Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy.
Ashanti’s dad is in ICU with a stroke & is on a ventilator and she is asking why are they in a hurry to push him out to LTAC.
My Dad is 5 days in ICU with a Stroke & is Ventilated. Why Are They In A Hurry To Push Him Out to LTAC?
Hello Patrik,
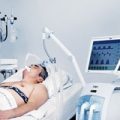
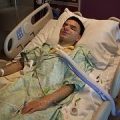
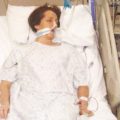
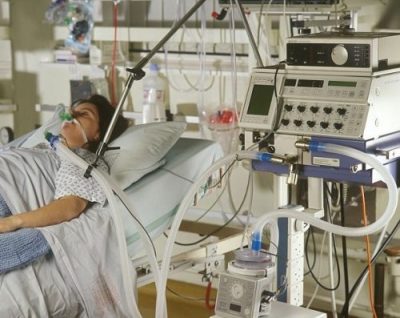
My dad who is 91 years old is currently in neuro ICU for 5 days due to brain hemorrhage. He was admitted last Thursday to the hospital due to shortness of breath, he was also tested positive for COVID. He was feeling better for the first 4 days until Tuesday. He was on blood thinners like aspirin and given Lovenox injections to prevent stroke. But due to his fluctuating blood pressure and combination of these medications he developed brain hemorrhage on Wednesday afternoon. He got disoriented and could not communicate as before. Based on MRI (Magnetic Resonance Imaging) scans, doctors gave medications to stop bleeding. It stopped for a brief period but on Wednesday afternoon the bleeding worsened and cardiologist put him on ventilator support. He was sedated as well along with blood pressure medications so that bleeding doesn’t worsen.
Now he is paralyzed on the left side due to bleeding on the right side of his brain. On subsequent scans bleeding had stopped and he was hemodynamically stable for the past few days. But he is very drowsy, occasionally waking up. He is not on sedation for the second day. Respiratory therapist tried the SBT (Spontaneous Breathing Trial) for yesterday and today and it was not successful so continued on with ventilator support. I presume that they are going to try it in the coming days as well. Hope this would progress well so that he could wean off ventilator support. His ventilator setting as per nurses seems to be on lower end. (Tidal volume about 400).
Due to COVID restrictions, I cannot be on his side during this tough period. Sometimes I feel very helpless but only after watching your videos could I feel comfortable. Only getting updates through the phone. He has a feeding tube inserted through the mouth. On the improvements/positive side, he has not been sedated for the past few days, vitals are stable, IV medications have been reduced/stopped. All the medications are powdered and given through a feeding tube.
For other updates, they have done SBT (Spontaneous Breathing Trial) for him before they decide to go with tracheostomy as the next step.
I know there are risks with tracheostomy but it’s a safe procedure for critical care patients and I hope due to old age he will be able to withstand it.
Doctors were negative and earlier trying to convince me about his body not able to withstand the pain of going through tracheostomy. But I was insisting on providing him all the care needed.
I hope the brain bleed gets absorbed in the body in the coming weeks as mentioned by doctors/nurses.
I also hope that my dad is progressing in the right direction and hoping that his condition will get better so he could be weaned off the ventilator support.
As he is very old, severely debilitated, he might need rehabilitation/care once he is weaned off his ventilator and moved out of ICU to a regular hospital room. I also wonder about his quality of life after this.
Earlier doctors and others were discussing palliative care and eventually moving him to LTAC as well. They mentioned as we progress they have to go by the hour and day. I know it’s a long process to come out from this situation. How best to handle this period as I feel very anxious and sad at times.
Awaiting for your replies and further course of action. Also aware of the risks about Long-term Acute Care (LTAC) once he is out of hospital ICU.
I am really very interested about your service.
Thanks & Best Regards
Ashanti
Hi Ashanti,
Thank you for giving the details of your dad’s current situation.
So the primary reason your dad is in ICU is not COVID, it’s the stroke and he has been in the ICU for only 5 days.
So, looking at the quality of life. When patients survive intensive care, you don’t know what the quality of life looks like in six months’ time. So you really got to break your goals down into steps. I guess, at the moment, the goal is to get your dad out of intensive care alive. We don’t know what that looks like. We don’t know, does he need a tracheostomy to get out of intensive care alive? Nobody knows at this particular point in time.
Whether he can come off the ventilator, or if he ends up with a tracheostomy, nobody knows at the moment. The easiest way would be to get him off the ventilator without a tracheostomy. That should always be the goal.
Here is the thing, if someone can’t come off the ventilator with the breathing tube after 10 to 14 days. Then a tracheostomy needs to be considered. If for whatever reason, either the patient or the family doesn’t want a tracheostomy. Well, you could argue let’s stop treatment, and let’s look at the end-of-life options. But that is still your decision. It’s not the hospital’s decision.
