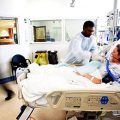
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Cathy as part of my 1:1 consulting and advocacy service! Cathy’s mom is critically ill in ICU and the ICU team wants to do tracheostomy and PEG insertion. Cathy is asking if it is too much for her mom’s condition.
The ICU Team Wants to Do Tracheostomy and PEG insertion for my Mom in ICU. Isn’t it too Much for Her Condition? Help!
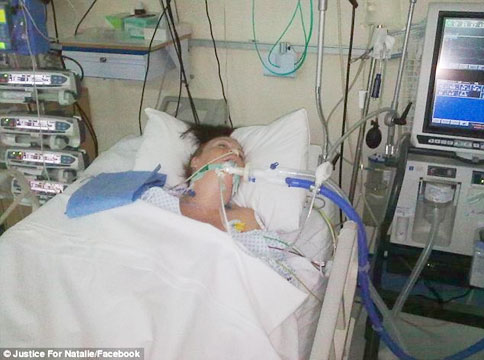
“You can also check out previous 1:1 consulting and advocacy sessions with me and Cathy here.”
Patrik: So, those are the main reasons why you wanted to move to a tracheostomy, but there’s other reasons as well. In your mom’s case, I would argue once somebody has a tracheostomy, I’m almost bound to say they have more time to come off the ventilator, in a time that works for the patient. And also, things like mobilization is so much easier. It’s a much more stable airway compared to a breathing tube.
Cathy: Got it, got it.
Patrik: Much safer.
RECOMMENDED:
Cathy: Okay, so if I, my initial response was, “Is this too much at once?”
Patrik: Yes.
Cathy: Say yes to the tracheostomy and just tell them to move the feeding tube for now.
Patrik: Yes.
Cathy: And then concentrate, because he even said he thinks she may be able to breathe on her own with the tracheostomy because of just how she’s been doing since Friday when they changed the setting. But again, these are things that I have to point out to them. There’s no positive feedback at all on any of this. I’m like, if I didn’t have decent science classes in school, I wouldn’t even know how to navigate this and I understand why people, it just drives them nuts.
Cathy: Maybe people have better doctors, but mine just, I have to pull everything out of them. It wasn’t like, you’ve just explained to me, which is what I would expect. He’s like, “Oh, so I understand you want to keep going with this. Okay, we need a PEG and a tracheostomy. Nurse, give her the forms.”
Patrik: Yeah. Exactly, exactly. Sign on the dotted line. I know how you feel. They approach everything from, “Your mom’s life is not worth living. Let’s just move on with those things quickly.”
Cathy: Right, yeah. So, that’s where I’m leaving. So, if we did the tracheostomy and see what happens, then when should I consider reassessing getting the PEG in?
Patrik: So, given that your mother is breathing spontaneously by the sounds of things, given that she’s probably in a, have you heard of a CPAP mode?
Cathy: Yes. Yeah. like the sleep apnea mode?
Patrik: Yes.
Cathy: Yeah.
Patrik: Have the mentioned that?
Cathy: The only reason I know that is because when he switched the settings, when she was taking too long to breathe, the warning that came up was like sleep apnea mode, yeah.
Patrik: When you’re back in the hospital, do you think you can send me a picture of the ventilator?
Cathy: Sure.
Patrik: That would be good because I’ll tell you why. If your mother is breathing in CPAP or it’s also considered as pressure support, there is a very high chance that she might be able to breathe spontaneously without a ventilator, and she may need a tracheostomy but she may not need a ventilator.
Cathy: Got it. Okay.
Patrik: So, the sooner we can establish what mode she’s in, the sooner we can establish where is this going.
Cathy: Okay, okay.
Patrik: Have I answered your question in terms of why people need tracheostomies?
Cathy: Yes, yep. You have.
Patrik: Okay and I will send you some articles as well just to explain a little bit more about why with tracheostomies.
