Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
What Will Be My Sister’s Quality Of Life After Weaning Off The Ventilator?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’s sister is still with a tracheostomy on a ventilator and Joyce is asking what she must do to reach her goal of weaning her sister off the ventilator in ICU.
My Goal Is For My Sister To Get Off The Ventilator in ICU! What Else Do I Need To Do? Help!
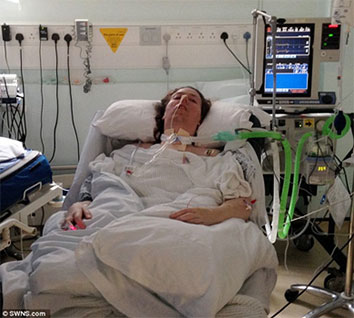
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Patrik: Look, unfortunately, your sister is a number there, unfortunately. And what I’m seeing at the moment, the whole COVID is not helping. Hospitals are completely overwhelmed, it doesn’t help. But compared to when we spoke last time, I guess, besides the issue with a PEG tube, it sounds they have been-
Joyce: The vent is better. I’m telling you. We were saying, “Oh my God, she would never.” Even the guy said she would never, but now it seem we’re getting close to just spontaneous breathing trial. So that gives me an indication maybe she could get off, maybe.
Patrik: Oh, look, spontaneous breathing, trial is great.
RECOMMENDED:
Joyce: I mean, even the fact that we’re close to it is great. The fact that we’re even close to it is a sign of something, correct?
Patrik: Absolutely.
Joyce: Okay, so here’s my thing. What happened now? No one approached me and I’m going to fight tooth and nail to stay there. But what if I don’t, am I going to be totally transferred in a new place? I don’t know what to do I’m scared.
Patrik: Oh, look, right now I can’t tell you how bad LTAC is, I just can’t. It’s just an absolute shocker. The stuff that I’m seeing, there, I’m talking to an LTAC at the moment every day, I have no clue, it’s shocking. And the challenge that I can see as you remember when we last spoke, I believe that was when they just shifted your sister from ICU to the step down, you got to be on high alert that the same won’t happen with LTAC, all of a sudden at two o’clock you get a phone call, “We’ve called the ambulance that taking your sister to LTAC at four o’clock, something like that.
Joyce: No, well, I think that would have a choice of where they put it up.
Patrik: No, I agree, you need to have a choice and you need to keep consent, but I can tell you at the moment.
Joyce: But you’re right, because I was at my high and might think she’d never get off the ICU. And you saw that live, so you’re right.
Recommended links:
Patrik: Yeah, that’s right. Yeah, what you can do is I think it’s probably best to bring it up early so there are no surprises. On the one end, you don’t want to talk about the hot topics but on the other hand, I think you got to bring it up and say to them early on, you want to keep her where she is.
Joyce: I’m going to wait for the surgery and I’m going to say, “Listen, I don’t feel safe with this very temporary thing, I want her to stay there until she gets a PEG.” And that’s my argument, my argument is this feeding device will get clogged up and leave it as not a permanent solution. And I don’t feel safe or whatever. I mean, that’s the only thing I have a leg to stand on.
Patrik: Very much so. But just coming back to the ventilator weaning, let’s just say best case scenario. If she can come off the ventilator with a Glasgow Coma scale, less than 11, she won’t be able to have the tracheostomy removed. But being ventilator free, I mean, that would be definitely a huge step forward.
Recommended links:
Joyce: But eventually she’ll be able to, I’m hoping that. Here’s the thing, here’s our goal. She really has to be very conscious in order for this to be really taken away.
Patrik: I tell you why a GCS less than 11 is almost contraindication for having the trach removed. She won’t be able to protect her airway with a GCS of less than 11. Doesn’t mean she can’t breathe, I’m not saying that, but she needs to be able to swallow, she needs to be able to cause more important that she needs to be able to follow simple commands.
Joyce: She hasn’t followed any commands yet.
Patrik: But that shouldn’t stop her. If she’s breathing spontaneously, shouldn’t stop her to get off the ventilator but it might stop her to have to trach removed.
Joyce: And then we’ll just be like a bag or like a tank connected to it. But what happens after the ventilator? Now you leave the trach, what do you connect then?
Patrik: Yeah, just the trach, nothing unless-
Joyce: The trach already has but where does it get the air from?
Patrik: Oh, she’s either going to breathe or she’s hooked up to a humidifier.
Joyce: So is it still a machine?
Patrik: Yeah, it’s humidified air, but it’s just humidified air or humidified oxygen if she needs oxygen.
