Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer the succeeding questions from one of my clients Peter as part of my 1:1 consulting and advocacy service!
They gave Lasix to my Dad in the ICU but he produced inadequate urine. Is he at risk for pulmonary oedema?
You can also check out previous 1:1 consulting and advocacy sessions with me and Peter here.
Patrik: Yeah, that’s exactly right. If they gave him albumin, and he’s not making urine, that could cause trouble. That could get him into pulmonary oedema relatively quickly, especially with-
Peter: Now-
Patrik: … Especially with his heart-
Peter: …Now if it causes trouble, is the medicine have to blame for this? The … What’s it called? Is it Lasix? Is that typically the cause of this type of thing?
Patrik: No, it’s usually a combination of the hypotension and … Has your dad been on Lasix before? Do you know?
Peter: Oh yeah, he was taking 10 milligrams a day.
Patrik: At home?
Recommended:
Peter: He was doing fine. He was taking in about 2200, between water, free water, and what do you call that stuff, the feeding solution.
Patrik: Oh yeah.
Peter: And he was putting out 14 to 15. He was putting out about 1400 a day.
Patrik: Mm-hmm (affirmative).
Peter: Sometimes 1800. He had beautiful kidneys.
Patrik: Yeah, the-
Peter: But the Lasix, 10 milligrams never bothered him.
Patrik: Right.
Peter: 20, he was on 20 before. That didn’t bother him, and they doubled it to 40.
Patrik: Right, right.
Peter: And that was it.
Patrik: The other thing that I am wondering and she didn’t mention anything yesterday, whether … What antibiotics he’s getting? Sometimes the antibiotics can cause kidney issues too.
Peter: He’s getting Cipro.
Patrik: Cipro, yeah. Cipro usually doesn’t. The worst antibiotic for kidney failure is usually Gentamicin, but they haven’t mentioned that, so …
Peter: Yes, I’ve heard about that nasty one, yeah.
Patrik: It is very nasty.
Peter: That one’s bad. They say even too, that what-do-you-call-it, isn’t exactly easy either. The big, heavy-hitter they use. What’s the big one that they use? The number … The biggest … Vanco.
Patrik: Oh, Vancomycin, yeah, Vancomycin.
Peter: Yeah, yeah. He’s been on that.
Patrik: Yeah, that’s toxic, for the kidneys.
Peter: He was on that for about a week.
Patrik: Right, right, and that could cause kidney problem, and how long ago would he have been on Vancomycin? Was that recently?
Peter: Yeah, in this past admission and they’ve done of this.
Patrik: Ah, okay. Yeah, and that could cause-
Peter: They watched him though. They watched him really well. His creatinine stayed good. 1.1, 1.2, they told me. It didn’t go up. They watched it every day, and they’d do the Vanco levels too.
Patrik: Yeah, but that’s … There can be a delay. So with Vancomycin and the hypotension, and the furosemide, that could be enough to set him off into renal failure, but again, I would wait-
Recommended Articles:
Peter: So what- … I’m sorry, go ahead.
Patrik: I would wait another 24 hours, and if by tomorrow he hasn’t made any urine, he needs to go on dialysis.
Peter: What do they do with the dialysis? Do they …? How will they get that started? What do they …? They put the …? I forget what … I remember fistula in their arms, but that was the long term patients.
Patrik: Yeah, that’s right.
Peter: When you have an emergency like this, what vessels do they use?
Patrik: Yeah, so your dad would have had a central line in ICU. Have you heard of that?
Peter: Yeah. Right now he has a PICC line.
Recommended Links:
Patrik: Yeah, yeah. So if he goes on dialysis, he needs what’s called a vascular catheter and that’s similar to a central line, just the lumens are a bit bigger.
Peter: Where do they put that, is in his arm?
Patrik: Probably neck or groin.
Peter: Oh yeah, the sub- … Yeah, I remember now that you mention it, yeah, and that’s just an emergent type thing? Isn’t that just like and inside, and an outside type thing?
