Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Stop the ICU Team from Sending My Ventilated Dad to LTAC? Help!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ashanti, as part of my 1:1 consulting and advocacy.
Ashanti’s dad is in ICU with a stroke & is on a ventilator. Ashanti is asking why they are pushing her father out of ICU so fast.
My Dad is Critically Ill in the ICU & Why Are They Pushing Him Out of ICU So Fast?
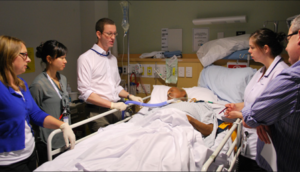
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ashanti here.”
Hi Ashanti,
Thank you for renewing your membership, thank you for your support, and for being a client!
Good news overall with much progress.
The first question that comes to mind is how long can they cap the tracheostomy for?
If they can cap the tracheostomy for 48 or 72 hours and your dad is breathing, swallowing, coughing, talking and oxygen levels are within normal limits I can’t see why they couldn’t remove the tracheostomy.
Does he still need suction?
The wound/pressure sore and VAC dressing are a concern, however, it is not a criteria to stay in ICU or step down ICU.
A pressure sore should never happen in the first place and is a sign of poor nursing care, unfortunately.
As you mentioned, now that he has come thus far, he should have the tracheostomy removed and go on to neuro-rehabilitation and not to LTAC, let alone palliative care.
Kind regards,
Patrik
Hi Patrik,
Thanks, Patrik, for your prompt reply.
Few clarifications regarding your email reply.
If they can cap the tracheostomy for 48 or 72 hours and your dad is breathing, swallowing, coughing, talking and oxygen levels are within normal limits I can’t see why they couldn’t remove the tracheostomy.
>> It’s been more than a week/10 days after they have capped the trach tube. They did not do much of the swallowing test/speaking test. His coughing is okay, and he does it with a bit of effort when needed. He is on a feeding tube (bolus feeding).
Does he still need suction?
>>Oral care is needed. Sometimes suction is needed, not always. As far as my observation he is doing okay and as per discussion with the respiratory therapist as well.
One thing that is a matter of concern from the doctor’s side is that he is not alert and awake from a neurological perspective and they mentioned that it’s a risk after decannulation if he is not able to manage his secretions and he will have to be intubated if situations worsen. Need your comments and advice on this specific area of concern. From my point of view, they did not try it in the first place.
Also, he is in this state of closed eyes with the occasional opening of eyes while repositioning every couple of hours and coughing etc. Is it a concern considering his severe stroke? They are giving him Provigil once daily in the morning to stay more awake /alert.
Today I got a call from one of the doctors stating that they can’t do much with his status and he would be discharged with trach tube or else palliative care. This is not acceptable to me.
The wound/pressure sore and vacuum-assisted closure (VAC) dressing are a concern; however, it is not a criterion to stay in ICU or step-down ICU.
>> His wound is not even 50 % healed. How can I discharge him out of a non-ICU considering the fact that the care outside the hospital would be much less compared to here? I don’t want any complications from it due to premature discharge. Is this not a serious thing to consider before discharge?
Planning to discuss this again with the pulmonologist about decannulation and go from there.
Let me know your thoughts.
Thanks & Best Regards
Ashanti
RECOMMENDED:
Hi Ashanti,
How are you, Ashanti?
We hope that you and your family are doing well.
Your dad had progressed really well, and it is indeed good news.
You mentioned about your dad, that it’s been more than a week/10 days after they have reduced and capped the trach tube, had been on room air for 2 – 3 weeks now without any significant issues or complications; requiring suctioning at times. Though, there is a concern about his neurological status that he is not alert and awake per neuro perspective.
With your dad’s current progress in terms of being able to tolerate capping trials, trach tube reduced, been on room air without any issues and minimal suctioning required, a bit of effort when coughing as needed. They should routinely continue with physical therapist (PT)/ occupational therapist (OT), undergo timely swallowing tests/speaking tests, and should try decannulation.
