Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
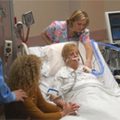
In this episode of “YOUR QUESTIONS ANSWERED“ I want to share this experience from one of my clients, Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU on a ventilator and on sedation. Joyce is grateful for our advocacy and consulting service because it gave her sister a fighting chance to survive in ICU.
You Gave My Sister a Fighting Chance to Survive in ICU with your Advocacy and Consulting Service. Thank you!
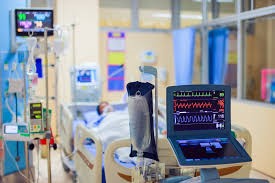
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Joyce: It’s a smaller hospital. So they said they did tracheostomy to one person throughout the whole eight months. So I don’t think my sister is their typical case because she’s still showing… He says, “Why move your sister, she’s so unstable?” But she’s still showing that she’s staying at 55. So if it was getting severely worse, wouldn’t the oxygen jump up at 80 to 100?
Patrik: No, not necessarily. If it was getting worse, her CO2 would probably go up. Her carbon dioxide would probably go up as well. Not necessarily oxygen would go down. So there’s two indicators when someone is on ventilator that you’d be looking at. Number one is oxygen levels in the blood, but also carbon dioxide level in the blood. So I would want to know what her carbon dioxide levels are. You don’t necessarily have to go up with oxygen. If carbon dioxide goes up, you will see the-
Joyce: Is that the oxygen in the blood?
Patrik: No, no, no, no. Carbon dioxide is what we exhale.
Joyce: Okay. So hold on. Can you… wait, carbon-
Patrik: Yeah, I can email that to you.
Joyce: Email it to me, because I’m going to ask them.
Patrik: Yep. So I don’t think it’s carbon dioxide is that bad with the people of… Now that you mentioned she’s in a small hospital, how many ICU beds?
Joyce: I didn’t get the number, but I am sure that-
Patrik: 10 or less?
RECOMMENDED:
Joyce: 10 or less, for sure. I’ll tell you this, because I buy lunch and we do stuff for the nurses all the time just to get whatever we can get out of them and show them appreciation, of course. There’s a max of 15 nurses, max. They have about two patients max in the ICU. That would give us about 10 and less for sure.
Patrik: So no, this is very important information. So you are basically saying that even now with COVID, she is the second patient getting a tracheostomy this year?
Joyce: Correct. She said there were two people that transferred with trache.
Patrik: Okay. Okay. No, that is very important information. So most ICU’s that I’ve worked in were big metropolitan ICUs with… Last ICU I worked in was 45 or 50 beds. So if you work in a big metropolitan ICU, it’s probably three, four traches happening every day.
Joyce: Okay. So what does that mean?
Patrik: Well, what does that mean? The big metropolitan ICUs has a wealth of knowledge because they’re dealing with trauma. They’re dealing with heart conditions. They’re dealing with lung conditions. The exposure to the sickest patients is there all day, every day. So I argue that with COVID now, your sister with ARDS outside of COVID, they might have transferred your sister to a bigger hospital straight away at the beginning of ARDS.
Joyce: Well, she didn’t have it right away, she developed it, the problem with her hospital, they said she would have been stable enough to go there in a couple of days ago, but her hospital has no beds. I’m sure they have beds, but I’m sure in my sister’s ICU situation, they probably didn’t want to take the risk of the transfer. And listen, trust me, I’m sure they have a caseworker on my sister’s case. And they’re paying that bill every day and I’m sure they just doesn’t want to take the liability because God forbid, I don’t know what the… If they transfer her and she’s unstable and she goes on their watch, I’m sure there’s some kind of a liability there. So they just said, “Keep her.”
Joyce: I’m trying to think, I was in better hands because I think that the service, the phone call is right, spot on. The service while you’re getting a hold of somebody is right. Her hospital would have been a nightmare because you can’t even get a hold of somebody, even if your life depended on it. They’re like a factory. So I feel like I’m in a good place in a sense that I need that cuddling. I need that cuddling, like hold my hand, give me access to my sister. And we have that. And we have that. So regardless small or not, that won’t-
Patrik: But small means limited exposure to sick people. That’s what small means.
Joyce: Right. But there’s nothing I could do.