Patrik: The end goes inside. It’s pretty much like a central line, just not as long, and probably the diameter is a little bit bigger.
Peter: So how long would they leave that in, then? You’re saying until his kidney function comes back?
Patrik: Pretty much, yes, pretty much, yes.
Peter: So why wouldn’t the water … and I know you’re the right one to talk to. From what you understand, Patrik, where does all that water go? Why doesn’t it filter through the kidneys? You know the principle there?
Patrik: Yes, the principle is … So they wanted to give him albumin, okay? So his albumin level is low, and once the albumin level is corrected, all the water from the tissue will be drawn back into the vessels, into the blood vessels. That’s how it works. So I can see why-
Peter: Why he wasn’t able to do that?
Patrik: I can see why they don’t want to give him albumin yet, because if they give him albumin and his kidneys are not working, he could go in to pulmonary edema relatively quickly, if that makes sense.
Peter: Right, because they wanted to try the 1500 of saline, and they said Dad only produce about 60 to 100 of urine, he didn’t have enough urine, and it’s-
Patrik: That’s right, but you’ve got to try those things, to make sure that … Sometimes, if you give 1500 of saline, the kidneys start working. Sometimes it’s just a perfusion problem, but that doesn’t seem to be the case, if they’ve tried that and failed.
Peter: Yeah, I think they’ve … I mean, I don’t know what’s been … Like I say, I don’t know for sure what happened to him, but it seems like he’s had plenty of fluid. Like, his pressures have been good.
Patrik: Hmm.
Peter: I would think … I mean, what I know, what’s going on down there, but-
Patrik: I think you have a very good understanding of what’s going on.
Peter: I don’t know.
Patrik: I think you have a very good understanding of what’s going on, as far as I can see. You’ve picked up-
Related Links:
Peter: The basics. I only know the basics.
Patrik: Yeah, but you’ve … The next step is, he’s waking up slowly, from what you’re saying, and the next step is to … He’s out of bed, which I think is great, too. And the next thing is to get his kidneys managed.
Peter: Right. So why, theoretically now, I know from what you’re … From what you’re trained to understand about why as the water comes in, say he’s at 20, and blood flows to his kidneys.
Patrik: Yep.
Peter: What would be inhibiting him from peeing? Because, did the Lasix screw some chemistry up down there, or something?
Suggested Links:
Patrik: Yeah, the Lasix might have-
Peter: Theoretically.
Patrik: The-
Peter: Theoretically.
Patrik: The Lasix might have, but I think it’s more the hypotension, because 40 of Lasix, or … Yeah, he’s had in ICU, is not a lot. But, if he’s been taking Lasix at home even, for a period of time, which might cause some slight damage as well. And now, with the hypotension, that might have just been too much for the kidneys.
Peter: But I mean, he hasn’t had hypotension in days.
Patrik: But, didn’t you say-
Peter: His blood pressure’s been fine.
Patrik: Yeah, but you-
Peter: And his kidney? I’d say his kidney function was doing alright.
Patrik: Right, but you were telling me-
Peter: For the last couple of days.

Patrik: Right, but you were telling me earlier, he had hypotension in ICU, and he had epinephrine.
Peter: Yeah, but that was like about three days ago.
Patrik: Yeah, but that’s-
Peter: About three or four days ago.
Patrik: Yeah, but that would be … Often kidney failure doesn’t show up straight-away.
Peter: Oh, I see.
Patrik: It doesn’t show up straight away.
Peter: Oh, I hope not, but I mean, well how do the … If the kidneys are …? How could they theoretically come back? Do they just have to rest, like any organ?
Patrik: Very much so. They need to rest, and they need to be … With the dialysis machine, they will get that rest.
Peter: They will get what?
Patrik: If he’s going on a dialysis machine, the kidneys will get that rest.
Peter: Oh, okay. I see.
Patrik: Right.
