Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
When is The Best Time to Remove the Breathing Tube of My Critically Ill Dad in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Irene, as part of my 1:1 consulting and advocacy service! Irene’s dad is with a breathing tube and on a ventilator in the ICU. Irene is asking why the ICU doctor tells her to just let her dad pass away.
Why Does the ICU Doctor Tell Me to Just Let My Dad Pass Away? Help!
Patrik: So mobilization is inevitable. I know the first couple of weeks in ICU people don’t necessarily get mobilized because they’re too critically unwell. But as soon as you can mobilize, you need to mobilize. Now the Levophed that you mentioned earlier, or the norepinephrine depending on the dose might stop him from being mobilized. That could be a contraindication depending on the dose. But as soon as that’s off, there shouldn’t be anything stopping him from mobilizing. And it will help him with expanding his lungs, it will help him with cognition, it will help him with everything.
RECOMMENDED:
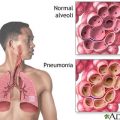
Irene: Matter of fact, last year when dad was in their ICU… And the bad thing happens, as he’s brought in the ICU the doctor took over and he looked at me, dad had this pneumonia, sepsis issue. It was these secretions flooding his lung and the doctor says; “Oh, Irene, why don’t you just let your dad pass away?” And I was very calm as a cucumber. I just turned I looked out the window, composed myself, turned around and I was wearing a mask. And I said, “Doctor let’s get my dad out of this bed and put him in a cardiac chair and see how he does”.
Patrik: Yep.
Irene: And within two hours he was giving the staff high-fives with his hand. And then they all started coming in there and he was kicking their hands with their toes.
Recommended:
Irene: So this two hours ago and they were wanting to shut him down. And I said no, I know how dad recovers. He’s got these back fractures, his spine, this compacts his lung. If you stretch him out tighter and you get him tight and snug in that cardiac chair, put pillows and keep him in there minimum eight hours a day. It might seem like torture but just put extra pillows around him and keep him warm, he’ll start kind of getting used to it. And his lungs were kind of stretching out and he’ll start getting better. That’s what started happening.
Patrik: Absolutely. So you can already see I’m preaching to the converted here already. So you can already see what needs to happen. You can already see, but I know that a lot of ICUs are complacent, especially at the moment with COVID. They’re all under the pump. They’re under the pump in normal times let alone at the moment with COVID, but it shouldn’t stop them from doing what needs to be done.
Irene: Right.
Patrik: Definitely not. Irene, I am pressed for time.
Irene: Okay.
Patrik: I am very, very sorry. What you can do is… I’ll send you the consulting and advocacy options. If you do want to get on a call with me and the doctors, we can definitely arrange that or with the respiratory therapist. What I always advise, if you do nothing… There’s so much information on our website. If you spend enough time on our website you get all the information you need, but obviously the shortcut is to talk to me.
Irene: I want you involved. Definitely.
Patrik: Okay. All right. Look, I’ve sent you the options earlier. If you want to proceed, just let me know.
Irene: So how soon can you get involved with the…
Patrik: How soon do you need me?
Irene: I would say talking to the doctors today would be helpful because they’re contemplating doing this extubation procedure. So it might be a good, good thing to talk to them before tomorrow.
Patrik: Okay.
Irene: Yeah. Right.
Patrik: Why don’t you ask them how quickly you can get onto them, or do you know already?
Irene: I was already onto both of them. I spoke to the neurologist just now. Then, I spoke to the critical care doctor earlier this afternoon already.
Patrik: Right. Okay. So is it as simple as you ringing them up and saying, yep, I want to talk to you. Is it as simple as that?
Irene: Typically, you have to call the nurse and tell them to page the doctor kind of thing. And depending on their availability I’ll get a call at some point. So I just keep the phone line open and I’ll wait until they call.
Patrik: I see. Okay. All right. Look, I probably can be available, you know? I mean, what’s the latest you think you want to have that call with them today? What’s the latest?
Irene: I’m not sure what their duty schedule is but they’re on all week.
Patrik: Yes.
Irene: Both the critical care doctor and the neurologist. They’re both on, all week. Whether they’ve left the hospital already today, I don’t know.
Recommended:
Patrik: Yeah, sure. Look again as I said, I can be flexible. If you want me there, you want me there? Do you think a zoom call can be arranged with them or would it be over the phone?
Irene: That’s a good question. Because normally on zoom they just put the zoom next to him so I can see him for an hour.
Patrik: Yep.