Your dad is only 5 days in the ICU and you have to ask them, why are they in a hurry to move him to LTAC (long-term acute care)? There’s no rush to let people die. LTAC is a better version of a nursing home and we strongly oppose sending patients to LTAC because of the risks it involved.
Ashanti, you need to ignore their negativity. They are negative all day long for their own reasons. Watch what they’re doing, don’t watch what they’re saying. As long as they’re treating your dad, this is way more important than them being negative.
Regards,
Patrik
Hello Patrik,
It was really good speaking with you yesterday.
Thank you also for your email.
Today, I happened to discuss with one of the intensivist doctors at the hospital. She was saying like weaning off a ventilator is going to be difficult as he is in a limited consciousness state. He cannot handle his secretions. She was giving me options, of whether my dad would like to have a tracheostomy and then weaning and then moving to long-term acute care nursing facility and he is only 5 days in ICU.
A bit frightened and concerned that medical professionals are rushing to move him out of ICU. Let me know how and when we could have our next call.
Thanks & Best Regards,
Ashanti
RECOMMENDED:
Hi Ashanti,
Look, the first thing that stands out to me here, Ashanti is, five days on a ventilator is not a long time. So moving someone to LTAC after five days, from my experience, is inappropriate. If you came to me five weeks, I would say, “Okay, all right. What’s happened in those five weeks?” Five days is not a long time.
So let me explain this to you, steps forward. LTAC, from my experience, is inappropriate at this time. As I said to you, if you came to me, “Oh, it’s been five weeks. He’s still on a ventilator. He’s not waking up.” Okay. Well, let’s reassess the situation. But for someone that is only 5 days in ICU, well, that is really inappropriate.
The question with the tracheostomy is really if he can’t come off the ventilator for 10 to 14 days, then a tracheostomy might be the right thing to do. If you feel they’re pushing you towards palliative care or LTAC, I wouldn’t get pushed, because that might be the end of the life for your dad.
Anyway, Ashanti, let me ask about his consciousness state. What is his GCS currently? GCS is Glasgow Coma Scale and it is a clinical tool used to reliably measure a person’s level of consciousness. Please see this link below for a detailed description of the GCS.
You can also send us pictures of your dad’s ventilator monitor, his most recent arterial blood gas, and chest X-rays. Is he on any sedation? Is he on any inotropes or vasopressors?
Going forward, Ashanti, I believe I can help you. One way I can help you with is certainly by giving you a second opinion, and talking to the doctors with you. I do believe that would be very helpful because I argue that they always tell families only half of the story.
So, they’re telling you, he should go to palliative care. He should go to LTAC. If you and I were on a call with the doctors, I would ask them a series of clinical questions. And I would ask them, “Well, have you done this? Have you done that? So, at the moment, you are in a position where you can’t ask all the questions. I’ve worked in the environment for 20 years. I can just rattle off some questions and they know, okay, they have to tell you the full story. They have to be transparent.
Kind regards,
Patrik
Hi Patrik,
Thanks Patrik for your email and for sending the GCS (Glasgow Coma Scale) article from your website at intensivecarehotline.com. As per my dad’s current situation, he seems to be GCS scale of 5 or 6. Not sure about his status. As per one article they are mentioning that 8 and below are comatose/low-level consciousness/vegetative state. It’s somewhat not clear to classify.
Also would try to get a picture of his ventilator settings. For arterial blood gas, they seem to check on his CO2 (Carbon Dioxide) and it seems to be okay as per the physician and they want to do another procedure or something to check it.
Chest X-rays seem to have no change. He is not on any sedation. Will check on vasopressors.
Also as per the intensivist doctor, they are planning to do a tracheostomy tomorrow for my dad and then subsequently do a procedure to insert tube into the stomach instead through an oral tube now.
Hopefully, these are safe and appropriate to perform for my dad’s recovery process.
Best regards,
Ashanti
Hi Ashanti,
They are safe procedures generally speaking however the aim should still be to get him off the ventilator and avoid the tracheostomy and the feeding tube.
I do believe that a picture of the ventilator and a full arterial blood gas result would gauge whether he needs a tracheostomy or not.
Having said that, with a GCS (Glasgow Coma Scale) of 5-8 he wouldn’t be in a position to avoid the tracheostomy at present.
Kind regards,
Patrik
Suggested Links:
Hi Patrik,
They are not trying to just wean off the ventilator without a tracheostomy. Today is the eighth day on ventilator support.
He seems to have done SBT (Spontaneous Breathing Trial) for about a couple of hours for the past 5 -6 days.
Do you think they have to delay tracheostomy?
They are making plans to do a tracheostomy tomorrow and a feeding tube the following day. Is this a good approach for him going forward as he is minimally responsive and not having much success with the straight weaning-off process?
I will try to get a picture of his current ventilator settings.
Thanks and best regards,
Ashanti
Hi Ashanti,
If they do a tracheostomy this quickly they might want to send him to LTAC which is going to be risky for him.
