Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can Prone Positioning Help my Critically Ill Loved One with COVID/ARDS in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about how to treat COVID- 19 ARDS/Lung failure in ICU.
Your Questions Answered Live: How to treat COVID-19 ARDS/Lung failure in ICU!
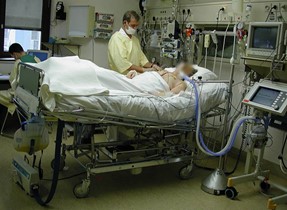
Hi, it’s Patrik Hutzel from intensivecarehotline.com. Today’s topic is about how to treat ARDS or lung failure for COVID-19 in intensive care. I want to welcome you to the live stream. I also want to welcome you if you watch this video at a later stage.
So before we dive right into the topic, what makes me qualified to speak about this topic? I have worked in intensive care as a critical care nurse for over 20 years. As part of that, I have done a postgraduate certificate in critical care nursing. I worked in three different countries around the world. I’ve worked as a nurse unit manager in intensive care for over five years. And I have been consulting and advocating for families in intensive care for nearly a decade now, staying on top of current practices by really talking to intensive care units all over the world, but predominantly in the United States, Canada, Australia, the United Kingdom and Ireland. So that is why I’m here today.
I assume that if you are here today, you have a loved one in intensive care with COVID-19 and ARDS/lung failure. And part of the issue there is that, a lot of ICUs simply lock out people at the moment because of real or perceived restrictions that they impose on hospitals. So where they think they need to protect other patients, they need to protect staff, but also need to predict other family members from being infected or getting infected with COVID-19.
RECOMMENDED:
Before we dive further into this topic, I would also want you to like this video, comment what questions that you have as we go along. Also share what insights you get from this video, and also subscribe to my YouTube channel where you get regular updates and regular live streams for families in intensive care who simply don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care.
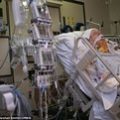
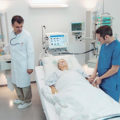
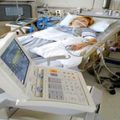
But let’s dive right into the topic. So again, assuming that you have a loved one in intensive care with COVID-19 with ARDS, a lot of patients that go into ICU with COVID-19 with a pneumonia can very quickly develop into lung failure/ARDS. ARDS stands for acute respiratory distress syndrome. At the end of the day it’s lung failure. So, up until COVID became a reality, some patients in ICU had ARDS/lung failure. And reality is from what I’ve seen, the way I looked after ARDS patients in ICU pre-COVID, not much has changed actually. That the change is that the majority of ARDS/lung failure patients at the moment that come into ICU are COVID-19 related, which puts a new spin to look at the situation of obviously the patients, the mortality rate of COVID-19 patients in ICU, which is basically the number of people that die in ICU from COVID-19 ARDS is around 40 to 50%.
Recommended links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
And bear in mind, COVID-19 first showed up in December 2019 in China. And here we are 18 months later or so. We’re just dealing with COVID-19 ARDS situations in ICU, and it’s all brand new. So all the research that is out there would probably change because it’s still new. So whatever data we’re getting at the moment is probably not accurate because there will be new treatment options. And just like there is a vaccine now, probably treatment options will be more effective going forward too, but we’re not there yet.
Anyway, cutting a long story short when patients go into ICU with COVID-19 ARDS, they might end up on BiPAP or CPAP to begin with for respiratory distress. That often isn’t enough. And then they get intubated with a breathing tube or an endotracheal tube, and they end up in an induced coma on sedation. They pretty quickly end up on inotropes or vasopressors because they’re hemodynamically so unstable with low blood pressure, high heart rate. They often show signs of sepsis very quickly, or even of a septic shock very quickly. Blood results are deranged. White cell count is high. Lactate is often going through the roof is very high. Oxygenation is dropping down. CO2 may rise, not necessarily, but oxygenation is probably drops down critically low, where then ventilation settings need to be changed to oxygen delivery of 100% through the ventilator. Patients become very unstable. For example, if someone is ventilated with 100% of oxygen with a high PEEP, and I don’t want to get too medical here, but some basics you may want to understand, high oxygen levels, 100% of oxygen as opposed to room air. Room is 21% of oxygen. The air that you and I breathe in is 21% of oxygen. So you can imagine, you need to go up to a hundred percent of oxygen, that’s how poorly ventilated the lungs are when someone is in ARDS/lung failure.
So when you look at chest X-rays of a patient with ARDS/lung failure, it’s a complete whiteout. And of course, no air is entering the body. And that’s why the mortality rate or the number of patients that are dying with ARDS is very high.
