Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Katrina, as part of my 1:1 consulting and advocacy service! Katrina’s son is in ICU with lung collapse and on ECMO and Katrina is asking, why has the tracheostomy procedure been delayed.
My Son is in ICU with Lung Collapse and on ECMO. Why Has the Tracheostomy Procedure Been Delayed?
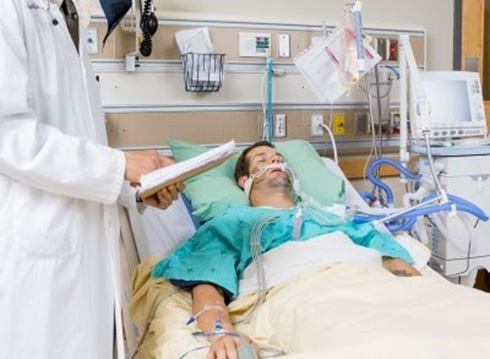
So Katrina has her son in intensive care on ECMO, now I will read out what Katrina wrote in her last email to me. So Katrina says it’s been six weeks now since my 36-year-old son was admitted to the ICU. He has blood clots on his lungs and the brain bleed. He received an ECMO for three weeks, and now he’s still on the ventilator. A tracheostomy was scheduled but he has lung collapse yesterday and he can’t hold steady oxygenation. I am really starting to get worried. He isn’t well enough for a CT scan. I am really scared. Please help me to understand what’s happening. And is there any hope.
RECOMMENDED:
So thank you, Katrina, for writing in and for being a client. So Katrina, here is the thing when your son has had some lung clots and some brain clots, so chances are that he would have been on heparin to thin his blood because, you know, if there must have been a circulation issue because otherwise, he wouldn’t have had those blood clots in the first place.
But you see, it all comes back to you don’t know what you don’t know, which is the biggest challenge for families in intensive that they don’t know what they don’t know, because intensive care is such a highly specialized area. And for any patients, let alone for a patient on ECMO. There are dozens, and I repeat that dozens of things happen, happening simultaneously that are all critically important. And that’s why, you know, if you haven’t worked in intensive care for decades as I have, you wouldn’t probably even know where to start. And the information that we often get for families is incomplete. And we can only make a complete assessment if we have all the relevant clinical information, which is why we need to speak to the doctors and nurses directly or review the medical records so that we can really help you.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
But anyway, to answer your question, Katrina, so one of the reasons that the tracheostomy was probably delayed as well is your son would have been on heparin. And when patients are on a high dose of heparin, you know, because of the blood clots, but also when patients are on ECMO, they are on heparin as well, because the risk when somebody is on ECMO, the risk that the ECMO tubes are clotting is very high. So, therefore, a blood thinner needs to be put into the mix to stop the blood from clotting.
So furthermore, with high PEEP and high oxygen requirements, because of the ECMO, the risk for doing a tracheostomy is reasonably high as well. However, they should have been able to control that risk of high oxygenation levels with the ECMO because, in theory, you could actually, in some situations, you could extubate the patient while they’re on ECMO. Because ECMO is doing all the work for the lungs and you could give the lungs a rest.
Okay, so as far as I can see with the information that you’ve shared Katrina, one of the reasons why your son cannot be having a tracheostomy yet is simply that he’s on heparin, and he’s got high oxygen levels or high oxygen demands on him while he’s on ECMO and that is a combination. That’s not great.
So the other issue that you’ve brought up is, you know, that he’s still on the ventilator after three weeks. So, you know, the question is, why is he still on the ventilator after three weeks. Was ECMO not giving him enough time to let the lungs recover? Because that’s the whole purpose often for the ECMO and VV ECMO is for lung failure. And that’s the whole premise of it to let the lungs recover so that you know, you can then eventually get your son off the ventilator and I’m not sure why it hasn’t happened. And that’s something we need to find out on our next phone call.
RECOMMENDED:
So, you know, you also mentioned that the tracheostomy has been scheduled but has been delayed. I did highlight that probably the combination of heparin as well as high oxygen requirements and high PEEP probably made it too risky for the ECMO for the tracheostomy to be done.
But on the other hand, the question is, you know, with the tracheostomy being delayed, that’s another risk because what happens is when somebody is having a breathing tube instead of a tracheostomy, they need to be in an induced coma. Most of the time because the breathing tube is so uncomfortable, which means the tracheostomy hasn’t been done, which means it’s less likely for your son to break up because he still needs to be in an induced coma or in a sedative state because of the breathing tube being so uncomfortable in his mouth. So you know, it’s not a good situation to be in for your son.
RECOMMENDED:
So the tracheostomy should be scheduled as quickly as possible. So he can be woken up can get out of the induced coma, and can start to breathe by himself, and then being weaned off the ventilator slowly. Now, you’re also mentioning that your son isn’t stable enough to go for a CT scan. Now, most patients on ECMO quite frankly, are very unstable. That’s the reality. And a lot of patients on the CT scan is going for a CT scan, I have been transporting many patients myself on ECMO to a CT scan, and most patients on ECMO are very unstable, but nevertheless, it’s a case of making it safe for them, providing the resources that are necessary to take somebody for a CT scan even if they’re unstable, and on ECMO.
You are also saying that you know, your son still has collapsed lungs, and that was another one of the reasons why your son didn’t have the tracheostomy. Again, your son may still be in an induced coma and on sedation. And if he’s not waking up and if he can’t breathe up, you know, the risk that he ends up with a Ventilator-Associated Pneumonia is pretty high, you know, so the tracheostomy is inevitable. And how do they treat the blood clots? That’s another question. How do they treat the blood clots mainly with again with the heparin that I mentioned before?
And you know, you also want to find out why he has those blood clots and why are they not going away? So you know, you also mentioned that because of the blood because of the lung collapse, he can’t hold steady oxygenation, which I would assume is oxygen saturation drops quite frequently, which would also show up in his arterial blood gases, probably with low arterial oxygen levels as well as high co2 levels. So the question is, why is that still happening after all this time, on ECMO?
RECOMMENDED:
You know, and he’s still not off the ventilator. So those are the type of questions you want to ask. Also, you want to look into if your son is still on any inotropes or vasopressors, to see if he’s on other life support, besides the mechanical ventilation. Inotropes or vasopressors are given for mainly low blood pressure over a weak heart. And you want to find out if that’s the case as well.
So you’re still having a lot of unanswered questions to look into to find out what’s exactly happening with your son and again, you should be looking at arterial blood gases. You mentioned the chest X ray, you also should be looking at the ventilator settings. What ventilator settings is he on, you see anywhere close to come off the ventilator for example, right. Other issues are you know, how likely is it that your son will need ECMO again and again that question you should be asking.
RECOMMENDED:
So, furthermore, you also want to find out when is the tracheostomy happening? You know, when is the tracheostomy happening? Is there any other timelines around when your son will have to tracheostomy because then he can come out of the induced coma, he can wake up. It’s also less likely for him to have any inotropes because sedation often reduces blood pressure. You also want to find out if the kidney function for few days is okay, a lot of patients that are on ECMO, and in an induced coma for prolonged periods, sometimes they go into kidney failure. So those are all the things you may want to look at.
RECOMMENDED:
So, I hope that helps Katrina. I know we’ve got a call scheduled in the next couple of days to find out what we’re going to do next and whether we need to talk to the doctors again, to get the outcomes that you will need and you know, that you will need for your son and more importantly, that you really understand what is exactly happening while your son is in intensive care.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!