Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy. Ashanti’s dad has been readmitted in the ICU and Ashanti is asking how to fight for his dad’s life whilst the ICU team is forcing to withdrawal of treatment.
How to Fight for My Dad’s Life Whilst the ICU Team is Forcing to Withdrawal of Treatment?
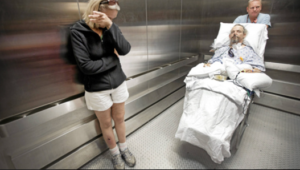
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hello Patrik,
Hope you are doing well. It’s been a few months since I contacted you earlier. I have your monthly membership still going on.
Yesterday my father was taken to the Emergency Room for hypotension and fluctuating diastolic blood pressure.
He is admitted to the nearest hospital.
Some of the medical problems he is facing are as below:
- His urine output is limited per hour than expected. They are giving him now albumin intravenously. Not sure how much it would help in his case.
- His blood pressure is 105/53 after giving him vasopressors.
- His blood creatinine is high due to the improper functioning of his kidneys. Not sure what could be done further.
- Some kind of bacterial infection through his urinary tract has affected him severely up to the kidney per his doctor. They are treating him with a broad range of antibiotics. Waiting on his blood culture to come back.
- His body temperature seems to be lower than normal. According to them, this is due to some kind of septic shock. He is being given IV fluid and provided with some kind of warming blanket and he is around 95 F.
All the vital parameters (oxygen saturation, heart rate, blood pressure, etcetera) seem to be okay after giving him IV fluids, vasopressors, and antibiotics.
Doctors and nurse practitioners are pressuring me with Do Not Resuscitate and withdrawal of treatment as he might not survive treatment. This is very pessimistic and depressing to me.
I have not agreed to it and mentioned to them to have full code resuscitation and provide all treatment and care needed to come out of this situation.
Very confused, anxious, and concerned with his situation and how the hospital team is handling him in the ICU. They are saying his organs are failing and he is not going to survive.
Awaiting your suggestions. input and things that need to be monitored for my father to come out of this medical situation.
In addition, just to mention his current baseline while being admitted to ICU
He has been without the tracheostomy tube for more than 3 months. Just 2 liters of oxygen was given through his nose.
He is mentally alert and conscious to a minimal level. Opening his eyes and looking at people and objects, moaning in pain, making limited movements on his right side. Left side paralyzed due to stroke that happened 6 months back.
His heart rate is slightly higher with atrial fibrillation.
Will check his liver function, and lactate levels. The concern is about his body temperature getting lower. I also asked about starting tube feeding for his nutrition as they are only giving IV fluids. They might start after consultation with a dietician. Also requested to give Vitamin C as well, not sure if they would do it. They are concerned about his heart functionality as he is on vasopressors.
How would the recovery be from here? What are the ways they monitor and tackle this kind of septic shock situation? How long a patient can be on vasopressor? How much would they taper? Right now he seems to be on it continuously since last night as his blood pressure got low.
I will hold on to the full code resuscitation and treatment going forward.
Awaiting your valuable comments.
Thanks & Best Regards
Ashanti
RECOMMENDED:
Hi Ashanti,
How are you, Ashanti? We really appreciate your ongoing membership with the intensive care hotline.
Thank you for sending us an email again.
Sorry to hear about your dad’s current condition.
Per your email, your dad has issues with his urine output being low, albumin being given, also with episodes of hypotension and on inotropes, being unable to titrate down, with blood creatinine high, with a bacterial infection that has affected his kidneys, being on antibiotics, awaiting blood culture result, with his temperature on the low side, mentioned about septic shock, IV fluids given and warming blanket for the hypothermia. All vital signs seemed okay after IV fluids, vasopressors, and antibiotics.
Regarding your most recent email and questions:
It’s good to hear that your dad has been decannulated for the past 3 months, and he is currently on oxygen inhalation per nasal cannula at 2 liters only for now. They need to closely monitor his oxygen requirement continuously for now.
It is important that the nurses and doctors are monitoring his Glasgow Coma Scale routinely to consistently evaluate the consciousness level of your dad. By routinely assessing your dad’s Glasgow Coma Scale, a downward trend in his consciousness level can be recognized early and so allowing time for appropriate interventions to be performed by the nurses and doctors.
With his body temperature getting low (hypothermia), yes, an altered core body temperature is a hallmark of sepsis. Although fever is most commonly associated with sepsis, hypothermia can also occur spontaneously, and rewarming your dad with the warming blanket may help. Though the doctors and nurses should target how to resolve the sepsis itself.
Tube feeding may be started for your dad as long as he is able to tolerate/digest feeds, with no signs of any respiratory distress at the moment. It is important that he is comfortably breathing okay with his current oxygen support before starting any feeds because we want to prevent aspiration pneumonia. Nutrition can be supported with intravenous fluids in the meantime, if they see that your dad is still not ready yet for tube feeds. And yes, he needs to be evaluated also by a dietician to appropriately assess his readiness and address his nutrition needs. Vitamin supplements can also be given.
There may be different significant things to consider when addressing his heart functionality. One is the current cardiac medication he is taking especially for his atrial fibrillation. Has he been followed up by the cardiologist to reassess his cardiac issues and his cardiac meds? Any recent electrocardiogram or ECHO (echocardiogram) done to assess his cardiac functionality? What were the results? Is his hemoglobin level within the acceptable range?
