Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
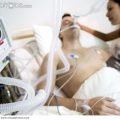
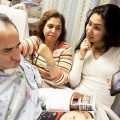
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Isabel as part of my 1:1 consulting and advocacy service! Isabel is determined to request for a tracheostomy for her husband in ICU and she is asking if it will help the ICU team manage her husband better with the discomfort caused by the breathing tube and move better with physical therapy.
I Want a Tracheostomy for my Husband. Will that Help Ease the Discomfort of Breathing Tube and So He Can Move Better for his Physical Therapy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isabel here.”
Eli: Yeah. That’s my opinion and Noel doesn’t want to hear that, but.
Isabel: I’m trying to listen to you guys and I’m trying to listen to my kids too. And it’s hard for me. I’m listening to your mom, your sister, you, and my kids have a totally different opinion than you do.
Eli: What are they saying? Let him go?
Isabel: They’re saying that he wouldn’t want to live like this. My two older kids. David is too little.
Eli: And they know him the best just as you do.
Helga: And I agree with that. I get what you guys are saying. If we are truly supposed to say we’re going to live by and sorry, Patrik, we’re getting into other and if this is the end of conversation, I’ve got to talk to my family about this, that’s fine. I just feel like when we’re going to live a certain way, then we’re not supposed to pick and choose what that is. And we’re always supposed to consult like, “Well, what does the word say? What does God say? What does he say about this?” And even though they’re saying that there’s good logic there, but then I would also say, “Okay, look as a family. What does the word say about these kinds of things and where are we putting ourselves in those decisions? Or are we letting and trusting God?” I liked the idea of trusting that and then, okay, let’s have a conversation if in the future, it’s not happening. I understand that, but I still feel like I would want to pray and have peace from God about those decisions. And I can’t see anywhere in the Bible it’s supporting that. Of what your kids are saying. So I’m just saying as a parent.
Isabel: Hold on.
Eli: Yeah.
Isabel: Go ahead.
Aurora: I just heard as a parent.
Isabel: As a parent, I just feel like Noel is not there to lead them and they have you, and they’re looking to you, and they’re giving you their input and that’s good that they are inputting that. And I know what he wouldn’t want. And I’m not trying to be selfish. I’m trying to say. In my own understanding, but you know, look to the Lord and he will direct our paths. And so I’m trying to think of that and say, “Okay, well, what does it say here?” Because I may want something and I may think something, but what is this going to say? And that’s what I can have peace about. Trusting is what I’m trying to get at.
Eli: You know what I would say as a dad or as a leader where I’m at and my kids, is I would agree with them. You’re right. Your dad wouldn’t want to live like this, but, not even a but, it would be an extension to that and say that God is in control. And that he decides, not us, not Noel. And in this case we are doing what is, I don’t even know how to say it. What’s in the best interest or what’s for the greater good.
Helga: It’s just trusting God. I don’t even think the greater good is the right thing. I think it’s more about just saying, “You know what? We don’t know the answer. We’re going to pray and ask God to guide us. And we’re going to trust that this is in his hands.”
Eli: There you go. There you go.
RECOMMENDED:
Helga: And if he’s going to take home Noel, that he’s going to take him home and we’re not going to have to make that decision. And just like he wouldn’t want to live. I feel like it’s hard to say that because just like I wouldn’t agree with suicide. And so if somebody is living and they don’t want to live anymore and they make that decision just because they were in pain or whatever was so awful in their life, they’re entitled to make that decision, but was that the right thing? And so that’s kind of why I understand why they’re saying that, “Oh, he wouldn’t want to live this way, but then we’re still trying to play God in that sense.” And so I understand and will support if he passes that we leave him be and let him be in peace that way. But as of right now, I just think it’s too early. I cannot support any type of letting him go on purpose.
Aurora: That’s my argument.
Helga: Hey Aurora, you can just got on. We’ll have to debrief you because we talked about a lot of stuff. We’ve been on for a while.
Aurora: That’s fine. I know, but I came in and I heard Eli and I hear you and I hear Patrik and I say the same thing. I understand he would not want to live that way. But the thing is that we say things out of fear, out of this, out of that, but then, who’s to say that he would not want to live just with whatever, however. I believe also in my heart that it’s God is the one to decide. The other way is that you’re deciding for him and not letting God decide. I don’t know. I’ve just reconnected with my faith and everything. And I believe that we should let God decide. And I don’t think I’m being selfish wanting to have my son around longer, however it may be. It’s till death do us part. For me to make the decision to let him go.
