Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Is It Safe For My Unstable Sister with Tracheostomy to Be Moved Out of The ICU?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to share this experience from one of my clients, Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU with a tracheostomy on a ventilator and Joyce is asking until when should her sister stay on a ventilator.
Until When Should My Sister Stay On a Ventilator In the ICU?
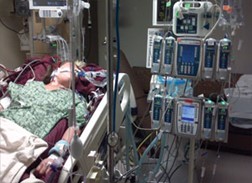
Joyce: Can you believe that? I mean, you saw this live right now. This is something that’s infuriating. I don’t know what else I can do.
Patrik: Joyce, I just had a quick look online, healthcare laws. There’s nothing in there that I could find. There’s talk about it, but I can’t find anywhere that this has been implemented.
Joyce: I mean, she just … She probably just said it because it’s all over the news. I don’t know how fast they implement it. But you saw, she’s saying I have no … I can call the charge nurse, I’m going to say the same thing. They’re still moving her. I mean, look, they’re moving her to a step down unit. Look, she said they’re moving her to a step down unit. I don’t really know what that means.
Patrik: Probably, I’ll tell you what it means. It means high dependency unit. It’s a step down. You’re going from ICU to HDU, which is high dependency unit. It’s a little bit lower acuity. But your sister sounds very unstable. I mean, they’re making this big fuss, they can’t transfer her to CT, but they can transfer her to a step down. Doesn’t add up.
Joyce: She’s saying the CT, they would have to change a bed. She’s not changing a bed right now, she’s taking the ICU-
Patrik: Yeah, I agree with all of that. I agree. But she’s too unstable to go for a CT scan, but she’s stable enough to go to step down? It doesn’t add up.
Joyce: Should I call the charge nurse? Patrik, will you be patient with me? This is moment by moment. I’m so sorry. Just right, you’re okay with this at the moment?
Patrik: I’m okay with this for the moment. I do have a next call at seven o’clock.
RECOMMENDED:
Joyce: Oh, no, that’s okay. Can I be connected to the charge nurse please? This is Joyce. I am one of your patient’s sister. I need to speak to the charge nurse please.
Sally: Okay, hold on please.
Joyce: Thank you.
Joyce: That’s fine, Patrik, we’ll be done by seven.
Patrik: Joyce, I can’t find anything online about healthcare rationing laws. There’s talk about it, but …
Joyce: Okay, so what do you … Do you have any recommendation on what I can say?
Patrik: Yeah, but is that what they told you, that because of healthcare rationing laws-
Joyce: She just threw that. I don’t know if she … The nurse, the one that’s moving her, she goes, “You heard about rational law.” But I don’t know if she put her stick in the sand of saying, “This is what’s …” Oh. You know what I’m saying? They’re throwing it around. But listen, there is a crisis, they’re saying the ambulance basically won’t transfer for people who don’t think they can make it. These are people who make 40,000 a year, they’re going to give them the decision of not trans … So listen, I don’t know, you heard a live conversation on what’s happening here.
Patrik: And this is the nurse looking after your sister, Nina?
Joyce: Yeah, she’s … Hello? Oh. Yeah, she’s the day nurse. And she’s moving her, because there’s somebody that needs the bed. And this step down unit, they’re saying it’s still the ratio one to three, they’re saying that … That’s what they’re saying. Because of the ventilator usage. They’re saying it’s the same ventilator, which I don’t know.
Patrik: Probably. Probably.
Joyce: Okay. So she said the minute she gets better, they could do rehab. But she’s not anywhere near that, so it doesn’t matter. So look, I don’t know … I know that if … I don’t know what the ICU is going to … I know that I need to be in the ICU.
Recommended:
Patrik: I tell you what you could do. And that’s certainly a strategy that some clients have used. You go to the Supreme Court for an injunction. And I have learned that sometimes you don’t even need a lawyer. You just contact the Supreme Court in your area. And I’ve seen it with clients in different countries, I’ve seen it here in Australia. You contact the Supreme Court. You tell them your situation. And if they think they can intervene on your behalf, they will.
