Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
What Would Be My Sister’s Quality of Life After Being on a Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
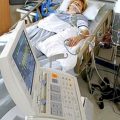
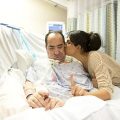
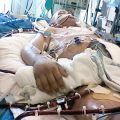
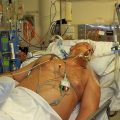
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU sedated and on a ventilator. Joyce is asking, what are the odds of keeping her sister on a ventilator?
What Are the Odds of Keeping My Sister in ICU on a Ventilator?
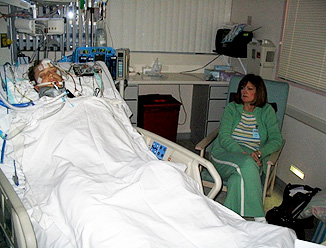
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Jane: So as a choice, we can put her under ventilator any longer, so what would be our choices?
Patrik: The choice you could, you remove the ventilator, not do anything, not give any medication, but that could mean suffering, could be a quick death, might not be a quick death, nobody knows.
RECOMMENDED:
Jane: But you can’t even say later because they said like 25, 23 that’s it. Like they’re saying this woman was on the ventilator for 21 days and she passed away from cardiac arrest, which was a really bad death, you couldn’t even see it, it was horrible. So that’s the question. I don’t want my sister to go in pain. I don’t.
Patrik: Yeah.
Joyce: And the question is what are the odds of. So right, we’re saying, but then again if we keep a little longer, maybe we have a little bit more hope, maybe there’s still hope with the sedation, you said the lungs get better, right?
Recommended links:
Patrik: Look, the dilemma here is people can stay alive for a long time with life support, that’s all doable. The challenge is what does the quality of life look like, is that acceptable for the person and for the family? That is the challenge, and there is no right or wrong answer. There are people that live a quality of life at home on a ventilator with a tracheostomy, they’re in the home, they’re surrounded by their family, they’ve got the nurses coming and going and that can be end of life situation, but they’re happy with that, but again, that’s not for everyone and it’s not for anyone to decide what’s right for your sister, what’s right for you as a family. That is something you as a family need to decide, and that’s a tough one.
Joyce: I think we’re coming to the end. My conclusion, Patrik is tomorrow I have a meeting at 11:00. What advocacy can I… You will be emailing me those two medications. I will be advocating for the ECMO machine. What else can I do to advocate. I’m still holding onto hope. I’m not going into this somber, I’m still in the battle. What else can I do? What else can I advocate for and how I can get her out of this for tomorrow 11:00 meeting?
Patrik: Look, the quickest way to improve her situation might be ECMO. I would need to know more about what they’re exactly doing, but that might be the quickest way. Another quicker way to progress with this would be a tracheostomy, no doubt about it, but then again then you open up another world, that gives her options. Definitely gives her options.
Suggested links:
Joyce: But that tracheostomy. You’re going to send me that medication because you’re saying if she’s on those two medications, they can’t move her to LTAC, right?
Patrik: No, they wouldn’t be able to manage that in LTAC. LTAC is for someone that is stable, on a ventilator with a tracheostomy. Your sister is not stable by what you’re sharing with me.
Patrik: So moving into LTAC she would have to be stable. Even if you were to agree to go to LTAC you’ve got to look at how likely is it for her to needing ICU again?
Recommended:
Joyce: Right, and then from statistics wise, people with COVID and with a tracheostomy, how long in a good scenario can they get weaned off? Two weeks, a month, six months?
Patrik: Oh, yep. Look.
Joyce: I just want to know if we make the tracheostomy decision how long are we in it for because I’m thinking, oh, another two weeks, but is two weeks really a reality?
Patrik: That is difficult to say because again, my experience is if people… and this is why I said earlier and yesterday as well, when people are in ICU it’s easier for them to be weaned off from my experience, because you’ve got more skills and higher level of expertise. As soon as they go to LTAC, that level of expertise will go out of the window.
