Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy.
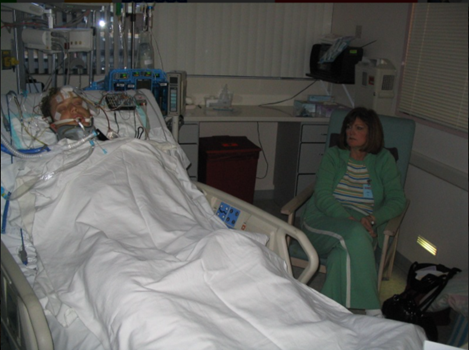
Ashanti’s dad is in ICU with a stroke & is on a ventilator. Ashanti is asking how long does it take for her dad to be weaned off the ventilator.
My Dad is Critically Ill in the ICU & How Long Does it Take for Him To Be Weaned Off the Ventilator?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hi Ashanti,
He will only be able to come off the ventilator if he can breathe spontaneously.
The ventilation mode before extubation is called CPAP (Continuous Positive Airway Pressure) or pressure support.
Keep asking for the following:
– What is the ventilation mode?
– What is the ventilator PEEP (Positive End-Expiratory Pressure)?
– How much pressure support is he on?
– What are his tidal volumes?
– His minute volumes – the volume of air that can be inhaled (inhaled minute volume) or exhaled (exhaled minute volume) from a person’s lungs in one minute.
– What is his ventilator’s FiO2 (Fraction of Inspired Oxygen)?
– What is the result of the most recent arterial blood gas?
– Does he have a good strong cough?
– How frequent are they suctioning him?
– Is he obeying commands?
For further reading and as a guiding article/video, you can click on the link below from our website at intensivecarehotline.com:
HOW TO WEAN OFF VENTILATION AND TRACHEOSTOMY STEP BY STEP!
Kind regards,
Patrik
Hi Patrik,
As per a brief phone discussion today with one of the nurses in the ICU. She mentioned that his ventilator mode is PRVC (Pressure Regulated Volume control). Other parameters are as given before in my previous email.
Positive End Expiratory Pressure – 6
Fraction of Inspired Oxygen- 35 %
Respiration Rate – 16
Tidal Volume – 400
Couldn’t get the minute volume as the nurse was not in his room. Currently he seems to be not responsive to any commands and only to pain stimuli movements. So, coughing might not be good enough.
As per nurse on duty, today he did undergo spontaneous breathing trial (SBT) and could last only for about 20 minutes before back on ventilator support.
He is hemodynamically stable. No fever. On his regular medications.
Thanks & Best Regards
Ashanti
Hi Ashanti,
As mentioned, as long as he is in a controlled mode, he won’t be able to come off the ventilator.
An arterial blood gas while he is on a spontaneous breathing trial would help to determine how far away he is from having time off the ventilator.
Any questions please let me know.
Regards,
Patrik
Hi Patrik,
Thanks Patrik.
Does arterial blood gas parameter show up on the ventilator? Or its through a separate instrument needed? The intensivist doctor did not answer me properly last time.
Not sure if he is making good progress on his spontaneous breathing trials (SBTs)? Weaning process in his case might take longer. It’s preferable to be in a hospital setting if he is in the weaning process, right? Is it better to talk to a pulmonary technician or doctor about the weaning process in his case?
I have a feeling that they are less inclined about weaning him and removing COVID restrictions than keeping his vitals stable.
Let me know your thoughts.
Thanks & Best Regards,
Ashanti
Hi Ashanti,
Per your last email, arterial blood gas results cannot be seen on the ventilator.
Arterial blood gas is a blood test to determine the current oxygenation/ventilation status of your dad which is important for weaning and they are using a separate machine to get the result of that.
You can have a look at this article to know more about Arterial Blood Gas (ABG):
https://intensivecarehotline.com/questions/what-is-an-arterial-blood-gas-test-abg/
Definitely, you can ask the respiratory therapist, nurse, or doctor if your dad is already in the weaning process. They need to explain to you what progress your dad is making with the weaning process.
For any further questions, please let me know.
