patrik: Potentially, but I can tell you what it can also cause. The steroids, often we can … If somebody’s on long-term steroids, it weakens them, for example … Have you ever seen somebody who’s on long-terms steroids? Usually their skin is really frail. Have you ever seen that?
Julie: I haven’t. But she hasn’t been on steroids for very long. She only got them since she’s been here.
Patrik: Right. Just a few days.
Julie: Not two days, but since she’s been here. I think they started her on steroids on Friday or something like that. Yeah, like, 15 days or 14 days or whatever. Yeah, almost as soon as she came in. I think they started on steroids once they saw how bad the pneumonia was.
Patrik: I see. And I didn’t ask that, do you know if she’s still on steroids at the moment? Do you know?
Recommended:
Julie: No. Did you say right now?
Patrik: She’s not.
Julie: Did you say is she on steroids right now?
Patrik: Yes. That’s what I was asking.
Julie: I think she currently is on steroids. Yes. I know they stopped the antibiotics, because they said the pneumonia was cured, and that the antibiotics ran its course, but then they started more today because of the current situation.
Patrik: I see. The other thing is …
Julie: Can you perforate a bowel from an enema?
Patrik: You could. Definitely. You could.
Julie: So, maybe the cause is the enema.
Patrik: Let me ask you … You know what I believe needs to happen next, you would have to speak to a gastric surgeon, because they’re the ones, probably, making the decisions whether she can go for surgery or whether she needs to go for surgery. Right?
Julie: Yes.
Patrik: But what I’m not concerned … I’m really not concerned about that they’re not trying. What I am concerned about, obviously, is what was leading up to this, like you. Why did they not … Why have they not been more proactive about bowel motion five days ago?
Julie: Yeah. And is there a way to come out of this ahead?
Patrik: There would be. They should know in ICU that for patients for open bowels, it’s critical, in order to prevent the situation that your mom is in now.
Julie: And now that we’re in this situation, do you feel that there’s still hope?
Patrik: Look, as long as there’s life, there is hope. For example, I tell you … At the moment, as far as I can see, your mother is in single organ failure. Now, what do I mean by that? At the moment, her lungs are not working, but all other organs are working. Okay?
Julie: Okay.
Recommended:
Patrik: The bowel is not an organ as such. The bowels are not working, and a lot of it will depend on whether the bowels are perforated or not. A lot of it will depend on that, in terms of taking the next steps.
Julie: So, if they’re not perforated, there’s a lot more hope than if they are perforated?
Patrik: Absolutely, because if they are perforated, bowel content will go into the abdomen. And if bowel content goes into the abdomen, it would be, basically, into the tummy area. That could really spread sepsis. It looks like your mom is already going into a septic shock which they are treating. But, if there’s bowel content spreading into the tummy, the only way, really, to handle that is by opening up the tummy and doing a big washout, but your mom would be too unstable at the moment. I argue she wouldn’t survive that. I argue that.
Julie: Okay. So, is there a sign in the positive that the nurse noticed that her tummy is not as hard? Like, if you had a perforated bowel, would your tummy get less hard?
Patrik: No. It would be rock hard. Absolutely. It is probably a good sign. He said yesterday it was much harder than today. And that could be a good sign, but at the same time, he says that the CT scan is sort of leaving them wondering are the bowel perforated or are they not perforated. That is something that the surgeon needs to decide, probably together with the radiography, whether the bowels are perforated or not and then make a decision from there.
Julie: So, if it is perforated and she can’t do surgery, are you saying that the comfort route is the way we go? Or are you saying we try to fight the sepsis, even though her bowels are emptying into her abdominal? How much time do we have?
Patrik: Yeah. So, I also asked him about sedation. Is she sedated? What is she sedated with? And so forth. I am not concerned about her comfort level, and I’ll tell you why. She’s on the Precedex, but she’s also on Propofol and Fentanyl, which is telling me she’s well-sedated, and I’m not really worried about her comfort level, unless you are telling me you don’t think she’s comfortable. Do you have any indication that she’s not comfortable?
Julie: Maybe not today other than the blood pressure going up if you touch her. But there are other … Like, yesterday, she got a furrowed brow, or her face is red and is sweating profusely, or they do say that they have to raise the sedation if she has panic attacks.
Patrik: Okay. But that’s not … What I’m looking for is she’s not lying in bed, potentially moving around because she would be in a lot of pain. You have not seen that.
Julie: No.
Recommended:
Patrik: Right. So, from that perspective, let’s just run through the worst-case scenario and run through the best-case scenario, as far as I can see with the information that I have. The worst-case scenario would be that they continue treating, but she’s going into septic shock. She would shut down. What do I mean by shut down? That the nurse, Mel, has already told me that she’s very cool in her legs and in her arm. That it’s a sign of septic shock. And, if they keep going up with the Vasopressors, the Norepinephrine and the Phenylephrine, and I don’t want to get you disheartened but you need to understand the mechanisms of the Phenylephrine and the Norepinephrine. It’s important for you to understand.
When somebody has a cardiac arrest outside of hospital, or in hospital, basically their heart stops. One way to reactivate the heart is with those medications, Norepinephrine and the Epinephrine, and your mom is on those drugs. Now, her heart is fine, however the septic shock causes her to become hypotensive, which means she’s currently having a very low blood pressure, and in all that, to manage that low blood pressure, they need to give her those drugs. And they are considered life support.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!