Irene: But something new is going to be tried tomorrow at 5:00 AM. They’re going to have this trial with the RT and I’ll be on zoom then, so I can ask the RT questions. I haven’t been able to ask the RT any questions, but usually it’s on the phone with the doctors. But we might be able to do a zoom, if it’s discussed I can tell them I can do a zoom if possible.
Patrik: Yeah. Look, I think the next step is really… You could book an hour with me or you can select from the consulting options and then you can organize a call with them. We should probably look at that as a next step.
Irene: Okay.
Patrik: Okay. All right. Look, I need to go. I’ll wait to hear from you.
Irene: Yes sir.
Patrik: Okay. All right. Thank you so much.
Irene: Thank you.
Patrik: Thank you. Take care. Have a good day. Thank you. Bye.

Patrik: Hi Irene.
Irene: Hi Patrik.
Patrik: Looking from the outside it’s very concerning what we see just in the news with COVID.
Irene: Worried about the new variations that are starting up, the variation.
Patrik: Yes. Yeah. So, with regards to your dad. So, from doing a tracheostomy, or not doing a trach, any ideas why?
Irene: The doctor wanted to do a… He was telling me to do a trach and he was commenting about dad’s paperwork that he filled out with his wishes a few years ago, he signed that I want all life treatment. So he brought that up he says if we’re going to give your dad full treatment, and he wants to live as long as he can we need to do this trach. And that was the comment that the doctor made. And then an hour later I get this odd call from his management, and social worker, two ladies, and they said the hospital’s not going to do a trach, and your dad’s going to have to go to another facility which is going to do supportive care.
Patrik: Right. Supportive care meaning… It sounds to me like hospice care?
Irene: I think they will leave the-
Patrik: The breathing tube.
Recommended:
Irene: Breathing tube in the mouth the way it is, and they will just keep a breathing machine on it. That’s what I guess supportive care would be, and a feeding tube.
Patrik: Doesn’t make a lot of sense because the breathing tube has a limited life time. It should be no longer than two weeks. Having said that at the moment we are seeing delays because of COVID, we are seeing delays, but outside of COVID breathing tube is sort of the two week mark and then you should proceed to a trach if you can’t wean someone off the ventilator. And what is this other facility? Do you have any information there?
Irene: The comment was you’re going to have to find him another facility or something like that.
Patrik: And on what grounds… Is that some… On what grounds… Just to help-
Irene: I didn’t respond to anything that he said. I just responded to the fact that is this the meeting that you were trying to have with me that has been postponed, I say the meeting is not now, the meeting will be by next week, it’s been postponed and I cannot comment. Goodbye and I hung up.
Patrik: Right and what is this issue? When I read through your email, that your dad is a full code status as per advanced care directive, and you need to make a decision, what do they want you to make a decision about?
Irene: The tracheostomy.
Patrik: Okay. But there was no pressure from them that you had to make a decision about a DNR, because the way I read your email is that they wanted you to sign a DNR?
Irene: No.
Suggested links:
Patrik: No. Okay. Okay so that was-
Irene: It’s well known he’s full code.
Patrik: Okay. Okay. Have you spoken to a doctor or a nurse in the last 24 hours about your dad’s ventilation situation? Do you know how he’s ventilated?
Irene: Yes. I talked to the doctor. He’s the attending doctor of my dad by the way. He’s the intensivist that’s attending to him and he said basically dad has been about the same, he did get into the parameters on the ventilator the other day. And I asked her a few questions about what those numbers were, they looked actually pretty close to him being safe to be extubated, if I recall right.
Patrik: Can you share some of that?
Irene: I think I can find my… It’s on a margin here on the side I wrote… Let me see… right here. Yeah there’s like the FiO2, and the other one-
Patrik: Yep. Yep.
Irene: Okay. Yeah. Okay so here are the numbers on the other day, the tidal volume was at five, FiO2 was at 25.
Patrik: Yep. Tidal volume can’t be five Irene, can’t be five. Because that’s five-
Irene: No. No. I think that’s the PEEP.
Patrik: PEEP. Yeah, absolutely.
Irene: Yeah. That’s the PEEP. Tidal volume was 300 millimeters, Right?
Patrik: Yep.
Irene: Okay. And then FiO2 was 25%.
Patrik: Yep. And do you know what ventilation mode?
Irene: Oh, I know he breathes over the ventilator, I’ve been told.
Patrik: Okay. Okay. Okay. Okay. So if that’s the case, in order to extubate someone, they need to initiate every single breath themselves. Right. So, if he’s breathing-
Irene: Yes. He initiates all single breath.
Patrik: He does?
Irene: Yeah. Apparently he does.
Patrik: Okay. Well that’s a good sign.
Irene: Yeah.
