Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad is Critically Ill in the ICU & Why Are They Pushing Him Out of ICU So Fast?
You can check out last week’s question by clicking on the link here.
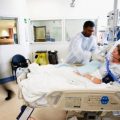
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I want to answer questions from one of my clients, Ashanti, as part of my 1:1 consulting and advocacy. Ashanti’s dad is a long-term ventilated patient in ICU and the ICU team is hesitant to proceed with further treatment for her dad. Ashanti is asking if the ICU team is limiting treatment for him.
The ICU Team is Hesitant to Proceed with Further treatment for My Dad? Are They Limiting Treatment for Him? Help!
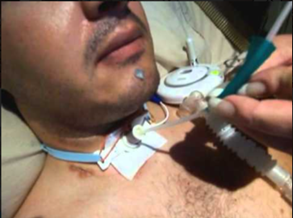
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hi Ashanti,
Thank you for your response.
Anyway, with regards to your last email regarding your dad’s pressure sore.
By this time, the issue with your dad’s delayed wound healing despite treatment with a wound vac, and routine wound care with debridement, should have been addressed already. The wound care team needs to be looking at other causal factors or contributing causes for this.
Here are a number of things that can delay or complicate the healing of wounds, including:
- Diabetes mellitus
- Low HGH (human growth hormone)
- Rheumatoid arthritis
- Vascular or arterial diseases
- Zinc deficiency
Again, the involvement of the whole team, including the doctor, nurse, therapists, patient care technician, and dietitian will help get the wound better for your dad.
And, yes, Ashanti, as I have mentioned before, it is indeed concerning, particularly your dad having a STAGE 3 pressure ulcer as you have stated before and that it needs to be treated or have it improved at least before he even gets discharged to prevent any occurrence of possible infections.
You can communicate with the wound care team and ask for their treatment plan for your dad’s pressure ulcer discussing the healing progress of the wound with them would also be beneficial but making sure that they are really doing something about it.
Regarding your question: “Also with regards to de-cannulation if any patient has problems afterwards can they be re-cannulated easily. Any risks/complications associated with it.” The doctor is the one who can assess that. Different patients have different concerns. You can have your dad’s doctor discuss this with you as well.
We hope this information helps.
For any further questions, please don’t hesitate to ask.
Thank you.
Kind regards,
Patrik
Hello Patrik,
It’s been a few weeks since my last email. In the meantime, hospital case management and hospitalists have pressured me to find a nursing facility as part of discharge planning. They have mentioned that his pressure sore which is level 4 might not heal and he has to leave the hospital with it and wound vac and continue further. They also mentioned that he doesn’t need any further medical care. This is not acceptable to me and voiced my concern. Also, they are very hesitant on decannulation simply stating that he has a high risk of aspiration.
As mentioned before in my emails. He was capped for more than 3 weeks without any issues and now he has slight congestion and is doing some saline humidification through his trach tube for this week. No regular suctioning and no other areas of concern. They are not trying decannulation and are adamant. Is this good medical practice?
Sometimes I feel helpless and have to let them know what they have to do next.
Awaiting your response.
Thanks & Regards
Ashanti
Hi Ashanti,
Thank you for sending us an email again and sharing your dad’s current condition.
With regards to your dad’s tracheostomy, as mentioned before, if they can cap the tracheostomy for 3 weeks and your dad is breathing, coughing, swallowing, talking and oxygen levels are all acceptable, I wonder why they can’t remove the tracheostomy.
However, now that your dad’s pressure sore progressed to stage 4, these wounds need immediate attention, as this may possibly also need surgery.
Stage 4 ulcers are the most serious because these types of sores extend not just below the subcutaneous fat but deep into tissues like muscles, tendons, and ligaments. In more severe cases, they can extend as far down as the cartilage or bone and there is definitely a high risk of infection at this stage.
Though, yes, pressure sores may not be a good criteria to stay in the intensive care unit (ICU) or stepdown ICU but Stage 4 pressure ulcer definitely needs medical attention.
You can always discuss these issues with the doctors and ask them about their treatment plans.
Keep us updated on your dad’s status.
Thank you.
Kind regards,
Patrik
Hello Patrik,
It has been 10 days now since he has been moved from Neuro ICU to a regular Med-Tele Step-down unit. He was capped on the trach tube for more than 3/4 weeks afterwards. Recently he got some congestion and is now on saline humification. As mentioned earlier, he had 98 -100% O2 saturation, swallowing, coughing is okay, breathing on room air, and speaking is okay. Not sure why they are delaying decannulation.