Peter: By resting the … Maybe they’ve been working too hard, huh?
Patrik: That’s exactly right. That’s exactly right. And that’s what I think, in the next 24 hours, if he’s not peeing, that’s what I think needs to happen. They need to start him on the dialysis.
Suggested Articles:
Peter: That can be done … That doesn’t take a lot. That could be done as soon as they put the needle in there, they can-
Patrik: They can start.
Peter: Do it right away, right?
Patrik: Absolutely, absolutely.
Peter: There’s no … The good thing about it, you know, is that if he ever needs dialysis, and he’s a veteran, and there’s a Boston VA. It’s really one of the best, as far as dialysis units. The doctor that runs that is one of the best around.
Patrik: Right.
Peter: I used to work with him.
Patrik: Right.
Peter: Like I say, I spent 15 years in there.
Patrik: Right.
Peter: So that’s the first thing I’d do, is get Dad in there.
Patrik: Right, right.
Peter: He’s a veteran, you know.
Patrik: Right, and again-
Peter: I’d use it.
Patrik: He may not necessarily need ICU, he may just need … Go on a dialysis ward. There’s probably no need for ICU, but that’s something that needs to be seen.
Peter: I just hope they didn’t have to … I’ve always hoped and prayed his kidneys wouldn’t … That was one of the best things about him. If I had known that, that he had stage-three kidney disease, I would have had him seeing a nephrologist, or a … much more frequently, to protect his kidneys, you know?
Recommended Informations:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: But, they would have taken regular bloods, on your dad, because of the Warfarin. So, I’m wondering whether this is really new, because with the Warfarin, he would have had regular checks for his INR, and that means if he had stage three kidney disease, they would have seen that in his blood results. So, this could well be new, and it wouldn’t surprise me if it was new.
Peter: I know his INR’s about 1.9, they told me.
Patrik: Right, right.
Peter: Normally, it was supposed to be between 2.5 and 3.5, because he has that antiphospholipid syndrome that … Did you ever heard of that?
Patrik: I haven’t. What’s the syndrome called?
Peter: It’s called antiphospholipid.
Patrik: Right. No, I haven’t.
Peter: Have you heard that one?
Patrik: I haven’t, actually.
Peter: It’s for people whose blood is genetically thicker than most people.
Patrik: Right.
Peter: It enters a small hole, and it’s tied to a PFO, so-
Patrik: Right.
Peter: Anyway, I thought I’d run that by you, and see what you thought.
Patrik: Yeah, I think for now, for now, just make sure that they’re prepared to either take him back to ICU for dialysis, or to do the dialysis on the renal ward. I think that would be some of the boxes that I think they need to tick.
Peter: Should I push hard, or let them manage him, and not … I should probably mind my own business, I think, and not interfere?
Related Articles:
Patrik: Look, I think just get a feel for what they’re trying to do. Get a feel for whether they want dialysis or not. As far as I understand, yesterday when I spoke to Erica, there are no treatment limitations. So, that means there’s no reason why your dad shouldn’t get dialysis.
Peter: Right, right when she was talking to you though, he was putting out a decent amount of urine.
Patrik: Right.
Peter: It was after she left, then he never made any more, and he started having some blood coming out, and Jesus. Anyway, I’m pushing to get a kidney doctor in here to look at it, and just intercede. It’s a weekend too. That stinks, because the staff … I don’t know how you guys work on your end, but on weekends, all the attendants go away. They leave it up to the residents to run everything.
Patrik: Right, right.
Peter: So …
Patrik: Yeah, and if you feel more comfortable having a nephrologist there, by all means, I think you should get one.
Peter: Yeah, I’ve been pushing for it, but … Anyway, I just thought I’d run it by you, and see if you’ve seen this before, and maybe what to expect, or what to ask for, you know?
Patrik: Yeah, definitely seen it before, and I would imagine, again, 90% of people who go on dialysis, has intermittent dialysis. They will have dialysis while they are critically ill, sort of thing.