Joyce: What does that machine looks like? Is it a machine?
Patrik: Yeah, it’s a machine, it’s not ventilator, I can send you a picture.
Joyce: A little thing where she gets like, let’s say take it with her and put it there.
Patrik: Yeah, taking it with her is fairly complicated. When people go out with a trach, they usually have a filter sitting on the trach, a filter. But overnight, for example, people on trachs and not on ventilation have a humidifier because otherwise the trach will dry out and block.
Joyce: Oh my God, okay. And then hopefully she can get off that and then we can, I mean.
Patrik: And how do you and your family feel so far of keeping going? How do you feel about that at this particular-
Recommended:
Joyce: My mom is very, very strong. Listen, Patrik, what do we do? There’s no other option. The person is alert. My mom is very, very strong about, she doesn’t want to make the choice. She’s still full code in the hospital. She said, “If it’s her decision, it’s her decision to make.” She will not make it under any circumstances and what am I going to disconnect it and watch her, no, I can’t. None of us are going to do that. And I’m hoping that these things come on their own if she really does struggle, we believe the spirit makes their own decisions.
Patrik: Oh, look, I’m with you on that one. I do believe things happen for a reason. I’m all with you on that one.
Joyce: Because we’re fighting with her, we’re like, “Come on.”
Patrik: Absolutely.
Joyce: I think we’re more involved than any other family in this hospital, they think we’re crazy, but we’re literally with her, not an hour that goes by.
Patrik: Take that as a compliment if they think you’re crazy, you should take that as a compliment.
Joyce: Well, we are who we are because I’m not letting her-
Patrik: Exactly.
Joyce: She’s my sister, I can’t.
Patrik: Absolutely.
Joyce: So what do you say, Pat, so we’ll let this go and see what happens and we’ll follow along and see.
Suggested links:
Patrik: Yes, and now the thing you need to ask for, if she’s having spontaneous breathing trials, you got to ask for the tidal volume. Because tell me your sister’s weight again, roughly.
Joyce: I don’t know. She’s so frail now.
Patrik: 170 pounds?
Joyce: I don’t know. She went in there 190, but now she’s literally skins and bones so I don’t know.
Patrik: Just give me a second, please, I just need to, because I’m in the metric system, I just quickly need to find out how many kilos 170 pounds are. Just give me a second. That’s 70s, okay. So the tidal volumes are important and they’re usually gauged around weight and you would be looking at seven to 10 mls per kilo, she’s about 80 kilos. So you’d be looking at sort of tidal volumes of 600 to 800 mls, anything less than that.
Joyce: Six to 800.
Patrik: Six to 800, assuming that the weight is accurate. That’s what we’re looking for. Keep in mind, so 600 to 800 mls, this is why mobilization is so important. You can’t get-
Joyce: I wouldn’t get on top of it. They keep telling me no. I have maybe seven people telling me if she doesn’t participate, they will not do physical therapy.
Patrik: Yeah, so you could picture this, you can’t take 600 mls in if you’re lying in bed.
Joyce: Right, that’s the problem though, Patrik, they’re not used to having a patient for so long. My sister is the longest patient in the hospital. They don’t know what to do with her. And I think she’s reached a point, that they’re not a rehab place. So the hospital is good, but they’re bad in the sense that they’re not rehabs either.
Patrik: I get it, but I tell you something as much as they are-
Joyce: It’s better than LTAC.
Recommended links:
Patrik: They’re selling you the LTAC for reason basically-
Joyce: They haven’t told me anything, no one has spoken to me of that.
Patrik: But they will. And that the LTAC, it’s disaster area.
Joyce: I know, listen, what am I going to do? It stresses me out, but look, she is still there. And hopefully my goal was to get out of ventilator. I’m going to fight tooth and nails to have her, I’m going to try to make every argument in the book and the argument right now is I want to stay there until she gets a PEG. They might, I don’t know, that’s the only argument I have.
Recommended:
Patrik: Yeah, for sure. And what’s happening there? The COVID situation is really bad, so-
Joyce: COVID is still really bad, I think they taper down a little bit, and we just got off the surge. It’s still really, really bad. And I think the vaccine is a hot mess because nobody can get it, it’s crazy.
Patrik: Yeah, the reason I’m asking is simply, if she’s COVID free at the moment she’s going to another place who knows what’s floating around there.
Joyce: And there’s a new strain and there’s a whole thing.
Patrik: If, God forbid, your sister was to have another COVID infection. That could be the end of all of your efforts.
Joyce: 100%, unless they give her a vaccine but I don’t even know.
