Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can We Prevent Our Daughter to be on a DNR (Do Not Resuscitate) Status in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about What Questions to Ask if You’re Locked Out of ICU Due to COVID and Your Loved One is Critically Ill!
What Questions to Ask if You’re Locked Out of ICU Due to COVID and Your Loved One is Critically Ill!

Welcome to another Intensive Care Hotline livestream. I’m your host, Patrik Hutzel from intensivecarehotline.com. So, today’s livestream is about, “What questions to ask if you’re locked out of ICU due to COVID and you have a loved one critically ill in intensive care?”
Before I dive into the topic, I want to quickly talk about what makes me qualified to talk about this particular topic.
I am a critical care nurse by background having worked in intensive care for over 20 years in three different countries. Out of those over 20 years, I have worked as a nurse unit manager in intensive care for over five years having given me all the insights behind the scenes. I also have worked and am still working with Intensive Care at Home where we provide services at home for long-term intensive care patients, predominantly on a ventilator with tracheostomy. I have been professionally consulting and advocating for families in intensive care all over the world since 2013. I’m talking to people in intensive care or I’m talking to families in intensive care all over the world every single day. So, that’s a little bit about my background. I obviously run the intensivecarehotline.com website together with my team of very experienced intensive care nurses. I also run the Intensive Care at Home, and you can check out intensivecareathome.com for more information there.
RECOMMENDED:
But let’s dive right into this topic today.
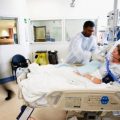
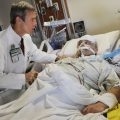
So, it’s critical what questions to ask when you have a loved one in intensive care, and that has always been the case. It had nothing to do with COVID, but then obviously COVID came along early 2020 and, all of a sudden, families in intensive care found themselves locked out of intensive care because intensive care units would not allow families to visit. It has been very challenging for families in intensive care before COVID. Now, all of a sudden, there’s another layer of complexity where families can’t be with their loved ones when they need them the most. It’s been absolutely heartbreaking to see what’s been happening all around the world, that all of a sudden, families were locked out of intensive care.
If you followed my blog for any length of time, I’m always talking about the perceived power that intensive care units have, or intensive care teams have. And now, this was aggravated by families being locked out of intensive care, only being able to visit for a few minutes, only being able for one family member to visit. In-person visits were replaced by FaceTime, via Zoom, or WhatsApp, or any technology that hospitals could really use, but that would never replace being physically there with your loved one and talking to the doctors, talking to the nurses. All of a sudden, there was another layer of complexity. And then, the next layer of complexity that came was families were then trying to call intensive care units and doctors/nurses not being available because the workload had dramatically increased with COVID patients literally pouring into ICU.
So, an already difficult environment pre-COVID was getting even more difficult with COVID coming in and families locked out. So certainly, throughout this period, we’ve spoken to numerous intensive care teams, doctors, nurses, and help families to ask the right questions, but I also realized our capacity is limited.
And then, even in June 2020, I did make a big blog post about, “What questions to ask?”, realizing that now is the time to make intensive care even more transparent because families were struggling to get in front of intensive care teams, asking the right questions and negotiating with them, trying to find out what’s really happening. That’s when I came up with a lengthy blog post in June 2020. The title of the blog post, which I’ll link after this video is, “What questions should you be asking if you have a loved one in intensive care?”
It’s really critically important that when you talk to doctors and nurses, especially remotely because they’re not allowing you to visit, that you can come to the point, extract information from them as quickly as possible because it’s literally life or death. Let’s dive right into that in a minute.
And just, the other thing that we’ve seen over the last nearly two years now is families ring up intensive care units and ICU’s doctors/nurses and say, “I’m busy. I’ll call you back.” They never call back. If they do call back, they call back at a time that’s not convenient for the family. People are at work, have other commitments, and so forth. So, we are finding an incredibly challenging environment that families and also intensive care units are operating in at the moment, but let’s dive right into it.
So, when asking questions, I approach it in a way that I would approach if I received handover from a doctor or from a nurse in intensive care. If you and I were to get on a call with the doctors or with the nurses, the way I approach it is as if I was to get handover from a doctor or from a nurse in intensive care myself, as a bedside nurse, or as a nurse in charge, whatever the case may be. That means you’re going, literally, from head to toe.
