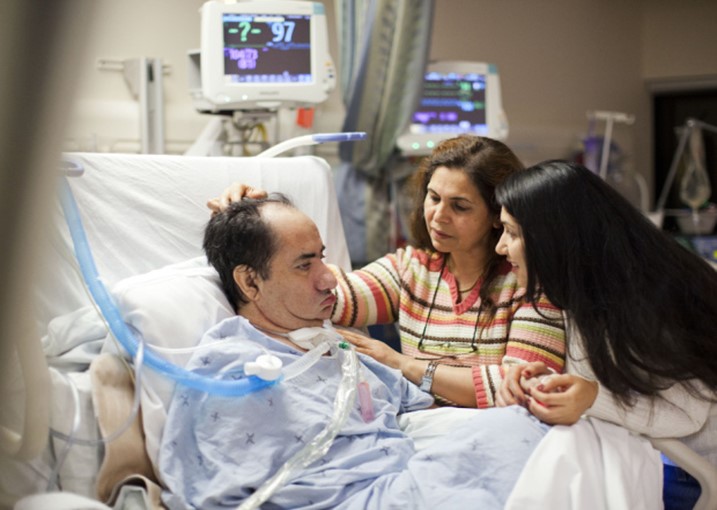
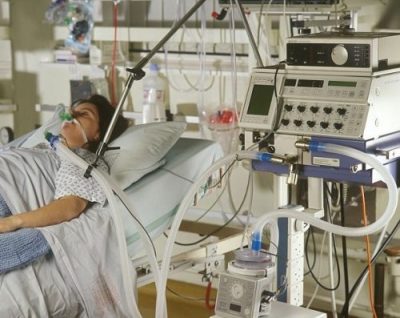
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad is in ICU with a Stroke & is Ventilated. What are His Chances of Weaning off the Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy. Ashanti’s dad is a long-term ventilated patient in ICU. Ashanti is asking how can they stop the ICU team from sending her dad to LTAC.
How to Stop the ICU Team from Sending My Ventilated Dad to LTAC? Help!
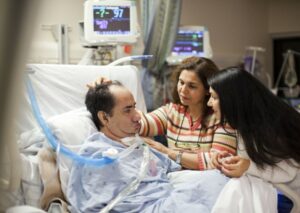
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hi Ashanti,
How are you, Ashanti? I hope this email finds you well.
Thank you for emailing us again.
It’s nice to know that your dad has been hemodynamically stable.
In regard to weaning your dad off the vent, having neurological issues such as stroke is one of the most common issues that might prolong weaning off a ventilator. The process of weaning off the ventilator for your dad might not be a straightforward process and numerous setbacks might occur and therefore delay and prolong the weaning process. Your dad may have the ability to be tried getting off the ventilator but not enough endurance.
It is extremely challenging for sure and sometimes frustrating when we are faced with a loved one that is unable to be weaned off the ventilator. However, the weaning process for your dad is a team effort. It is a multidisciplinary team approach, while the respiratory therapists initiate the protocol for weaning your dad, nurses, doctors, nutritionists, and physical therapists should be involved in the process giving emphasis on good clinical assessment.
Moreover, I have seen that you mentioned about a pressure sore stage 4. That needs to be fully addressed and needs to be assessed by the wound care management team so they can advise how to manage and prevent any potential infection this may bring.
The following precautions can help minimize the risk of developing pressure ulcers in at-risk patients and to minimize complications in patients already exhibiting symptoms:
- Patient should be repositioned with consideration to the individual’s level of activity, mobility, and ability to independently reposition. Q2 hour turning is the standard in many facilities, but some patients may require more or less frequent repositioning, depending on the previous list.
- Keep the skin clean and dry.
- Avoid massaging bony prominences.
- Provide adequate intake of protein and calories.
- Maintain current levels of activity, mobility and range of motion.
- Use positioning devices to prevent prolonged pressure bony prominences.
- Keep the head of the bed as low as possible to reduce risk of shearing.
- Keep sheets dry and wrinkle-free.
I hope this helps.
Take care.
Kind regards,
Patrik
Hi Patrik,
Thank you for the information.
