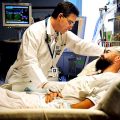
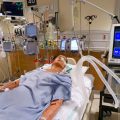
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’s sister is still with a tracheostomy on a ventilator and Joyce is asking what will be her sister’s quality of life after weaning off the ventilator.
What Will Be My Sister’s Quality of Life after Weaning off the Ventilator?
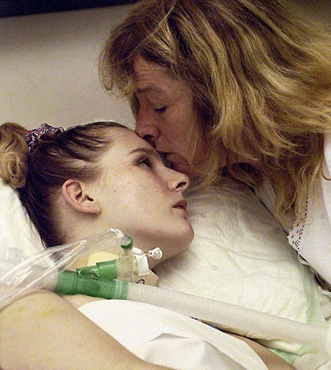
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Patrik: Of course. What about issues like is she absorbing feeds, is she opening bowels? There’s no issue in the digest.
Joyce: Good question that you said that she has a rectum tube in even though I’m trying to get the rectum tube out, because I’m so pissed that it’s there. And it’s been there for a long time and I don’t know if they’re doing that because they don’t want to clean her, I’m trying to obviously stay on top of it. But they said the reason the rectum tube was there for so long it’s because she’s developing bedsores. So they’re saying we don’t want it to get more infected. So she has a rectum tube. Now, she’s not even making that much stool because she’s on sugar water or whatever they’re giving her. And today, she said that because of the procedure yesterday, she’s letting a lot of gas out from the surgery and they have to change the bag. No poop is coming out. I was kind of like being advocate about taking this tube out, but I don’t know.
Patrik: Look, if someone has diarrhea and if someone has pressure sores and stools get into the pressure sore, you would want the rectal tube but the rectal tube needs to be managed properly. They need to change it regularly because if they-
Joyce: Okay, so I think if we keep asking, then they’ll keep changing it.
Patrik: Absolutely, and I’ll tell you why. If the rectal tube is not getting changed regularly, that could cause trauma in the bowels potentially cause a perforation. So really look as-
Joyce: I’m going to ask them. I watch her all day long. I watch if she’s getting turned. I watch if the RT is there, I’m watching it and I’m literally with somebody every half an hour seeing some movement. But again, I will ask for it to be changed.
RECOMMENDED:
Patrik: Definitely, the risk of a bowel perforation is there with the rectal tube.
Joyce: Okay, and so what else do you think? I mean-
Patrik: Yeah, so it’s okay, we’ve got the bowels out of the way. There’s no issues with digestion by the sounds of things.
Joyce: I mean, I don’t know, not really-
Patrik: Definitely a question you should ask. The risk of this getting into something bigger if they don’t do the wash out and the drainage is there. It sounds to me overall, since we last spoke, your sister has been improving, and would that be fair to say?
Joyce: I would say she’s more stable, yeah. Look, she got to a five, last time we were still eight we’re five. I guess the 33 is still kind of high in the carbon dioxide.
Patrik: No, carbon dioxide 38 is fine.
Recommended links:
Joyce: Okay, because I said to him, “What about the spreading?” He’s like, “No, you don’t want to do too soon because then she can have a whatever.” So I’m like, “Okay.” And I don’t know if the PEEP at 33-
Patrik: Yeah, the PEEP is high. The PEEP pressure is high. If the PEEP pressure high, it usually means there’s a lot of resistance in the lungs.
Joyce: The frequency have been going down too, what is it called? The suction, they suck it out?
Patrik: Okay, yeah, that has gone down?
Joyce: A little bit.
Patrik: The frequency?
Joyce: The frequency, yeah.
Patrik: Well, that’s good.
Joyce: Or the volume of it.
Patrik: Okay, that’s good. Well, with the ventilator settings, there’s two more things, is she breathing by herself or is the machine doing all the work?
Joyce: I think she’s breathing by herself because when I was speaking to the RT thing, she’s with the machine, breathing on the machine. Because every time she gets off sync that has that… So she is definitely breathing on her own. And when she would turn off the machine, obviously not for a long time, five seconds but she’s definitely with the machine. Because when she gets off sync it beeps. So she’s definitely breathing. I think she said she was stressed out, it was 33 and then it was going down to 29.
Recommended:
Patrik: Can you ask them what ventilator setting she’s in? Okay, so if she’s breathing by herself, she should either be in a CPAP mode.
Joyce: Sleep pap, wait-
Patrik: I’ll text it to you, CPAP mode or pressure support mode. It’s the same, but the terms are used interchangeably.
Joyce: Okay, you’ll text that to me.
Patrik: I’ll text that to you.