Now, what is important when you’re starting with the head, from head to toe, is the first thing that needs to be assessed is the neurological condition. Why is this important? You might be thinking, “Why is neurology important if my loved one is in intensive care with COVID?” For example, with COVID, pneumonia, COVID ARDS (Acute Respiratory Distress Syndrome), or any other condition where neurology is not the main focus. Well, I can tell you why it is important.
Many patients in intensive care are ventilated. Most of our clients have a loved one in intensive care that’s ventilated, which means most of the time, they’re in an induced coma or they’re on strong sedatives, strong opiates, for them to be able to tolerate mechanical ventilation. If someone is on sedatives, or even if they’re not on sedatives and they have a breathing tube, you need to assess the neurological condition because if a patient can’t talk, well, you always need to rule out a neurological event such as a stroke, seizures, anything that’s related to a neurological event. Therefore, that’s where you start because if the brain is not working for whatever reason, you got to question, what else is going on? Therefore, you got to start with, “Is someone in an induced coma?” If they are in an induced coma, what medications are they getting? What is their Glasgow Coma Scale?
Now, Glasgow Coma Scale is a neurological assessment tool that’s being used in intensive care all over and it’s being used multiple times a day. If someone has a head and brain injury, it’s being used hourly. If someone doesn’t have a head or brain injury, it’s still used multiple times a day because it’s a very good tool to assess neurological condition in the absence of people being able to talk, and so forth. So, I would recommend for you to ask for the Glasgow Coma Score. There’ll be a link to a Glasgow Coma Score below this video, again, so that you can have a look at it and make sense out of it because I think every family in intensive care needs to know about a Glasgow Coma Score.
Other issues when it comes to the neurological condition is pupil reaction. If someone’s brain is working and you shine a torch into someone’s eyes, the pupils are reacting to light, which means they’re constricting. Someone that’s brain dead, for example, you shine a torch into the eyes and the pupils are not reacting to light, that could be one sign of someone being brain dead.
Coming back to sedation, you don’t want to oversedate a patient. It’s critically important that you minimize sedation. It should only be used temporarily while someone is ventilated with a breathing tube or endotracheal tube. If they can’t be extubated, well they may need to go onto a tracheostomy, but we’ll talk about that later. It is more important that you ask for sedatives. What sedatives is your loved one on? What opiates or painkillers is your loved one on? How does that impact on the Glasgow Coma Scale, on the neurology? Are pupils reacting to light? If, God forbid, your loved one has a history of seizures, are there any seizures? If there are seizures, how are they managing it? That’s all part of a neurological assessment.
Suggested Links:
Other assessments that need to be done as part of the neurology are, if you talk to your loved one, are they opening eyes? Are they obeying commands such as squeezing hands, squeezing fingers, and so forth? That’s all very, very important to get a good understanding of where your loved ones at neurologically.
Then, also part of a neurological assessment, at the moment, especially with COVID (COVID ARDS and COVID pneumonia) is that many patients are being proned. What that means is if they’re going into prone position, they need to be deeply sedated, but they’re often also paralyzed with paralytic agents, which is another layer of complexity, especially when it then comes to be woken up because there’s often even more delays. Someone is in an induced coma, sedatives, and opiates are given and it can take quite a while for them to wake up. If someone is paralyzed on top of that, it takes even longer to wake up. So, that gives you a good understanding about what needs to happen from a neurological point of view.
We’re going from head to toe, remember.
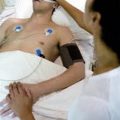
Next, we need to look at the hemodynamic assessment or the cardiovascular assessment. So, what does that mean? You need to find out if your loved one is in a regular heart rhythm. That’s very important.
Some patients in ICU are in an irregular heart rhythm, such as atrial fibrillation, also known as A-fib. If they had a cardiac arrest, they might have other irregular heart rhythms, so that’s really important question to ask.
Next, blood pressure. Is blood pressure compatible with life? It’s a very important question to ask in intensive care. If it’s not compatible with life, patients often are on inotropes or vasopressors to maintain a blood pressure that is compatible with life. Inotropes or vasopressors such as noradrenaline, norepinephrine, epinephrine, adrenaline, vasopressin, milrinone, dopamine, dobutamine, and the list goes on, are considered life support. So again, very important question, is blood pressure compatible with life?