Anyway, for the updates, my dad is being given SBT (Spontaneous Breathing Trial) every day. He had tolerated it for about 5 hours for the last couple of days. Now hospital people want me to plan for his discharge with ventilator support in a long-term care facility.
He is also being treated/cared for pressure sore by the wound care team. He had gotten it after coming to the hospital this time around. I would say primarily due to negligence on the part of care providers at the hospital. He is on a wound vacuum device to drain out any excess fluid. He is also treated with antibiotics.
Do you know how long/how fast this can take to heal? As per the current assessment, he is at GCS (Glasgow Coma Scale) level 7 or 8 showing slow improvements. Though PT (Physical Therapy) and OT (Occupational Therapy) had to be more involved going forward.
I am not ready to discharge until this wound heals. Also weaning him off might take weeks at his current level. He’s on an ICU setting for over a month now. Will the hospital force me to discharge in such a situation?
I even asked whether he needs an ICU environment at the hospital for his care considering his hemodynamical stability thus far. They are hinting that he cannot be weaned off the ventilator and can continue in LTAC (Long-Term Acute Care). This is kind of premature on their part.
Confused as to how to handle this situation and proceed forward.
Thanks & Best Regards,
Ashanti
Hi Ashanti,
Thank you for your reply.
Your dad is showing progress. It would be better if your dad can be weaned off totally from the ventilator.
It’s good to know that his wound has been already attended to by the wound care team. Good nursing care, appropriate wound care management, proper nutrition, and mobilization play a vital role in wound healing.
And as we always advise, you can always say no if you see that your dad is still not fit to be discharged.
Regards,
Patrik
RECOMMENDED:
Hello Patrik,
Attached are his ventilator settings pictures for the past few days. He is in CPAP (Continuous Positive Airway Pressure) mode of breathing. Showing some improvements.
How would be his path forward from here in terms of ventilator weaning perspective? How long it might take? What all precautionary measures and monitoring that needs to be done in specific?
Let me know.
Thanks & Best Regards,
Ashanti
Hi Ashanti,
Thank you for the update.
A few questions for clarification.
1) I assume he is on the trach collar when you are referring to an SBT (spontaneous breathing trial)? Do you know how much oxygen he is on when on the SBT?
2) How often does he needs suctioning and does he have a good spontaneous cough?
3) Are they doing or have they done arterial blood gases?
4) Are they doing regular chest X-rays?
5) What size of tracheostomy is it?
6) Do you have access to the medical records, including test results, medical and nursing progress documents online?
7) Is he getting mobilized or physical therapy?
8) Why does the hospital want to discharge him, is it because of the health insurance and your dad running out of entitlements? If you haven’t heard from the health insurance directly I wouldn’t worry too much about the hospital trying to discharge to LTAC.
9) You mention clinical instability, is he on vasopressors or inotropes?
https://intensivecarehotline.com/your-loved-ones-treatment/inotropes/
10) As far as the VAC (Vacuum-Assisted Closure) dressing and the pressure sore is concerned, it is definitely negligence because a pressure sore must never happen and can be prevented by good nursing care. It is difficult to say how long it’s going to take to heal but it can take many weeks.
11) What antibiotics is he on?
12) Ventilator pictures: he is breathing CPAP/ pressure support with a PEEP (Positive End-Expiratory Pressure) of 6 and a pressure support of 14. His breathing rate is comfortable at 15-20/minute but pressure support is too high to get him off the ventilator completely. Pressure support ideally is less than 10. Tidal volumes look a little low but then again it depends on arterial blood gas results.
30% of oxygen is okay, how much is he on when on the tracheostomy collar?
Kind regards,
Patrik
Suggested Links:
Hello Patrik,
Thanks for your support. Currently, my dad is off the ventilator support and CPAP support for the past few days. Nearing 7 weeks in ICU after initial COVID then hemorrhagic stroke.
He is on something like T-Piece support as per what I hear from nurses. He is been hemodynamically stable. Now he is on 28% oxygen support. Something like 9 liters of oxygen. I have sent a picture of his ventilator monitor with the setting.
Is he making good progress in terms of his respiration?