Joyce: And then does that make a difference for us, should we-
Patrik: Yes, absolutely. So if she’s breathing in CPAP or in pressure support, that’s the last step for someone to come off the ventilator. So if someone is breathing 24 hours CPAP or pressure support, the next step is to take them off the ventilator and see how they’re doing.
Joyce: I’m telling you today she was going to do a thing. But the RT lady was like, “No, don’t do it.” Because this morning, I think it was she grimace because of the gas. And I think she was stressed out at that particular moment so she said, “No.” Which just pisses me off and I really want to try. But she said, “Don’t try to fast because you don’t want her to like-”
Patrik: Yeah, tire out. I agree with all of that you got, it’s a process, it’s not an event, it’s got a step by step but she needs to come to the point where she can breathe in CPAP or pressure support for 24 hours then you can take them off the ventilator and see how it goes.
Recommended:
Joyce: I’m going to ask them today. Look that surgery is going to happen. And the surgeon’s like, “Well, after five days they’re good to go wherever.” No one’s spoken to me, I’m going to fight tooth and nails like I fought tooth and nails in ICU, you saw where that got me. Which by the way, this place was actually for the better, the step venue actually worked for me better. Remember I was fighting them tooth and nails.
Patrik: Yes.
Joyce: I’m in a step-down unit but it actually worked in my benefit because I feel like she’s getting a better care in a sense that. So I feel like in a sense that they have more time and they have more people and they’re not as stressful as ICU. ICU had other critical-
Patrik: Oh, yeah, full on.
Joyce: Somebody even combed her the other day, it was cute. We feel spiritually better and my mom got a compassionate visit. Even though my sister’s still stable, I was able to fight.
Patrik: Is your sister still COVID positive?
Joyce: No, negative.
Patrik: Fantastic. So it’s a bit strange to me that they’ve done the PEG, they’ve done the tracheostomy and they haven’t pushed her to LTAC. What stopped them so far?
Joyce: Because the PEG was infected and without having a working PEG, they cannot bring her anywhere. From what I understood through the doctor, because, trust me, they kind of wanted me to disconnect, we’re like, “No.” And he said, “Well, then I guess your sister’s going to have to be here because we have to have them until we fix the PEG.” She can’t leave anywhere without a PEG. She needs to be fed.
Recommended:
Joyce: And so we were like, “Okay, that’s good.” Because that bought us a lot of time. The other family, I’m telling you, they put the PEG in and he was out. The minute he put the PEG on out in no time. And so I’m thinking to myself, “Oh my God, nobody called us.” Something went off somewhere because we didn’t get any phone call after that surgery. Oh, actually, no, the reason we didn’t get that, I remember, we had the PEG and then we had the air pocket.
Joyce: We had the PEG done and everything was fine. We had the air pocket in the lungs. She needed to be sedated severely because they didn’t want it to get worse. And finally, the air pocket after a week went away on its own and then we took them off sedation and then whatever, whatever, whatever. But the reason we didn’t get that phone call is because the air in the pocket. There’s a lot of things that happen, I don’t know.
Patrik: How many days ago was the PEEP done?
Joyce: Oh my God, I would say maybe three weeks ago, four weeks ago.
Patrik: Okay, all right, okay.
Joyce: A long time ago, she’s been out, without a PEG, for at least two to three weeks because they had to take it out, it was infected. Then she had the thing with the nose to try to give her medication. Finally, they took that out because I guess no medication right now. So listen, I’ll do the surgery, I have no choice, I’ll do it. I will fight tooth and nails. Look, I’ll try and tell them, absolutely not, I want to stay there until she gets the PEG. I doubt it. Is there a dangerous zone of her being in this… Because they say the minute that thing comes out, it can close within an hour.
Patrik: Oh yeah, sure, that might be the case, probably does but probably does close quickly.
Joyce: But it’s still significant enough for her to be fed for at least very temporary awhile, correct?
Patrik: Oh, absolutely.
Joyce: The intestine one is called PEG, pig, what is called?
Patrik: PEJ, P-E-J.
Joyce: Okay, and that could be temporary for the next couple of weeks to months. Until it gets clogged up, they have to go back with the PEG.
Patrik: Yes, that’s why I asked. That is assuming everything goes well, she’s got no digestive issues, she’s opening bowels. That’s why this question is so important.
Joyce: Digestion issues, but I don’t think if they did, I think they would have brought it up to me.
Patrik: I would think so-
Joyce: How will you know she has a digestion issue?
Patrik: By asking, they’re basically-
Joyce: No, I know, but if she’s making stool, does that mean that it’s a digestion issue?