Patrik: That’s a good sign. Can you ask them if he’s breathing in CPAP or pressure support.
Recommended:
Irene: Oh, okay.
Patrik: Ask them, because if you’re telling me he’s breathing over the ventilator that is a bit of a mixed message for me in there. It’s either that he’s breathing on top of a set breathing rate or it could also mean he’s triggering every single breath himself, but if he’s triggering every single breath himself, it’s usually called CPAP or pressure support ventilation.
Irene: Okay.
Patrik: That is a very important question. Now what’s your father’s weight roughly?
Irene: Before he went in, he was in the 140s. I don’t know what he’s lost now, but he’s in the 140s.
Patrik: Okay. I just need to calculate that into kilos and I’ll tell you in a minute why. So that’s 140 pounds. Is it?
Irene: Yes.
Patrik: Just give me one sec. I just need that into kilos. And then I can tell you if the tidal volume is adequate.
Irene: Actually I say he’s probably like 135 because he was still recovering from last month’s ICU. So he wasn’t quite back to 140.
Patrik: Okay.
Irene: Let’s say 135.
Patrik: Yeah. That’s about 60 kilos, tidal volumes. Did you say 300?
Irene: 300 milliliter?
Patrik: Probably a little bit too low. You’re talking about 7 to 10 mls per kilo. 7 to 10 mls per kilo. So let’s just take 7 times 60 is about 400, 420. Anyway, look, it’s not the end of the world. The next question that is, okay, let’s just say he’s breathing spontaneously. Tidal volumes is 400 for argument’s sake, PEEP is 5. Oxygen is 25% and the arterial blood gases are good and he’s obeying commands. He should be ready for extubation. And he’s coughing.
Recommended:
Irene: He’s got good coughing. He yawns, he swallows. He gets red in the face because oftentimes secretions go down and his whole face turn red, red, red, and then he gets it down, and then the suction picks it up. That happens every three minutes, his face turns beet root red.
Patrik: Right. And he’s not obeying commands. I mean, we talked about Glasgow Coma Scale.
Irene: No, he’s doesn’t understand English. My dad is not literate.
Patrik: Yes. Yes. Yes, I remember that from your email. Yes.
Irene: I don’t know. That’s a good point at the big hospital there’s a couple of nurses that spoke to him in his language, but at this hospital, I don’t think there’s any that I know unless they come over from the main one. So you don’t get a lot of immigrants living in that area, more in the city like where my grandfather used to live.
Patrik: Right. I see. I see. So look, even if he’s breathing by himself with good tidal volumes and with good arterial blood gases if he doesn’t obey commands, their argument would be, he won’t be able to maintain a stable and safe airway. And I, I would agree with that.
Irene: Okay.
Patrik: Which then leads to a trach. He may be able to come off the ventilator, but he may still need the trach.
Irene: I see.
Patrik: If his Glasgow Coma Scale is seven, eight, there’s also the risk of aspiration. Do you know what I mean?
Irene: They’re worried about that the most?
Patrik: Yeah. I would be too.
RECOMMENDED:
Irene: He’s aspirated in the past. He’s aspirated many times in the past and he’s been to speech therapy, but it’s mostly because of his sinusitis. It coats the back of the epiglottis and the epiglottis gets sticky. And so when he swallows sometimes, and he’s tired, it’ll go down the wrong way. But it’s mostly aspirations from his chronic sinusitis and it comes back after he left the ICU. On the right side chest surgery on the sinusitis, and the big fungus were removed. But even after that there’s a layer of pus in the base of it, you see with endoscope and it was still there. And what would happen is, dad would sit and watch television in the kitchen table and his nose will start dripping. He’ll start sneezing. And it starts dripping more and more and more and the infection never goes away.
Irene: And when he go on bed and lay down and then it’ll go the opposite way down his throat and coat his trachea. And I would have to suction him at home sometimes four times a day. And I would suction him with a needle tracheal suction through the right nares using a 14 French. I would run the 14 inches, and as I’m pulling it back out, it would go really wild right here in the last three inches, right at the sinus opening and this fill up the sinuses, will just fill up the suction like three or four feet a white cloud repeatedly. That’s what’s going on with the infection. It’s a chronic fungus infection that we just can’t get rid off. And we just get into the cycle, he’s home for a month and then he develops it again. And the weather’s cold. He’d go back to the emergency room. That kind of thing.
Patrik: Yeah. Okay. So I feel like the sooner a trach the better on the one hand, on the other hand, I don’t know whether we discussed that on our last call. If they end up doing a trach, they definitely want to send him out then. Did we speak about that? I think we did.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!