To tell about your dad’s recovery from his current condition now, we need to know the results of his current laboratory tests like the complete blood count, lactate, electrolytes, CRP (C-Reactive Protein), blood culture, and urine culture. What are the latest vital signs for the past 24 hours? Any increase/change in oxygen support? What is his current Glasgow Coma Scale? What IV fluid he is having now? Does he have any central line or arterial line? Any arterial blood gas done? What antibiotics is he currently on? What other medications are they giving him?
For septic shock management, these things are important: early recognition, source control, early and adequate antibiotic therapy, early hemodynamic resuscitation, and continued support to maintain adequate organ system function for your dad with proper oxygen support/respiratory management.
Weaning your dad off the inotropes depends on his response to his current treatment/management. It is important they also monitor his hemoglobin level as well to see if he needs to have a blood transfusion that may improve his cardiopulmonary function. Also, targeting the source of infection by giving the appropriate type of antibiotic.
And definitely Ashanti, you can hold on to the full code resuscitation and treatment going forward.
Hope this helps.
Please update us on your dad’s current condition.
Thank you.
Kind regards,
Patrik
Suggested Links:
Hello Patrik,
Thanks for your email replies. To update on his current condition.
All his vital parameters seem to be okay. He is on Vancomycin and another antibiotic based on his urine culture. He had a severe UTI (urinary tract infection) that affected his kidneys. Currently, his urine output seems to be okay. They seem to have given some blood as well. Kidney function is just okay but needs monitoring. A nephrologist comes and checks on him periodically.
I need your advice and suggestions. His skin on the abdominal area near the PEG tube has become damaged due to secretions from stomach acids and secretions. They have stopped PEG tube feedings and are going through nasal feeding for the past few days.
Spoke with the gastrointestinal doctor over the phone on Monday and as per him, they are going to continue with wound care around the stomach area. They are cleaning and dressing as often as required. This would take weeks to heal.
He is being given Tylenol to manage pain and discomfort. Now as usual the hospital authorities are suggesting palliative care/hospice care without giving time for his recovery from earlier sepsis. I mentioned that he needs all the curative care and needed to be patient in recovery.
They always pressure me with the withdrawal of treatment, DNR (do not resuscitate), etcetera, but I stay strong and push back.
Frustrated and concerned by this approach by the hospital rather than providing the proper care towards his recovery. I am surprised as to why they don’t want to focus on the treatment rather than talking about palliative care and hospice. Can they somehow force any patient to go with this kind of care in spite of refusal? It’s making me very stressed with regards to his care.
He has shown improvement in a week’s time. How would his recovery be going forward? They seem to be negative about his prognosis with gastrostomy tube area wound healing. How long can it take to heal? considering secretions. Does it close by itself and heal?
I was of the belief that since the stomach area wound is not pressure related it might heal faster than a pressure sore.
Awaiting your inputs at your earliest.
Thanks & Best Regards
Ashanti
Recommended:
Hi Ashanti,
Thank you for updating us on your dad’s current condition.
Good to hear that all his vital parameters seem to be okay.
With regards to your dad’s current problem/issue with his abdominal wound from the PEG tube site, here are some information I want to share with you:
**The most common complication of the PEG (percutaneous endoscopic gastrostomy) tube insertion site is an infection at and around the area and infection can occur as a result of poor hygiene when handling the tube.
**Gastric secretions leaking around the gastrostomy can result in skin excoriation and there are methods of minimizing irritation to the skin as specified below:
Use of a barrier ointment. Recommended products include Calmoseptine ointment or a zinc ointment.
If the site is affected by thrush, do NOT use a zinc-based product as this may worsen the infection. Suitable alternatives include Orabase or Coloplast paste.
Medications to halt gastric acid production like Omeprazole can also be prescribed.
**Red, irritated, swollen, oozing skin surrounding a gastrostomy can be treated with:
A foam dressing, gauze to absorb excess ooze.
Hydrocolloid powder to aid in stopping bleeding and absorb excess moisture.
A thin hydrocolloid dressing to protect and aid in the healing of excoriated skin
The right type of antibiotic after wound culture results.
**Recommendations above as per advice by the medical team after assessment.
For his gastric tube site wound healing, it depends on how severe the wound is and your dad’s response to treatment. It is also important to know what type of treatment they are giving him. It would be advisable to have a wound swab taken for culture if the site has clinical signs of infection prior to commencing treatment. It is important to know if there may be bugs present within the wound that needs to be targeted with the right type of antibiotic.
RECOMMENDED:
Now they stopped PEG tube feedings and if they plan to have it removed to relieve pain, he needs to have a good and patent access to nasogastric tube feeds. They need to do routine checking of the nasogastric tube correct placement to prevent aspiration.
Wound care under aseptic technique also plays a very vital role.
Evaluation by a wound care specialist may also be done to appropriately advise for the right kind of wound care/wound dressings/topical antibiotic cream to be provided for faster healing. Proper nutrition also aids in healing with supplements.
Sometimes, the stoma or site does not close easily on its own especially if it has been there for a long period of time, and had problems with the site. It also does not close easily if there are certain medical conditions that make healing more difficult. Sometimes, surgeons may need to surgically close the site but typically, doctors will wait before performing surgery to try to allow the site to close on its own.
Hope this information helps, Ashanti. Keep pushing for what you think is right for your dad. The medical team will always be negative and advise for withdrawal of treatment. But you always have the right to refuse and fight for your dad’s recovery.
Thank you.
Kind regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!