Cathy: Okay, but yeah, that makes total sense. I don’t know. I was just reading, I guess, at the height of the whole COVID thing, these people being on ventilators for all these days and they’re not coming off.
Patrik: Yeah, but the COVID is unique in terms of there have been a lot of delays of people getting tracheostomies because of staff being at risk contracting COVID. So, the COVID patients, I know of cases, the patients didn’t get a tracheostomy until they were COVID-free.
Cathy: Got it, okay, okay.
Patrik: But that was mainly to protect the staff.
Cathy: Right, okay. And for the switching the tube for the feeding, what would they come back with me if they wanted to object to that request?
Patrik: No, they would come back to you and say, “She will never eat. She will never eat again, so she needs a PEG.” That probably will be their response. That’s why I also ask you is your mother coughing, and I think you should be asking them if they have seen her cough. If she is not coughing, that’s probably another sign that she has some significant brain damage, but they may have seen her cough. Again, especially when they turn her, wash her back or whatever, she might cough then.
Cathy: Okay.
Patrik: Do you know how often they suction her?
Cathy: Well, it used to be pretty often at first and now, I haven’t seen them do now because I was there today for maybe two and a half hours, and I didn’t see them suction her at all.
Patrik: Okay. And when you have seen them suction in the past, she didn’t cough there at all?
Cathy: No, not at all.
Patrik: That’s definitely a concern, especially since she hasn’t been on sedation from day 1. For someone that has optimal brain function, the breathing tube and the suctioning, people report that they feel like they’re drowning. So, that is definitely a little bit of a concern there, that some areas of her brain may not work 100% if she’s not coughing after such a massive stimulus, because suctioning is a massive stimulus.
Cathy: Okay.
Patrik: And also, bear in mind, the cough is a natural reflex, but that leads me to the PEG. If she is not coughing and even if she was waking up, if she has got a limited or a cough reflex that’s not present, she, as a matter fact, won’t be ever eating again because she can’t eat with a cough reflex. Does that make sense?
Cathy: Yeah.
Patrik: Sorry to be so blunt, but I know you want answers. She will not eat without a cough reflex, and that then would make it more likely that she does need the PEG.
Cathy: That she does need the PEG, okay.
Patrik: Yeah, yeah. Definitely a question you need to ask, does she have a cough?
Cathy: All right, I think that answers everything. Just with the PEG because they’re taking her into surgery, because I tried to have him when I was trying to say, “Well, is this going to be too much for her?” And he was saying that they just kind of, I guess they go in through the mouth, shine a light, put the needle in, and then put the tube in. So, is that something that might be typically done in the ICU room?
Patrik: Yeah.
Cathy: Why is he going into surgery?
Patrik: That is a question, good question. Is this the person that you’ve spoken to, is this an ENT surgeon, an ear, nose and throat specialist, or is this an intensivist?
Cathy: That’s a good question. I don’t know what he is. This is the guy that I haven’t talked to that I’m supposed to talk to tomorrow, Dr. Sequio.
Patrik: Find out his specialty. Most ICU consultants in this day and age should be able to do the tracheostomy at the bedside. The ICU consultants, however, are generally speaking not doing the PEGs.
Cathy: Okay. Well, he’s supposed to be doing both of them.
Patrik: Then he’s probably a general surgeon or an ENT specialist. He must be some kind of surgeon, I would argue.
Cathy: Okay. All right.
RECOMMENDED:
Patrik: And then from your email, you also wanted to talk about home care. Is that right?
Cathy: Yeah. I was just talking about the progression, and a lot of that will probably depend on even if they accept her at all. So, LTAC wouldn’t even be an option, but as you pointed out, if I get her on something where they’re going to give me a 24-hour nurse or just for some hours, then you just plan it around that, and she would just come straight home.
Patrik: Yep. Look, some thoughts on that. We have some clients here where we don’t provide 24-hour care even though, from our perspective, the clients need 24-hour care. It can be a funding issue. If clients don’t have funding for 24-hour care even though they are ventilated, have a tracheostomy, most of my clients ask for overnight nurses, not so much for daytime nurses because I believe families need some sleep at night. It’s also that clients are more vulnerable at nighttime than they are at daytime.