Next, body temperature. A lot of patients in intensive care are having a temperature because they might have an infection and so forth. Other issues when it comes to hemodynamic assessment, also blood results: white cell count, hemoglobin, electrolytes. It’s all part of the hemodynamic assessment: electrolytes, coagulation, liver function, kidney function, arterial blood gases. I’ll talk a little bit more about arterial blood gases in a moment when we talk about the respiratory status.
So then, also when it comes to hemodynamic assessment, also need to look at, does your loved one have a central line? A PICC (Peripherally Inserted Central Catheter) line? Does your loved one have an arterial line? Does your loved one potentially have a Swan-Ganz catheter, or a PA (Pulmonary Artery) catheter, or a PiCCO (Pulse index Continuous Cardiac Output) catheter to monitor cardiac output, cardiac index, SVR (Systemic Vascular Resistance), SVRI (Systemic Vascular Resistance Index), and so forth? So, I’m getting more into the nitty-gritty here, but if someone is hemodynamically unstable, and many patients in intensive care are hemodynamically unstable, they might have things such as a PA catheter or a Swan-Ganz catheter.
Also, what is their CVP like: central venous pressure? Very important number to assess fluid status of a patient, to assess are they fluid-overloaded? Are they dry? Are they in a happy medium? And so forth. So, that’s it in a nutshell when it comes to hemodynamics in a critically ill patient in intensive care.
Just quickly going back to neurological condition, I forgot to mention one thing, especially when it comes to head and brain injuries such as a traumatic brain injury, subdural hematomas, subarachnoid hematomas, and so forth. It also comes down to then asking whether your loved one has an ICP, an intracranial pressure monitor. What is their intracranial pressure? Is it life-threatening? Has a CT (Computed Tomography) of the brain been done? MRI (Magnetic Resonance Imaging) scan of the brain being done? Those are all very important questions.
Now, if your loved one does have an ICP and an intracranial pressure monitor, and if they have high brain pressures, that can be life-threatening. Again, then the question is how is that being managed? How is that being treated? Is it treated with venting the extra ventricular drain that’s sitting in the brain? Is it treated with hypertonic saline? Is it treated with sedation? and so forth. What is the CPP like, the cranial perfusion pressure? Making sure that enough oxygen is going to the brain. I just wanted to throw that in here.
So, we talked about neurology, we talked about hemodynamics. Now, we will be talking about the respiratory system or respiratory assessment. Again, we’re going from head to toe: neurology, heart, hemodynamics, and now we’re talking about the lungs.
As I mentioned, many patients in intensive care are ventilated. They might be ventilated with a BIPAP (Bilevel Positive Airway Pressure) mask. They might be ventilated with a breathing tube or endotracheal tube, or they might be ventilated with a tracheostomy or a trach, or they might not be ventilated at all. They might be spontaneously breathing, but they might have high oxygen demands. They might have high-flow nasal prongs, and so forth.
So, what do you need to assess when it comes to the respiratory function? You obviously need to assess. First question for you, if you have a loved one in intensive care is, are they ventilated? Are they spontaneously breathing? If they are ventilated, what settings are they on? If they’re not ventilated, what’s the next step? If they are ventilated, what is the next step? If someone is on a breathing tube, can they be weaned off the ventilator? Do they need a tracheostomy? If they can be weaned off the ventilator, can they go on to spontaneously breathing? Do they need to go onto BIPAP or CPAP (Continuous Positive Airway Pressure)?
Now, one way or the best way to assess respiratory function is obviously by assessing a patient, seeing what’s their breathing like. Is the breathing calm? Is it labored? Can they take deep breaths? Can they cough? Are they in pain when they’re breathing? Obviously, another way to assess respiratory function is looking at oxygen saturation, which is often with a finger clip or with an ear clip being transmitted to a monitor. It should be above 96% most of the time.
Other assessments you can make is obviously skin color. If the lips are blue or cyanotic, you would be very worried about their respiratory function. But one of the best ways to assess respiratory function really, besides looking at the ventilator, besides knowing/understanding the numbers on the ventilator, is to look at arterial blood gases.
Now, arterial blood gas will tell you pretty much everything you need to know. How well ventilation is working? How well spontaneous ventilation is working? It gives you a very good assessment of other issues as well such as lactate, potassium, bicarbonate, and so forth, which are very important assessment tools as well, especially if someone is septic, especially if someone is having kidney failure. So, the arterial blood gas is a really good assessment tool for a lot of things.