So then, common therapies for ARDS/lung failure in ICU are, to start patients on steroids. Dexamethasone, prednisolone, methylprednisolone, those are common ones. And that might help, but often what happens as well with ARDS/lung failure, patients will be started on nitric oxide, and that is in very small doses because nitric oxide as a chemical substance can be toxic as such, but in very small doses. And we’re talking about very, very, very small doses. We’re talking about nanoparticles or not sure whether that’s the right term even, but we’re talking about very small doses. So nitric oxide in small doses can actually help to open up some of the alveoli in the lungs and help with ventilating a patient. Other treatment options can be to start nebulizing with prostacyclin, also known as epoprostenol. That can help as well. Other treatment options can be sildenafil also known as Viagra tablets for pulmonary hypertension, which can sometimes happen with ARDS/lung failure.
So those are the most common options for treatment obviously at the moment because COVID is obviously a viral infection. A new drug has come up on the scene that’s being used for COVID-19. It’s remdesivir. It’s not a new drug, but it’s a drug that’s specifically used for COVID-19 ARDS in ICU. Whether it’s effective or not, I think the debate is still ongoing, but it’s certainly being used.
What we’ve also seen when working with ICUs directly, we have also seen the use of antibiotics. We have seen the use of antifungals because if the lungs are in such a bad shape, often secondary infections might occur as part of the COVID-19 ARDS/lung failure. So what might have started with COVID-19 may now have developed into a bacterial infection or a fungal infection. We were just working with a client recently where that has been the case. They were more or less in the end COVID-free, but they still suffered from the ARDS, but now they were dealing with all sorts of bacterial and fungal infections. So it’s definitely not a straightforward situation by any means having ARDS/lung failure for COVID-19 in ICU.
So if the conventional therapies or the therapies that have been known for many years are failing, the next step generally speaking is to start proning. Proning basically means you’re turning a patient by 180 degrees and you put them on their tummy. So the back of the lungs can be inflated and oxygenation of the lungs can be improved. I have seen this even 20 years ago for ARDS/lung failure. That was way before COVID obviously, but I have seen in my early days in intensive care that patients are being proned. And often very effectively, proning can work, but proning is also a lot of work. It also comes with a lot of undesired side effects. And I’m going to talk to about them in a minute.
So for example, picture this. So you’ve got your loved one in ICU. You’ve got them lying on their back or on their side. And while they’re lying there 24 hours a day, important parts of the lungs can’t get perfused because there’s just too much pressure just from lying on the bed. So by turning a patient on their tummy, head down, the back of the lungs is free and it’s easier to get oxygen into the lungs. But, as you can also imagine for someone that’s already critically ill, that is incredibly vulnerable, turning somebody on their tummy head down so that also secretions can drain out of the lungs because gravity is at work, that’s also very taxing for someone that’s already critically ill, which means they need a lot of sedation.
When someone is in an induced coma for the breathing tube, because it’s so uncomfortable, you can imagine how uncomfortable it is by turning somebody on their tummy with a breathing tube in their mouth, maybe in their nose, or even with a tracheostomy, if they have a tracheostomy already, it’s very uncomfortable. They need even more sedation. And the more sedation and opiates, pain medication, a patient needs in ICU, the more rapid they lose their muscle tone. They decondition very rapidly. So, you could argue that if prone position is saving a life and is improving the ARDS condition, what’s the price that patients are paying for this? And it’s certainly something that families need to be mindful of that the recovery may be possible, but what does the recovery look like then down the line if a patient can leave ICU alive. Can they go on to rehab? How strong are they? How weak are they? They are all questions that need to be considered in a situation like that.
Suggested links:
Another issue is with prone positioning in particular that I talked about sedation a minute ago, it’s often not enough. So what needs to happen for prone positioning so that the patient can tolerate that is they also need to be paralyzed. And there are medications that can be used to paralyze the patient completely so that they can’t move. But that again then increases the need for even more sedation because you don’t want the patient to be paralyzed by medication and then being sort of semi awake. It would be terrible. So it certainly comes with a lot of undesired side effects, and that is a challenge in and of itself.
The other challenge with prone position during ARDS is that the risk for pressure sores, while lying on your tummy, on your stomach is very high. You really have to cushion a lot of body parts with foam, with gel pads. From a nursing perspective, it’s really specialist’s skill, making sure that patients are safe and making sure that patients receive best care and treatment so that they don’t injure themselves. And again, I have seen proning to be very effective. You prone a patient for three days and all of a sudden ARDS can improve. If the antiviral, antibacterial, antifungal therapy is working, maybe you’re adding on a little bit of nitric oxide into the mix, a little bit of epoprostenol/prostacyclin nebulizer. You might add on some sildenafil/Viagra to the mix and it may work.
