Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
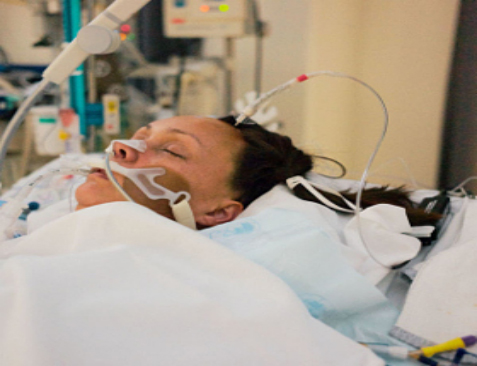
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tim as part of my 1:1 consulting and advocacy service! Tim’s mother had gastric surgery and has COPD in the ICU for pneumonia and Tim is asking if his mum can come off the ventilator soon.
My Mother Had Surgery and Has a History of COPD. Will She Be Able to Recover Soon?

Patrik: Intensivecarehotline Patrik speaking, how can I help?
Tim: Good day. Just going through your website there, and just seeing about the tracheostomy. My mom had a tracheostomy at the hospital.
Patrik: Right. Are you … Go on, sorry.
Tim: And obviously they’re sort of making out she’s not getting much better. She got, what do you call it, pneumonia, but it was aspirated pneumonia.
Patrik: Right.
Tim: She had a tracheostomy almost two weeks ago now. The trauma ICU get her off it but she’s still a bit wounded. She has got COPD as well. They’re just saying, “Look …” you know. She had a major operation.
Recommended:
Patrik: What did she have?
Tim: She had gastric surgery.
Patrik: Right, okay. My goodness, I see. So, how long ago did she go into ICU and when did she have the tracheostomy? Two weeks ago, ICU, or two weeks ago tracheostomy?
Patrik: Right, my goodness. I’m so sorry to hear that. I’m so sorry to hear that, that’s terrible. That’s terrible, that is disgusting. So, when you say, just let me ask you … Right. Right, okay. Let me ask you this, because you obviously found our website, we have a couple of websites. Intensive Care at Home, or Intensive Care hotline? At home? No, that’s great. You’ve come to the right place.
Patrik: Right. Well, thank you. Right, that’s great. Good, that’s great. Yeah, absolutely. Whereabouts, are you? Are you in Briston, or in Queensland? I see, which hospital is she at in Sydney?
Patrik: Right, I’m not surprised what I’m hearing there because we’ve had clients before at Stamford. They’re very, very negative now, very negative. So, if she wants to go home, would that be in Sydney, or would that be in Queensland? In Sydney? Okay.
Patrik: And you have private health insurance, that would help. But even without private health insurance, I can tell you that, for example, we get funding for our clients through the department of health, mainly in Veinport at the moment, but we are submitting proposals to the department of health in New South Wales, as well. Whatever they’re telling you that she’s too sick, she’s too much work, the reality is, some of our services are funded. From their perspective, what you said, like, they think it’s not worthwhile. Like, who are they to judge?
Patrik: Right, absolutely. How old is your mom? That’s not very old. Who’s the professor? No, don’t know him. We’ve dealt with Stamford before. They’re a nasty bunch there from my experience. But that shouldn’t stop you from doing what you’re doing. From my perspective, it’s doable. The next step would be to either talk to your private health fund, or to the department of health in New South Wales. But you might be luckier going to the private health fund, and I’ll tell you why.
Patrik: The private health fund now, they would be paying $5,000 today roughly for the bed in ICU. So, if we went back to the private health fund and said, “Look, you’re paying $5,000 per day for this ICU bed, we can cut the cost by more than 50%.”
Patrik: This is a win-win. Your mom is in an environment where she wants to be, the health fund is slashing 50% of the cost, and the ICU has an empty bed. Does that make sense? It’s a win-win. You want to get your mom out, she probably wants to go home. We’re slashing the cost for the health fund by 50%, and the ICU has an empty bed. Everybody’s winning.
Recommended:
Patrik: Okay, yeah. So that they continue to pay? Yeah, that’s-
Patrik: I see. So, now she’s at Stamford? But she’s a private patient there? Okay, yeah. I think that would help your cause. I think being a private patient would help your cause. And it’s good that HCS is continuing to pay. Usually we’re finding that the private health funds, if the ICU stays for longer than expected, they tend to pay, there’s no issues. But again, they would have an interest in cutting the cost if there is an alternative. So, how many days did you say in the hospital, 70 days? 7-0?
Patrik: (silence)
Patrik: Intensivecarehotline. That’s all right.