Now, next, you should be asking about chest X-ray results. You should be asking about, how often does your loved one need suction? Again, are they coughing? It’s very important because if they’re not coughing, it means they can’t really maintain a stable airway. Amount and frequency of suction are very important to know to find out if there is an infection. If they need too much suction, they’re probably not ready to come off the ventilator as yet.
Other issues you should be looking for or should be managing in this situation is, again, how far away are they from coming off the ventilator? Are they too deeply sedated to be woken up and having the chance to get off the ventilator? Because if they can’t be weaned off the ventilator, well, the next steps are to potentially look at a tracheostomy. Also, is your loved one fighting against the ventilator? What I mean by that is many patients, if they’re in a semi-coma and only on light sedation, they might be fighting against the ventilator. If they’re fighting against the ventilator, they might need more sedation. So, there’s a lot of issues that you need to look at when someone is on a ventilator. Again, looking at it in much detail. For example, you need to understand what are present ventilator settings in ICU: SIMV (Synchronized Intermittent Mandatory Ventilation), ACV (Assist Control Ventilation), pressure support/CPAP, pressure control versus volume control. There’s a whole range of things you need to look at.
Recommended:
I often get phone calls from prospects or from clients and they say, “Hey, I’ve got a family member in intensive care. They’re on a ventilator. They’ve had a stroke. Can you tell me whether they’re going to survive?” And I say, “Well, it’s not enough information.” It needs to be broken down into what we’re talking about now, into questions that you’re asking and knowing and understanding the nitty-gritty.
Again, the biggest challenge for families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights. They don’t know how to manage doctors and nurses in intensive care. So, it’s a very complex arena and that’s why I’m making these videos so that you can understand what you need to look for.
One last question, if your loved one is ready for extubation, for having the breathing tube removed or having the tracheostomy removed, the intensive care team needs to make sure that your loved one can breathe independently and spontaneously with a good cough, with good blood gases, clear chest X-rays, and so forth.
Sometimes patients in intensive care also have chest drains for pleural effusions. You got to ask, do they have chest drains? If so, why do they have it? When will they come out? And so forth. Other issues that can happen when someone is ventilated, they might have a bronchoscopy where a camera goes down into their lungs and to see whether where the infection sits, sometimes to suction out mucus to clear the lungs, and so forth.
Now, carrying on number four, going from head to toe, is GI tract or gastrointestinal system or gastrointestinal tract. Now, why is this important? Your loved one, if they’re on a ventilator, not being awake, they probably have a nasogastric tube or a PEG (Percutaneous Endoscopic Gastrostomy) tube. They get enteral feeds through those tubes. You need to find out how much are they getting? Are they absorbing feeds? Are there any residuals? Are they opening bowels? Is their tummy distended? Are they feeling bloated? Are they opening bowels? Very important questions when someone is in intensive care. Feeding, generally speaking, should be started as quickly as possible. If they’re not absorbing feeds, can be managed medically; can be managed with Maxolon; can be managed with erythromycin to improve absorption or digestion of feed. If all that doesn’t work, if enteral feeds can’t be tolerated, can’t be taken for whatever reason, the next step is to look at TPN or IV nutrition (Intravenous nutrition). The TPN stands for total parenteral nutrition, but at the end of the day, it’s intravenous nutrition as an alternative.
So next, also before we move on to kidneys, when someone questions around the gastrointestinal system, you also need to think about some patients in intensive care might end up with stomach ulcers. Even worse, they might end up with stomach bleeds. It can be a stress response from the body just by being a patient in intensive care. That can result in stomach bleeds or GI bleeds. Also, when someone is in intensive care, they should also have a proton pump inhibitor to minimize the risk of bleeds. That can be pantoprazole. It can be something like ranitidine or esomeprazole.
Next, kidney function. When someone is in intensive care, it’s easy for the kidneys to go off. Why is that? Kidneys can go off because of low blood pressure. Many patients in intensive care have low blood pressure, which means the kidneys are not getting enough perfusion. It can be a byproduct of sepsis. It can be a byproduct of an infection. Can be a byproduct of antibiotics being given; painkillers being given. So, many patients in intensive care do go into kidney failure, temporarily, most of the time. So, what you should be asking for is, how much is urine output? Are the kidneys working? Are kidney markers looking okay? What are fluid balances like? I.e., how much fluid is going in/how much fluid is going out? You don’t want the fluid balance to be too positive because that is a risk for fluid overload and it’s a risk for pulmonary edema, for example, which is then, in retrospect, a risk for not being able to come off the ventilator.
