Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another frequently asked question from our readers and the question this week is
What are reasons for not being able to come off the ventilator/respirator?
A lot of families of critically ill Patients in Intensive Care come to our website because they have a loved one in an induced coma with a breathing tube and on a ventilator.
Others come to INTENSIVECAREHOTLINE.COM because they have a loved one critically ill with a tracheostomy and on a ventilator.
Therefore, the answer to the question “What are reasons for not being able to come off the ventilator/respirator?” needs to be looked at from two different ankles.
In either situation, if your critically ill loved one is on a mechanical ventilator with a breathing tube (Endotracheal tube) or on a mechanical ventilator with a tracheostomy there can often be delays in coming off the ventilator.
Let’s look at both situations in more detail.
1. Not being able to come off the ventilator with a breathing tube (Endotracheal tube)
Whenever a critically ill Patient is induced into a coma, mechanical ventilation with a breathing tube (endotracheal tube) is mandatory.
Therefore, no induced coma without mechanical ventilation and the breathing tube (endotracheal tube) and vice versa.
There is the odd exception to the rule where critically ill Patients are being mechanically ventilated with a breathing tube(Endotracheal tube) where they are not induced into a coma and this is usually only the case when they have sustained brain damage or if they are unconscious already.
In both circumstances, having a breathing tube(Endotracheal tube) and being mechanically ventilated can lead to being unable to come off the ventilator.
Therefore, the reasons for being unable to come off the ventilator after an induced coma when being on a breathing tube (Endotracheal tube) can often be related to your critically ill loved one not having “woken up” after an induced coma, despite the sedatives and Opiates (=pain killers) being ceased.
Therefore, not being able to come off a ventilator with a breathing tube(Endotracheal tube) is often a direct result of not “waking up” after an induced coma.
Related articles/videos:
Other issues that lead to the inability of not being able to come off a ventilator and the breathing tube(endotracheal tube) are simply airway diseases like COPD, Asthma, Pneumonia, ARDS (lung failure) and also other critical illnesses such as lung transplantation, Guillan Barre syndrome, Cardiac arrest, Heart attack, Stroke, Sepsis, Heart transplant, liver failure, Pancreatitis, Seizures, Traumatic brain injury etc… Also, issues like airway swelling after trauma or Ear-nose and throat surgery can delay extubation (=removal of the breathing tube).
You always have to keep in mind that a critical illness is a severe issue and therefore often leads to the inability to breathe and hence mechanical ventilation support and the breathing tube (Endotracheal tube) is required.
Therefore, any prolonged critical illness with an induced coma can lead to a critically ill Patient not being able to come off the ventilator /respirator with a breathing tube (Endotracheal tube).
What are time frames that one should be looking at in when a critically ill Patient should come off the ventilator with a breathing tube (Endotracheal tube)?
The answer is that it all depends.
Usually when it comes to critically ill Patients that are ventilated with a breathing tube (Endotracheal tube) and once they are out of an induced coma they should “wake up” after about 48-72 hours at the latest, but again it depends on a number of factors, including the nature of the critical illness as well as the sedatives and the opiates (=pain killers) being used in how quickly they “wake up” and when they can be taken off the ventilator/respirator.
Therefore the answer is really often dependent on the nature of the critical illness and in how quickly your critically ill loved one can “wake up” after the induced coma and if there are any other airway/breathing or respiratory issues.
If you’re loved one can’t come out of the induced coma because they are not “waking up” after the induced coma and hence there is a delay in extubation (=removal of the breathing tube) it usually goes back to the issue of not “waking up” from the induced coma.
Once a critically ill Patient on a ventilator and a breathing tube is awake and breathing with minimal support, they should be ready to come off the ventilator.
This also leads me to the next issue when it comes to critically ill Patients not being able to come off the ventilator and the breathing tube(Endotracheal tube), because a tracheostomy might be the next logical step.
Now before you or your family member is giving consent to your critically ill loved one having a tracheostomy, you want to make sure that you and your family are making the right decisions.