Yes, they have mentioned and know for a fact about the risk of decannulation if he is not able to manage his secretions and he will have to be intubated if the situation worsens. And so, it is but reasonable and justified that they need to try your dad to be decannulated now with all the expert people around to assess if he will be able to tolerate it before pushing him out. That should include as part of his treatment plan for someone who has a tracheostomy and with notable good progress as you’ve mentioned.
And yes, you can discuss these issues collaboratively with a pulmonologist/neuro/respiratory therapist about decannulation, let your dad be thoroughly assessed and go from there.
And should your dad be transferred, he needs to go to neuro rehab where he will be receiving appropriate care and treatment as his current condition warrants, not to long-term acute care (LTAC) or palliative care.
I hope this helps.
Thank you.
Kind regards,
Patrik
Hi Patrik,
Thanks, Patrik, for your replies. Hope you and your family are doing well.
Will discuss with the pulmonologist and neuro doctor about the decannulation process considering his neuro and respiratory status. Since his trach is capped, is it not very similar to the removal of the trach tube as he is breathing through his nose and using his regular air pathway? Then, why are they scaring me about this next step as he would have respiratory distress and pass away? This is exactly what they need to try when being in the hospital. Hard to understand.
What about his pressure sore? From what I could see through the wound pictures, it’s not even 50% healed after weeks of wound vac and care. This had happened in the hospital due to poor care and should it not be fully cured or at least 80-90% cured before discharge considering the fact it needs a special bed repositioning every 2 hours.
Let me know.
Best Regards
Ashanti
Suggested Links:
- Quick tip for families in ICU: What are the right steps when weaning off ventilation & tracheostomy?
Hi Ashanti,
With your dad having a pressure sore on his tailbone, pressure sores are areas of localized damage to the skin and tissue, and they occur as a result of prolonged pressure or friction on the skin and usually affect those with limited mobility or those who are confined to a bed for prolonged periods of time.
Whilst sometimes pressure sores can develop even with high levels of care, pressure sores are often preventable and should not occur in a hospital setting if your dad was appropriately risk assessed and repositioned on a regular basis.
A risk assessment, preventative care, and nursing plan are usually done during hospital admission, and if there is a change in your dad’s condition, which identifies measures to prevent or reduce the risk of a pressure sore developing such as how often your dad should be repositioned and in what positions and these risk assessments are very important and should be reviewed on a regular basis.
Your dad has a Stage 3 Pressure Ulcer now and definitely a result of failure carrying out appropriate risk assessments; poor nursing care, delayed medical treatment, and poor record keeping.
After weeks of having the same issues with his wound, despite wound care and wound vac, the wound care team or tissue viability nurse along with the health care team should then at least have a treatment plan for this. We do not want another infection to happen again and they should be doing this before your dad gets discharged.
You can discuss this as well with the doctors.
Please update us on your discussion with the pulmonologist/neuro team regarding decannulation.
I hope this helps.
Thank you.
Kind regards,
Patrik
Hi Patrik,
Thanks, Patrik, for your replies.
With regards to wound care for my father’s pressure sore, they seem to have no treatment plan. As before they are rushing towards a discharge plan even before this medical issue is addressed. Though did not have a detailed discussion about it with the wound care team, they simply say it would take a long time to heal and he can get discharged with wound vac and continue the same at a long-term care facility. It’s hard to understand their way of thinking when their existing treatment seems to be not making significant progress in terms of healing.
From my understanding, how do such wounds get healed in general? What are your thoughts? Is there any alternative to a wound vac? This is kind of frustrating.
I have mentioned the seriousness of this medical condition as the chances of infection is high due to the nature and location of the wound. Can they force me to discharge with this condition?
With regards to tracheostomy, I couldn’t discuss it with his pulmonologist. He seems to be less optimistic in terms of him managing his secretions and aspiration risk. But I feel he is able to manage his coughing and swallowing as needed though not great. Will keep pushing back on at least trying to decannulate him while he is in the hospital and under medical monitoring.