Thank you.
Regards,
Patrik
RECOMMENDED:
Hi Patrik,
My father has been in intensive care for the last 17 days. He was diagnosed 20 days for covid and treated initial 4 days for the same. As you know that he had a brain hemorrhage and is on a ventilator with tracheostomy and feeding tube for the last 17 days. They had mentioned they would be de-escalating to move him to the non-covid Intensive care Unit (ICU) tomorrow.
They have been trying to wean him off the ventilator for the last week or 10 days. He made some progress. 2 days he did with continuous positive airway pressure for 6-7 hours before back on the ventilator and yesterday could last for only 4 hours. My father also has atrial fibrillation, and his heart rate was higher, so they did not do his spontaneous breathing trial (SBT) today.
Doctors would have a meeting with me tomorrow to discuss further steps toward discharge. Not happy if they are talking about discharge now. He had not completely weaned off his ventilator. Though he is minimally conscious want him to be weaned off in the coming weeks before thinking about discharge.
Please address my concern as to how to deal with this situation as he seems to progress in the right path under medical observation. His secretion management also needs to be kept in my mind apart from consciousness and ability to follow directions. They have not done much in terms of neurostimulation or physical therapy yet.
Awaiting your reply. We can talk briefly tonight as per our availability.
Thanks & Best Regards,
Ashanti
Hi Ashanti,
I hope this email finds you well.
With regards to your email:
It’s good if he will be transferred into a non-COVID ICU as he still needs ICU care.
Your dad was able to be weaned from the ventilator for the past week but needs continuous monitoring of his tolerance to that. They need to do arterial blood gas tests, and chest X-ray, and monitor him clinically overall to determine if he is tolerating the weaning process and be ready to completely come off the ventilator.
With regards, to his atrial fibrillation (Afib), have they sought any cardiac consultation for his Afib? That needs to be addressed as well.
He definitely needs to be stable first and eventually come off the ventilator before they talk about discharge.
Secretions need to be managed as well. How frequent are they doing the suctioning for him? What is his current Glasgow Coma Scale? And yes, he needs to start mobilizing, he needs to get physical therapy to get his function back. This can be a long process, but the sooner he can start, the better.
Your dad needs to be assessed well if he is really a candidate for weaning off the ventilator, taking into account, reviewing his clinical improvement with his oxygenation/ventilation status, mental status, secretions, and cardiovascular stability.
If they will persist in discharging your dad soon, you can definitely say “no” if he had not met the criteria.
Regards,
Patrik
Hello Patrik,
Thanks for your replies. More answers and other questions/clarifications below your comments.
He has been hemodynamically stable during his stay in ICU after his initial treatment and care. He is on blood pressure medications and also to control his atrial fibrillation. He had been hypertensive and diabetic for the past 2 decades. Weaning I would say with moderate progress. Some days he could tolerate it better than others. His kidney function has also been monitored and a diuretic (40 mg daily) has been given through IV.
Based on his current level of progress my guess it would take weeks to come back to say 80% of his regular breathing as a conservative estimate.
Question: Does he need to be in an ICU until he is on ventilator support? Can the weaning process happen in a non-ICU setting if he is say 50 % of the time on mechanical ventilation?
Please address my concern as to how to deal with this situation as he seems to progress in the right path under medical observation. His secretion management also needs to be kept in my mind apart from consciousness and ability to follow directions. They have not done much in terms of neurostimulation or physical therapy yet.
Have to check on his current suctioning interval. He might be on 5 or 6 on Glasgow Coma Scale. Opening eyes only to pain/other physical movements. Left side paralyzed. Movement on right side arm and leg to pain stimulus.
Yes, it appears to be a slow and long process. The hospital environment and monitoring are much better in his case. Nothing much done so far on rehab/physical/audio therapy of any sort.
Having a concern that they might simply prematurely conclude/put pressure that it would be difficult to wean him off due to his health status and he has to be discharged with ventilator support and tube feeding to long-term nursing care with palliative care. I can say no but will they listen towards it?