Isabel: That’s why it’s so hard on me because, I just have to pray. Like you said, I just have to pray. I just don’t want him suffering. That’s all. I don’t want him suffering.
RECOMMENDED:
Aurora: Isabel, didn’t they tell you already that because he is the way he is, he can’t even feel anything right now?
Isabel: No, that’s not what she said. She said that she potentially believes that he is suffering.
Aurora: Oh, okay.
Helga: No, that’s not correct. The nurse had said that he.
Aurora: You see? That’s what’s scary. One tells you one thing, another one tells you another thing. And so you’re bouncing back and forth. Do we believe one or do we believe the other? What’s the truth? Only God knows.
Isabel: I know. The nurse said that. And the doctor was telling Eiren that there’s really no definite way to know, but it does react to when the ECMO came off, he did react in a discomforted way. It’s not consistent.
Aurora: Okay, then that’s a sign.
Isabel: With the pain stimuli that they do daily. She said it wasn’t consistent with that kind of reaction, but there was some sort of reaction.
Aurora: Well, that alone tells you, come on now. That alone tells you that he’s with us.
Isabel: But it also tells me that he’s in pain and they’re not giving them any medicine for it.
Helga: I understand. I was worried about the pain the night before we got the MRI readings, the night before we had talked to the nurse, I don’t even think he was off ECMO yet. It was actually the night before he got off of ECMO, we had a really grim report from the night nurse. She told us all the updates of how he wasn’t doing well. And she thought that he was suffering. And he wasn’t on any pain medicine. The next day comes off ECMO and we talked to the doctors and they actually say because of his state, because he’s most likely, he’s unresponsive. He doesn’t feel anything. And so they don’t know for sure, but with the brain damage he’s had, they most likely cannot feel it. He’s only responding because of the brain stem that’s not damaged and the reflexes.
Isabel: But Patrik, do you recall the other doctors saying on two occasions that he was in pain?
Patrik: Absolutely. And I feel like it varies slightly, the information they’re giving varies slightly. It probably also depends on the day. Probably depends what’s going on. Another important distinguishing factor, I believe was mentioned not this morning, but it was definitely mentioned earlier this week. He’s not brain dead. Right? He’s got reflexes, he’s breathing. If somebody was brain dead, they would remove him from the ventilator and he would die immediately. So that is definitely not the case. Anybody that’s got eyes open and has a spontaneous breathing effort, breathing, is not brain dead. Right? So I’m just putting this out there. And some people, depending on their faith, depending on their beliefs, they might even argue, if someone’s brain dead, they might even say, “Well, I don’t agree with it. I want them to live irrespective.” So it’s all in the eye of the beholder. There is no right or wrong. It’s really comes down to preferences.
Aurora: I just feel that anyone that’s making a decision to take them off and just let them like that. To me, it’s just like killing him. That’s my opinion. You’d be killing him without letting God do what his will is.
Helga: Patrik, is there a way to go forward with what we’re talking about? Like getting the MRI’s. Well, the thing is, when the nurse had told us that she thought he was in pain, it really scared Isabel and I. This was before he got off ECMO, we had asked, “Well, can he be put on some type of medication?” She said that because they didn’t know the MRI yet, the neurological part was superseded, like whatever pain he was in, because they needed to make sure where he was at. Now that we know where he’s at with the brain damage, would it be conflicting to give him something? Because then he wouldn’t be able to respond or be better? To mitigate like kind of both at once?