Joyce: I know, but I think I’m such a moment to moment at the moment.
Patrik: When did you find out? When did you find out about it.
Joyce: Literally four hours ago. Four hours ago she goes, “Just a rumor that it’s happening.” And then literally when I called, she was like, “Oh, it’s happening now.” It literally unfolded within four hours since I texted you. It just literally unfolded. And literally, she’s being moved out right now. I am furious beyond belief, and I don’t know…
Joyce: Look, they’re saying my sister is at 50 PEEP. She made some indication yesterday. I don’t know what the step down unit is, but I know it’s not the ICU, I know that it’s not … Okay, I don’t know-
Patrik: It’s better than LTAC. It’s better than LTAC, I can tell you that much. But it’s not ICU.
Joyce: And they’re saying every time they move her, she gets desaturation. So how do you … How?
Patrik: How do you go from one to one in ICU, to one to three if you are unstable?
Joyce: And they are aggressively taking down … All of a sudden, I felt … This obviously was planned. This was obviously planned, because they took off the steroids, they took off … They slowly.. They took off the sedation. Which is fine. We wanted them to take off the sedation. Do you know what I’m saying? But now she hasn’t woke up seven days.
Recommended links:
Patrik: Why have they stopped steroids and antibiotics? Are her lungs fine?
Joyce: Oh, antibiotics, she’s still on.
Patrik: Okay. Okay. So what are they saying are her lungs doing? What are they saying?
Joyce: You know what, I know that the air pocket is gone. And she was saying something about … By the way, I’m getting the medical records tomorrow, because I’ve just emailed them and waiting for approval.
Patrik: Okay.
Joyce: Okay. I mean, that’s as far as I understood. Her blood gas is 62.
Patrik: Yeah, that’s not … An arterial blood gas, you get 10 readings.
Joyce: I know. Hold on, she said to me … Hold on, let me see my notes. It’s hard to hear them when they’re in the room, because it’s-
Patrik: Sure.
Joyce: So Patrik, tell me if this makes sense. 7.35, CO2 62.
Patrik: Yeah, okay, CO2 62. Okay, yeah, what else?
Joyce: Yeah, hold on, guys.
Sally: Hi, sorry about the wait. Now, the charge nurse says she’ll be right with you.
Joyce: Okay, who is it? Who’s the charge nurse for the night?
Sally: Carol.
Joyce: Carol. Okay. Is there anything else I can tell them that I can have them advocate, so they can put in the system?
Patrik: Yeah, I think yeah, you can do that. And I would … Have you, in all of this time since we’ve spoken, have you spoken to a lawyer?
Suggested links:
Joyce: No. I will.
Patrik: Yeah, I don’t think that you do. But I just think it could be as simple as you calling the Supreme Court in your council, finding … They have an after hours number. They must have an after hours number.
Joyce: But is there anything I can note in the system, now, that is against the step down unit, that I can bring up to them?
Patrik: I think if you talk to them, Joyce, can you record the call that when you talk to them, because I think you need some evidence. I mean, I’m your witness, but it would be good if you had some evidence that you tell them that you are against the moves.
Joyce: Right.
Patrik: Because otherwise, they might say, “Oh, you’ve never said that.”
Joyce: Yeah.
Patrik: And I’ve heard you saying it, right. That is my own advice. They are doing, at the moment, whatever they want to do. But it doesn’t make sense not sending her for a CT scan because she’s too unstable, and then they’re sending her down-
Joyce: It feels that they don’t have the staff. I believe that they-
Patrik: Yeah, yeah, I’m all with that.
Joyce: So I believe the fact that it is risky, so I don’t want to push anything that will send her over the edge. So she’s saying, “There’s not enough staff for me to support.” So fine, I’ll let that go. What’s the point of me finding out what’s wrong, and her not surviving the CT scan? It’s not worth it.