Tim: If I touch it, yeah.
Patrik: No, no, that’s all right. That’s all right.
Tim: The NBN.
Patrik: Pardon?
Tim: NBN. It’s the NBN network.
Patrik: Oh, right. Fine.
Tim: So that alright.That was on November 23rd-ish. They took the Fentanyl away, and the only thing she was having was just the food thing through the nose, and a drip, and she’s got a patch on, the lowest patches to get through pain. I was talking to her about getting a week extra there, because the tracheostomy is probably not that long. It’s been two weeks of the tracheotomy. Two weeks on Monday.
Patrik: Have you mentioned to the ICU that you are considering taking her home if they can’t take her off the ventilator? Is that something you have mentioned to them?
Tim: I did. And then they got someone out from the hospital there from the respiratory ward, and they said that it’s all too much work and she’s not a candidate for it.
Patrik: That’s all right. I wouldn’t worry about that now too much, because they haven’t used our service yet, so they don’t know what’s possible, really. I would think that the next step is for you to tell them that you want that, and that you will contact your health fund. Are you the next of kin for your mom? Are you the medical power of attorney?
Tim: Yes.
Patrik: You are?
Recommended:
Tim: Yes.
Patrik: That’s good. So, the next step is to contact the health fund. The other thing-
Tim: Before I speak to the hospital or …
Patrik: I’d probably do it simultaneously. You can say that you found someone who can do that, you know? What you need is, you probably will need a letter from them about her current situation to go back to the health fund, but it’s a matter of really making that argument. Also, when you talk to the hospital, make sure they know there’s something in it for them as well, which is the empty bed.
Tim: Oh, I understand there, like put a positive spin on it.
Patrik: Right. But if you want to set up a meeting with them, I’d be very happy to dial in over the phone to tell them more about what we do. Have any trouble, on this number. I’d be very happy to do that.
Tim: Right. You’re not 24, or you’re not seven days a week or …
Patrik: No, no. I’ll tell you, we provide … Okay. So, if your mom was to go home on a ventilator with the tracheostomy, we can provide 24 hours a day. If she goes home from ICU from 24-hour care with those high needs, she will need 24-hour care. Unless you are saying as a family, “Oh, we could do some of it ourselves,” but I can tell you from my experience, it’s very difficult.
Tim: Yeah. I think if she gets out of there and gets a bit more physio, because they don’t really do the physio, they’re not really worried about trying to get her strength back up. They’re just really sort of focusing what’s up on the lungs. It seems a bit strange, but they’ve said they’ve got rid of most of the stuff and there’s no infection, and this and that.
Recommended:
Patrik: That’s good. That’s good. But keep in mind, with the ventilator and the tracheostomy it’s an unstable airway. To give you an example, we have patients at home that don’t have a tracheotomy and a ventilator, and they have an unstable airway because they stop breathing. So, imagine … What I’m saying, there’s a reason why she’s in ICU and that reason is the ventilation, you know?
Tim: Yes.
Patrik: It’s going to be high risk going home without support, right? Your mum would bounce back to ICU quickly. Whereas, our number one goal is to keep patients out of ICU, otherwise we wouldn’t be in business.
Tim: That’s right. I understand. So, what would be the out-of-pocket expense to you guys for us, roughly? Or does the health fund it?
Patrik: Now, I can tell you that all of our clients are not out of pocket. We have no clients that are out of pocket. Bear in mind-
Tim: Ok, go on.
Patrik: Bear in mind, they are funded through the Department of Health. If you were to get HCF to cover, there could be out-of-pocket expenses, but that’s why we need to start approaching them to find out what the options are.
Tim: That sounds good.
Patrik: Right. And you may have to get a letter from Stamford about her current situation, but they may have that already. You know, Stamford-
Tim: They would have it?
Patrik: … They would have it because HDF wants to know, why is she in ICU?
Tim: I’ve got pretty much the same letter.
Recommended:
Patrik: Yeah. So, they would be aware why she’s in ICU.
Tim: That makes sense, doesn’t it? Yeah. They would already have a copy of that.
Patrik: Sorry?
Tim: It makes sense. They would already have a copy of that-
Patrik: Yeah, they would, and if they-
Tim: Even if they would do full works on that.
Patrik: Right, right. And if they don’t, they would ask for one. But by the same token, parallel to this, your private health fund is probably your first go-to organisation, but the next step is then to go to the Department of Health.
Tim: Yes, I understand that.
Patrik: Right. What was your name again?
Tim: Tim.
Patrik: Tim, okay. So, those would be the next steps, telling the ICU about your plan, as well as talking to the health fund.
