Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Sister is Off the Sedation in ICU Now. Will She Come Off the Ventilator Soon?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to share this experience from one of my clients, Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU on a ventilator and Joyce is asking how long will it take for her sister to get off the ventilator.
How Long Can We Get Our Sister Off the Ventilator in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Patrik: They can’t talk. They might talk, they might revert back to having nightmares. There could be an element of her going … Worst case, one of the things that can happen is shemight go into ICU delirium. Have you heard of that?
Joyce: I’ve heard of delirium, but I don’t know really know what it is.
Patrik: It’s basically again a result of being in a prolonged induced coma. She wakes up, she has no recollection of what’s happened. She’s in this strange environment. She looks up the ceiling, she doesn’t know where she is. Of course people go mad, can’t talk.
Joyce: Then we’ll be like, “Hey, you’re here. We’re fine. This is happening to you. Blah, blah, blah.” And she’s just looking, not knowing what’s going on, because she can’t speak. How can she communicate?
RECOMMENDED:
Patrik: Eventually, hopefully once she’s got the movements back, maybe she can start to write, maybe. Maybe she can point her finger to a letter board. Bear in mind, the added on complexity at the moment for most ICU patients is, there is no family. If you and your family could be with her.
Joyce: We’re 24/7 on the camera.
Recommended:
Patrik: Sure, but it’s not the same than sitting next to her, and holding her hand, and talking to her.
Joyce: What am I going to do?
Patrik: This is new for me too. I have never seen families being locked out of ICU. I have never seen that.
Joyce: And I think the nurses also don’t know. I mean, they like the fact that we’re out of the way, but they also have the emotional component too. My question to you is, after speaking to you now, I’m kind of like … I thought today was good news, and now I’m freaking out. I guess there is no way to know how this is going to go.
Recommended links:
Patrik: There is no way to know how this is going to go. I do believe you bought your sister time. I do believe, give your sister some days to wake up. And maybe she’s at a point where she can make her own decision, maybe.
Joyce: Decisions for what?
Patrik: Lay out the options to her.
Joyce: I don’t think she has another option. Here is the deal, there is no option. There is an only option of going to LTAC, or whatever, subacute, whatever the different names are for them to get physical therapy if she’s on the ventilator. So there’s really not much.
Patrik: No, but she may come to the conclusion, if she can, she may come to the conclusion and she says, “Look-
Joyce: That she doesn’t do anything?
Patrik: Yeah.
Joyce: First goal is to get her out of the hospital, and then if she gets out of the hospital … If we can get her off the vents, unless she struggles, and doesn’t want that, then I can bring her home. From what the palliative care said, that there’ll be like … At least she can be home from a new hospice if that’s the case. You know what I’m saying?
Patrik: Yeah.
Joyce: But right now she’s off the sedation, so she can technically. That was our first goal, because we wasn’t able to go anywhere with the sedation that she was getting. Now that sedation is out, I don’t know if she’s not cognitive there, I still don’t think she can make decisions for herself.
Patrik: Yeah. Look, it is going to be a tricky one. It depends on how long does it take for her to wake up? If she is awake, what is his cognition like? It depends on all of those things. Again, that looks differently for everyone.
Joyce: I feel like maybe it’s cooler maybe if she could just breathe, and breathe, and all of a sudden something turns on, because the minute she’s awake, the lungs can work, you know?
Patrik: Sure. The minute she’s awake she should be starving to breathe herself. With the COVID, is she COVID positive still?
Joyce: Yes.
Patrik: She is?
Joyce: But that’s only … I mean, it stays in your system. Not to say she’s contagious, but she’s still testing positive.
Patrik: She could still infect other people basically.
Joyce: Well, no, because I think that they say after a certain amount she’s not infectious.
Patrik: She’s not infectious.
Joyce: It’s just the virus is still in your body.
Patrik: Sure.
Joyce: Like my mom is non-infectious but she’s still testing positive. But they said, “This can linger in your body for months.” I don’t think she’s infectious.
Patrik: I see. Yes. I think for now she needs to wake up. Then I guess from there we’ll take it from there.
Recommended:
Patrik: You’re going to take it from there. Look. The way I approach life, and I’m sure you do, last time I think you mentioned you’ve got a business yourself. Everything in life is negotiable. I know the hospitals don’t see it that way. The hospitals try to make rules all day, every day, but I’m a big believer, everything in life is negotiable. That’s the way to approach it.
Patrik: They probably already know that you’re not following their lead easily. They probably already have an inkling of that. They know that you’re researching, they know you’re not just going with the first option that’s being presented to you, and they know that you’re questioning. They already know you are probably different compared to most of the people they’re dealing with.
Patrik: The other issue that I hear at the moment by talking to clients is, there is definitely also issues around getting people into LTAC, because not all LTACs are taking COVID patients either. The whole-
Joyce: I mean, she could be stuck in the hospital, because the palliative care said, “Listen, if we have placement, we don’t have placement for her. She might be stuck here too.”
Patrik: Correct.