If you’ve done any research about LTAC, you would find very negative feedback about LTAC.
You can send us the picture of his current ventilator settings Ashanti.
Regards,
Patrik
Hi Patrik,
They have already done a tracheostomy today. They were mentioning that tomorrow they would be doing a feeding tube procedure. They also mentioned that they would continue with ventilator weaning with tracheostomy in the coming days.
Makes me concerned. Also mentioned about 24/7 skilled nursing facility. Please let me know as to whether we are going in the right direction.
Also one of the nurses mentioned as now ventilator setting is back to 100% as he just did a tracheostomy.
Thanks and best regards,
Ashanti
Hi Ashanti,
If they are moving him to a skilled nursing facility you need to object.
Weaning sounds good, you need to make sure it’s actually happening. Trust but verify!
Ventilator is back on 100% of support because he has been given general anesthesia during the tracheostomy procedure.
It should be temporary. Let’s keep monitoring.
Regards,
Patrik
Hi Patrik,
Thanks Patrik.
As of now, they are not moving out of the hospital. But one of the hospital case managers discussed today afternoon about my dad’s long-term care options. I mentioned that I don’t have anything in mind and could send me some options to my email address.
I had mentioned that he has to be continued with weaning and any neuro therapy needs to be done and it’s early to discuss at this point. Also, the current place he is staying is not capable of providing the needed care.
I will further update you, Patrik.
Thank you.
Best Regards
Ashanti
Recommended:
Hi Patrik,
My dad completed both procedures – tracheostomy and PEG PEG (Percutaneous Endoscopic Gastrostomy). He seems to be doing okay.
They are trying to wean him off the ventilator by doing daily SBT. But my dad seems to tolerate it only for some time. Today on interacting with one of the nurses, I got the ventilator settings. They hesitated to send out pictures of the same.
PEEP (Positive End-Expiratory Pressure) – 6
FiO2 (Fraction of Inspired Oxygen)- 35 %
Respiration Rate – 16
Tidal Volume – 400
As per them, this seems to be set on the lower side. Dad is still not fully awake and responding to oral commands /signs. They seem to not be doing any other neural stimulation or therapy of any sort as of now. How long is the weaning process? Would it take weeks to make some meaningful progress in my dad’s case?
As per interaction with them, I would guess they are inclined to move him out of the ICU sooner if he is stable and continue the weaning process and then discharge to LTAC.
Based on your previous experiences please share some insights and guidance further.
Thanks.
Ashanti
Hi Ashanti,
The numbers look good with PEEP (Positive End-Expiratory Pressure) of 6, FiO2 (Fraction of Inspired Oxygen) of 35 %, respiratory rate of 16, and tidal volume of 400.
What ventilation mode is he on?
Are the 16 respiration rate per minute spontaneous, machine delivered or a combination of both?
This is where the rubber hits the road, please find out.
Weaning can take from days to weeks or months.
It sounds like he is making progress, but please find out the ventilation mode he is in and also find out if there are any recent arterial blood gases.
Physical therapy and mobilization is not optional!
We need to know as well if his vital signs are all stable and that he is not having any fever.
Kind regards,
Patrik
Hi Patrik,
Thanks Patrik for your prompt reply.
Based on my interaction with the nurse tonight, his respiration rate of 16 seems to be a combination of spontaneous and machine-delivered. Though they seemed not to have done any SBT (spontaneous breathing trial today) today.
They mostly would be doing one tomorrow. His vitals seems to be okay. Not on any IV medications. He seems to have a loose bowel movement due to his tube feeding for the last 12 days. Also had a low-grade fever of 99.1F. These seem to be minor in nature.
They did a chest X-ray this morning. No significant change from his COVID pneumonia that was existing before. As per our conversation, 5-6 days back his COVID-related biomarker seems to be coming down in his routine blood test.
This could be confirmed again tomorrow.
Let me know your thoughts.
Regards,
Ashanti
RECOMMENDED:
Hi Ashanti,
He will only be able to come off the ventilator if he can breathe spontaneously.
The ventilation mode before extubation is called CPAP (Continuous Positive Airway Pressure) or pressure support.
Keep asking for the following:
– What is the ventilation mode?
– What is the ventilator PEEP (Positive End-Expiratory Pressure)?
– How much pressure support is he on?
– What are his tidal volumes?
– His minute volumes – the volume of air that can be inhaled (inhaled minute volume) or exhaled (exhaled minute volume) from a person’s lungs in one minute.
– What is his ventilator’s FiO2 (Fraction of Inspired Oxygen)?
– What is the result of the most recent Arterial blood gas?
– Does he have a good strong cough?
– How frequent are they suctioning him?
– Is he obeying commands?
For further reading and as a guiding article/video, you can click on the link below from our website at intensivecarehotline.com:
HOW TO WEAN OFF VENTILATION AND TRACHEOSTOMY STEP BY STEP!
Kind regards,
Patrik
Suggested Links:
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!