Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
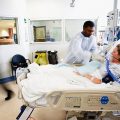
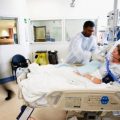
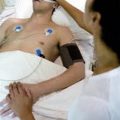
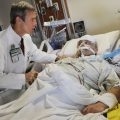
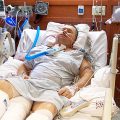
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’ssisteris still in the ICU on a ventilator and is now off the sedation. Joyce is asking if her sister is ready to come off the ventilator now.
How Will I know if My Sister in ICU is Ready to Be Weaned off the Ventilator?
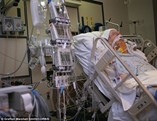
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Patrik: Yeah, it’s very confrontational. And most people can’t deal with it. Most people give in because it’s too confrontational and I understand that it is incredibly confrontational.
Joyce: Yep. Okay. Okay. All right. So Patrik, that’s where we’re at. I’m going to get on it today, and we’ll talk again tomorrow.
Patrik: Okay. All right.
Joyce: Just send me that number so I can WhatsApp you.
Patrik: Yes, I will be in touch. Will WhatsApp you in a second.
Joyce: Okay. Thanks Patrik. Talk to you soon. Bye-bye.
Patrik: Take care. Thank you. Bye.
RECOMMENDED:
Joyce: Hi Patrik.
Patrik: Hello Joyce. How is your sister now?
Joyce: Well, they have decreased the PEEP, eight to seven. I just have the rest of therapies, she’s at seven, she’s at 50. Yesterday she was at 40. I guess it doesn’t matter what she was. Today she’s at 50 and seven PEEP. They have not needed blood pressure medication. The air pocket that we’ve been monitoring has now passed.
Patrik: What air pocket?
Joyce: They had an air pocket in the lungs. I’m sure there is a medical term for it. There was an air pocket from what I understood.
Patrik: Yes.
Joyce: They’re monitoring it, to make the reason why after the tracheostomy they weren’t able to bring her too much the sedation they didn’t want to have that bigger, have the lung collapse. So, they just did nothing until the air pocket passed.
Patrik: Okay.
Joyce: It looked like the air pocket has improved to the point that they were not aggressively taking off sedation. So we’re now off sedation, the air pocket has subsided basically. The nurse said it has gotten better, and subsided. So we don’t have an air pocket at the moment. She was running a fever two days ago. She was running a fever, and I was talking to palliative care. She was again trying to put the black cloud against me.
Joyce: Ever since they took cultures, she hasn’t been running a fever, she wasn’t running a fever for last night, and all day today. She hasn’t been needing blood pressure medication, which gives us the indication that her body is not fighting …
Patrik: Correct.
Joyce: We’re still waiting for their report.
Joyce: Okay, here is where I’m at. We’re still in the ICU, I now need to speak to you about what are they going to try? So far, no one has called, not the social worker, not the caseworker. No one has talked to me. I think I’m going to stop talking to palliative care guy, because I think he tries to get into my mind to find out where I’m at, and relaying the message. Because I spoke to the doctor in the morning, yesterday. Then the palliative care guy goes, “What did the doctor say? Where are you at?” I’m like, “Why do I have to recap to you?” I think I just need your advice how I handle everybody.
Recommended:
Joyce: As of now, I want to know what they’re going to try to do, what the next steps are for my sister’s situation. What should I advocate to have her stay as long as possible? Then look, I know I’m only going to have so much time.
Joyce: The other lady was like, “Look, she already had a referral to go to a subacute.” No one has spoken to us yet at all though, officially. I want to know what’s happening. What do I advocate for? Then I want to talk to you about … If we go over half an hour, bill me, no problem. What happens next is we want to talk about what would it cost to bring her home? Do we do a subacute for a little bit and then bring her home?
Joyce: Financially, my mom has additional house that if we need to sell we will. We just want to get ready. When I brought this up to them they thought I’m way advanced, way above. I think 1,000 miles ahead.
Joyce: I wanted you to guide me, what am I looking at? What should I advocate for? My advocacy is to keep her in the hospital as long as possible, but I also want her to get the physical therapy, and we move on.
Joyce: Tell me, from what I told you now, where am I at with my sister’s care? Everything else is working though, all the organs, all the electrolytes, everything. And they’ve always been working.
Patrik: No kidney issues, she’s not on dialysis?
Joyce: She said something about the kidneys today, but she didn’t really say much about it.
