Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in the last episode was
You can check out last weeks question by clicking on the link here.
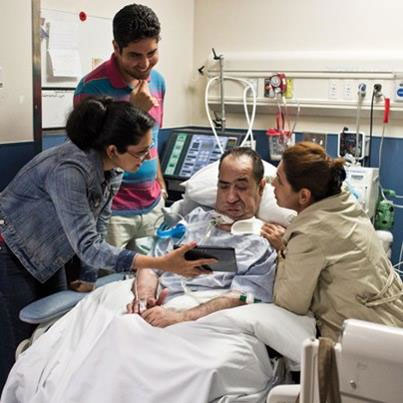
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to continue answering the next questions regarding James’ and Christine’s Dad in ICU who’s had a haemorrhagic stroke.
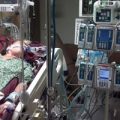
James’ and Christine’s Dad had a brain decompression where they evacuated a large bleed from his brain after the haemorrhagic stroke. And their Dad also underwent a craniectomy (partial removal of skull) to decrease the brain pressures after the bleed.
James’ and his sister Christine were getting their Dad in one of the best hospitals in the USA, the Cleveland clinic in Ohio.
In the meantime, their Dad was getting a tracheostomy because he couldn’t be weaned off the ventilator and the breathing tube. He also had a PEG tube for feeding inserted.
He also had ongoing seizures due to the stroke and his anti-seizure medications needed to be optimized so he could “wake up” and progress to Neurology Rehabilitation.
In today’s 1:1 consulting and advocacy sessions with James and his sister Christine, we look at some setbacks their Dad is going through.
He had to be put back on the ventilator due to a Pneumonia and he also ended up with a central line (CVC) and arterial line again.
In the meantime he has come off the ventilator but still has the tracheostomy after over 5 weeks in ICU.
This series of 1:1 consulting and advocacy is a real testimony for getting advice, run with it and get results.
If you want to avoid LTAC and a nursing home for your loved one, you need to read all of the consulting and advocacy sessions with James and Christine!
So in today’s episode of “YOUR QUESTIONS ANSWERED”, I answer a series of questions from James and his sister Christine again that are excerpts from various 1:1 phone/email consulting and advocacy session with me and the topic this week as part of this series of 1:1 consulting and advocacy session with me and the topic this week is
Is it best for my Dad to go from ICU to step-down or should he be going to Rehabilitation straight away?
You can also read or watch previous episodes of 1:1 consulting and advocacy with James and his sister Christine here
Let’s dive into James’ questions.
Thanks Patrik. Good advice.
Why do you suppose neurosurgery is saying one thing and epilepsy team is saying another??
This is very frustrating because it is a form of neglect.
They have neglected to manage his seizures and I have neglected to give him physical therapy.
Physical Therapy says he keeps sliding out of the chair so they sat him on the side of the bed today for 25 minutes. That’s simply not enough time!
Do you have any suggestions on how to get him more Physical Therapy?
Many thanks
James
Hi James,
I think it’ll be very important to find out who is the primary decision maker now.
There must be either a doctor or a speciality he has been admitted under. They will be the one calling the shots.
Maybe the Epilepsy team wants to get the meds sorted before moving on (which I think is a good sign) and maybe Neurosurgery wants the discharge because of potential bed blocks, especially if Neurosurgery is the parent team.
Agreed that if they are not communicating that this could well be neglectful.
On the other hand, as I have said right from the start, your Dad is on a long road to recovery with an uncertain outcome, therefore always keep checking your as well as their level of frustration.
Especially with the brain being so unpredictable there will be a lot of frustration and uncertainty that needs to be managed. I know it’s easier said than done, take one day at the time.
Even though Epilepsy and Neurosurgery are related specialities, they are two separate teams and they may or may not work well together.
Physical therapy is certainly challenging and it usually works well if the nurses are involved as well. With him now in step down he probably has one nurse looking after two, three or even four Patients on a shift as opposed to 1:1 nursing in ICU.
They will need to continue doing Physical Therapy daily and sitting him on the edge of the bed is good, if he’s sliding off the chair he may well be considered a “high falls risk” and it could well limit the time he maybe able to spend in a chair.
Recovery with a brain injury/stroke will happen over time and will take a lot of rehabilitation, nurturing, patience, persistence and a positive environment!
Stay positive and try and embrace that your Dad’s recovery is a process and not an event. This makes time lines impossible to predict at this stage. It’s a puzzle where many things have to align for him to move forward.
He’s still only in step down, meaning he’s in between ICU and the hospital ward. It also means he’s not ready to be discharged yet to a hospital ward if he’s at risk of having seizures.