Pressure sore had been at this level from the beginning. It seems to have not worsened. Dimensions are 4.2 x 7 X 2.6 cm
They are taking pictures every week to track progress.
Please share your thoughts as to my stance to remain put at the hospital and not budge to case management and hospitalists pressuring to discharge my father to a long-term nursing facility in this condition.
Thanks & Best Regards
Ashanti
RECOMMENDED:
Hi Ashanti,
Your dad really made good progress in terms of his oxygenation status. They should take the next step of trying to decannulate your dad while he is still in the step-down unit so they can still further monitor and assess his overall tolerance without the tracheostomy and if he will further develop any signs of respiratory distress. They should consider decannulation in the stepdown unit where this current clinical setting can safely support his decannulation process.
Also, it will be much better for your dad to be managed without the tracheostomy if he will be transferred out. And should he be discharged, he needs to go to neuro-rehab so he can still receive the appropriate care and treatment from the skilled health care team given his medical condition, not to long-term acute care (LTAC) or palliative care.
In terms of his pressure sore, as far as I have reviewed past notes, I got the information from your prior email where you stated, “He also has Level 3 pressure sore on his tail bone of the size of 7x5X2.5 cms. for which they are doing wound care /wound vac.”
Stage 3 or 4 is still definitely a concern but can’t be a criterion for a step-down unit stay. However, this is a result of your dad being previously critically ill with poor nursing care. Given this fact, they should exhaust efforts, at least in improving your dad’s pressure sore and not to further develop any infection.
Hope this helps.
Kind regards,
Patrik
Hello Patrik,
In another development, today afternoon my father seemed to have pulled out the trach tube by himself as per nurses.
They seem to have covered the trach tube hole and are monitoring his oxygen saturation. So far, it’s been good.
Is he on a good path based on continued monitoring of his respiration/oxygen levels and other vital parameters?
Please let me know how his care needs to be going from here in the coming days and weeks.
Thanks & Best Regards
Ashanti
Hi Ashanti,
Thank you for emailing us again.
Following your dad’s unplanned decannulation, your dad requires close monitoring to identify signs of unexpected airway compromise. They need to monitor your dad’s respiratory rate, heart rate, oxygen saturation, color and work of breathing.
Immediately report any episodes of increased/decreased respiratory rate & heart rate, oxygen desaturation, increased work of breathing, restlessness/anxiety, color change or cyanosis & failure to clear secretions & gagging.
Following the first 24 hours post-decannulation:
- Your dad needs to stay in the ward to be further assessed by the medical team to have a “safe airway”. The average hospital length of stay post-decannulation is 36 – 48 hours but may take longer if clinically indicated.
- Encourage usual activities to assess exercise tolerance – may consider exercise testing/respiratory function tests
- Encourage coughing to clear secretions from the upper airway if required. Involve the respiratory therapist/physiotherapist for support.
- A follow-up to the speech pathology/swallowing team should be considered if your dad does not resume normal voice production following decannulation or with inadequate swallowing.
Hope this information helps.
Thank you.
Kind regards,
Patrik
Suggested Links:
Hello Patrik,
Subsequent to my dad’s accidental decannulation by himself three days ago. He is being given breathing treatment as he has some kind of wheezing/congestion in his airway. His oxygen saturation levels have been good around 96%-97% throughout after decannulation. Yesterday he was in some discomfort as he was feeling very itchy on his left side. Only after me letting them know and they changed the sheets, cleaned him up, and repositioned him. He seemed to be a little better after giving him some Benadryl (antihistamine) apart from hydroxyzine every 8 hours. Today he seemed to be better than yesterday in terms of itching.
Yesterday, I noticed he had some good coughs though not very strong after his breathing treatment using some mucus thinning medication.
Today one of the hospitalists called me and mentioned to me that they are continuing to monitor him and give breathing treatment. If he seems to be very congested, they have asked my permission to intubate him and put him on ventilator support. Is this the right path of treatment? For this had questioned them whether he cannot be re-cannulated as he was just decannulated three days back. For this, they consulted with the pulmonologist and replied no.
This is like going two steps back after making this much progress. Makes me concerned. Awaiting your reply and advice at the earliest in this regard.