Patrik: But she’s not on dialysis? You can almost rule out she’s not-
Joyce: No. No dialysis. Nothing. No dialysis. There is something about the kidney, but nobody said anything actually. As of now she said everything is working.
Patrik: Okay. I’ll give you the short version what you should be advocating for, and then we go into more detail. The advocacy is all about getting her off that ventilator because once she’s off the ventilator everything would be so much easier.
Recommended:
Patrik: I am a bit surprised that they didn’t take her off sedation straight away, when she had the tracheostomy, because that is one of the main advantages doing a trach, you should be able to switch off sedation straightaway.
Joyce: They said the air pocket, is that true?
Patrik: Yeah. Sure. That may well be a reason why they didn’t stop sedation straightaway, because I almost feel like she lost valuable time there to be weaned off the ventilator. But now that she’s off sedation she should get physical therapy. She should be sitting up. She should potentially be mobilized into a recliner chair to just get her back to normality as quickly as possible. That will be a slow process don’t get me wrong, but that is a process they need to start as quickly as possible.
Patrik: Now, I’ll tell you what they will probably tell you. They will tell you that they are not specialized on weaning people off the ventilator, especially if they have a trach. They will tell you the LTACs are the specialists. Well, I believe nothing could be further from the truth, but they want her out probably as quickly as possible.
Patrik: The palliative care guide will probably rear its ugly head at some point again, saying, “Oh, look, if she can’t come off the ventilator, why don’t we just move towards end of life?” I think that will happen eventually again. We just don’t engage our guests.
Joyce: Here is the thing, if they don’t give me physical therapy in the ICU … Basically, here is what I say, from right now it’s ICU, then it’s a step down unit at the hospital, because they just won’t send her to subacute right away, correct?
Patrik: Yeah.
Recommended:
Joyce: This need to happen first. Look, they say I don’t have a choice. They’re like, “You shut up, because you get what you get.” I mean, really it’s like, you don’t really have a say. My question is, is it basically ICU for a couple of days right now, then when she wakes up, and whenever she’ll go to a subunit, like a step down unit, correct? From there they will ship out. How can I advocate saying, “I want physical therapy. I want this.”
Patrik: Have they mentioned step down unit next? Have they mentioned that?
Joyce: Well, they mentioned it way before she was even at that step. They were just marking it saying, she’ll probably be in the ICU. Then the minute she wakes up she’ll go to a step down unit, and then she’s getting shipped off to a subacute. Or they might go straight to the subacute. I don’t know, because everything is so full. That it’s like they’re so beyond capacity. I don’t know where they’re going to … I have no idea.
Joyce: I don’t know if I can even advocate physical therapy, nor I can do anything, because I’m in their thing. So what’s your thought?
Patrik: Do you know if she had physical therapy at all to this point?
Joyce: Never, she did not have physical therapy at all. By the way, when I looked at his foot, it’s really swollen, and her hands are very swollen. No physical therapy.
Patrik: Right. The swelling is definitely a side effect of being immobile for so long. But then again physical therapy would help.
Joyce: If they’re not giving it who can … Right now they’re like, “We’re not giving physical therapy.”
Patrik: Once she’s off sedation, and once it’s verified that she doesn’t need the blood pressure medication, they will probably send her to step down, which may not necessarily be a bad thing. In step down they may start physical therapy. It’s a question you should be asking. To keep her in the ICU for as long as possible. Let’s take the physical therapy issue aside for a moment, to advocate to stay in ICU, or in this particular hospital, even in step down for as long as possible, the argument from my perspective is always continuity of care.
Recommended links:
Patrik: So, imagine a critically ill patient going to subacute or LTAC. That is a disruption of a care episode of a critically ill patient. That is really a bad thought in my mind. Those people that needs continuity, not a disruption of a care episode.
Patrik: Then there are other issues. Once people go to subacute or to LTAC, they always bounce back into ICU. So, you’re disrupting the first care episode from ICU going into LTAC, and then you’re disrupting the next care episode, because you’re bouncing back into ICU.
Joyce: Patrik, you were completely frozen. So I missed that whole part.
Patrik: Sorry.
Joyce: You were just frozen then came back. Start with the fact that you said, you can advocate for physical therapy if you advocate to be in the ICU.
