Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joefbert as part of my 1:1 consulting and advocacy service! Joefbert’s father-in-law is critically in ICU and he is asking why does the ICU team reintubated him back after 24 hours of extubation.
My Father-in-Law is Critically Ill in ICU. Why Did the ICU Team Reintubate Him After 24 Hours of Extubation?
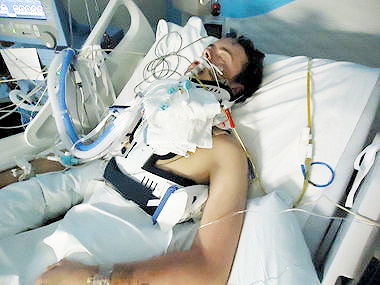
Patrik: You’ve got your mother-in-law in ICU. Is that correct?
Joefbert: Father-in-law
Patrik: He’s in ICU, has got a poor ejection fraction, edema. What’s your biggest challenge at the moment?
RECOMMENDED:
Joefbert: Biggest challenge is how to revive the lungs.
Patrik: Have they talked about ECMO?
Patrik: Is he on ECMO?
Patrik: Have you heard of ECMO as a treatment option?
Joefbert: No.
Patrik: Alright. I’ll send you a link. ECMO is a treatment option for lung failure. What other challenge? So he’s had, he was extubated?
Joefbert: Yeah! He was extubated then for 24 hours. But again, he could not sustain. So then again, he was put on ventilator. Now he’s on a hundred percent ventilator support.
Patrik: And how many days has it been?
Joefbert: 24 hours. Then he was extubated for 24 hours total to five days going six today.
Patrik: Okay. So it’s fairly new. How old is your father-in-law? Oh, 67? Yeah. Okay. What are they saying is the next step?
Joefbert: They’re just hopeful, but the main problem is the lung infection which is not, maybe the antibiotics are not responding.
Patrik: The reports are still pending. We don’t really know what they’re treating yet. With a hundred percent of ventilator support. Do you know if he’s getting anything like nitric oxide?
Joefbert: No.
Patrik: All right. So that definitely treatment options set up. I’m sure you’re not aware of, have you heard of prone position?
Joefbert: I’m not aware because I’m not from medical background. Maybe you can give me some options then I can just discuss with you accordingly.
Patrik: So one option is a prone position. It basically means you’re turning a patient upside down to drain the lungs, it’s very effective, but you also have to put patients in a very deep coma and you potentially have to paralyze them temporarily. The other option is ECMO, which is a bypass machine. And then the other option might be depending on the nature of the pneumonia, or the lung failure. Another option might be nitric oxide. You can go back to them and say and see what they say. I do believe the shortcut would be if you had me on a call with the doctors, that would, I believe would be the shortcut. So you have someone that can advocate for you or for your father-in-law on a clinical level. That would be the shortcut. No, COVID has been ruled out. That’s good. Is he on any inotropes? I can’t see that in your, oh yes.
Joefbert: Yeah he’s on inotropes.
Patrik: Do you know how much and do you know what are the inotropes?
Joefbert: That I don’t know? I don’t have any idea, but maybe if we can have a video conferencing with the consent doctor, then probably be a good idea.
Patrik: Absolutely. What’s their prognosis?
Joefbert: Hmm.
Patrik: What is the doctor’s prognosis?
Joefbert: It is very difficult to say because they are not getting any leads so far. So basically they are relying on the antibiotics, earlier they tried some Vancomycin, then there’s a Tazobactam-Piperacillin and a Meropenem and now after ET culture, they have changed it. Now it is Colistin and Tetracycline. So this was the only antibiotic which was found to be sensitive against these particular bacteria. That is what I have determine the name I have written.
Patrik: Yeah.
RECOMMENDED:
Joefbert: It’s Acinobacter Baumannii, which is basically maybe due to long-term ventilation or maybe due to some hospital conditions.
Patrik: I’m just looking, I’m just reading everything now in more detail. So he had surgery not too long ago.
Joefbert: Surgery was on six, so it is almost eight days.
Patrik: And that was for a mitral valve repair or replacement.
Joefbert: Yeah. And I noticed that was planned. That was planned. Okay.
Patrik: And there was no bleeding after surgery as far as you’re aware.
Joefbert: Bleeding while they’re after surgery.
Patrik: Okay.
Patrik: Does he still have drains in his chest?
Joefbert: No.
Patrik: Okay. And when your father-in-law was at home, was he still active?
Joefbert: Yeah, he was still active during the day when the procedure of stenting was done, he was recovering well but that time we didn’t know that there was some leakage that regurgitation was there of the mitral valve. We are not aware earlier. It was mild, but later on it became worsened and maybe within a two-month period it became very severe. So due to which the part of this mitral valve replacement and then associated problem of aneurysm was also detected. And then both the surgery was done successfully. He was like a chronic smoker due to which he was diagnosed with COPD 15 years back and that patch was there in the lungs and later on it deteriorated and the lungs could not sustain after the surgery. So that is the basic concern. If there is any hope that he can revive back.
Patrik: Look.
Joefbert: But again one more thing happened that the two days back sorry three days back he was, the urine output ratio decreased and he was put on dialysis because almost no urine output was there. There is problem of kidney also due to maybe diabetes, or I really don’t know.
Patrik: Yeah, that’s good. That’s good. Okay. It’s nothing out of the ordinary that patients go into kidney failure after open heart surgery. He’s got diabetes, he’s got a poor ejection fraction. So I’m not surprised that he’s gone into kidney failure. If his lungs don’t recover, the first two options are probably, see whether the antibiotics are working and whether they can find a growth bacteria and then target with the right antibiotic. That’s number one, number two would be, potentially nitric oxide and a number three might be prone position, but that could be a little bit of an issue because he’s got a chest wound.
RECOMMENDED:
Joefbert: Yes
Patrik: Not impossible, but could cause further damage and number four could be ECMO. Those would be the options. But that’s really only after they have found a bacteria and hopefully targeted that bacteria with the right antibiotic. What about, can you visit your father-in-law or are you locked out because of COVID?
Joefbert: No, I can visit. I’m just going there. I got a call from doctor, I’m just with it. If you need, then we can have a video conferencing with the doctor and probably whatever is your prescription of best care please you can just email me, then we can have this question. Maybe if that can be of some use to us and you can pull us out of this situation, it can be a great help.
Patrik: Yup. Look at the next step is you would have to select from one of the consulting options. Obviously, if you wanted, advise any further, you would have to sign up for one of my paid consulting and advocacy options, which are emailed to you and also put in Skype. Very happy to help you. You just have to select from one of the options that I sent you and go from there.
RECOMMENDED:
Joefbert: I will discuss with the doctor and get back to you. Okay?
Patrik: Okay. Thank you so much, Joefbert. You take care.
Joefbert: Thank you so much. Bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!