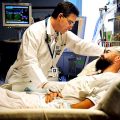
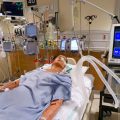
Hi, it’s PatrikHutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU ventilated and on sedation. Joyce is asking why the ICU team talks about DNR (Do Not Resuscitate) too early.
My Sister is in ICU on a Ventilator and Sedation. Why Does the ICU Team Talks About DNR (Do Not Resuscitate) Too Early?
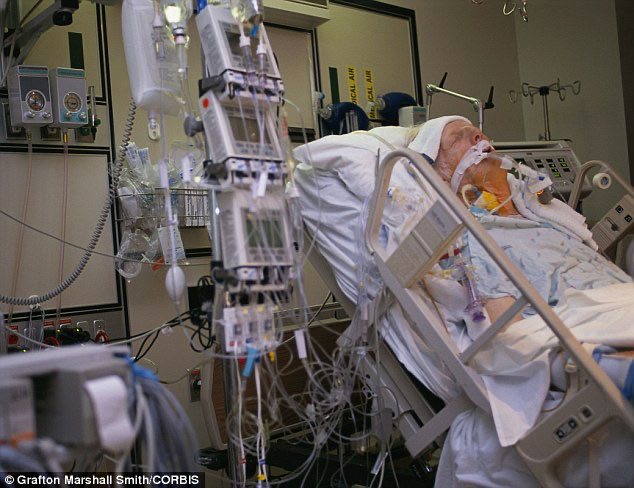
Joyce: Something like that or if it’s bigger. They say they’re going to put someone on board that does those surgeries and be able to cut and put a tube.
Patrik: Yes, a chest drain to drain secretions that are sitting on the peripheries. Okay, that makes sense. Again, the longer someone is ventilated, especially with COVID and the ARDS. Have you heard of ARDS, A-R-D-S?
Joyce: Yes. Yes, and that’s what she has. She’s developed that, yes. Her lungs are now stiff.
Patrik: Yeah, very stiff and there would be some fluid accumulation. So again, nothing on. Well, something that should be prevented, but again, you see this quite frequently in ARDS.
Patrik: Okay, you as a family, the medical power of attorney for your sister?
Joyce: Technically, yes. But the rest of us siblings, we’re advocating for her and we all discuss as a unit and we’re pretty much in sync.
Patrik: Is there an advanced care directive? Do you know what I mean? Does your sister have-
Joyce: No.
Patrik: No.
Joyce: No.
Patrik: Okay. Has there been any talk about limiting treatment or about DNR?
Joyce: Yeah. They brought it up to us. They’re basically kind of prepping us for that. A DNR, do not resuscitate. They say basically there’s a zero chance… They actually said, “There is a zero chance of surviving it,” right? The guy said zero chance.
Jane: Because they have to stood up and they won’t make it on time.
Joyce: Most likely there’s a zero chance, but we did not comment on that. Then also they were kind of pushing us saying, “Look, you don’t want the trach.” Joey, who’s the social worker guy I’m talking to every day or the head nurse there is painting a different picture and he basically says, “You should probably think of… You got to figure out which way we’re going, but do you want her to keep suffering.” So there’s been massaging I think.
Patrik: Sure, but you haven’t signed the DNR?
Joyce: No.
Jane: Nope.
Patrik: All right, okay. That’s probably enough information. With the COVID, what have they done to treat it? They’ve given her Remdesivir, they’ve given her dexamethasone.
RECOMMENDED:
Joyce: They’ve given her another anti- inflammatory.
Jojo: Plasma.
Joyce: What is it?
Patrik: Plasma.
Jojo Plasma.
Joyce: Plasma.
Patrik: What about nitric oxide?
Joyce: I don’t know what that is.
Patrik: Okay nitric oxide is a gas that they insert into the ventilator for a period of time. It can be very effective.
Joyce: Yeah, hold on.
Patrik: Nitric oxide.
