Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
I Want My Husband To Have The Tracheostomy Now But Why Is The ICU Team Reluctant To Do It?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Isabel as part of my 1:1 consulting and advocacy service! Isabel is worried that her husband who just got off the ECMO is developing another infection based on his new blood test results and she is asking what to do and what could have caused it.
My Husband Has Been Off ECMO But Still Has Central Line And Needs Dialysis. Could It Be The Cause Of His Newly Developing Infection? Help!
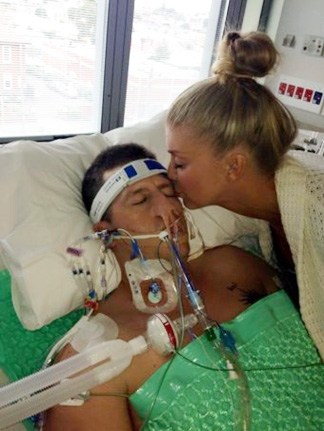
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isabel here.”
Isabel: Yeah, yeah. Yeah. So thank you, Helga, for just being there for me and helping me through it. Because you know, it’s hard. It’s hard. I have cried, like I want to say 25 days straight. And honestly like my tears are just, I’m just numb now. I have no feeling in me no more. But I couldn’t do it without your help, Helga, and Aurora, and everybody. Eli too. And your brother Jonah.
Helga: And when those keep happening too, like when the calls, remember call Patrik, if he’s not able to call me, call whoever. I don’t want you to do those alone, please. I want you to have somebody there to help you, because it is a lot. Even the time that I’ve been helping you, I’ve felt it. And I’m not even in it the way you are. And it’s been a lot. So, just know we’re all here. And we have Patrik, who we trust to tell us the truth, and then we can just make our decisions together, okay? You’re not alone.
Isabel: Okay.
Helga: Okay. Was there anything else you wanted to ask, Isabel? Because I would think I’m ready to talk to you separately.
Isabel: Okay.
Helga: I just want to be respectful. I don’t know. I know that we’re not the only people Patrik helps, so I feel sensitive to making sure he’s available for other families.
Patrik: We can leave it here.
Helga: Okay. Sounds good. I’ll talk to you, Isabel.
Patrik: Thank you. Take care.
Isabel: Thank you. Bye-bye.
Patrik: See you, bye.
RECOMMENDED:
Patrik: Hello Helga. How are you?
Helga: I’m good Patrik. How are you?
Patrik: Okay. All right. So, your brother, he has been decannulated, has been taken off ECMO?
Helga: Yes. Right Isabel? We actually have a debrief, yesterday from the doctor, that we had already wanted to talk to you about and then we had an update today that we wanted to talk to you about. Right, Isabel?
Isabel: Yes.
Patrik: So, when you say update, did you have another Zoom meeting with the doctors?
Helga: No, just the phone call updates, where they call Isabel daily. And I’ve asked to help Isabel with, because it’s a lot to sort. I’ve asked her to call me and have me join in on the calls. And that just started as of yesterday, or Sunday night actually was our first time doing that with the night nurse. And because they weren’t as positive or they weren’t as encouraging or supportive, of getting pictures in the room, telling Isabel that, “His eyes were closed, so what’s the point?”, kind of thing. And so I was kind of not happy with that. So, I spoke with them, and started explaining our reasoning for wanting to speak to him daily, anyway, we started doing those group calls.
Patrik: Okay, good.
Helga: On that night, we were told it wasn’t that great, he was on continuous dialysis. He had blood in his urine, a host of things, it was just a rough day. And then the next morning, was when overnight, he had had some type of progress where he passed the test and was decannulated and removed from ECMO, which we didn’t know why he was removed from ECMO. Isabel just got a call saying, “He’s been removed from ECMO.” So, we were all kind of freaking out, because we didn’t know if this was removing him from support, or what had happened and that’s when I messaged you, and we got an update that the doctor removed him because he no longer needed it.
Patrik: Okay. And so that was yesterday Monday morning or afternoon?
Helga: Yesterday Sunday for us so that was morning.
Patrik: Oh yeah, Sunday for you, yeah of course.
Helga: Sunday Morning. Today is Monday for us.