Tim: Okay. That’s what I’ll do then, yeah.
Patrik: I can also tell you that the first response you might get from ICU, as well as from the health plan, is a no. That may be the first response, but in a situation like that, you can’t give up. So, don’t let that stop you.
Tim: So, what would be their options then? Wouldn’t they say, “Oh, look, it’s not worth it?” What do they do, just drag my mom off and then just slowly neglect her or something?
Patrik: The worst-case scenario-
Tim: Or transfer her to another ward.
Patrik: That could happen, that they will try and move her out to save costs, but then she won’t have the skills on a ward she will need, which is then a risk for deterioration, right?
Tim: Yeah.
Recommended:
Patrik: For example, if they moved her to a ward on a ventilator, again, there’s a very high chance she will deteriorate and potentially bounce back into ICU. What they might try and do is not readmit her to ICU, and that’s where you need to be vigilant.
Tim: Okay. Because half the time they have two family meetings and just sort of try to paint a bad picture and all that sort of stuff.
Patrik: I wouldn’t-
Tim: Yeah, I know. After reading your stuff, I stayed up all night, Patrik, and it was good, actually. You sent me an email, as well, and I learned a lot from that, as well. And I just sort of stuck by my guns. They wanted me to sign the “do not resuscitate.”
Patrik: Good, good.
Tim: I said no way.
Patrik: Good.
Tim: And that was when mum was in an induced coma. Because I had a feeling that … I just sort of sensed. I remember you saying about read the body language and just have a feel of the vibe around the ward, and I sort of sensed it there. It felt like it was all too hard. “What’s the point,” sort of thing.
Patrik: Absolutely. And I can tell you that if … We’ve had two clients in the past at Stamford. And when I mean clients, not for intensive care at home, we were doing consulting and advocacy through the hotline. So, we never went in there with intensivecareathome but I can tell you they’re butchers there.
Tim: Wow. Good to know.
Patrik: They’re horrible. They’re horrible, and you would have seen some of that already.
Tim: Yes. Yep. They’re a bit blunt.
Recommended:
Patrik: So, then that-
Tim: Good day, Patrik. Sorry, it’s put off again.
Patrik: That’s all right. That’s all right. They are vultures there, you have to be quite assertive.
Tim: Right.
Patrik: But there is a way forward.
Tim: That’s good news.
Patrik: There is a way forward, but we will have to be very persistent. Okay? Are you there?
Tim: Yes Sir.
Patrik: We will have to be very persistent though.
Tim: Okay.
Patrik: Tim, I have to run in a minute.
Tim: Well like I said, I appreciate I didn’t get to talk to you personally.
Patrik: That’s all right. What’s your mobile number?
Tim: Hang on a sec. Hang on a sec.
Recommended:
Patrik: Okay. Tim, let me know what you want to do next. Very happy to help.
Tim: Well, I need to fix that right?
Patrik: Right. And it will probably help for us to go back to HDF with you. Because you will need some support there. What are your plans? Are you going to Sydney any time soon or?
Tim: Yes. Tomorrow at lunchtime. I’ll just pack a lunch then.
Patrik: And are you having a meeting lined up with them tomorrow?
Tim: And I said, no I’m looking for
Patrik: If you do want to have a meeting it needs to be on your terms.
Tim: I agree.
Patrik: And your terms are you want your mum at home.
Tim: That’s right. Is it just something on the phone and–
Patrik: They need to understand what we are providing. And they need to understand what’s in it for them.
Tim: And you got a point there.
Patrik: I think the next step is gauge the situation tomorrow. Okay? The other thing that could happen is she might well get off the ventilator. You know, you don’t know. She may–
Tim: They’re trying to do venting again today. They didn’t counsel us about it. I think because I had a phone conference yesterday at Family meeting with them.
Recommended:
Patrik: What I can help you with is and potentially, If she wasn’t going home. If she comes off the ventilator. Do you need help to manage the dynamics? I can certainly help you with that too. I’ll give you two scenarios. I’ll help you with getting her home with intensive care at home. I can certainly help you with that. And I won’t charge a fee there because if we provide service we will–but if you want me to help you with managing the dynamics there then I would charge the consulting fee. But I’ll tell you now the goal is to get your mum home. Why don’t we talk tomorrow? Get in there tomorrow and gauge the situation and then we can see what the next steps are.
Tim: Okay, so I’ll just give you a call sometime tomorrow. Absolutely.
Patrik: All right.
Tim: Awesome. I really appreciate it.
Patrik: Okay, thanks a lot, Tim. All the best for now. Take care. Bye.
Tim: Take care. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!