Joyce: Okay, nitro oxide
Patrik: N-I-T-R-I-C oxide, O-X-I-D-E. Another medication that can be given in ARDS is a nebulizer Flolan, F-L-O-L-A-N. There is another name for it. I need to go get it, but…
Joyce: Okay, can you email this?
Patrik: Yeah, I’ll email that to you. Yes, I’ll email that to you.
Joyce: Thank you.
Patrik: Okay. So now coming to bigger picture. 90% of patients in ICU survive, that’s 9 out 10 survive, okay? ICUs are always negative by default, always. So you always have to read between the lines, the overwhelming majority of patients in ICU survive. Now, that’s not talking about quality of life. That’s talking about leaving intensive care alive. Not qualifying that, just saying 90% of patients leave intensive care alive.
Patrik: So the negativity you can almost forget about because it’s not reality. If you look at pure statistics, 90% of patients survive. So that’s the negativity sort of taken care of. Why are they negative? They need to manage their beds, they need to manage that downside, which is if they’re telling you, “Yep, right now we’ll treat your sister for two weeks and then she’ll leave ICU alive,” if that’s not going to happen you could sue them. So they’re managing their downside by being negative. That’s number two.
RECOMMENDED:
Patrik: They’re managing their beds. Even outside of COVID ICU beds are in high, high demand. Now it’s gone through the roof. So they’ve got people knocking at their door that they can’t take, so any bed that they can empty, whether it be by doing a trach and sending them onto LTAC or by letting people die, is a bed that they can free up. Again, it’s unfortunate. It’s been an unfortunate reality before COVID being heightened at the moment. So that’s sort of the bigger picture.
Patrik: We have certainly seen that tracheostomies are being delayed with COVID because of ARDS, because of high PEEP, because of high FiO2. Normally, day 10 to day 14, you should be looking at trach for all the reasons that you’ve already come up with in terms of too much sedation. As soon as patients have a trach, sedation can be stopped most of the time and people can wake up, they wean off the ventilator in their own time. There’s no guarantee for that. Some people do end up on a ventilator and a trach for the rest of their lives, that does happen.
Patrik: I would argue with COVID the fuller picture hasn’t really emerged yet in terms of when COVID patients with ARDS end up with a trach, what does that look like compared to people having a trach before COVID? But in terms of, people can live with a trach and people report a good quality of life with trach, but the goal for a trach should always be to wean off the ventilator. That should always be the goal for a trach, it should not be the goal for someone to live on a ventilator with a trach for the rest of their lives, unless they have injuries such as spinal injury after an accident, that’s a different story, but for someone with COVID ARDS the goal should be trach temporarily, wean them off the ventilator and hopefully get back to normality as much as possible.
Patrik: What does that look like in reality? My biggest concern is a lot of patients in the ICU end up with a trach and then they send them to LTAC. I don’t know what you know about LTAC. Do you know anything?
Joyce: We just know that the nurse is saying exactly what you’re saying. If she would qualify for a trach she will be sent off to LTAC and he said it’s a nursing home, obviously with kind of like an ICU, but a nursing home, and it’s only three four options. They only thing is if they’re full at the moment, they will have to keep her until something becomes available. So I don’t know what our rights are because I watched your video, so I know how you feel about that.
Patrik: So LTAC is probably a euphemism for nursing home. I feel very negative about LTACs for all the reasons. Anybody with a ventilator and a tracheostomy does need an ICU team around them, right? It doesn’t happen in LTAC. LTACs have been designed to save money and not for clinical need. LTACs have been designed to save money for the insurances, definitely not for clinical need.
Patrik: So your sister health’s insurance is paying $5,000 a day at the moment, they go to LTAC, that cost goes down to, I don’t know, $1,000, $1,500 and people are at risk of either dying because they don’t the care what they need or they’re at risk of bouncing back to ICU and next thing you know is they’re back in an ICU that they weren’t in before because there’s no bed or different location. Anybody in a situation like that needs consistency of care, not being shifted around to other facilities. The LTAC is such an irony from my experience and that’s probably-
Joyce: What’s our rights though because when I spoke to the doctor he said we don’t have rights.