Patrik: Oh, yeah, definitely.
Joyce: Because I took the first vaccine, now, the problem is it’s so short, I don’t even know if I can get the second one. It’s like the wild, Wild West, I’m totally screwed.
Patrik: And you’re feeling fine with the vaccine.
Joyce: I got the Moderna shot. I felt a little tired, but I feel great, other than that. I have another, three weeks to get the second one. I have a friend who actually is in the medical field who kind of let me skip the line because they just do healthcare workers. So I had to do the wild, wild west to protect myself because I’m going to go see my sister eventually, I had to protect. So I had to kind of get it under the table, not illegally but illegally because I wasn’t next in line.
Patrik: Semi.
Joyce: Hey, listen, what I learned in this industry and meeting you, if anything, I can’t take anything for face value anymore.
Patrik: Can’t take anything for face value that they. And it is important to get informed as you can see, I have answers for you, but I don’t have a quick fix either, there is no quick fix in a situation like that.
Recommended:
Joyce: I know, and I think they were stuck too, they don’t know what to do with her. They literally waited and waited and waited and it wasn’t getting better.
Patrik: So yeah, but look out for the tidal volumes, look out for the mobilization.
Joyce: I’m going to fight for that.
Patrik: Absolutely, and if they are pushing you with LTAC, your argument should be continuity of care in the hospital. And the other argument should be, if they tell you, yes, you’ve got LTACs choose from, look up the online reviews, they’re probably pretty bad, show them the online reviews. And also, I don’t know if they do send her to LTAC, would it be up the road? Where would that be?
Suggested links:
Joyce: But the other kicker is the health insurance that she has, she’s not in the hospital, she’s not in network hospital, she’s actually in a much better hospital that kind of got stuck with her. So the other insurance is paying a lot of money, but technically this is not her hospital. She should have been in a completely different hospital in a different thing but because she got stuck here, she’s gotten a lot better care than she probably would have been in her other network, it’s Kaiser versus a different thing. Because they’re paying for my sister tooth and nail every single day because they can’t transfer her.
Joyce: If a normal setting, they would have scooped her up and took her to that hospital so they don’t have to pay the hospital bills, but they’re paying the hefty hospital bills. So that’s another stacker because it’s so bad. But so far we’re still there and we’re able to get the numbers low enough. The surgery is going to throw us up for a loop also going to throw so for physical therapy because now you’re talking about an incision. I had a C-section scar. That’s not easy, and I was young, let alone 74. But listen, I don’t know-
Patrik: Should be a small incision.
Joyce: He said up and down, I don’t know how big it is.
Patrik: Really?
Joyce: Vertical, I think.
Patrik: Oh, that’s a worry because she will need a general anesthetic for that.
Joyce: She is getting it, she’s going into major surgery. You have to go in there and fix everything. But she said, I mean, I spoke to her and she goes, “You don’t have a choice. I mean, leave it open, you’ll get infected. What are you going to do?”
Patrik: Yeah, okay-
Joyce: Yeah, go ahead.
Patrik: Any other questions?
Joyce: No, I think you’re so good. So I think let’s follow up again and I’ll let you know how it goes. I mean eventually we’ll end up being in a place? I mean it’s inevitable.
RECOMMENDED:
Patrik: Oh yeah, you don’t want to be in ICU forever and a day, but it’s got to be the right place. It’s got to be the right time.
Joyce: I know, but nobody is talking to me about it. So I’m not even going open that door. There’s so much in my head? And I’m not going to investigate anything until it comes to me and then I can bite.
Patrik: You’re not taking any prisoners. They know that by now.
Joyce: I’m a sharp cookie, so they know. That’s the only reason to let my mom and they didn’t let anybody in eight months because I’ve been feeding them has showed so much gratitude to the nurses and lady calls and goes, “I’m going to do this for you. I’ve not done that for anybody but she’s been here 60 days, I lost my dad two years ago, I’m going to do it for you guys.” And you know why, this woman gave the gift my mom’s 50-year anniversary and she gave her the gift, Patrik, she was alert. But my goodness, she was alert. I need to be alert and not follow command, but can she still be there?
Patrik: Look, definitely, we have clients in the home, they are alert, but they can’t follow commands, but we know they’re there.
Joyce: You see them and they’re there.
Patrik: To see it, definitely.
Joyce: You just take it for what it is that you treat them just like everybody else without her. Just like she’s my sister, like nothing matter.
Patrik: Joyce, right now, I need to run. Thank you so much. And let me know, thank you. Take care, all the best, all the best, thank you, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!