Patrik: Yeah, yeah, yeah.
Helga: So, yesterday we had a.
Helga: Go ahead.
Patrik: Yeah, no, no. I’m just trying to clarify timelines. So, are they saying he must have improved then.
Helga: Yeah. So, Tuesday when we got a phone call, Isabel called back asking, “Why did you remove him?” So, then doctor, she called us back, and explained to us that he was removed because he no longer needed it. His lungs had healed enough to be off of it. And we were kind of excited, and they had quickly kind of shot that down saying, “Hold on, we still are concerned about his brain.” His GCS was around four, the highest is five, because he was still in the comatose. She was actually there when he went into cardiac arrest And so, she says it was 20 minutes. She had said that they still wanted to do an MRI, but he wasn’t stable enough to get one done. So, she didn’t want to chance that, because he had had such a big day coming off of ECMO, that his viral pneumonia still looked like it was there, but “It could take six weeks for that to show up on the X-rays,” it’s what she said.
Helga: They were still going to do another EEG, but as of right now the last EEG and their clinical bedside exam was still consistent with him not being responsive.
Patrik: So, that would confirm the GCS four to five. I don’t know, have I emailed you that?
Helga: Yes, you did.
Patrik: Right.
RECOMMENDED:
Helga: So, that was what they had said. She had said that he was still on continuous dialysis and the goal was to get him off of it today, and then today we got a call saying that, “He was not going to be taken off of continuous dialysis, he was still okay there.” This was completely brand new news for us, but that his blood pressure. Yesterday his blood pressure we were told, “was concerning”, to the doctor, because he was on two medications, for blood pressure. Today, we’re told he’s gone from 30 micrograms to 10 micrograms of the medication, and his blood pressure is a 120 over 60.
Patrik: Yep. So, can you just repeat…
Helga: Yeah so that’s really great.
Patrik: … can you just repeat that he went from 30 micrograms to 10 micrograms.
Helga: Correct.
Helga: Per minute, is that right?
Patrik: Which one?
Helga: Per minute.
Patrik: Per minute, yeah, yeah. Do you know the drug name, is it Epinephrine, is it Norepinephrine?
Helga: I wrote it down, my phone. It definitely has a “pinephrine” at the end. Let me see what I wrote down.
Patrik: Pinephrine all right. Or could be Phenylephrine, could be either.
Helga: Isabel did you get the name of it? I wrote it on my phone.
Isabel: No, no, I didn’t.
Helga: So, today was, where’s that? Micronephriprine, does that sound right?
Patrik: Micronephriprine, no it doesn’t, but that’s okay, that’s okay.
Helga: No. Okay. Maybe I can hear it right.
Patrik: Probably, no, probably something like norepinephrine wasn’t vasopressin.
Helga: No, it had a nephriprine on the end.
Patrik: Yeah, that’s okay, that’s okay.
Helga: The other update was that, his ventilator settings were now at 55%, with high 90s for the oxygen levels.
Patrik: Yep. Okay.
Helga: Which was completely different, because on ECMO he was at 100%, with 55% oxygen levels. He, he had now been on 24 hours on the ventilator at 55%. So, he had around 5:00 a.m. this morning was when he had decreased to 55%, because yesterday was still higher, because of coming off of ECMO. She said that was normal. His blood gas exchange is good, it’s above normal, and it was showing that he had a solid stable amount of oxygen. So, that’s why she felt that it was okay to go ahead and get him to MRI.
Patrik: Oh, and they’ve done the MRI or just planning?
Helga: They were setting him up for it, and so, as of right now, we’re assuming it’s done. We don’t know. They were prepping him for it earlier, she assured us that his respiratory therapist and his nurse would be with him.
Patrik: Okay. So, they would not do an MRI if he couldn’t cope off the ECMO, that’s for sure? So, that’s very positive. I like everything that I’m hearing. The only change from my notes is on the weekend I asked that “Is he on any vasopressors” which is the Epinephrine or the Norepinephrine. He wasn’t on the weekend, so they must have used that in the meantime. That could be just as simple as needing dialysis, because dialysis will get the blood pressure down.