Patrik: So that’s why I strongly feel like if your sister has a tracheostomy, she needs to stay in ICU for as long as possible, to maximize chances to get off the ventilator. Now, they would probably tell you that if she goes to LTAC, she will get physical therapy and she will get this, that and the other, which they won’t do in ICU. However, my argument is, yes, she will get that in LTAC, but the doctors and nurses are at different skill level and at a much lower skill level.
Joyce: Right. So can I say, “Look, I’ll do a tracheostomy, but only if you keep her in the ICU.” Do I have a bargaining chip on the table for that aspect or no?
Patrik: I think you should ask and see what they say. They would probably say, “Oh, we need to send her to LTAC because of insurances,” and this that and the other, but then again, as long as you haven’t given consent nothing is going to happen.
Joyce: Let’s just say if I do the tracheostomy, I have to give consent to go to LTAC?
Patrik: That rarely happens from my experience, rarely happens. It’s one step at the time. It would be new to me that when you give consent to a tracheostomy, you also have to give consent to go LTAC, that would be new to me.
Joyce: Right, but if I don’t consent to LTAC they would keep her there.
Patrik: They have to.
Joyce: Okay, I didn’t realize, I didn’t know that.
Patrik: Where else?
Joyce: Right. They cannot just move her without my consent?
Patrik: No.
Joyce: Unless the insurance knocks on my door and say, “Hey, get out of here,” but if they’re not contacting me or knocking my door I can’t let the hospital bully me around and tell me where to go.
Recommended:
Patrik: No, do not let the hospital bully you by any means. They’re very good. I can’t stress that enough. The hospitals are very good to pretend they’re operating in the vacuum. They will just say, “Oh, we’ll do whatever we want to do.” No, it’s not a simple task. If you don’t give consent to a tracheostomy, the tracheostomy won’t happen. If you don’t give consent to go into LTAC, and also with LTAC you can buy time just by saying, “Hey, I want to have a look at those places. I want to have a look where my sister is going. I want to talk to people.” You could buy time there just by doing your research, but bear in mind ICUs are under pressure outside of COVID because of lack of ICU beds, that has just exploded. So they are under real pressure to empty their beds.
Jane: Let me ask you another question just because you know so much about everything. Would you get the vaccination? You know I have to ask you.
Patrik: I have to laugh because nobody I would say no, I trust my immune system. However, I’m running a business here where I have direct patient contact, with a highly vulnerable patient group and I probably would because I can’t risk my clients or my staff. If I was whatever, if I would be working in a supermarket or whatever I probably wouldn’t care, but I guess the industry that I’m in and that I have direct patient contact and staff contact, yes, to protect my business and staff and clients. Other than that, I’m against, I wouldn’t get vaccinated otherwise.
Jane: Got it. Okay.
Joyce: Okay, Patrik, so here’s what I’m going to do. You’re going to send me the medication names. I’m going to stay on top of that, I’m going to ask for an ECMO, I’m going to fight tooth and nails and see. You and I, depending on how my meeting goes, I’ll email you for probably another session to go, if needed, maybe you can make my Thursday meeting with the doctors. I’m going to kind of loop you in and then if need be, I’ll have you probably Zoom in so you can advocate for us tooth and nail, so they see that we cannot be pushed around whatsoever.
Patrik: Yes.
Joyce: Once they see you, they know we’re not an average schmo off the street and we will not go down without every rock turned. So I appreciate your time. I think… does anyone else have a question for Patrik?
Recommended links:
Jane: No.
Joyce: Okay, Patrik. So you’ll email me those medications.
Patrik: Yes.
Jojo: Thank you. That was very informative.
Patrik: Pleasure. I want to help wherever I can help. It’s a difficult situation. There’s probably no right or wrong answers. There’s only the right answer for you as a family.
Joyce: Yeah. Well, thank you so much for the thing and I will contact you tomorrow. Send me that information.
Patrik: I’ll send you that information.
Joyce: I’m on the ground running and we’ll figure this out till the end. So I will contact you again and probably take another session with you as well, so we can stay on top of everything.
Patrik: Okay, I’ll email you that information now. Thank you.
RECOMMENDED:
Joyce: Thank you, Patrik.
Jane: Thank you.
Jojo: Thank you.
Patrik: Okay, all the best. Thank you. Bye.
Jojo: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!