Check out the following articles and videos to find out if your critically ill loved one should have a tracheostomy or not.
This leads us to the next situation when critically ill Patients can’t come off the ventilator.
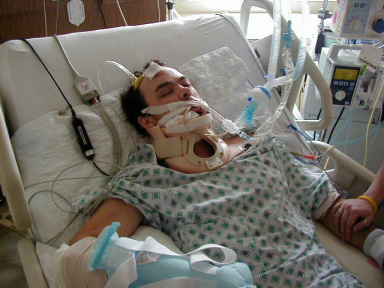
2. Not being able to come off the ventilator with a tracheostomy
Not being able to come off the ventilator when your critically ill loved one has a tracheostomy is a very different story and has a whole set of different challenges altogether.
Let me explain why.
Once your critically ill loved one has a tracheostomy they
- Have the inability to come off the ventilator with a breathing tube (Endotracheal tube) because of the nature and length of their critical illness
- Might have needed a tracheostomy early on in their Intensive Care stay because they needed a safe and secure airway to manage their critical illness more effectively and give them a better chance for recovery
Whatever scenario has led to the tracheostomy of your critically ill loved one, if they can’t come off the ventilator, there are a number of things that need to be considered.
In some if not most cases in Intensive Care, a tracheostomy leads to critically ill Patients having their first weaning trials off the ventilator early on, often within 24-48 hours after a tracheostomy has been done.
This is due to the fact that a tracheostomy is much easier to tolerate compared to a breathing tube/endotracheal tube and sedation, as well as opiates can often be ceased or at least they can be reduced.
Now, if your critically ill loved one has a tracheostomy and can’t be weaned off the ventilator here are the main reasons for it
- Respiratory conditions such as Pneumonia, COPD, Asthma, Pleural effusion
- Lung transplant
- Excess sputum production that requires regular and frequent suctioning via the Tracheostomy
- Neurological conditions such as stroke, brain or head injuries/TBI
- Obesity
- Confusion and aggression
- Depression in Intensive Care
- Lack of Quality of Life in Intensive Care
- Lack of Privacy& Dignity in Intensive Care
- Feeling helpless and not in control of the situation
- disturbed day and night rhythm
- lack of sleep or sleep deprivation
- lack of natural daylight
- and sometimes there can also be a psychological dependency on ventilation support, especially after many setbacks and failed trials to come off the ventilator!
But even after many setbacks and after many weeks and sometimes even many months on the ventilator and tracheostomy, hope is never lost and Patients can come off the ventilator with the right strategies and the right nurturing, the right psychological support and most importantly the right environment!
Whenever Patients on a ventilator with tracheostomies are in environments like Intensive Care or LTAC, they are not the right environments.
They are sterile, depressing and institutionalized environments that are non Patient and non-family friendly.
Therefore if you are finding yourself in this situation where your loved one can’t be weaned off the ventilator and the tracheostomy, because of one or some of the reasons that I mentioned before the right environment can do wonders!
Related articles/videos:
What’s the right environment you may wonder?
The right environment for weaning somebody off the ventilator and the tracheostomy is an environment where Patients and their families are feeling more in control and more empowered!
And that environment is a home care environment and not an institutionalized environment like Intensive Care or a long-term weaning facility or LTAC.
A very conducive home care environment has been created by INTENSIVE CARE AT HOME a highly specialized service that can provide Intensive Home Care services and also wean Patients off a ventilator with tracheostomy.
In a home care environment quality of life and in some instances quality of end of life can be restored much quicker.

Imagine you, your family and your loved one can be at home with a specialized service like INTENSIVE CARE AT HOME and imagine your loved one can be weaned off the ventilator and the tracheostomy in their own home, which one would you choose?
Your own home or an Intensive Care Unit/LTAC?
I think the answer is a “no-brainer”!
INTENSIVE CARE AT HOME is a fully accredited health service and can provide up to 24/7 care at home even if your loved one needs ventilation with tracheostomy.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