They seemed to have tried to make his breathing on room air. Is this the next step in the weaning process of tracheostomy? Please clarify. If so how long it typically takes? They also tried speaking valve by speech therapy. Would removal/ decannulation of the tracheostomy tube take place afterward?
Meanwhile as before Case Managers have started to reach me to pressure me to look for LTAC facilities. I had mentioned that I don’t want to jeopardize his health by moving him out prematurely after working so hard thus far.
It’s really astounding to know such compassionless care for such ICU patients.
Not much useful PT and OT are currently provided. They are not referring to rehab facilities as well. In fact, the hospital has one but is not willing to accommodate due to lack of insurance coverage for such services.
As mentioned before he has a pressure sore which is being treated with a wound vacuum. There might be some progress but not sure how much it would take to fully heal. This had been negligence in care on the part of the hospital.
With this condition, not in a position to move him out of the hospital. They should attend to these medical conditions then probably step-down the non-ICU unit and then if stable move to rehab etc.
Am I thinking/planning right in my dad’s slow recovery and path forward?
Also, the case manager was adamant in his conversation that if I don’t find the next place for my dad then they have to find one (LTAC). Is this even allowed and legal to force patients out? This is harassment.
Awaiting your reply at the earliest in this stressful time period.
Thanks & Best Regards,
Ashanti
Hi Ashanti,
How are you, Ashanti? I hope you are doing well in these trying times.
Anyway, with regards to your last email, you mentioned that your dad has been off the ventilator support and CPAP for the past few days. The picture of the ventilator attached shows he was still on a ventilator on PS (Pressure Support)/CPAP mode, FiO2 (Fraction of Inspired Oxygen) of 30%, PEEP of 6, PS of 14, breathing at 15-21 bpm, tidal volumes on the low side. But then, you mentioned that he’s currently on T-piece oxygen support, with FiO2 28%, Flow 9 liters of O2 (Oxygen).
We just want to know how your dad is responding through the oxygen support via T-piece (Is he breathing okay with that, no desaturations, heart rate and BP (Blood Pressure) within acceptable parameters), how many days your dad has been off the ventilator support and if they have done any recent blood gases after that. We need to see these results to see further how he is doing with the current oxygen support to be able to tell how he is really progressing respiratory-wise. PT/OT plays also a vital role in his recovery.
How is his wound right now? Can we also have a picture of his wound if you may? What treatments are they doing for his wound? It sure is a part of medical negligence on the part of the hospital.
Another concern is the picture of his monitor where he was having AF (Atrial Fibrillation). What treatments are they doing to manage his Afib? Was he on any current medications for this? Any cardiology consult?
For any questions further, please let us know.
Thank you.
Kind regards,
Patrik
Hi Patrik,
Doing good in these trying times.
Now my dad has been moved to a non-ICU hospital ward/room. He is also on room air coming through with humidification. This is progress on his respiration side. They also started with a Passy Muir speech valve so that he could communicate. They are also monitoring him to see if he could tolerate it.
All his parameters like heart rate, BP, and respiration rate are being monitored and seem to be okay. Trying to get a picture of his wound. For his AFib condition, he is being given metoprolol and Cardizem, and his heart rate is maintained in the right range.
Now he is able to say a few words with a speech valve and he should be given more PT and OT for his mobility and physical movement. So far not much had been provided. I feel this is the next most needed one.
I am not going to talk further about discharge until he is completely weaned off from the tracheostomy tube, perform swallowing test and come to regular feeding rather than bolus feeding and the pressure sore completely healed. Is this the right approach?
Let me know.
Thanks & Best Regards,
Ashanti
Recommended:
Hi Ashanti,
Thank you for updating us on your dad’s current condition. In response to your email, please see below:
Your dad made real progress in terms of his oxygenation status. Though it’s been quite a while since he was taken off the ventilator, but I think he still needs to be assessed from time to time for his tolerance to breathing on room air.
In terms of his AFib condition where he’s on metoprolol and Cardiziem and has maintained his HR (Heart Rate) within normal range, a follow-up consult with a Cardiologist would still be necessary, and also for his medication regimen to be reviewed.
PT (Physical Therapy) needs to be done on a routine for your dad because it totally assists your dad in regaining his strength, coordination, balance, and control of movement. Along with OT (Occupational Therapy), which focuses on restoring functions for his daily living, and we can consider these 2 therapies as the core of his stroke rehabilitation.