By the way, I have raised a formal complaint today about the facility in terms of how the case management is pressuring me for discharge with these medical conditions for my father.
Make me worried and concerned that these people would jeopardize whatever hard progress made thus far on my father’s health. Let me know your thoughts and comments.
Thanks & Best Regards
Ashanti
Recommended:
Hi Ashanti,
Let me thank you for sharing his current condition with us.
With regards to your dad’s pressure sore, I believe his pressure sore was already evaluated by a wound care specialist, right? It is important that the wound must be re-assessed to evaluate the effectiveness of the wound vac.
Vacuum-assisted closure of a wound or wound vacuum-assisted closure (VAC) is a type of therapy to help wounds heal. During the treatment, a device decreases air pressure on the wound. This can help the wound heal more quickly. A wound VAC is indicated to be used for a large wound because large wounds can take a longer time to heal.
A wound vacuum system may help your wound heal more quickly by:
- Draining excess fluid from the wound
- Reducing swelling
- Reducing bacteria in the wound
- Keeping your wound moist and warm
- Helping draw together wound edges
- Increasing blood flow to your wound
- Decreasing redness and swelling (inflammation)
Wound VAC offers some other advantages over other types of wound care. It may decrease your overall discomfort. The dressings usually need changing less often. And they may be easier to keep in place.
Other pressure sore management to consider are:
- Cleaning and dressing the wound.
- Reducing pressure on the sore by frequently changing one’s position. This improves blood flow and allows faster healing.
- Proper nutrition. High protein diet is encouraged too.
With regards to the complaint you filed, I believe you just made the right decision. You always have the say when the services that you received aren’t enough or if the services you needed were not completed as expected. In that case, it is good that you filed a complaint.
I hope you find these helpful.
Let us know of your other concerns so we may assist you further.
Kind Regards,
Patrik
Hello Patrik,
Thanks for your email explaining about wound vac and how it helps. They had also done debridement twice so far. Need to discuss the healing progress of the wound with the wound care team. Also posting below your comments from your earlier email.
After weeks of having the same issues with his wound, despite wound care and wound vac, the wound care team or tissue viability nurse along with the health care team should then at least have a treatment plan for this. We do not want another infection to happen again, and they should be doing this before your dad gets discharged.
This is concerning from my end.
Also, with regards to de-cannulation if any patient has problems afterwards can they be re-cannulated easily? Any risks/complications associated with it.
Let me know.
Thanks & Best Regards
Ashanti
RECOMMENDED:
Hi Ashanti,
Thank you for your response.
Anyway, with regards to your last email regarding your dad’s pressure sore.
By this time, the issue with your dad’s delayed wound healing despite treatment with a wound vac, and routine wound care with debridement, should have been addressed already. The wound care team needs to be looking at other causal factors or contributing causes for this.
Here are a number of things that can delay or complicate the healing of wounds, including:
- Diabetes mellitus
- Low HGH (human growth hormone)
- Rheumatoid arthritis
- Vascular or arterial diseases
- Zinc deficiency
Again, the involvement of the whole team, including the doctor, nurse, therapists, patient care technician, and dietitian will help get the wound better for your dad.
And, yes, Ashanti, as I have mentioned before, it is indeed concerning, particularly your dad having a STAGE 3 pressure ulcer as you have stated before and that it needs to be treated or have it improved at least before he even gets discharged to prevent any occurrence of possible infections.
You can communicate with the wound care team and ask for their treatment plan for your dad’s pressure ulcer discussing the healing progress of the wound with them would also be beneficial but making sure that they are really doing something about it.
Regarding your question: “Also with regards to de-cannulation if any patient has problems afterwards can they be re-cannulated easily. Any risks/complications associated with it.” The doctor is the one who can assess that. Different patients have different concerns. You can have your dad’s doctor discuss this with you as well.
We hope this information helps.
For any further questions, please don’t hesitate to ask.
Thank you.
Kind regards,
Patrik
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!