On top of all these, recently 3 days back I came to know that he has a palm-sized wound on his back due to laying down on his back. This is being attended by the wound care team. This might take weeks to heal fully.
I felt it was negligence on their part. Cannot talk about discharge in this condition. Want to remain strong on this matter as it’s unreasonable and not medically sound.
Let me know.
Thanks & Best Regards
Ashanti
Suggested Links:
- The 10 things you must know about ventilation & tracheostomy weaning in intensive care- live stream!
Hi Ashanti,
The pressure sore is very concerning and potentially negligent.
I agree that they need to take ownership of their potential negligence and not send him somewhere you are not feeling comfortable with.
What are they doing with the wound?
Is he on a vacuum-assisted closure (VAC) dressing?
Kind regards,
Patrik
Hello Patrik,
Today, I met with his hospital case manager and critical care specialist. Also, today was the date they allowed me to visit and see him from behind a glass door. He would be de-escalated to a non-COVID ICU due to being 20 days from his COVID admission to the hospital. Also, his bio inflammation related to COVID coming down.
They have a wound care team to address his wound. They are using some kind of natural honey to treat it. This was reported to me 3-4 days back. Not sure how long it would take to heal considering he’s being in the bed most of the time. At least they are addressing it now.
He was on CPAP (continuous positive airway pressure support) for 6 hours today before they put him on ventilator support. This is a slight improvement from 3-4 hours from a few days ago.
What do you think?
But the ICU doctor was pessimistic and kept saying that he is on a higher pressure support and he cannot wean off the ventilator as his brain function damage due to hemorrhage is irreversible. I feel that he is making little progress while being hemodynamically stable.
They seem to rush to conclusions instead of looking at the positives. His secretions need attention like 1-2 times during the day time and 2-3 times during the night.
If I am able to go and visit his going forward can take picture of his ventilator settings as well.
They also wanted me to plan for his stay and care after discharge from the hospital. For which I mentioned that they can send to me but we are far away from discharge.
Your thoughts on these please.
It’s difficult to remain positive and optimistic when they give these scary comments.
Had also asked about his brain CT scan and whether it has shown any improvement. The doctor kept on saying how difficult is his situation to wean him off the ventilator.
Also insisted on therapy of any sort, which they are minimally providing if not anything.
Awaiting your thoughts as to how to proceed from ICU care, regular hospital care, and then to external long-term care.
Thanks & Best Regards,
Ashanti
Recommended:
Hi Ashanti,
What is his current Glasgow coma scale?
Even though he’s breathing on CPAP or pressure support, if the CPAP or pressure support is too high, he won’t be able to come off the ventilator.
Pressure support needs to be less than 8-10 with good sustainable tidal volumes, minute volumes, oxygen saturation levels, good arterial blood gases, and normal breathing rate.
A picture of the ventilator would be great!
Arterial blood gas results would be great!
Hospitals will continue to be negative by default because they are managing their liability.
After you provide more clinical details, I.e. ventilator settings, arterial blood gas, Glasgow coma scale, etc… I will advise you of the next steps.
Regards,
Patrik
Hi Patrik,
Thanks Patrik.
From what the nurses had mentioned to me he is mostly in 5 or 6 in Glasgow coma scale (GCS). Will try to get a picture of his ventilator settings as soon as possible. Try to get arterial blood gas results as well. He seems to tolerate it for hours before going low on oxygen saturation. Is this normal during the weaning process?
I am kind of surprised, mildly shocked, and concerned to know about his wound on the tailbone area 4 days back from a nurse and this seems to be hospital negligence even in ICU care.
Thanks and regards,
Ashanti
RECOMMENDED:
Hi Ashanti,
It’ll be difficult although not impossible for your dad to come off the ventilator with a GCS (Glasgow Coma Scale) of 5 or 6.
Please get a picture of the ventilator and arterial blood gas results so we can see and review them. These are important parameters to know if he is tolerating the weaning process and hopefully to get him off the ventilator.
Pressure sore stage 4, I would argue is hospital negligence and that should never happen!
Please keep us updated.
Kind regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!