Yes, definitely, you can raise your concerns with the medical team regarding weaning your dad from the tracheostomy tube. Another very important to address is, yes, to perform a swallowing test to prevent the risk of aspiration and assesses the severity of aspiration risk, and recommend a special diet accordingly for your dad. With the pressure sore, he still needs to be seen by the wound care team unless his wound is healed and they have signed off already from his care.
I hope this helps.
Thank you.
Kind regards,
Patrik
Hello Patrik,
Thank you for your response.
And for another update, my dad as you know was in Neuro ICU due to a hemorrhagic stroke. He was ventilated for a month and now he had been extubated and has been on room air for 4-5 weeks now without any complications. His tracheostomy tube size had been reduced and capped as well. He tolerated it for a week to 11 days without any significant issues. Now hospital doctors are saying that he can be ready to be discharged with a tracheostomy tube in place. They did not try decannulation of the tracheostomy tube. They are threatening me that if I insist on the removal of the tracheostomy tube he must be put on palliative care and he would pass away. This is not the desired outcome after having worked so hard for the last 4 months.
Below is his status with respect to the criteria for decannulation.
- Good strong cough/gag needs to be present in order to protect the airway
>> He had a good cough/gag and able to move it and swallow it as needed as per my observation
- Swallow reflex needs to be present so that your loved one is not aspirating secretions, sputum, gastric content, or food.
>> Swallowing test was done for an initial few days and then stopped and he had difficulty because of the long intubation period. He seems to be good and manage his secretions in my opinion.
- Able to obey commands (In the non-neurologically compromised patient)
>> He is in a minimally conscious state and needs interaction in our native language and could talk back to me on a few things. His speech is okay. Though he could not follow a lot of verbal commands. The right side of the body is paralyzed and able to make some movements of the upper and lower limbs.
- Adequate cough and ability to clear secretions effectively and independently.
>> He could cough independently and be able to swallow his secretions on a tracheostomy tube as I have observed. He needs someone to still monitor him in case of any problems.
- Cardiovascular and hemodynamic stability. – Good so far without any issues. Heart rate and BP had been good and are being monitored. He is on Afib which he is receiving medications.
- No new lung infiltrates on chest X-ray.
>> Chest X-ray seems to be normal.
- Tolerates cuff deflation for 24 hours.
>> Seems to have tolerated it.
- Tolerates speaking valve for 12 hours or more (usually during daytime) or decannulation cap for up to four hours (If the airflow is present on finger occlusion). In patients following head and neck surgery, the decannulation cap may be left for longer periods at the discretion of the surgeon.
>> Yes, tolerated speaking valve. He had tolerated decannulation capping for the last 10 days without any issues. O2 (Oxygen) saturation level is 99-100%.
He also has a pressure sore on his tailbone for which they are doing wound care/wound vacuum. This seems to be a slow process and could take weeks before coming to even 70 -80 % healing. They seem to be not bothered by it and insist that he could leave the hospital with a wound vacuum.
With this current state is it advisable to discharge him from the hospital and move to LTAC/palliative care? I feel this is totally unacceptable. Please share your thoughts at your earliest. Had to go through this tough situation again and the hospital doctors are rushing for discharge by tomorrow or move to palliative care.
Thanks & Best Regards
Ashanti
Suggested Links:
Hi Ashanti,
Thank you for renewing your membership, thank you for your support, and for being a client!
Good news overall with much progress.
The first question that comes to mind is how long can they cap the tracheostomy for?
If they can cap the tracheostomy for 48 or 72 hours and your dad is breathing, swallowing, coughing, talking and oxygen levels are within normal limits I can’t see why they couldn’t remove the tracheostomy.
Does he still need suction?
The wound/pressure sore and VAC dressing are a concern, however, it is not a criteria to stay in ICU or step down ICU.
A pressure sore should never happen in the first place and is a sign of poor nursing care, unfortunately.
RECOMMENDED:
As you mentioned, now that he has come thus far, he should have the tracheostomy removed and go on to neuro-rehabilitation and not to LTAC, let alone palliative care.
Kind regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!