Patrik: Okay, the reason I’m explaining this to you is, when someone is on the vasopressors like the Epinephrine or the Norepinephrine, that’s considered life support. Okay. So, without the Epinephrine or Norepinephrine his blood pressure would plummet quite low, and would not be sustainable with life. But he would have lost blood by getting him off the ECMO, because there would have been blood left in the circuit that they couldn’t return. So, he would have lost 150 mils of blood, which is a lot. He would lose blood by being on dialysis, because again, there’s blood going through an extra circuit. So that brings the blood pressure down.
Patrik: So, those issues around dialysis and around ECMO usually gets people on those vasopressors, but given that he went from 30 to 10, that’s good news. That’s really good news. Do you know if you had a blood transfusion?
Isabel: No, she didn’t tell us he had a blood transfusion. They usually do.
Patrik: Yes. It’s best to ask if he had.
Patrik: You did or you didn’t ask?
Helga: We did not ask. The last time he had a blood transfusion was during the ECMO.
Patrik: Yeah. Just ask. Because that could be one of the reasons why his requirements have gone from 30 to 10, could be one of the reasons. Again, the good news, I mean, there’s overall good news. The only news that is consistent with, from the weekend, is he’s not waking up. Which is why they want to do the MRI. But if he was too unstable off the ECMO, they wouldn’t do the MRI. If he’s now on 55% of oxygen, and his oxygen levels are in the high 90s, that’s fantastic news. That is great news.
Helga: Yeah, we thought so too. We were pretty excited, because of just the last conversation from Tuesday to Saturday, the Tuesday call that you did with us to the Friday call, getting told he’s going to be removed and may not survive the weekend, to now being he’s off of it overnight, and then now today. Isabel was concerned that they were rushing the MRI, and so she had asked them, because yesterday he wasn’t stable enough to do it, but then today he was, so she had asked some good questions like, “Well, how long does he need to be stable for, what are the numbers that justify taking him to do that?” And so that’s when she gave us the blood pressure numbers, and said that she wouldn’t do it if he wasn’t stable enough to make it through.
Patrik: Definitely. So, are there any news, so from Saturday to today have they changed any of the treatment? Because I do remember from my notes on the weekend, they gave him the Remdesivir and they gave him the Dexamethasone, that was all they did from what I understand. You know whether they’ve changed the approach of the treatment?
Isabel: No, they haven’t changed their approach because the Remdesivir was given to him the first week he was admitted to the hospital, which today we’re at day 30. So, after the Remdesivir, they couldn’t give it to him when he went on ECMO because of the kidneys. So, then they gave him the Dexamethasone.
Patrik: Yes Dexamethasone, yeah.
Isabel: Yes they gave him that, probably few days after the Remdesivir. He got eight days of that. And then he got 10 days of the steroid.
Patrik: Okay, that’s good information. Because basically what that means is, the last doctor we spoke to on the weekend on Sunday, I mean, he was more Way more positive than the doctors we had the day before. And all he said at the time is, “Well, we want to give him more time, there’s no guarantee but maybe just time.” Just giving him time. So, and what are they outlining as the next steps?
Isabel: Well, they’re getting the results of the MRI.
Patrik: Yeah.
Isabel: And pretty much it, from their medical standpoint is that they want to line up their clinical exam with the EEGs, and the CT scans, and the MRIs, and then come to their conclusion of what’s happening and why he’s not waking up.
Patrik: Okay. They’re not highlighting any other issues, terms of blood results and infections, they’re not highlighting any other issues at the moment.
Isabel: No, no.
RECOMMENDED:
Patrik: When I look at my notes, I do remember he was talking about, so they’ve taken out the ECMO, which is good, because that’s one source of infection that they eliminated, but he was also talking about other lines such as central line, arterial line, they need to be changed every seven days, and I can put that in a quick email when we come off the call, just to for you to ask, “Are they having any other concerns about any other sources of infection?”
Patrik: So, he’s got a line either in his neck, or in his groin, where they give infusions, but those lines need to be changed regularly, because again, they could get infected. And he was talking about this specifically.
Helga: She did mention that they had done cultures yesterday, because of his white blood count had went up, I think she said the number 27, and she said something about the lines. She wanted to make sure that they had put them on an antifungal, just in case. Because ECMO could have been a source of infection, it’s what she said.