Patrik: Of course. Hospitals are very good to pretend they’re operating in a vacuum. They’re very good to pretend and say, “Yep, we’ll do whatever we want to do and just sit by idly.” That’s certainly not the case. Unless your health insurance is coming to you and says, “Look, we need to stop paying for your sister’s ICU bed,” you have every right. If the insurance comes to you and says, “Look, your sister is running out of entitlements,” okay, all right, that’s probably a different story, but from my experience, unless you sign a piece of paper-
RECOMMENDED:
Joyce: How do I stop it? How do we go… because I know we’re covering a lot, but if we were to consider a trach and that will give her a chance to keep on fighting, but the only way we would agree, I think, is that she be kept in the ICU and there’s a certain period of time that we will probably decide saying, “All right, look, we’ll give this another month. We’ll track it. If we don’t see much results then we can make peace but whatever,” but I will be damned if I will be rushed one week and just let her dwindle. I will not give up.
Jane: I have a question before. What’s the criteria for having a trach because right now she’s running on 70, the PEEP at 8, but 70 and her heartbeat was really fast this morning. They didn’t even tell us right now that even if we have a chance to get it.
Joyce: Right.
Patrik: Look, you mentioned earlier that the criteria is quite simple, 10-14 days on a ventilator with a breathing tube, the inability of weaning off the ventilator, and then a PEEP of 8 or less and FiO2, 45%, 50% of less. That’s pretty much the criteria. The COVID has thrown that criteria upside down definitely because the risk for staff to get infected when they’re doing a trach is huge, with all the people.
Jane: So, I don’t know, did he even give us the talk about being a trach.
Joyce: The nurse said we have to advocate. The reason, Patrik, we have you on, the nurse said to me this, “You need to guys know what you want.” Tuesday I have a meeting. We need to speak to you and our rights and what we can do because if we advocate tomorrow, we say, “This is what we want. You need to turn the world upside down to give this to us,” then they will do it, but we can’t be wishy-washy about it.
Patrik: No, you can’t be wishy-washy about it, definitely you can’t. The reality is that if your sister won’t have a trach, she will stay sedated with a breathing tube, assuming he can’t wean off the ventilator. When someone is in an induced coma for too long they’re deconditioning very rapidly, they’re losing all their muscles. Your sister might wake up eventually, but may not have the strength to come back. The minute he can have a trach they can at least lower sedation and that gives room for her to start moving, even if it’s only moving her arms or her legs. It’s simple things like that.
Patrik: So the recovery time after a trach has been done can certainly be shortened because the breathing tube is so uncomfortable that it can only be managed with an induced coma.
SUGGESTED ARTICLES:
Joyce: So she’ll never be weaned off because it’s literally we are just wasting time. Every day that we go by we have wasted a day.
Patrik: Correct. Let me ask you a few other questions. Do you know if she’s on vasopressors or Inotropes? Do you know what I mean by that, epinephrine, norepinephrine?
Joyce: I do not know.
Jane: Never heard of that.
Patrik: Okay. Big question to ask because she would have been on that at some point. It’s considered life support. Basically when someone is in induced coma, their blood pressure goes down, they end up on medication to maintain a blood pressure that’s compatible with life.
Joyce: She was on that. I don’t know the name, but she was on medication to keep it, because when they keep her sedated they gave her something to keep her blood pressure up because it went so low because of the sedation. I’m not sure of the name, but I’m sure she was on that.
RECOMMENDED:
Patrik: I’m sure she was on it too, and if she’s still on that, chances for her to go to LTAC are pretty slim. So it also depends what’s going on or things such as I talked about nitric oxide earlier, I talked about Flolan. If she requires any of that, chances for her to go to LTAC are pretty slim because they couldn’t manage that there.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!