Well then you also have the issue when someone is lying head down, proning, a patient in ICU should be started on nasogastric tube feeds as quickly as possible. And then you have the issue. If someone is lying on their tummy, head down, you have the issue that feeding may not be able to be tolerated because they’re facing head down and they are facing head down and they can’t absorb feeds, and the risk of vomiting aspiration is real. And those are all the risks that you need to consider.
Moving right along if ARDS/lung failure can’t be treated with prone positioning, the next step is ECMO. That is ECMO, or I should say VV-ECMO? ECMO is a bypass machine. It can take over the function of the lungs and of the heart temporarily. For ARDS, you need VV-ECMO. It’s for lung failure. And basically a lot of patients in ICU where prone positioning isn’t working for lung failure simply need to go on ECMO. Now, the problem is that not many ICU’s have ECMO available as a treatment option. I would say one, maybe two out of 10 ICU have ECMO available. So it’s a very scarce resource.
Recommended:
So when I first started in ICU in the late 1990s, early 2000s, there was no ECMO. So if proning didn’t work, there were no other choices, and for the patients where proning didn’t work, they often passed away unfortunately. Nowadays ECMO is an option. A lot of families in intensive care don’t know about ECMO. So we have many families in intensive care come to us and say to us, “Look, my mom, my dad, my brother, my sister, my spouse is in ICU with ARDS and they’re being proned and it’s not working.” And then I tell them, “Well, what about ECMO?” And then they have never heard of ECMO. The ICU hasn’t told them about ECMO, which is again, why I keep saying families in intensive care don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. And they also don’t know their rights. They don’t know how to manage doctors and nurses in intensive care. Can’t say this often enough because it’s so true. And now you can understand that the families are not being told about ECMO as a treatment option for ARDS. They’re being misled. ICUs are not transparent, and yes, it often does take a transfer to another ICU if ECMO is an option. Okay. So let’s just say you’re in New York and you are in a hospital where in a smaller ICU and your loved one is being proned but he or she is not improving. And then you come to us and I tell you, “Well, have you considered ECMO?” And the ICU is telling you, “Well, ECMO is not an option. We don’t have ECMO. Transferring your loved one to another ICU is not possible, blah, blah, blah.” Well, I dispute all of that. If you don’t ask, you don’t get.
The biggest challenge at the moment with ECMO is probably that, again, now that you understand that more patients go into ARDS/lung failure with prone positioning, ECMO beds have been in high demand before COVID-19. And now the demand for ECMO has just simply gone through the roof. And with ECMO, it’s such a limited resource because A, it’s a machine, it’s a very expensive machine. That’s number one. Number two, you need intensive care doctors, intensive care nurses, respiratory therapist. All the health professionals in ICU are highly specialized, highly trained, and now you need ECMO and you need to do another training to look after ECMO.
I’ve done ECMO training while I was working in ICU. And I’ve looked after many patients on ECMO, but there is a fair amount of training you need to go through to be able to look after ECMO patients. So it’s not only a case of do we have an ECMO machine? It’s also a case of, do we have the doctors, do we have the nurses to look after the ECMO 24 hours a day for prolonged periods. And that’s why it’s such a scarce resource, but it also saves lives. So those are the options available for ARDS/lung failure for COVID-19, but also for ARDS/lung failure not caused by COVID-19. It’s an option that’s available for anybody with ARDS/lung failure irrespective of what’s caused it.
Recommended:
So other things, other risks that are coming into play when patients are in ICU with COVID-19 and ARDS is that they often develop a septic picture and they might even go into septic shock, which is often life-threatening. Other issues are that other organs besides the lungs can be impacted very quickly. That starts from the heart. Kidneys are often very impacted very quickly because of hemodynamic instability, which means blood pressure is dropping. If the blood pressure is being dropped for a prolonged period, it means that the kidneys might not get enough perfusion, and that puts them into acute kidney failure. And then the patients on ARDS often end up on dialysis/hemofiltration. Okay, this can be managed, but it’s just an added on complication that nobody really needs, but often happens in ICU unfortunately.
Other organs that can be impacted very quickly are the liver as well because patients end up on so many medications while they’re on ARDS and in ICU specifically that the liver may be impacted as well. The heart can be impacted simply because it’s sitting next to the lungs. If the lungs are not getting perfused because of the lung failure, it’s difficult for the heart to keep pumping blood around and therefore the heart can go into failure too. Other issues are, the lungs are already impacted, but there can be interstitial lung disease that can be fluids on the lungs. It’s really a catch 22 when someone is in ARDS/lung failure.