Patrik: Okay. The reason for advocacy to stay in ICU, or even in step down; one, step down is fine if she’s off the blood pressure medication, if she’s off sedation, step down will probably be fine. One advocacy route there is really continuity of care. So, from my experience, a critically ill patient needs continuity of care, not disruption of care. If she was to go to LTAC, or to subacute, that’s disruption of a care episode, right? Plus-
Joyce: How do I control that?
Patrik: Let me just illustrate that further. When someone goes to LTAC, in a situation like your sister is in, the chances of her bouncing back to ICU are pretty high. So, you’re disrupting the first care episode by her going to LTAC. Then potentially you’re disrupting the next care episode by her going back to ICU. And not necessarily the same ICU.
Patrik: I have seen patients going into the three places within days. That is unbelievable. That is so bad. Everything that your sister has achieved to this point could be gone within days.
Suggested links:
Joyce: What you’re saying is great. I don’t know if I have really a leg to stand on. That’s the problem. I know what it can be, but I’m really at this service, because from what I understand, from what everybody is telling me, they could do whatever they want with my sister.
Patrik: Yeah. They’re very good at saying that all the time. Hospitals are the master at telling you they’re operating in a vacuum. But we know they’re not.
Joyce: What can I say to them? Even if you need to call and start using these medical things. I can say just like what you said, but they’ll be like, “Sorry.” You know what I’m saying?
Patrik: Yeah.
Joyce: I can bring that up to her health provider, who by the way that’s not her hospital. So, I’d have to make the argument with them saying, “You guys are taking a huge liability by moving her,” and everything that you said. And I’ll have you get involved in that, but basically it’s us pleading our personal view, and it can go on deaf ears. Correct?
Patrik: Yeah. It could go on deaf ears, but there is two things to that. Have they suggested any subacute facilities? Have they suggested anything to you?
Joyce: No one has spoken to me about anything at all. I know you said you can buy time. When somebody does speak to me, you said I have to go check it out, I have to blah, blah, blah. You and I will speak again. I’ll do the cat and mouse game as much as I can to delay but they’ll say, “Well, you don’t have an option. This is the one place that she’ll go, and you don’t have an option.” But I’ll say, “Hold on, I can-
Patrik: They’ll probably give you a couple of options. They’ll probably give you two or three options, depending on bed availability of course. But what I’ve also learned, and what families have learned the hard away. They might give you an option in another state. I am not joking.
Recommended:
Joyce: Do I have an option-
Patrik: I’ve seen-
Joyce: Yeah, actually, somebody said that to me. She said, “If they have a subacute, they have the ability to send them there.”
Patrik: Absolutely. I’ve seen people going from state to state for LTAC.
Joyce: How do I stop that?
Patrik: Well, the way to stop that is … My argument in this situation, and I don’t know the legislation, but most of the time you need to give consent to the hospital for the transfer. The major issue that I can see is the health firm coming to you, They will come to you and saying, “Look, your sister is running out of ICU entitlements.” They could be putting that on your head.
Patrik: The hospital in and of itself, they can’t force you to give consent to get your sister to another hospital. But they can tell you, “Your sister is running out of ICU entitlements.”
Joyce: Let’s put that on the shelf now, and we can go on circles. I’m not going to waste your valuable time. That could be a possibility, but let’s shelf it and see what transpires.
Joyce: My other question to you is, what is something like this, going to a place where there is physical machine therapy … We know you talked about obviously doing it at home. Do you know of any place … Again, we don’t know if she’s going to need a ventilator, or is she going to need a BIPAP. We don’t know yet.
Joyce: My husband said, “You can’t do that. You have no idea how much it’s going to cost. You can lose everything.” She’s very conservative. She’s my sister though, and I’m not going to send her to a place she doesn’t deserve. She’s my sister. What are we looking at? And is that something that you think is even on the table?
RECOMMENDED:
Patrik: Okay. Giving you the short version there, Joyce. We have INTENSIVE CARE AT HOME here where we are taking ventilated patients or tracheostomized patients at home here in Melbourne all the time. We also look after medically complex patients that are not ventilated but have unstable airways. However, our clients are getting government funding, because the government sees value in what we’re doing. That’s number one.
Patrik: Even if you have government funding, number two is probably the bigger problem. Can someone pull this off? Because it’s a very specialist skill. If we take clients home here … We can take clients home here recently quickly, but we are experienced and we either take them home from ICU/PICU and we make sure they don’t go back to ICU/PICU from home because we send highly skilled ICU/PICU nurses into the home. We couldn’t do it as quick five years ago as we do it now.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!