Thanks & Best Regards
Ashanti
Hi Ashanti,
Decannulation failure may be apparent within 48 – 96 hours, and a stoma that has not fully closed may have the possibility of being reopened if deemed safe and necessary.
The pulmonologist/ENT team/RT should come and see and assess your dad’s tracheostomy stoma and his overall status if he can be safely recannulated back with the trach tube.
Tracheostomy tubes that have been in place for more than 7 days can usually be reinserted and placement confirmed with fiberoptic inspection of the airway following the accidental decannulation.
They can either use:
- Tracheal dilators to have a good visualization of the stoma
- Exchange device
- Bougie/Cooks airway exchange catheter/guidewire/introducer
- When inserted via the stoma into the trachea will guide the tracheostomy tube into the correct position.
- Cannulation with a smaller tracheostomy tube. Following a failed attempt to reinsert a tracheostomy tube of the same size, a tracheostomy tube one size smaller may be easier to insert. It should be remembered that this will result in a narrowed airway and your dad should be monitored accordingly.
However, this is important to know that repeated attempts at recannulation may cause trauma to the stoma and trachea. Hemorrhage and edema may further compromise your dad’s airway making further attempts at cannulation more difficult. Care must be taken to avoid unnecessary trauma.
**If after a failed attempt at recannulation, priority must be given to maintaining oxygenation.
** If attempts at recannulation are unsuccessful, oral intubation may be required to secure your dad a patent airway and maintain oxygenation.
Otherwise, they can continue with giving nebulizers to your dad, give oxygen support as needed, clear his secretions, perform chest physiotherapy and closely monitor your dad’s hemodynamics.
Keep us posted with your dad’s current health status.
Thank you.
Kind regards,
Patrik
Hello Patrik,
As mentioned in my previous email that my father had decannulated a couple of weeks back accidentally by himself. They were monitoring his respiration afterwards. He was having some congestion for the past week and had been given nebulizer treatment. As per doctor, yesterday morning he had her oxygen saturation coming down and he was put on BIPAP ventilation.
He is doing okay on pressure support at 30% oxygen. Will attach a photo subsequently. His oxygen saturation is good 98-100%. They have taken chest X-rays taken and show slight improvement. The hospitalist called me earlier and mentioned that the next step would be intubation if the condition worsens. He is hemodynamically stable on BIPAP (bi-level positive airway pressure) support.
Concerned about this situation. How long would they do the BIPAP ventilation before they take the decision on the next step? He seems to have some fluid on his lungs, and they are giving him medications (diuretics). He seems to be comfortable.
The Doctor who attended seemed to be very pessimistic and asked me whether to continue with all the medical practices going forward as well. I confirmed yes to it. Couldn’t understand why they are hesitant to proceed with further treatment and betterment. They are mentioning that there wouldn’t be any improvement on his condition going forward.
Also, they have stopped tube feeding citing aspiration risk of his lungs due to burping/reflux. My concern is that his nutrition would be very affected. He did not have any such issues so far. Please share your advice as to how this could be approached. I am not convinced with their approach.
Awaiting your replies.
Also, I have attached a picture of the BIPAP settings for my father as taken yesterday for your reference.
Thanks & Best Regards
Ashanti
Recommended:
Hi Ashanti,
Thank you for updating us on your dad’s current condition.
Your dad is currently on minimal bi-level positive airway pressure (BIPAP) setting: FiO2 30%, inspiratory positive airway pressure (IPAP): 12; expiratory positive airway pressure (EPAP): 7, Rate: 4. While your dad is on BIPAP, please take note of these points:
- Apart from the routine nebulization for your dad, the respiratory therapist needs to be involved and perform routine chest physiotherapy (CPT) for your dad to improve his lung function and help him breathe better. What good about chest PT is that it expands your dad’s lungs, strengthens his breathing muscles, and loosens and improves drainage of thick lung secretions which can then support and further improve his oxygenation status.
- Your dad can continue with BiPAP ventilation if he has a good response to it like maintaining above acceptable oxygen saturation without any signs of respiratory distress like increased work of breathing, increased heart rate or altered mental status. An arterial blood gas will be needed as well while he is on BiPAP to assess his response to therapy.
- They can seek specialist respiratory input (pulmonologist/respiratory therapist) with regards to the duration of therapy and weaning if seen possible.