Before we go to the endocrine system, I also want to throw in for kidneys. If kidneys are not working, there’s several things that can be done. If dehydration is the issue, you can do a fluid challenge: give more fluids. If there’s enough fluids on board, you can give furosemide to increase urine output, or you could do hemofiltration and remove fluids with a dialysis machine.
Next, endocrine system. Endocrine system means things such as blood sugar regulation. Many patients in intensive care, as part of the stress response that I was talking about earlier, end up with high blood sugars and they end up on insulin, often temporarily. If someone is in stress, the adrenal gland is producing more sugar again as part of a stress response and then insulin is needed to counteract that. It’s quite a common phenomenon in intensive care that patients have high sugars temporarily and they just need to be managed. Obviously, if someone is in intensive care and is diabetic already, that’s a separate issue. Then sugars, from my experience, are even more difficult to be managed.
Now, last but not least, you also need to look at general aspects of being a patient in intensive care, i.e., nursing care, regular washes, regular turns, making sure there are no pressure sores because that can happen very easily when patients are in intensive care. They get pressure sores because they’re not being mobilized. They can get pressure sores on their head, on their sacrum, on their heels, on their elbows, on their shoulders, and all sorts of places. So, it’s very important that patients are being looked after very well in terms of turning them regularly, in terms of inspecting their skin regularly, washing them regularly, providing mouth care regularly, providing nose care regularly. Those are all very important aspects of care. Nursing care in intensive care. You don’t want your loved one to end up with pressure sores or the likes. Again, hygiene is very important: regular washes. If they’re more stable, maybe they can have a shower. All very important issues to be looked at.
Now, that’s it in a summary. I’m really curious to find out what questions that you have on this call. While I’m waiting for your questions, I’m just going to Helene’s questions.
Helene, you’re asking, “What about if a patient suffered Iatrogenic malfeasance hypoxia encephalopathy brain injuries?.” So, that probably comes back to the neurological assessment that I was talking about in the beginning. If someone has hypoxia, then the neurological assessment is critically important. So, you got to assess their Glasgow Coma Scale. Again, I urge you to familiarize yourself with the Glasgow Coma Scale. You can google Glasgow Coma Scale and you will find information. It’s very easy to interpret. It’s very easy for you to interpret. So, important to make regular assessments of a Glasgow Coma Score. It’s important to look at CT scans, MRI scans of the brain. You potentially need to look at an EEG (Electroencephalograph). You need to look at what is happening… If their Glasgow Coma Scale is low and they’re not waking up, are they also on sedation? It’s critically important that if someone has a brain injury, that they’re not on sedation; or if they are on sedation, how does that impact on the brain injury?
Suggested Links:
The problem there is, Helene, that often when someone is having an anoxic brain injury, when they’re coming out of the induced coma, if they’re not waking up, it’s difficult to say whether they’re not waking up because of the brain injury, or whether they’re not waking up because of all the sedatives that they had. Because many patients in intensive care without a brain injury, there’s often a delay in them waking up after an induced coma.
Helene, does that answer your questions or did you have any other questions in regards to that? Also, if there’s encephalopathy, your loved one might need an ICP, an intracranial pressure monitor, or at least an EVD, an external ventricular drain, to drain some of the CSF (Cerebrospinal Fluid), especially with high pressures in the brain.
Now then, you’re also asking Helene, “What are pressors or what is pressor?” There are two terms for pressor, either vasopressor or inotropes. Now, what is an inotrope? What is a vasopressor? So, when someone has a low blood pressure in intensive care that is incompatible with life or is not sustaining enough kidney perfusion, which comes back to the kidney failure that I was talking about a minute ago, they often need a pressor or an inotrope. Basically, what it is, medications such as norepinephrine, noradrenaline, epinephrine, adrenaline, but also vasopressin for example, they are called vasoconstrictors. What that means is they’re constricting the blood vessels in the peripheries, in the arms, in the legs, and concentrate the blood towards the heart, which in essence is increasing blood pressure. That’s one way.
There are other inotropes or vasopressors such as dobutamine or milrinone. They are not a vasopressor, but they’re working on the contractility of the heart, so they’re positive inotropic and they are working on the contractility of the heart. If they’re working on the contractility of the heart, blood pressure increases, ejection fraction increases often. Ejection fraction, again, is an assessment that can be made with an ultrasound in intensive care or in other areas to assess the contractility of the heart and dobutamine and milrinone, in particular, are doing that, and that’s often increasing the blood pressure as well.