Joyce: So that’s also on the table, which is I work for a benefit.
Patrik: Correct. I’m talking to people from different places every day, what I’m hearing is, there are definitely bed locks in LTAC as well because of COVID. So, it’s not as simple as a year ago, absolutely. They would try to receive your sister out as quickly as possible.
Joyce: Her health insurance would have took her anyway. They would have wanted her back. But they have no bed, so they’re paying your hospital’s bill. They’re paying it because they’re not even trying to save money at this point.
Patrik: The environment is shifting at the moment, big time, because of … That’s why I’m also thinking, the argument for home care is getting bigger and bigger. Just on that level with COVID as well.
Joyce: I know it’s going to take … I mean, I think for this to be the mainstream like Australia is right now, I think we would be breaking the mold. But look, I am all about breaking the mold. And I’m all about trying to do whatever it takes. I guess today was a little bit of a win, because we’re off sedation.
Patrik: That is a win.
Suggested links:
Joyce: But we still have a long, long way to go, and it’s a matter of how she wakes up, and how long can we get her off the ventilator.
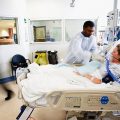
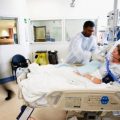
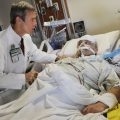
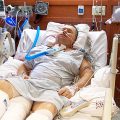
Patrik: Yeah. Can you show me your sister again?
Joyce: Yes.
Patrik: Can you do that?
Joyce: Hold on.
Patrik: I’ll tell you something that I can see straight away.
Joyce: Okay.
Patrik: She needs to get up the bed. They need to pull her up the bed, and sit her up 30 degrees. She’s lying too flat to get off the ventilator, lying too flat.
Joyce: I ask that for the nurse?
Patrik: Yeah, nurse, absolutely.
Joyce: Will they just pull her right up the bed?
Patrik: Yeah. But they need to pull her up a little bit. That pillow, I can see it’s stressed … It should be under her neck. It looks uncomfortable to me.
Joyce: Yeah.
Patrik: Her neck is sort of tilted.
Joyce: Right.
Patrik: Her neck should be straight, and she should be sitting up 30 degrees.
Joyce: So, maybe she should sit up, they should just move the bed up?
Patrik: Absolutely. You can’t get someone off the ventilator by lying flat, you just can’t.
Joyce: Here is the problem, they don’t think … I will tell the nurse today, which I think she’s in ICU for 35 years. I’ll ask her if she can move her up. The problem is I can’t tell them what to … I mean, I can try-
Patrik: Of course, I know.
Joyce: But you know how it is. The pulmonologist, he says, “You shouldn’t be monitoring anything. You don’t have a doctor degree. You shouldn’t be,” I said, what about my advocacy? He said, “You shouldn’t advocate. You should let us do our job. Stay out of it.” I’m a little feisty person. But again, he’s the pulmonologist, he’s the doctor, I have to shut up, what am I going to do?
Recommended:
Patrik: Absolutely. I mean, you’re a business woman, I’m a business owner. Entrepreneurs don’t listen to other people, they just do what they do.
Joyce: But in this situation I can’t stop, I’ll move.
Patrik: I know, of course.
Joyce: I would, trust me Patrik, I would move mountains for my sister if they let me in the door.
Patrik: Of course, the biggest challenge is at the moment, and I see it across the board, families can’t be with their loved one. It’s terrible. It’s an unprecedented situation. It would be difficult enough if you were there in person, but you have way more leverage if you’re in front of people, way more leverage.
Joyce: Absolutely.
Patrik: It’s unprecedented on that level too, but I also believe the argument for home care, as long as the pandemic is going on, and even once this pandemic has settled down with vaccines, and whatnot, the argument for home care won’t go out of the window at all. The pandemic has shown everyone who wants to be in a hospital.
Joyce: Listen, if her insurance goes, “But again, you’re talking 20, 30,000, that’s a lot.”
Patrik: Don’t be discouraged by that Joyce. Don’t be discouraged by the figures. It’s pocket money for them.
Joyce: I mean, look, listen, I will have you back for me once we’re there. You said a lot of information today. My recap is, once I ask the nurse all these settings, I’m going to text it to you.
RECOMMENDED:
Patrik: Please.
Joyce: So you could just tell me where I’m at. I’m going to wait for her to wake up. I’m going to tell them to go sit up. I’m going to actually call her, tell her to pull her up, let’s see how she takes that critique. When my sister wakes up, what advice would you give me from the emotional standpoint? Tell her, “You’re going to be okay. We’re with you.” Just that encouragement … I’m just freaking out.
Patrik: Yeah. You don’t necessarily have to tell her she’s okay. I mean, positivity I believe helps. But at the same time you don’t want to sort of mislead her either. Probably depends on how cognizant she is. It depends on a number of things. You know your sister best.
Joyce: Right.
Patrik: I do believe, it’s so important for her to hear you. I do believe that is so important.
Joyce: Do you think she still hears me now? I mean.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!