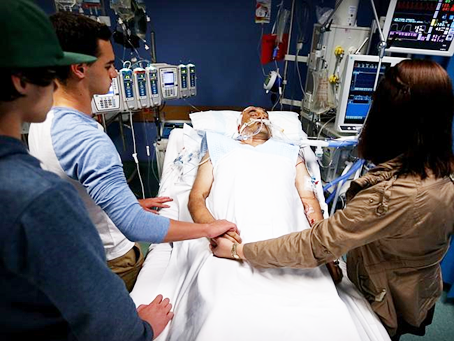
Patrik: Great question. So when I saw him earlier on the video call, one thing that’s struck me is breathing looked very labored. He was sort of breathing heavily. He was breathing fast. It didn’t look comfortable to me. Now, there could be a number of reasons for that. It could be pain. I believe it’s mainly the breathing tube. And he’s a little bit more awake. The breathing tube in the throat would be very uncomfortable. But if it’s not the breathing tube, he could have some pain from something. We don’t know. If it’s uncomfortable for him, there’s two ways forward. Yes, you could give him pain relief. Or if the breathing tube is causing the discomfort, it probably would be as simple as doing a tracheostomy. A tracheostomy is painless. I have not heard anybody complain about pain from a tracheostomy. I believe the labored breathing would subside as soon as he started tracheostomy.
Aurora: I agree because of what experience I went through with my brother. I’m not saying that it’s exactly the same or anything, but there is a lot of difference.
Helga: So you’re saying the way to help him right now from suffering is to get that thing out of his throat and keep him on support, but in a more comfortable way by having a tracheostomy? And we would already relieve a lot of discomfort he’s in right now?
Patrik: Very much so. If you look at the literature, I think I mentioned briefly, usually a tracheostomy is done after two weeks of mechanical ventilation with the breathing tube. Now at the moment, those guidelines are going out of the window because of COVID, but they’re going out of the window everywhere, because you’re opening up another airway. COVID sits in the lung, so there’s a huge risk of COVID spreading. At the same time, they are developing techniques now to perform a trach in a safe environment, even on COVID patients. So they have brought it up as part of the discussion this afternoon. So I think it’s definitely doable. And yes, you could give him pain medication in the meantime, but that might also sort of delay waking up. Right?
Eli: Let’s request a tracheostomy.
Helga: I’m all for that. Yeah.
RECOMMENDED:
Isabel: So giving him pain medicine will delay him from waking up if he’s.
Patrik: Well, let’s just say part of not waking up is. When patients are critically ill, there’s often a delay in them waking up even without a brain injury. Now, he’s at the point, now he’s been off sedation since the 12th of August. Given that he hasn’t woken up, chances are that he’s got a significant brain injury, but today is the 24th. So that’s 12 days of sedation and minimal waking up. There are patients out there that are not waking up for 12 days and they don’t have a brain injury. I’ve seen that. Induced comas are very powerful and the side effects are very powerful. It looks like he’s got a brain injury, but what I am saying, there are patients that don’t wake up after 12 days of a prolonged induced coma and they don’t have a brain injury.
Isabel: So have you witnessed anybody waking up from a brain injury like his?
Patrik: Probably not so much in ICU because once Noel has a tracheostomy, he can potentially get off the ventilator. When people leave ICU, they’re often not at a point where they’re fully awake. When you interview patients, weeks, months later, “Do you remember when you got discharged from ICU?” They don’t remember a single thing often. Even though they are awake, they don’t remember much.
Eli: I think we should request the tracheostomy. Analytically, looking at everything, if this was on a whiteboard, I think that would be the right thing to do.
Helga: And especially because it’s going to relieve any discomfort with the ventilator right now, being down his throat. As we look at the MRI result report and as we get a second opinion, at least he will be in comfort, if he can feel that. And should be able to breathe better.
Aurora: I want to emphasize on the question about the medical records and reports. What would be the reason that they haven’t given us that yet?
Eli: COVID.
Aurora: And when Isabel, because our hands are tied, we have to rely on Isabel talking to the doctors and asking questions.
Isabel: You do not, Aurora.
Aurora: So, the thing is that, how can we get those records and how is it possible to have someone else read them? In other words, can we take those records to someone to read them? I don’t know.
Patrik: I would argue that’s almost a second opinion. Once you’ve got access to the medical records, you can go wherever you want with those medical records. You can go to a neurologist.
Aurora: Okay, that’s what I’m asking.
Helga: Isabel asked about a second opinion today. Yeah, that was something we talked from the beginning where she’s going to ask for a second opinion and we were trying to decide whether the neurology would be outside of the hospital or not, due to COVID.
Patrik: It’s probably just depends on the medical records. Let’s probably just stipulate on an administrative level. There shouldn’t be an issue of you accessing medical records. I would hope that it’s all online. They might even just send you a link to a website and you get a password and you log in and you have access to the medical records. I would hope it’s as simple as that. It’s all moving electronically now. I would hope it’s as simple as that. You get a link to a website, password, and there you go.