Patrik: Oh, look, there’s probably nothing you can do now. I should have asked that question on Sunday because my experience is there’s pros and cons for bigger and smaller ICUs, but a big disadvantage of a smaller ICU is just simply not enough exposure to the sickest patients there are.
Joyce: And that’s what I feel, because they said we have to find someone who’s willing to do it. And then they’re still playing me around. And every day that goes by, her numbers are not improving. So I’m like, hello, their urgency wasn’t there, and that pissed me off.
Patrik: And also, smaller ICUs, they definitely need the bed. Definitely bigger ICU has more capacity to absorb. They have more resources. Smaller ICUs, if there’s 10 beds, she’s taking up 10% of their bed capacity. That’s huge. That’s huge.
Joyce: Oh, okay. So Patrik, here’s what we’re going to do. I’m going to wait for the… I just hope this Joey guy is not going to try to play with the numbers to get my sister out. But he can’t do that, because I would have to get record. He can’t do that, right? That would not be medical sound to try to fab the numbers, right? That would not be medical… No, I’m just scared now the guy wants her out and they’re…
Patrik: Yeah. Look, he wants her out but at the end of the day, he’s at your mercy for consent. He can’t just-
Recommended:
Joyce: Okay. I’m so happy I spoke to you. You are right now in my fighting corner. You and I will speak many, many times throughout the process because I trust you 100% more than I do anybody else. And I did think it was very weird that he called me on the side. I thought that was very strange.
Joyce: I’m going to now get a conversation with everybody, get back on board. I’m going to do this procedure and I’m not going to let him paint me this picture, because listen, I don’t have to be six months into it. If I see her struggling, pull the plug, but why do I have to do it now? Why do I have to live the fact that that’s what would be on his grave site and say, I didn’t do anything I could.
Patrik: The closure aspect, when it comes to end of life is so important, I believe, and ICUs don’t have the appreciation of giving people the time they need to come to terms. And I understand why ICUs don’t have the time. I get that. I’ve been in the environment. I know the demand. I get that. But for families, this is so important.
Recommended:
Joyce: Should I just be patiently await for the consult or should I keep asking the doctor saying, “When is the consult coming?” How can I push this farther?
Patrik: What have they told you? What are their next steps? Have they given you any timelines?
Joyce: When I spoke to Joey today he said that there had been an order to get doctor whoever is going to do a consult today. And he will be contacting us today to see where we’re at. So I’m hoping now that he is a candidate for a tracheostomy.
Patrik: Here is the other thing, Joyce. So in a big ICU, 40 beds, 30, 40, 50 beds, most ICU teams do it at the bedside. They don’t even consult the surgeon anymore. So this is another sign to me that they need to go externally or wherever they need to get a surgeon from. It sounds very cumbersome. In a big ICU, if they think it’s safe, they get a team together, ICU doctors, an anesthetist and done, 30, 40 minutes done.
Joyce: Okay. So should I call Joey and tell him… Or you know what I should do, I should actually call Joey back and when I get Joey on the phone and I’ll say, “Joey, I spoke to my family and they’re 100% moving forward with the trache,” just so he knows my mindset because I think he shook me up and he actually made me cry and he actually made me second question myself where my mind was going over. But I think I should call him back today and say, “Just so you know, we’re 100, 1000% moving forward. Let me know when the doctors are…” Just so he knows that we’re moving still ahead. I think that’s what I’m going to do. I’m going to call him right now and tell him, don’t mess with me.
Patrik: Yeah. Who is he? Is he an intensivist? What’s his title?
Joey: Joey is palliative care. He’s an ICU head nurse, and I think he works with palliative care. I don’t know what palliative care means.
Patrik: Yeah. I tell you what palliative care means. So palliative care means two things. You can get palliative care involved for end of life care, but you can also get palliative care involved for pain management. Unfortunately nine times out of 10, when palliative care is involved in a hospital in ICU, in particular, it’s for end of life care. Are you saying this is a nurse, not a doctor?
Joyce: He is a nurse. He’s a head nurse. And the funny thing is, I actually left the doctor a message this morning, and I’m not getting a lot of communication with the doctor. So Joey calls me every day. But he is an ICU head nurse that he’s been around for long years. He said, he’d been in ICU. And the thing is, he said, “I’ve been in ICU for long years and I’ve seen this go down and you don’t want to be on the thing.” But I think he’s babysitting me. Listen, there’s something in my stomach, and the reason I contacted you and I went out of my way to Google and see who can help me is when the doctor actually told me that A, I can be an advocate and just basically let us do what we need to do, and B he said, I don’t have a leg to stand on because, “We know what we’re doing, leave me alone.”