Patrik: Not really, no, not at all if she’s making stools that’s good. That means that she’s digesting.
Joyce: So then will answer that, I asked does she have a problem with the digestion?
Patrik: Yeah, and ask her if she’s absorbing and digesting her nutrition. And ask them if she’s got regular bowel movements.
Joyce: She does. I mean, she had bowel movements, not a lot, but she’s had it.
Patrik: Good.
Joyce: So we believe she did it?
Recommended:
Patrik: Keep asking that because the minute that, for whatever reason stops, there’s all sorts of risks with that. Starting from abdominal pain, increased pressure on the lungs because of a distended abdomen, aspirational risk.
Joyce: I think this now surgery might delay my getting off the ventilator, because now we have an incision and we have a major surgery. And would I be delayed with her going back to her… I just got them back. Patrik do you also think do I have her back or do you think that’s not enough? She is not fully fine compared.
Suggested links:
Patrik: What’s her Glasgow Coma scale?
Joyce: I didn’t ask for a while but she still hasn’t been following direction.
Patrik: Okay, so the last-
Joyce: But her eyes are open and she’s moving, do you think this.
Patrik: If someone asks her to squeeze hands or squeeze fingers-
Joyce: She couldn’t, she was really swollen and she had a lot of latex. So my mom said it was just like dead because she was there, it was just kind of flopping.
Patrik: It wasn’t.
Joyce: Hold on, it’s not connecting, but I’m trying to see if I can show you video maybe, hold on, let me see if that would help, I don’t know if that would help because I need you to clarify with me because I don’t know if this… Look, Where are you? Can you say that?
Patrik: Oh, well-
Joyce: Hold on.
Patrik: Is that a live video?
Joyce: It’s not a live video.
Patrik: It’s a recording. How long ago was that?
Joyce: This was on Tuesday.
Patrik: So three, four days ago, okay. Yeah, it’s hard to tell, but I mean, she looks way more awake than last time that’s for sure.
Joyce: 100%, but she’s not following commands. So can we still have hope that I know we were saying 14 days, it’s a lost cause, we were also saying day 60 is a lost cause and we’re kind of starting to get to these like, “She’s day 51 in the ventilator, she’s way past 14 days with sedation, but she’s showing something.” Nothing to the bank but can you give me a picture of where I’m heading? I know you’re not God but-
Patrik: No, okay, let me ask you this. Is your sister getting mobilized?
Joyce: They’re telling me physical therapy will not come up if she’s not participating. I’ve asked four or five times, they said, “If she’s not participating, they won’t.” I said “No, that doesn’t make sense. I want her legs to move.” And they’re moving them every two hours. But that’s not significant of moving.
Patrik: So are you suggesting she hasn’t been in a chair since she’s been there?
Joyce: Correct.
Patrik: Oh, my goodness.
Joyce: How did they put her in a chair? She’s like flopping over.
Patrik: Well, that’s not an excuse in my mind. You can always support people with pillows. Imagine you’re lying-in bed? Did you say 55 days? Of course, the cognition isn’t getting better. There’s no stimulation. You don’t have to be sitting up 90 degrees in a chair, even like a cardiac recliner, just start somewhere.
Joyce: And they could even just move her legs. All right, listen, I’m not going to take no for an answer, I’m going to tell them, “You need to do some kind of physical therapy.”
Patrik: Absolutely, this is one of the missing links there. They’re just too complacent, she is a lost cause in their mind and they’re just not trying.
Recommended:
Joyce: You think that’s how they’re thinking?
Patrik: I think so.
Joyce: I mean, that’s what the doctor basically told us, but I feel we’re going all the way, we’ve gone well. Even the palliative guy came on camera and said, “Oh, your sister’s doing better, I could have shot him, I can literally shoot him.
Patrik: I remember you talking about the palliative care.
Joyce: We’re gone with him. But he literally came on, grabbed me and said, “Oh, she’s doing better. I could have killed him.”
Patrik: Look, unfortunately, your sister is a number there, unfortunately. And what I’m seeing at the moment, the whole COVID is not helping. Hospitals are completely overwhelmed, it doesn’t help. But compared to when we spoke last time, I guess, besides the issue with a PEG tube, it sounds they have been-
RECOMMENDED:
Joyce: The vent is better. I’m telling you. We were saying, “Oh my God, she would never.” Even the guy said she would never, but now it seem we’re getting close to just spontaneous breathing trial. So that gives me an indication maybe she could get off, maybe.
Patrik: Oh, look, spontaneous breathing, trial is great.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!