Isabel: Yeah, I’ve been waiting for that. I left several messages, emails.
Patrik: Keep pushing for it.
Isabel: I’m pushing, but you know, I can’t. My hands are tied.
Eli: I have a question for Patrik. I know we could probably push back as much as we want, but how much can we keep asking? And them playing or not answering or not giving us the request or the questions that we are looking for before. Are they waiting for us to give up?
Isabel: I’m almost done, yeah. I’m almost done. Give me a couple more minutes.
Eli: You know what I’m saying?
Patrik: Yeah. I know. Of course, of course. Look, I’m dealing with many ICU teams. And I have been part of ICU teams in the past, myself. My feeling at the moment is that they’re not overly aggressive, but that could change. That could change. But my feeling at the moment is that they’re quite amenable to you directing them. That’s my feeling at the moment. Again, that could change, but I believe that waiting for you to direct the next steps. I mean, we were talking this afternoon, Isabel. We were talking about a tracheostomy. There wasn’t any indication when we brought up the tracheostomy that they would flat out deny that. That wasn’t my impression. And again, when it comes to decisions about end of life, Eli, it’s not that they can just say, “Oh, well, we just pulled the plug and we withdraw treatment.” It’s not as simple as that. End of life decisions can’t be made in a vacuum. Isabel, you would have to give consent to that. You can’t just stop life support because you just feel like it.
Isabel: Yeah.
Eli: Yeah. But then there’s also, how do we prove that they did that? Or there’s also the concept of, well, we don’t understand how something works. So they make it seem like they didn’t do that, but they do it anyway.
Isabel: He’s basically saying like.
Eli: You know what I mean?
Isabel: Patient neglect. Okay, they know that his brain’s this way. They know he’s going into renal failure. They know that his lungs aren’t, so he’s basically saying, is this something that they would potentially neglect per se?
Eli: Yeah. Yes. There you go.
Patrik: Absolutely, Eli.
Isabel: And there’s no way to know.
Eli: There’s no way.
Patrik: Absolutely, Eli. Absolutely. I’ll tell you something that I believe I saw earlier when Noel was on the camera. Isabel, you might recall when we had the call with the doctor this afternoon, she was sort of saying they’re doing the physical therapy, they’re doing the arm movement and the leg movement and they’re sitting him up. Now, from what I saw in the video, he’s just lying there. He’s not even sitting up.
Isabel: Right.
Patrik: Right? So I kind of question of what she said that they’re doing X, Y and Z. I question. You’re spot on there, Eli. And they would be so busy at the moment especially with COVID. They would be so busy. Yes.
Eli: Understaffed.
Patrik: Definitely. There could be an element of neglect. Absolutely. Yes. And also what I referred to as a silent DNR. You refused the DNR, but then there is in sort of more health, professional terms as silent DNR. Yes. You may have it on paper, but everybody in the eyes of.
Eli: What are we going to be able to do about it? We’re not there.
RECOMMENDED:
Patrik: Absolutely.
Helga: Exactly.
Aurora: We’re not there. With this COVID we couldn’t even see him, we can’t even go be with him or anything, and that’s the worst part because they can tell us that they’re doing this and doing that, we don’t know.
Eli: Okay.
Isabel: She keeps bringing up the DNR, because, when I had a conversation with her and Dani, before I got on this call, she brought it up again. I kind of just shut her down and told her that.
RECOMMENDED:
Eli: Here’s the thing then, here’s my analytical thinking on that then, if that is the case and it’s 50/50 chance that that is happening, we have to act quickly on the requests that we think can put them in a better position, like the tracheostomy and the second opinion. So, as soon as we can get those in, time is of the essence I guess. We need to ask for that as soon as possible.
Helga: I agree, Eli, I agree. Getting the second opinion, getting the MRI report and then asking for the tracheostomy. Not necessarily in that order, but definitely, I feel like the tracheostomy is important because it’s going to help give them some comfort and even ability to move better. I would even say, whenever you’re calling in and talking to the night nurse to ask them, what physical therapy have you done during this round? What movement have you done?” And if depending on the answer, I would ask them, “Well, could you do it now?” If they haven’t already. Because Patrik has heard that that was physical therapy was part of brain stimuli.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feEling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!