Peter: Alright, I was just wondering, do they ever have any treatments for this? Like medications, or?
Patrik: The standard medication really, is Lasix. That is standard. There is nothing else. There’s nothing else. So, if the Lasix doesn’t work, he really does need dialysis.
Peter: Alright. What about giving him more fluids? That’s not good?
Patrik: It could be risky, with is cardiac failure, and with the pneumonia, and by already having fluids on board. That could be setting him off, back on the ventilator, and they want to avoid that at all costs, because he’s … They don’t want him to go back on a ventilator, which is probably the biggest risk out of all.
Recommended Links:
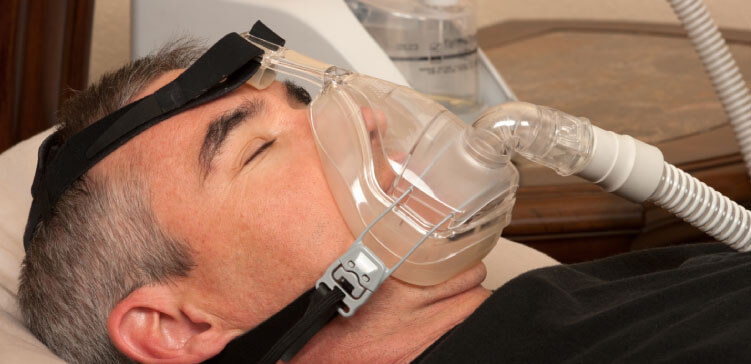
Peter: Right, well he actually never made it to a ventilator, but he was almost going to go. But, they managed to keep him off of it. He used CPAP last night for the first time.
Patrik: Right.
Peter: It didn’t bother him too much. It didn’t bother him too much, he survived the CPAP.
Patrik: Right.
Peter: That’s at least one, little, progress there.
Patrik: Absolutely.
Peter: So he has a better sleep with CPAP.
Recommended Topics:
Patrik: Right, and did you stay with him last night?
Peter: Oh yeah, I stayed. Yeah, but I fell asleep halfway though.
Patrik: I bet, I bet.
Peter: It’s just awful timing, to see him …
Patrik: Right.
Peter: It’s awful, you know
Patrik: Yes. Does that help, Jim? What we’ve talked about?
Peter: Yeah, a little bit. Yeah, a little bit.
Patrik: I-
Peter: Like you say, it’s maybe … What helps is when you said that a lot of these patients have to … And that it may be temporary.
Patrik: Yeah.
Peter: That they have to do dialysis.
Patrik: That’s right. It’s often part of the ICU admission, unfortunately.
I can tell you, I’m … As I said to you, I’m on a night shift, and I’m looking after a patient tonight, and they had a lung transplant. They are in kidney failure. They are on a dialysis machine. That’s nothing out of the ordinary at all.
Peter: Yeah? What’s that, three hours for it? Three hours? Is it three hours, three times a week?
Patrik: Four hours. Yes, three hours … No, no. Sorry, sorry. Three times a week, like it’s usually for a whole day, but they may have to be a little bit more aggressive whilst he’s in hospital, to sort of do a little but if ICU treatment, and then get him to the ward. It’ll come out in the next 24 hours. They’ll keep an eye.
Recommended:
Peter: Yeah. Alright now, I’ll let you go. I don’t want to hold you-
Patrik: Not at all, not at all. It’s been a pleasure. It’s been a pleasure helping you, and let me know when you need to chat again.
Peter: Okay, alright then.
Patrik: Okay.
Peter: You take it easy, now, alright?
Patrik: And you. All the best. You look after yourself. Thank you.
Peter: Yeah, I know, that’s true.
Patrik: Yeah, you-
Peter: Alright, we’ll see you now.
Patrik: Okay, take care. Bye-bye.
Peter: Okay, Patrik. Bye-bye. Bye.
Patrik: Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!