- Another important note, BiPAP can reduce cardiac output and cause hemodynamic instability, so it is important to monitor your dad’s pulse and blood pressure closely, his overall condition. You’ve mentioned about having some fluid on his lungs and they are giving him diuretics. Though he seemed to be comfortable with it, your dad still needs to be monitored closely. Questions to note: Have they discussed with you the reasons why your dad has fluids in his lungs? Have they started him on any prophylactic antibiotics? Any episodes of fever? Any recent blood works done for him?
- You also mentioned that “they have stopped tube feeding citing aspiration risk of his lungs due to burping/reflux”. Well, one thing I see also on this is that, while your dad is on BiPAP ventilation, and while in the course of monitoring his response to therapy, they are thinking of potential intubation as his condition worsens.
- And now that they have stopped the feeds and giving him diuretics, this predisposes him more to a potential risk of electrolyte imbalance (low Potassium, Sodium, Calcium, and Magnesium) that could further aggravate his condition especially since your dad has cardiac issues. They need to monitor this aspect as well. They also need to monitor fluid balance and give IV fluids or start Total Parenteral Nutrition as necessary.
- Normally, if BiPAP ventilation fails for your dad between 24-48 hours and he continues not to improve despite other therapeutic measures and management, they should not wait for him to deteriorate further and so they need to escalate to intubation.
Keep doing what you do Ashanti for your dad. You are on the right track, and we are here to advocate for you. Doctors are always like that. They will discourage you and even push you to limitations of treatment for your dad, but you can always defer them and exercise your right to be heard of what you think is right and good for your dad.
Keep us updated.
Hope this helps.
Thank you.
Kind regards,
Patrik
Hello Patrik,
My dad has been on Nephro 1.8 formula for tube feeding as his potassium came out high due to lab work. It’s already been a long time since he was on the other high-protein formula.
Is this the right approach? What about the nasogastric tube (NGT) and Dobhoff Tube (DHT)? Can you tell me something about it?
He also has diarrhea stools.
Please advise.
Thanks & Best Regards
Ashanti
Hi Ashanti,
Your dad’s current nutritional needs should be assessed by a registered dietician/nutritionist. They will be able to determine which type of feeds your dad needs as his current condition dictates. They can look over the result of your dad’s current blood works (serum electrolytes, renal profile) to thoroughly assess which type of formula they need to give your dad. Protein needs will be estimated as well by a registered dietician and estimated protein needs should be adjusted according to the severity and type of illness. Shifting to the Nephro formula may have something to do with it.
Regarding NGT (Nasogastric tube) vs DHT (Dobhoff tube) for enteral feeding:
A nasogastric tube is a special tube that carries food and medicine to the stomach through the nose. It allows delivery of nutritionally complete feed directly into the stomach; or removal of stomach contents.
A Dobhoff tube is a narrow-bore flexible tube with a diameter of 4 mm, used to deliver enteral nutrition. Unlike nasogastric tubes, which can be used for gastrointestinal drainage, suction cannot be applied to a Dobhoff tube, limiting its use to enteral feeding and medication delivery.
Dobhoff tube is a small-lumen feeding tube that can be advanced into the duodenum. Drieling tube a double-lumen tube having a metal weight at one end to carry it past the stomach into the duodenum. At the other end are two tails, one used to collect gastric specimens and the other to collect specimens from the duodenum.
Dobhoff tube delivers meds and fluids, nasogastric tube provides suction to decompress (can also deliver meds/fluids); nurses place NGT while doctors (and ICU nurses) place Dobhoff tube.
For the potential causes of tube feeding and diarrhea, there may be some medications that can lead to diarrhea. Also, gastrointestinal infections can irritate the intestine and also lead to watery stools. Furthermore, formula contamination caused by improper handling and storage can also induce diarrhea.
Sometimes diarrhea also occurs during tube feeds if the feeds have been given very fast. So, they need to slow it down while giving feeds.
The doctors need to look if any of your dad’s medications could contribute to loose or watery stools. Sometimes changing the form of the medication comes in can help. It is also important that before giving feeds, they need to perform good hand-washing, wash all equipment with warm water and check formula expiration dates. Use one feeding bag for no more than 48 hours and hang the formula for no more than eight to 12 hours.
Also, if your dad has frequent bouts of stool, it needs to be referred to the doctors right away to prevent dehydration and to manage it appropriately on a timely basis. They can take a stool sample as well for culture to rule out any infection.
Hope this helps.
Kind regards,
Patrik
RECOMMENDED:
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!