Patrik: Definitely, Did you say white cell count? 20.
Helga: She said 27, I don’t know what that means.
Patrik: Yeah. So, no, no, that’s good information. So, white cell count is a marker in the blood for infection. Okay. So, white, normal blood cell count is four to 11, and so 27 is elevated, which means there is something brewing. Right. So, I believe you need to ask where is it coming from, or do they know where it’s coming from. If there is a source of infection, they usually need to do a blood sample, to find out, is there a bacteria growing in the blood. They should do a sputum sample, which I’m sure they would have done. And they should do a urine sample to again find out is there an infection in the urine, is there an infection in the blood, is there an infection in the sputum. Those are the most common sources.
Patrik: And then once they’ve found where the infection is, then treat it accordingly. If it’s a bacterial infection, treat it with antibiotics. If it’s a fungal infection, treat it with anti-fungal. If it’s a virus, which is what COVID is, there’s limited treatment.
Isabel: She did say, what did she say about…
Helga: You were saying, he was saying that reminded me of something she said today, about the blood count and, I need look at the notes. She said that Oh, that they did find some clotting in the dialysis machine and that they’re finding with COVID because of having to figure out the blood thinner, or something about that prevents it, but that they were going to be replacing the bags because they couldn’t be reused.
Patrik: Okay. So, did they talk about whether he’s on heparin? Do you know what I mean by heparin?
Isabel: Yes. He was on heparin. I’m not sure if he still is, but I know they put him on heparin because of the ECMO, and to prevent clotting. So, I’m not sure if he still on that, after taking him off the ECMO.
Patrik: He wouldn’t be on heparin just for the ECMO, but he might be on heparin now for the dialysis, which would be a much lower dose. But still, I guess again, probably best to ask because giving heparin helps with the clotting in the filter, but it’s also, heparin comes with side effects. There are other risks associated with giving heparin so yeah. The more you understand about what they’re doing, the better it is. The more you understand about the risks, I believe the better it is. Just so that you’re aware of some of the things that could happen as well.
Isabel: I know they had mentioned heparin causing bleeding.
Patrik: Very much so.
Isabel: … and so that’s why he was getting transfused because of the heparin.,
Patrik: That’s probably one of the reasons, but also when someone is on ECMO and dialysis, the risk of a blood clot is so high that they need to give heparin to manage the risk of a blood clot. On the other hand, the risk of giving heparin is that you might end up with a bleed. Right. So, yeah, just to be aware of the risks.
Patrik: Now, so they’re doing an MRI, he’s not waking up yet, so now the focus can almost be shifted on the brain, at least for now, I mean, the goal is still to get him off the ventilator. That is still the goal, have they talked about this at all?
Isabel: She did say that it was going to take him a while, for him to get off the ventilator. Isn’t that what you understood Helga?
Helga: You know what, I didn’t catch that part, but I did hear her say that she was keeping it at the 55% just because of so much happening. She wanted to give him the support, even though he may not have needed that much today. So, I didn’t hear anything about weaning him, the plan, I don’t know that part.
Patrik: Okay.
Isabel: I believe she said it was going to take a while.
Helga: Okay.
Patrik: It would be very hard for them to put timelines on it. It would be very difficult for them. I do believe the next step really is to look at a tracheostomy. Do you remember that we spoke about this on the weekend?
RECOMMENDED:
Helga: I remember you saying that, “that’s usually how you start weaning”, but because he was on ECMO, it was kind of too late for that.
Patrik: Now, now, yes. I don’t think I would have mentioned that it’s too late, it’s really never too late for a tracheostomy, but the risk of him having a tracheostomy while he was on a lot of heparin.
RECOMMENDED:
Helga: Yes, that’s what I meant with the ECMO, he didn’t need it because he was on ECMO at the time.
Patrik: Yeah. Look, generally speaking, if someone goes above two weeks of ventilation, patients should have a tracheostomy, generally speaking. Right. Now that he’s more or less taking the next step in his recovery, I do believe they need to look at a tracheostomy. Sorry, what’s your brother’s first name again, Noel?
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!