Patrik: It needs to be planned, it needs to be planned and managed. Yeah. Is your sister-
Joyce: I am totally screwed now with the step down unit?
Patrik: I think step down unit is better than LTAC. But she’s too unstable.
Joyce: And what makes her unstable? Can you give me some terminology right now so I can bring that up?
Patrik: You mentioned it. When they turn her, she desaturates. That’s dangerous enough to not have her go to a one to three nurse to patient ratio.
Joyce: They’re saying right now at the ICU, they’re one to three anyway because of the pandemic. She said they’re one to three because they literally went from 10 beds to 28 beds. And they just are over here, and it’s the same ratio, the step down unit is the same ratio. And she’s been the longest ICU patient, because she’s been there a month. She has a tracheostomy, she’s been keeping the numbers at 50 at eight. So for them, out of everybody, she’s the most stable. But obviously not.
Patrik: Is she still COVID positive? Do you know?
Joyce: You know what, two weeks ago she was. They didn’t do another test.
Patrik: Swab.
Joyce: I mean, it’d be interesting to find out. But my question is, now, she’s still trached, they just let her be. Look, I don’t listen. Between you and I, I don’t think they’ll risk her life by moving her, since I think the bed will still … I don’t know. But I’ve made it loud and clear, and I’m making it noted here, so if something does happen to her, oh my God, I will go with a vengeance. I mean, you know me a little bit, but I’m-
Recommended:
Sally: Hi, Joyce, I’m sorry about the wait. Are you able to continue holding?
Joyce: I’m able to continue holding. Yeah.
Sally: Okay.
Patrik: Joyce, saying earlier, they haven’t mobilized her. Have you asked them why they’re not mobilizing her?
Joyce: What does mobilizing mean?
Patrik: Yeah, sitting her in a chair, sitting her on the edge of the bed.
Joyce: They’re saying, from what I understand is that every time they even turn her side to side, she desaturates. So the mobilizing goes out the window when you’re telling me that the minute you move her this way, and she needs 100, and the minute you move her this way, she needs 100, how the hell are they going to get her up?
Patrik: Okay. Yeah, fair enough. Fair enough.
Joyce: I mean, you know what I’m saying? But this is disappointing, because look, I don’t know what else I can advocate for? I understand. That’s why I was going to go over the medical records with you. I’m getting them so we can read them, to see what’s missed. I told you that I spoke to the doctor, and the doctors told me that there is a slim chance of her ever getting out of the machine. And she doesn’t know if she’s ever going to wake up. And my question to you is, is it normal for seven days to go by-
Recommended:
Patrik: I’d say anything up to 14 days, Joyce. Anything up to 14 days.
Joyce: What is the 14 days going to indicate for us?
Patrik: Well, okay, so I’ll illustrate that for you. Sometimes patients don’t wake up because they have a neurological event, which is what I mentioned to you earlier in the week. Sometimes patients don’t wake up, even though they don’t have a stroke. Just simply, they need time to wake up.
Joyce: Okay, so my question is, do we know what an indication of the stroke is?
Patrik: Yeah, they would see … But because she’s not moving, if your sister was moving, one side would be paralyzed, or difficult to move. But because she’s not moving … That’s why I asked earlier in the week. The only way for them to find out is through a CT scan.
Joyce: Okay, my other question to you is, it’s day seven. So you’re saying up to 14 days, there could be still possibility. After 14 days, what does that look like? Brain dead? I mean, what does it look like?
Patrik: No, no, no. Brain dead, they would be testing her for brain dead. They would have test-
Joyce: They’re not testing her for anything, but okay.
Patrik: Yeah, look, it is so hard to say. If someone is not waking up, they’re not waking up. Let’s just say they do a CT scan, and they rule out a stroke, okay, then you just play the waiting game. She may or may not wake up. But your sister … Just remind me, your sister was proned at some point, wasn’t she?
Joyce: Prone meaning on the belly?
