Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Will I Know If My Sister In ICU Is Ready To Be Weaned Off The Ventilator?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to share this experience from one of my clients, Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU on a ventilator and is 100% off the sedation now. Joyce is asking if her sister will be able to get off the ventilator for the next two weeks.
My Sister is Off the Sedation in ICU Now. Will She Come Off the Ventilator Soon?
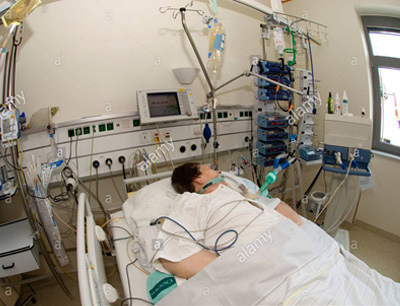
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Patrik: Okay. Giving you the short version there, Joyce. We have INTENSIVE CARE AT HOME here where we are taking ventilated patients or tracheostomized patients at home here in Melbourne all the time. We also look after medically complex patients that are not ventilated but have unstable airways. However, Australia is different in respect, our clients are getting government funding, because the government sees value in what we’re doing. That’s number one.
Patrik: Even if you have government funding, number two is probably the bigger problem. Can someone pull this off? Because it’s a very specialist skill. If we take clients home here … We can take clients home here recently quickly, but we are experienced and we either take them home from ICU/PICU and we make sure they don’t go back to ICU/PICU from home because we send highly skilled ICU/PICU nurses into the home. We couldn’t do it as quick five years ago as we do it now.
RECOMMENDED:
Patrik: At the moment they’re paying $5,000, $6,000 a day for an ICU bed. So, our sales pitch to anyone here is we’re cutting the cost of an ICU bed by over 50%. That is our sales pitch.
Joyce: Sure. Let’s put that on the table again, because my other question to you is, with my sister making … First of all, do you think they will keep her for the next two weeks to try to get … Right now she hasn’t even woken up yet. So, when she opens her eyes, we don’t even know what we’re going to get.
Joyce: We don’t know if she’s going to freak out. That’s why we’re trying to keep the camera on. If everything goes well, is there such a thing that they’ll be able to get her off the ventilator within a week? I just don’t know what these things take.
Patrik: That is difficult to say. If you can give me some ventilator settings. I know you mentioned PEEP of seven, oxygen of 50%. But if you can give me the exact ventilator setting then I can probably give you an indication of how realistic is it for you.
Joyce: Well, that’s what I was hoping, tell me what I should ask for.
Patrik: Do you think you can get a picture of the ventilator settings? Just a picture of the ventilator?
Joyce: No. I’m not sure where it’s at right now.
Patrik: No?
Recommended links:
Joyce: No.
Patrik: Can anybody visit?
Joyce: Visit in the hospital? No.
Patrik: No. Do you think you can get the nurse to take the picture of the ventilator?
Joyce: Well, let’s see. That means she’ll need to take a picture. And then she’ll need to know how to test that.
Patrik: Yeah.
Joyce: I’ll try. I can try. Basically just take a picture?
Patrik: Right.
Joyce: Is there anything you want me to ask her though?
Patrik: Yeah, just ask her what ventilation mode is she in?
Joyce: Okay hold on, ventilation mode.
Patrik: Mode. Is she breathing spontaneously?
Recommended:
Joyce: Okay, breathing spontaneously.
Patrik: And if she is breathing spontaneously, how many breaths is she taking per minute? I’ll text that to you as well. Then what are her tidal volumes?
Joyce: Tidal, are you going to text this to me?
Patrik: I’m going to text this to you. What are her tidal volumes?
Joyce: If you’re texting it then-
Patrik: I’m texting it. Tidal volumes, is she breathing spontaneously? Ventilation mode. You mentioned PEEP is seven?
Joyce: Right. It was literally the first time that she brought it down from eight. They just announced a seven today.
Patrik: Yep. Okay. I’ll text you all that. Pressure support would be important to know. I’ll text it, I’m just typing as we speak.
Joyce: Okay. I only have tidal volumes, and pressure support. Is that it? Add the other one.
Patrik: Ventilation mode.
Joyce: Breathing spontaneously and how many breaths per minute?
Patrik: Yes, correct. Breathing spontaneously.
Joyce: That’s the SBA, right? Or no. Because I read about.
Patrik: There are so many ventilation modes. So it could be, but it depends what ventilation mode she’s in.
Joyce: Okay.
Patrik: We talked about, PEEP we know, we know oxygen. Those would be the most important things.
Joyce: I mean, I think she’s just beginning to be put off sedation, but my question is … Once I give you that information, then maybe you can tell me … I mean, look, she literally wasn’t even totally getting off sedation. Now that she’s 100% off sedation, I don’t know what it’s going to look like. Look, Patrik, I’m freaking out. I’m freaking out because the uncertainty level is so high. I don’t know-
Patrik: It’s huge.
Joyce: What is it going to be? Is she going to be pissed that we did that for her? Subacute is a complicated place? Why am I going to put my sister in that complicated place?
Patrik: Exactly.
Joyce: I’m freaking out.
Patrik: I totally understand. I can tell you probably the next challenge that is ahead, it’s great that she’s off sedation, she may not wake up for a week.
Recommended links:
Joyce: She said, two, three days, but it could be another week. And they can’t really do anything with her until she wakes up.
Patrik: Probably not, because they need to ask her, what does she want?
Joyce: You think they will?
Patrik: They have to.
Joyce: Really?