And what I have seen over the years really is you can’t cure ARDS in just a few days. Often ARDS patients are in ICU for prolonged periods of times, and it’s often touch and go quite literally. For example, what I mentioned before, when you prone a patient, when you turn them just to give that back a wash, when you change linen and so forth, patients can be so unstable that just turning them, you need three, four people. You need to prepare for it in much detail. You got to make sure they’re getting enough oxygen while you turn them. It’s almost like a life or death situation just turning them, making sure patients can tolerate that and are not going into a cardiac arrest or not deoxygenating where oxygen levels don’t drop to a dangerously low level. So it’s a real art just looking after a patient, just on a nursing level.
So then what’s also important when a patient is in ARDS/lung failure is you’ve got to monitor the blood every day. You got to monitor chest X-rays every day. You got to monitor arterial blood gases four-hourly making sure that every change you’re making, whether it’s in the patient’s ventilation, whether changes are happening with position of a patient is not impacting on the ventilation strategy straight away. The devil is so much in the detail. It would go way beyond this 30-minute video that I’m shooting here to look at all the fine aspects where you need years of training to understand and putting the puzzle together.
Again, that’s why I keep saying that the biggest challenge for families in intensive care is that they don’t know what they don’t know. When someone is critically ill, especially with ARDS/lung failure, there are dozens of things happening simultaneously. And unless you really look at them in detail and you understand them in detail and you’re putting together the puzzle, it’s very difficult for you to make sense out of this particular situation.
Another thing that I would like to mention is a lot of patients in ARDS/lung failure are on anticoagulation, such as heparin, because any patient that’s immobile is at high risk of developing a deep vein thrombosis/embolus. And that’s why patients are on heparin, but that’s also increasing the risk of bleeding. When someone goes on ECMO, they are also on heparin on even higher doses of heparin. And there are side effects that come with that, which is an increased risk of bleeding. It’s an increased risk of sustaining stroke.
So, as much as you’re trying to push forward with treatment and therapy when someone is in ARDS/lung failure, you got to watch for the side effects as well. Other side effects are most patients in ARDS/lung failure are on inotropes or vasopressors, such as norepinephrine, Levophed, epinephrine. In the UK and Australia it’s mainly known as noradrenaline, adrenaline, vasopressin. And those are vasoconstrictors. And vasoconstrictors means basically they’re constricting the skin. They’re constricting the blood vessels, which means patients are at a very high risk of sustaining pressure injuries. And if patients sustain a pressure injury while they’re in an induced coma, while they’re in ICU, the risk of them getting another infection is very high.
And again, it keeps coming back to what I said before. Patients are so difficult to be turned on their side or on their tummy. It is very, very difficult to keep the balance of the patient, making sure we can heal the lungs, but also making sure they’re not sustaining any other injuries that puts them at danger, such as a pressure injury. So, as I mentioned, a very fine line for those patients in ICU between slowly moving them to improvement, but also not causing any more damage from all the side effects from the treatment. It’s a very fine line.
Other issues are that when someone is in ICU with lung failure/ARDS, as I mentioned briefly, the length of stay for these patients in ICU is very long. I have seen patients staying in ICU probably for up to six to eight weeks. So if an ICU team comes to you and says, “Hey, your loved one has ARDS/lung failure COVID-induced, we should be withdrawing treatment, and we should let nature take its course, and we should let your loved one die” because the argument from the intensive care team is often, well, they won’t have any quality of life anyway if they survive that, again, from experience timelines vary and withdrawing treatment from my perspective is never an option. If your loved one wants to live, if you want for your loved one to live, time is just an artificial constraint.
Suggested links:
If ICUs are asking for withdrawal of treatment, it’s often because they need the beds, they want to save money and they don’t necessarily believe that a patient will have any quality of life down the line, but that’s not for the ICU to say. ICUs are very poor predictors at quality of life outside of ICU. And that is something you need to keep in mind, and you need to keep pushing for what you want.
But I also want to open up the floor now for any questions for the people that are on the call or that are on the video. What questions do you have specifically to ARDS and COVID-19 in ICU? Please type your questions into the chat pad. I’d love to answer them.
While I’m waiting for your questions to come through, I also want to quickly hone in on a ventilation strategy when patients are in ARDS/lung failure. So basically often what happens is patients are being ventilated. Patients are often being ventilated in a pressure control ventilation mode. I don’t want to go into too much detail, but basically there’s pressure control ventilation in ICU and there’s volume control ventilation. It makes a lot of sense to ventilate someone with a pressure control ventilation because that simply limits the risk of a barotrauma or a pneumothorax. It basically limits the risk of punching a hole in the lung quite frankly.