Patrik: Yes.
Joyce: Yeah, yeah.
Patrik: Yeah, so when she was proned, she would have had bucket loads of sedation, bucket loads.
Joyce: She did. That’s true.
Patrik: All right.
Joyce: Yes, bucket loads.
Patrik: Bucket loads of sedation, bucket loads of paralytics.
Joyce: Yes.
Joyce: That is very true.
Patrik: Bucket loads.
Joyce: Yes, bucket loads, yes.
Patrik: So let’s just say your sister wasn’t proned, and didn’t have bucket loads of sedation and paralytics, she could still be in a situation like this. But now that we know she was proned and had all this, she needs time. But bear in mind, we still … The first thing that they should have done, they need to rule out a stroke. They need to rule out-
Joyce: I can’t take the risk of the CT though.
Patrik: They can’t do it. I know they can’t do it. I know they can’t do it.
Joyce: Okay, so here’s my other question to you. Well, can’t rule … There’s no other way to rule it out. My husband is asking, “How else do you?” You can’t. So my other question is this, look, I also want to say this, okay, in addition to her neurological, the chest should be getting … This is two separate things. The head is the neurological, and the chest, right. Even if she wakes up and this is still bad, it’s still an issue. So we’re in day 30. I mean, we’re still having this issue. So my question to you is, should this get better? And if it’s not getting better after day 30, am I looking for a ventilator for the rest of her life?
Patrik: Look, you could argue that every day your sister can’t come off the ventilator, the risk of her staying on the ventilator for the rest of her life is increased, right. No doubt about that. Yeah, so yeah, every day, you could argue the risk is increasing.
Recommended links:
Joyce: So okay, so let me ask you a very important question. I said to my siblings, “I don’t want my …” obviously nobody does, right. We’re not going to be the family that’s going to keep them on forever and ever. Hold on one second. We are not going to keep her on a ventilator for the rest of her life, okay. I think my sister is holding on, because if the end is near, right, we want her home to do it with us, because the argument and the fight is different in the sense that, let her be in peace with us. At what point … I told my family, “Look, my sister would never want this. My sister would never want to be in this situation.” Obviously. At what point do we … We’re still in the hope of fighting.
Joyce: At what point can you guide us to say, “Okay, guys …” I trust you more than I trust the doctors or anything the hospital says. At what point can you guide us and say, “Look guys, it’s going to be …” And if that’s what you tell us with a very educated … We’ll have another family meeting all together. And you can say, “Listen guys , can I fight with trying to get a company …” You got to text me that company again.
Patrik: Yeah, yeah. Yeah, yeah. Yeah. Yeah, yeah. Intensive care at home
Recommended:
Joyce: And then I’m going to contact them and say, “Let her come home to do hospice, even if we need to do it for a week.” Then whatever the setup would be.
Patrik: Yeah, sure.
Joyce: Then I fight for that. But my question is, I don’t … Where am I with the fight? Where am I? How long do I have? What’s the typical fighting length of this situation?
RECOMMENDED:
Patrik: Yeah. Yeah, yeah. Look, I do believe you’ve got a … Okay, let’s just say, for argument’s sake, stroke has been ruled out, okay. Let’s just say stroke has been ruled out. If in another week, she still hasn’t woken up, I would say two weeks not waking up, no stroke, no other neurological event. That’s a pretty significant sign that the critical illness has really hit her hard.
Joyce: Okay. So you would say, from what I’m hearing is about one more week from today, to see where it goes. Now, if for some reason we wake up and it’s great, we … Right. But another 14 days, and this is not getting better.
Patrik: Well, I’ll tell you another thing. Waking up, as you can already see, it’s not an event, it’s a process.
Joyce: No, I see that.
Patrik: Right. So even in three days, she may still not have woken up, and maybe in five days she’s doing a little bit. So what do you do then?
Joyce: Right. And not even that, okay. So that’s one issue. But the second issue is, if she’s never going to get off a vent, then.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!