Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Wife Had a Brain Death Test in the ICU. Why Did They Do That Without my Consent?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients as part of my 1:1 consulting and advocacy service!
It’s also a question we get quite frequently from our readers and clients!
WHAT IS VENTILATOR ASSOCIATED PNEUMONIA (VAP)?
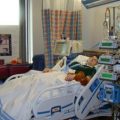
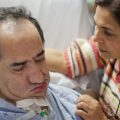
- Ventilator-associated pneumonia (VAP) is pneumonia that develops 48 hours or longer after mechanical ventilation is given to the patient by means of an endotracheal tube or tracheostomy.
- Ventilator-associated pneumonia (VAP) results from the invasion of the lungs by microorganisms. Intubation compromises the integrity of the oropharynx and trachea and allows oral and gastric secretions to enter the lower airways.
- VAP is a subgroup of hospital-acquired pneumonia.
- VAP applies to patients with an endoctracheal tube or a tracheostomy tube – does not include patients receiving non-invasive ventilation (NIV).
- Is a common complication in ICU (15-20% incidence if >48h ventilation).
- A gold standard test for diagnosis does not exist.
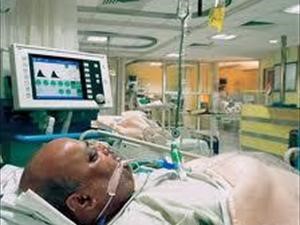
WHAT CAUSES VAP?
PATHOGENESIS
Events leading to VAP:
- Colonization of the oral cavity, upper airway, endotracheal tube and circuit with pathogenic organisms
- Passage of pathogenic bacteria from the above sites into the lower airways through aspiration or microaspiration of secretions and suction catheters.
Endotracheal cuffs
- effective at preventing macro-aspiration
- small folds on the surface of the cuff act as conduits for microaspiration of secretions pooled above the cuff
- In older patients, who may have tracheomalacia, there may be a leak around the cuff despite high intra-cuff pressure
CAUSATIVE ORGANISMS
- < 48 hours in hospital – often community organism
- 48 hours – 5 days – community + hospital organisms
- 5 days – often hospital grown multi-resistant organisms (MROs) such as methicilin-resistant Staphylococcus aureus(MRSA) and Gram-negative bacilli (GNB):
- Pseudomonas aeruginosa
- Klebsiella
- Enterobacter
- Acinetobacter baumannii
- Stenotrophomonas maltophilia
HOW TO PREVENT VAP?
IMPLEMENTATION
- Multidisciplinary Team (MDT) approach with staff commitment (doctors, nurses, infectious diseases team, physiotherapy, management)
- Recognition of the problem (determine VAP base rate in the unit)
- Identify interventions that improve outcome
- Educate staff (nursing education shown to decrease VAP incidence)
- implement preventative strategy as a ‘bundle of care’ with ongoing education and reminders
- audit and feedback results

INFRASTRUCTURE AND GENERAL MEASURES
- Infection control: hand hygiene compliance, cross control of infection, surveillance, close communication
- Antibiotic cover: adequate cover to reduce risk of Methicillin Drug Resistant (MDR) organisms
- Good staffing levels: decreases cross contamination
- Environment: targeted environmental sampling, disinfection during outbreaks
PATIENT CARE
Prevent colonization of the upper respiratory and gastrointestinal tract
- Good oral care (use 0.12-0.2% chlorhexidine twice daily with a sponge swab, brushing teeth)
- Oropharyngeal decontamination or selective digestive decontamination (reduces VAP rate but generally not used due to concern over MDR organism selection)
- Stress ulcer prophylaxis only when indicated (i.e. high risk: burns, traumatic brain or spinal cord injury, severe sepsis, coagulopathy and those receiving steroids equivalent of hydrocortisone > 250mg/day; or active peptic ulcer disease)
- Silver coated ETT shown to decrease the rate of VAP
- Probiotics (decreases VAP).
Prevent aspiration
- Maintain the head of the bed at 30-45° unless contraindicated (decreases VAP)
- Subglottic secretion drainage (SSD) (decreases VAP with NNT = 11 if ventilated for more than 24-48h, but when combined with head up nursing no difference observed)
- maintain ETT cuff pressures between 20-30 cmH2O, check q4h
- No benefit from ultrathin or tapered cuff endotracheal tubes (Jaillette et al, 2017)
- Consider early gastrostomy if indicated (may decrease microaspiration)
Minimize the duration of mechanical ventilation
- Assess readiness for extubation daily
- Optimize use of sedation and analgesia (avoid oversedation, decreases time on mechanical ventilation and thus VAP)
- Early mobilization
- Early tracheostomy (data controversial, only applicable to selected patients e.g. neurosurgical patients, high spinal patients)
- Use NIV (Non Invasive Ventilation) if appropriate (decreases VAP)
Endotracheal suction, humidification and care of the circuit
- Endotracheal suction when airway secretions are present (closed and open suction with a single use catheter are equivalent)
- Humidification and heating of the inspired gases (HME vs heated humifiers: data conflicting, considered equivalent if heated humidification with heating wire in the inspiratory or both limbs of the circuit is used to prevent condensation)
- Avoid routine ventilator circuit change (frequent changes doesn’t change VAP rate)
REFERENCES:
- Critical Care Compendium | Ventilator Associated Pneumonia (VAP) https://lifeinthefastlane.com/ccc/ventilator-associated-pneumonia-vap/
- Ventilator-Associated Pneumonia (VAP) http://www.patientsafetyinstitute.ca/en/Topic/Pages/Ventilator-Associated-Pneumonia-(VAP).aspx
- Ventilator-Associated Pneumonia Overview of Nosocomial Pneumonias https://emedicine.medscape.com/article/304836-overview#a11
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!