Patrik: Well, it’s all well and good and say, she’s going to subacute, or she’s going to LTAC, or she’s going home.
Joyce: If she responds they have a question to ask her?
Patrik: I mean, that’s not optional.
Joyce: Really?
Patrik: That is not optional. If she’s with it, they need to ask her what does she wants?
Joyce: And if she has a bad day and she says … My sister is a very stubborn feisty little lady. She goes, “I don’t want to live here anymore. I’m done with this situation.” She has a choice?
Patrik: Sure. Yes.
Joyce: What?
Patrik: Let’s just say that was the case. Let’s just say your sister wakes up, and makes sense, can communicate. Let’s just say that is the case, then there is usually a case … It wouldn’t just happen because she says it one day, it would have to be for a period of time.
Joyce: Really?
Patrik: Definitely.
Joyce: Interesting.
Patrik: I mean, there are people, they say, “Well, today I don’t want to live.” And they change their mind tomorrow.
Suggested links:
Joyce: Right. Listen, I mean, could it be a miracle since it’s COVID that we can … Look, the best thing is to get off the bed.
Patrik: Absolutely.
Joyce: If we can get her off the bed, then I think bringing her home, or subacute … Maybe subacute wouldn’t be that bad for a small period of time. Let’s say I do a subacute for like a month, or two months. And they can have the machines. It won’t be a long thing for her.
Joyce: My goal, I told my family, I want to bring her home. But I also want her to get what she can get. So, it’s such a tricky thing, because-
Patrik: Very tricky thing.
Joyce: It’s her body, and it’s like, “How long are we looking for?” Once I give you the mode, she’s been laying down for a month like a vegetable. We’re looking at six months? I mean, I know you can’t say anything.
Patrik: Hard to say. I’ll tell you … Look, I have seen anything from days to years. When I say years, I mean, if someone can’t off after years they probably are on the ventilator for the rest of their lives.
Joyce: I heard if you’re on the ventilator for 60 days or more, the odds of you being on there forever is high.
Patrik: You could say that every day you cut her off the ventilator the risk increases you staying on a ventilator for the rest of your life, for sure. Picture this Joyce, going home without a ventilator would be so much easier, right?
Patrik: The recovery changes significantly once she’s off the ventilator, right? Even once tracheostomy is still difficult, the best recovery would be off the ventilator, off the trach, then going home is inevitable. With the ventilator, and even with the trach, even for a trach without a ventilator, you need that specialist skill. It’s an artificial airway.
Patrik: I don’t want to be negative here, but I’ll just give you an example so you know why I’m saying this. We had three clients six weeks ago, with a trach, not ventilated. They didn’t have 24-hour care, because they didn’t have the funding. Three clients passed away during the day time when we weren’t there, because we were only having funding for night shift.
Patrik: All three clients passed away with medical emergencies when no ICU nurse was present. That’s how significant this is. I wish I had better news, but I’m just giving you-
Joyce: No, most likely it’ll have to be a subacute, but what I’m saying to you is right now we’re at day 25 on the vent. They were saying I’m not going to keep my sister forever on a vent, I will not. None of us will. We will let go, make peace.
Joyce: But my question to you is, every day that we go it’s, if she just woke up on the sedation. Right now if she can wake up, and she can advance and get … Because I’m thinking all the signs have been shown. Body is still working, this is working. Can we see a turnaround? Can we see her getting off the vent in a week, two weeks maybe?
Patrik: Yeah. That is possible.
Recommended links:
Joyce: Just so you know, with the thing being for three and a half weeks, they always sedated her. She was never not sedated.
Patrik: That’s a big, big issue. The more sedation, the more difficult it is to get that sedation out of the body system. Now the next step is physical therapy mobilization. Mobilizing the next step would be to get her in a recliner chair, but even that would be probably very uncomfortable for her, because she’s been in that bed for the last three weeks. It can be a sore process, but you just don’t know until they’ve started the process.
Joyce: So the best thing to do right now is just sit and wait?
Patrik: The next step is, Joyce, she needs to wake up.
Joyce: She needs to wake up.
Patrik: She needs to wake up, and that can take time.
Joyce: Really?
Patrik: Waking up in ICU-
Joyce: Today was the first day they turned it off.
Patrik: After such a prolonged coma is a process, not an event.
Joyce: Maybe I don’t know enough, because we’re literally staring at the camera and thinking the eyes are going to open at any moment. We think it’s going to happen. That’s why we haven’t left her for a second. She said it might take two days, but you’re saying this can take up to a week. Then she opens her eyes, and then what? What do we say there? What do you think we should know? What happens in her mind? Do you know?
Patrik: No, I don’t. But what I can tell you is that most patients that come out of a coma months down the track they say, “I don’t remember much. If I do remember anything it’s fractions.”
Joyce: But they can’t talk, so they just what? Signal?
Patrik: They can’t talk. They might talk, they might revert back to having nightmares. There could be an element of her going … Worst case, one of the things that can happen is she might go into ICU delirium. Have you heard of that?
Recommended:
Joyce: I’ve heard of delirium, but I don’t know really know what it is.
Patrik: It’s basically again a result of being in a prolonged induced coma. She wakes up, she has no recollection of what’s happened. She’s in this strange environment. She looks up the ceiling, she doesn’t know where she is. Of course people go mad, can’t talk.
RECOMMENDED:
Joyce: Then we’ll be like, “Hey, you’re here. We’re fine. This is happening to you. Blah, blah, blah.” And she’s just looking, not knowing what’s going on, because she can’t speak. How can she communicate?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!