Kind Regards
Patrik
Hi Patrik,
More great advice!
Hospital still very insistent on us getting out however the seizure team has now agreed to drop my father’s dose of Keppra from 3500 to 0 at 500 mg increments per day.
He is still on Dilantin and the other medication Zonisamide.
My question to you and my concern is are they are weaning him off of Keppra too fast???
I believe his cognition seems to be better even with a smaller dose he was able to say my sisters name today.
Recommended:
Schedule your free appointment here
However, I don’t want him to have a setback and have a seizure because our days in the hospital are numbered and I don’t believe once we leave the stuff is going to be that helpful in managing his medication.
Also we are probably going to take him to Chicago for a very aggressive rehabilitation hospital with just the flap.
I feel like my father is almost optimized however we may be one week premature.
Please let me know your thoughts on all of the above in writing so I can refer back to it in my notes.
Thank you.
James
Hi James,
No, I don’t think they wean him off too quickly.
Weaning Keppra sounds good as long as Dilantin and the other drug Zonisamide is being given.
They need to wean now while he’s still in hospital, monitored by an epilepsy team.
Setback may still happen, remember 2 steps forward and one step back.
They need to take measured steps now to optimize for rehab wherever it will take place.
Here is also a quick summary of what we discussed over the phone
- Try and find out if they want to keep the tracheostomy for the purpose of ventilating your Dad during the surgery or if they think it can be removed soon!
- Try and speak to Medicare and find out what his entitlements really are
- Remind them that moving around different facilities/ hospitals over the next few weeks is not going to be conducive for his recovery. Consistency of care is going to be important, especially with the ongoing confusion and delirium
- Also remind them that your Dad mentioned he doesn’t want to be moved (yet)
- You could also argue that seizure activity needs to be monitored for a few more days after he has come off the Keppra completely. Having another seizure could set back your Dad significantly and nobody would want that. LTAC (Long-term acute care) is not equipped to be closely monitoring any seizure activity
- Overall I do believe your Dad is making progress and I believe he’s coming very close to be leaving step down and that’s a good sign! Moving him to LTAC, then back to Hospital for the surgery and then potentially going to Chicago sounds very stressful and it is not the type of stress your Dad might need at this phase of his recovery, this is the level you should argue on
- Furthermore, I’m a big believer that everything in life is negotiable and I think you should put your best foot forward and see how far you can go with arguing on that level. Clinically I can’t see anything life threatening that may warrant to stay in step down, however arguing on all the other levels is definitely worth a try
I hope that helps James, let me know what else you need or if you need further clarification of those points!
Kind Regards
Patrik
Recommended:
Hi Patrik,
Great advice again thank you very much!
Thank you so much for the information.
I pleaded my case with the doctor today and believe I will be able to keep him in the hospital as opposed to going to LTAC based on your explanation of continuity!
You’re not just in ICU expert. I believe you understand the healthcare system very well And I value your judgement
Touch base with you soon
thank you again.
James
Hi James,
That’s great, well done thank you for letting me know!
If you found a strategy that works keep doing more of it and not less!
Thank you James for your kind words.
I tend to know which buttons need to be pushed to get to where you want to go. It also helps that you are not timid to implement. You are your Dad’s best advocate!
No matter my advice, you are the implementer and many families are often too timid or intimidated to implement!
So give yourself a pad on your back for implementing!
Very happy to help where I can.
Please see a quick summary from our conversation below
- Try and keep buying time in hospital if you can
- Talk to Patient affairs and keep arguing on the level of “Patient care continuity” and also the stresses of moving him to different facilities. Your Dad will need consistency and you don’t want to jeopardize any recovery he has already made
- Weigh up the pros and cons of going to Chicago vs going home. Home is not impossible but he may benefit from a rehab facility first
- Getting him to rehab within the Cleveland clinic might be dependent on the availability of skilled nursing staff who have the skills and expertise to manage his tracheostomy
- Getting the Cranioplasty done now and then move to rehab to Chicago would eliminate a transfer back to Cleveland. As I said, I don’t think moving him around from hospital to hospital will benefit your Dad and it would be very stressful to do so
- Your Dad is still in a vulnerable position, keep reminding them
- Their “one size fits all” approach to moving Patients along their pathways might fail in your Dad’s situation because of him coming from interstate and having limited family support around him. Their approach needs to be more tailored towards your and your Dad’s individual situation
I would really suggest to get the Cranioplasty done soon and then you are free to move either back home or to Chicago.
I hope this helps.
Any questions please let me know.
Kind Regards
Patrik
Let me know if you need anything!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!