Inotropes or vasopressors are considered life support and that is a very important issue to be looked at. If someone is on life support in intensive care, it’s a sign they can’t leave intensive care. So, that’s with the pressors, the vasopressors and the inotropes. I hope that helps.
And then you’re asking, “Can central lines be used for propofol and regular medication?” Yes, absolutely. “What if BIPAP injuries that resulted in overactive saliva glands, will that affect aspirations?” Yes. I can see why a BIPAP injury might result in overactive saliva glands. Yes, with the pressure I can see that. “Will that affect aspirations?” Yes, absolutely. If there’s an overactive saliva or if the saliva glands are overactive and there’s too many secretions, the risk for aspiration is definitely higher. Absolutely. And then, if there’s a risk of aspiration, you have a risk of an aspiration pneumonia, it could turn into a vicious cycle.
I am conscious of the time. I usually run those for about 30-40 minutes at the most. If you have any other questions about today’s topic or about any other topics in intensive care as it relates to your loved one, please type your questions into the chat pad, so that I can answer them.
While I’m waiting for your questions, I’m just trying to wrap this up, so thank you for coming onto this call. I usually do them every Saturday or Sunday. Saturday night in the U.S. time. Sunday morning here in Australia. They’re usually running at 7:00 PM Eastern Standard Time, 11:00 AM Sydney Melbourne time. I usually choose a topic that is highly relevant for families in intensive care.
If you have any suggestions, if there’s anything you want me to talk about specifically, please type it in the chat pad or just send me an email to [email protected] where you can suggest the topics that you want me to talk about.
Now, if you like this video, give it a thumbs up, give it a like, click the notification bell, and subscribe to my YouTube channel, of course, where you get regular updates and regular livestreams for families in intensive care.
If you have a loved one in intensive care, you can also go to intensivecarehotline.com and call us on one of the numbers on the top of our website. I highly encourage you to give us a call or send us an email, again, to [email protected].
We provide one-on-one professional consulting for families in intensive care. We talk to doctors/nurses. We participate in family meetings. We review medical records. We have a membership for families in intensive care and we get outcomes for families in intensive care. We get real results. We can advocate on a clinical level. We can talk to the intensive care team on the same level. We can provide a second opinion for you and for your loved one. Most importantly, we take the curtains away when it comes to intensive care. We help you speaking the “secret language” in intensive care because the doctors often talking in language where it’s difficult to understand what’s really going on. They’re often only telling you half of the story and we can get you the full picture. We can ask all of the questions in intensive care that are important to ask.
Recommended:
Today, I gave you most of the questions, but it really comes down to break it even down into more detail. I mean, really scratching the surface only today. The best we can help you is really by talking to you directly, by talking to the doctors and nurses directly, by participating in family meetings with you and looking at medical records. That’s how we can do our best work and get you the best outcomes for your loved one.
So, if there are no further questions, I want to wrap this up. I want to thank you for coming onto the call. Again, if you have any suggestions for next week’s topic, leave them below this video. In the meantime, I’ll have ideas for next week’s topic anyway and I will just schedule it if I don’t hear from you.
Thank you so much again for all your support. Thank you for coming onto the call. Have a good night.
Hang on. There’s one more question, “Should there be an ABG prior to discharge?” No, not really. Not really, Helene, and I tell you why. If someone is being discharged, they should have the arterial line removed, I’d say at least 24 hours before discharge. Don’t get me wrong, there are certain patients where you do an ABG (Arterial Blood Gas) before discharge, but they’re more people that are sitting on the fence and that also probably have a higher risk of bouncing back into ICU. But generally speaking, if a blood gas has been done 24 to 48 hours before discharge, that should be sufficient presuming a patient has been off the ventilator at least for 24-48 hours. I hope that helps.
RECOMMENDED:
Again, thank you so much for joining me and thank you for all your support.
This is Patrik Hutzel from intensivecarehotline.com.
I will talk to you next week on this call at the same time. 11:00 AM, Sunday morning, Sydney, Melbourne Time. 7:00 PM Eastern Standard Time, New York-Boston. 4:00 PM Pacific Time, L.A., and San Francisco Time. 6:00 PM Central Standard Time, Chicago Time.
Take care for now and wishing you and your families all the very best.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!