Recommended:
Joyce: And when he said that to me, all of these red flags went in my head, and that’s when I saw you and I was surprised you even picked up the phone because you were so accessible. I think what was meant to be was meant to be.
Joyce: So I’m going to call Joey and tell him we are 100% moving forward. I’m going to find out what the doctor will say. And we will fight. If she’s not a candidate today, who’s to say that she won’t be a candidate tomorrow, right? Just because I think today her numbers are a little off, I can still say, “Hey, when she’s ready to have the numbers, we want that trached up.” Correct?
Patrik: Yeah. So on Sunday, I think the numbers were 60% and PEEP of 10?
Joyce: Today it’s 55.
Patrik: 55, PEEP of eight?
Joyce: No, PEEP of eight. She’s been consistent and PEEP at eight and she’s at 55 at the moment. She went up to 70 this morning because of the sedation or whatever, but he moved down to 55.
Patrik: She’s probably not quite there yet. But the first thing they need to do is there needs to be a surgeon assessing the stricture and then go from there. But again, this is a sign. In a big ICU, the ICU team would go at the bedside.
Joyce: They would’ve had it already. And they also said, “We got to find someone willing to do it.” And I’m like, willing to do it? What is willing to do it? I mean, I get the COVID aspect, but don’t say willing because my sister is… I get it. But my sister’s life is on the line. So if I’m going to a hospital and you can’t give me the service of saving this patient’s life, then what’s the point of being in ICU if you have to find someone who’s willing to do it?
Joyce: I can’t go to a car mechanic and say, are you willing to fix my car? They have to do it. It’s I have to, not a willing. That willing, someone willing to do it, didn’t sit well with me because what do you mean willing? Not a will. You got to find it.
Patrik: Joyce, this is what I’m saying all the way long. ICUs or hospitals in particular are so good at pretending they’re operating in a vacuum, they can do whatever they want. It’s not the case. You just need to, just like they are trying to push the right buttons, unfortunately you have to push the right buttons too.
Joyce: Okay. So let’s shelf this here. I’m going to advocate right now to call Joey saying, we’re going with it 100%. I’m going to follow up with the guy who’s going to evaluate too… Whatever he says to me, I will follow up with you again. Question-wise, you have to keep sending me links to these conversations?
Recommended links:
Patrik: To Zoom?
Joyce: Yes. No. Well, My question is there is links that I can purchase independently, right? Or do you go-
Patrik: I’ll send you another email-
Joyce: Send me another one.
Patrik: … with all the links. I’ll send you another email with the links.
Joyce: Send me another one. And let’s adjourn. I will definitely have you back here tomorrow depending. And I’ll leave you messages.
Patrik: Yeah, please.
Joyce: And you get my texts, right? I can text you with my number?
Patrik: Yes, you can text. You can make an international text, WhatsApp?
Joyce: I can add you. Yeah. If you give me your number on WhatsApp, I can add you to WhatsApp.
Patrik: I’ll send you a text.
Joyce: Give you the exact numbers I have to put you under, so it pops up on WhatsApp and I will text you on your WhatsApp because I know you have to sleep, but we’re in… So whatever, we’ll do. But I’m telling you this is my sister’s life. I need an advocate and I need to know how to set my mind straight. You totally brought me back to this world that I need to be. And even my siblings didn’t want to take this call because they’re thinking I’m making soup of everything because they don’t want too much information. I am completely the opposite. I want to get underneath the hood and get everything in it. They don’t want to know.
Patrik: Yeah, it’s very confrontational. And most people can’t deal with it. Most people give in because it’s too confrontational and I understand that it is incredibly confrontational.
Joyce: Yep. Okay. Okay. All right. So Patrik, that’s where we’re at. I’m going to get on it today, and we’ll talk again tomorrow.
RECOMMENDED:
Patrik: Okay. All right.
Joyce: Just send me that number so I can WhatsApp you.
Patrik: Yes, I will be in touch. Will WhatsApp you in a second.
Joyce: Okay. Thanks Patrik. Talk to you soon. Bye-bye.
Patrik: Take care. Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!