Patrik: I’d still strongly feel that anybody that’s got a tracheostomy and is ventilated needs a nurse 24 hours a day. The stress on families is pretty big even if they have 24-hour care because it’s just, I mean, it is a stressful situation having a loved one at home on a ventilator. You’ve got people around all the time. It’s a big intrusion into your privacy.
Cathy: Okay. But yeah, because, again, it might not even be an option because she doesn’t get accepted.
Patrik: Look, I’ll give you the idea. Okay, let’s just say we were in your area. Let’s just run this through hypothetically. Let’s just say we were in your area. Funding aside, let’s just say funding was there for 24-hour home care. I would argue that the soonest your mother has a tracheostomy, has a PEG or a nasogastric tube, it doesn’t matter and she’s medically stable, meaning she’s not on vasopressors, she’s not on the norepinephrine that we talked about, she’s not on any intravenous medication even though intravenous medication can be done at home as well, we could take her home. Right?
Cathy: Right.
Patrik: So, the missing links then would be you’ve got to have a doctor overseeing the care, but that could be even your mother’s GP.
Cathy: Right and I have a message in to them with that question.
Patrik: Yeah. So, it could be a GP. It definitely needs to be someone that you trust. Does your mother have a GP that you or she would trust?
Cathy: Yes. She has a very good internist who we see now, who knows how she is and all that. So, yeah, I just have to wait for him to get back to me to see what they would be able to do.
Patrik: But you can look at other people too. Like it would great if she was to go home on a ventilator, it would be good to have a respiratory physician, or a pulmonologist definitely would be good.
Cathy: Okay, got it.
Patrik: As you know, all these specialists, their biggest problem is they often see home care as we need them. And that’s why I think a GP is good or there are some hospitals that have doctors employed that are treating patients at home. I’m not saying it’s not happening, but it’s not the norm.
Cathy: Exactly, yeah. Exactly, okay.
Patrik: Have you contacted the organization I am telling you about?
Cathy: I did and I have not heard back from them.
Patrik: Oh, that’s disappointing.
Cathy: Yep, I did but I haven’t heard back. So, we will wait on that.
Patrik: Whereabouts are you again?
Cathy: I am in Tampa Bay, Florida.
Patrik: And that’s where your mother is as well.
Cathy: Right, exactly.
Patrik: There would be other organizations as well. That organization is pretty prominent all across the States, but they may not necessarily have a branch where you are, but they would know someone.
Cathy: Exactly.
Patrik: They would know someone. Have you typed into Google? Hang on, just give me a second. Let me type into Google, tracheostomy home ventilation, Tampa Bay, Florida see what comes up. See what comes up. Yeah, there’s things coming up, but just judging from it, it’s mainly all LTACs, I believe but there could be. Hang on a second. There could be one link. Hang on. I’ll send that to you whether that could be something, it’s a highly specialized skill. It can be done, and it’s done all the time, but you also need to engage with the right provider. That’s really important. Do you have any other questions?
Cathy: No. I think I am ready to talk to Dr. Sequio tomorrow and we will go from there and keep taking it one day at a time.
Patrik: Yep, and no more talk about DNR.
RECOMMENDED:
Cathy: No. They’ve never even brought it up.
Patrik: That’s good. That’s good. Okay, and if you could send me a picture of the ventilator and the bedside monitor, that would be really good. Flick it to me in an email and I’ll tell you what ventilation mode she’s in because if she’s breathing spontaneously already, chances that she can come off the ventilator are there.
Cathy: Okay, sounds great. I will do that tomorrow.
RECOMMENDED:
Patrik: All right, excellent.
Cathy: All right. As always, thank you, Patrik, and I’ll talk to you again soon.
Patrik: Thank you. Thank you for being a client. Take care.
Cathy: All right.
Patrik: Thanks, Cathy. Thank you. Bye.
Cathy: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!