There is also in recent years, it’s a bit more old fashioned now, but there’s also the option of high-frequency oscillation ventilation. I’ve seen that as well. You can use that before you prone someone. It depends. Some people it’s effective. For others, it isn’t. It’s basically increasing the respiratory rate, the breathing rate up to a hundred breaths per minute. It’s giving short breaths, hopefully improving the perfusion in the lungs, increasing the oxygen intake in the lungs.
Other ventilation strategies are simply when someone is on VV-ECMO for the ARDS, it’s simply actually minimizing the pressure that’s going into the lungs because that gives the lungs time to rest and heal, which is the whole strategy for ECMO bypass machine or ECMO machine is taking over the function of the lungs. And it’s giving the lungs time to rest and heal. When someone is not on ECMO, they are also on a very high PEEP. Basically a PEEP is the pressure at the end of inspiration. It’s often very high in ARDS up to 15, up to 18 mmHg, and it just keeps the alveoli open. It just keeps the lungs open for perfusion. And that’s not always said to be effective because ARDS is such a critical illness.
Helen, you’re asking, “Outside of COVID, how does a patient get ARDS while hospitalized?” That’s a good question. It’s pretty much unknown. A lot of patients that I’ve seen with ARDS in ICU pre-COVID, they often come in with what might be considered a community acquired pneumonia, and then it develops into a full blown ARDS. Again, it then comes down to, is it caused by a bacterial infection? Is it caused by a viral infection? Is it caused by a fungal infection? At the end of the day, COVID is also a community acquired infection very much so. So that hasn’t really changed because ARDS is often caused by an infection, and yes, some patients might even get the infection while they’re in hospital, but most often they get it in the community through transmission from another person.
Recommended:
So, yeah, those were the ventilation strategies that I just wanted to quickly focus on. Usually pressure control ventilation mode, and then high PEEP, high levels of PEEP, high oxygen delivery up to 100%, the nitric oxide that I mentioned earlier, the prostacyclin, nebulizer, and potentially sildenafil/Viagra as treatment options. We talked about antivirals such as from Remdesivir. We talked about antibiotics. We talked about antifungals. We talked about the steroids that are often being given. Sometimes bronchoscopies can be done as well to suck out the mucus. But if someone is already on a hundred percent of oxygen and they are getting a bronchoscopy, it may not be safe because there’s even less oxygen going in while doing a bronchoscopy. So you really got to weigh up what’s safe for a patient.
Helen, you’re also asking, “Can a patient get it from being on a ventilator? Yes, they can. So you might’ve heard the term of ventilator-associated pneumonia. So when someone is being ventilated in ICU, in ICU, the risk of a ventilator-associated pneumonia also known as VAP is real. And that can also develop into ARDS. Yeah. The reality is this, Helen, if someone is on a ventilator in ICU, the risk for complications is just going through the roof. That’s why you only want to ventilate someone as a very last resort. Very last resort.
Are there any other questions before I close this topic for today? And while I’m waiting for any more questions to come through, I just want to close with saying thank you very much for joining me in this live video. They are trying times at the moment for families in intensive care. They’re trying times for everyone in the community. Lockdowns are still real. ICUs are overcrowded at the moment and families can’t even visit, especially when their loved ones are in ICU with ARDS and COVID obviously to keep them free of COVID. Very trying times at the moment.
RECOMMENDED:
Again, I want to thank you for coming onto the live stream. Please also check out intensivecarehotline.com for tips and strategies for families in intensive care. Obviously, if you want more of my time, if you want to talk to me directly, I have a free 15-minute consultation call available for everyone. After that, I do have paid consulting and advocacy options. I have other people on my team that work with me, have other people that work with me on my team that can help you as well. I also have an online membership for families in intensive care where you have access to me, my team, and to other families in intensive care online. And I would love to see you on any of that.
Helen you’re asking, can I discuss aspiration pneumonia next week? Yes, I can. Yes, I can. I’ll see what else I’ve got. If I don’t discuss it next week, I will discuss it the week after. I’ve got a whole list of topics that I want to go through. I will consider it. Helen, if it’s not next week, it’ll be the week after. Yeah. Well, thank you so much again for coming onto this live stream. I want to close off by saying thank you again, and please stay safe. Stay out of, stay away from COVID. Stay safe. I hope you and your families are well. And I wish you a wonderful weekend. Thank you for all your support. Take care for now.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!