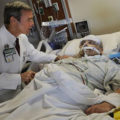
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
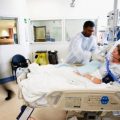
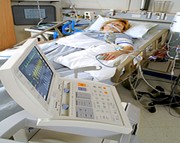
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ariel, as part of my 1:1 consulting and advocacy service! Ariel’s sister is with a breathing tube on a ventilator in ICU with acute pancreatitis. Ariel is asking if a meaningful recovery is possible for his sister with this condition.
Is a Meaningful Recovery Possible for my Critically Ill Sister in ICU with Acute Pancreatitis?
Patrik: Hello, is this Ariel?
Ariel: Hi there Patrik.
Patrik: Hi Ariel. Your sister is in ICU.
Ariel: Yes, she is. My sister. Yep. But that’s not my sister in that ICU, in my opinion there’s a body in there that’s not my sister.
Patrik: Oh, I see.
RECOMMENDED:
Ariel: So they’re right now debating doing the tracheostomy and I watched your videos. I do my bodywork and I do energy work, but this is out of my scope of practice. The clients that come to me, they have mostly psychological issues, as well as orthopedic stuff. If they’re having chest pain, I tell them to go to the hospital. And they may do some rehabilitation with me, but down the line. So I’m the only one in the family that has any medical knowledge at all and I feel like they get mad if I tell them what’s going on, but at the same time… So my sister’s spouse died two years ago at the age of 46. He’s older than me. It’s a lot of grief. And then she had blood pressure issues. And then she ended up going in with a stomach ache and acute pancreatitis and every complication you can have with that, everywhere.
Patrik: Yeah. I’m seeing that from your email.
Ariel: Yeah. Okay. I did write it. It just gets worse. They closed her up… I don’t know, you probably know what they did to her. Her belly was giant so they took the fluid out. They just closed that up and the next day they’re hitting us with the tracheostomy.
Patrik: How many days in ICU?
Ariel: So it’s two weeks in the hospital so maybe, I don’t know, 12 days.
Patrik: 12 days. And now they are basically saying to you tracheostomy?
Ariel: Yeah.
Suggested links:
Patrik: Or are they saying to you tracheostomy or stop life support? Are they’re saying that as well?
Ariel: No. So here’s the thing. This is the opposite of what I’ve noticed that you deal with.
Patrik: Oh yeah. Yes.
Ariel: The ladies are looking for some hope. So they’ll ask some questions like, “So if this was your mother, what would you do?” And the doctors are like, “We’d give it another couple of days.” I’m kind of seeing there’s money involved in this.
Patrik: For sure.
Ariel: With insurance too. This is just not realistic, but I think there’s liability with them. I’m reading the notes and the notes are where it’s at, but then not going to put the notes… We went through this with our parents and she had a great fear of ventilators, like everybody else but she’d never wanted this. She’s never been in a hospital, she’s never had anything wrong with her. It’s crazy.
Patrik: How old is your sister?
Ariel: She just turned 70, believe it or not.
Patrik: Does your sister have a documented advanced care directive?
Recommended:
Ariel: This is the problem. Yeah.
Patrik: She does?
Ariel: Yeah. Her eldest daughter has it and it says, technically what you always say is the burdens of treatment outweigh the quality of life. It clearly said that she would like pain relief and it’s kind of written like if I have one or more diseases. And they’re not seeing it that way. They’re like, “Well, if the pancreas is better, everything will be better.” But I know that’s not true. Her kidneys are failing. I’m seeing it as if she went home on a ventilator with tracheostomy. She’s a lot like me. I’m a little upset right now but she’s very active. Okay, maybe not as active as me. Anyway, tracheostomy, they did a PT consult. Give me a break, like talking about money here. And they’re talking about long-term rehabilitation and dialysis and probably a wheelchair. So I don’t know. Her soul is out of her body. This is how I go. She wants to live. So she has three children and one is speaking as I am. She’s like, “I can’t even go anymore, and it’s like looking at an open grave.” And the other daughter is being babied. And then there’s the daughter that has to make the decision.
Patrik: Look, I’ll give you my take. Your email is fairly good. You seem to have a good understanding what’s happening there. Look, from my experience, there’s probably a 50-50 chance for her to survive. We’re talking about survival, we’re not talking about quality of life. We’re talking about survival. We’re talking about her leaving intensive care alive. We’re not talking about what does that look like? What are the long-term implications of that? Now, you’ve got to understand this though, ICU professionals, doctors, nurses are very poor at predicting what’s happening outside of ICU besides death.
Ariel: They have one job, right? Which is to keep people alive.
Patrik: They have one job which is to save lives, that’s their job. They are highly unaware of implications of their jobs, of what they’re doing really well, which is saving lives, okay? I’ve worked in this environment for 20 years, but I believe I’m also highly qualified to talk about what’s outside of ICU. The reason for that is we’re running a service and full disclosure, I am in Melbourne, Australia. We are running a service here in Melbourne, INTENSIVE CARE AT HOME. We are looking after long-term ventilated patients at home. So we know what it looks like on the other end. Now I’m not.
Ariel: Special insurance…
Suggested links:
Patrik: Insurance and how who’s paying for it, that would be a whole another discussion in and of itself. Quality of life, what is it? It’s a term that is difficult to qualify for the individual. So it really comes down to what is acceptable for the individual, what is acceptable for the family, what services are available on the other end. Is there even a chance for your sister to fully recover? I would argue that either I am, or the ICU professionals that you’re dealing with at the moment are qualified to say what the recovery will look like if it gets to that point.
Ariel: I can’t even imagine that she would be who she was when she walked in there. It doesn’t make sense.
Patrik: It does. And she probably won’t be. The question is, can she live with a quality of life that is acceptable for her and for your family? I guess that’s what it comes down to and nobody would have a crystal ball to say.
Ariel: It’s funny she and I and my other brother, we’ve had these conversations. I’m like, “Hey, why do you put the wrong person as a proxy?” She’s talked to me about this. She wouldn’t want a ventilator, never. She never wants to be dependent on anybody. She’s completely healthy, mostly. She wouldn’t want any of this. My father, he checked out. He had COPD, he didn’t go to the nursing home. My mom did. So we had these conversations. People probably don’t have them with their kids, but quality of life, she needs to be independent. Goes to football games and walk her dog. She doesn’t want to be just the person in the corner..
Patrik: In a wheelchair.
Ariel: Yeah. The doctors won’t say these things to them.
Patrik: No, they won’t. What I will say though, is 12 days in ICU is not a long time.
Ariel: No, it’s not.
Patrik: The way I look at these things is there’s plenty of time to talk about end of life. There’s no hurry in starting the discussions about end of life. If in another 12 days’ time, things are still looking bad, well, let’s start the discussions around end of life. But I believe it’s a little bit too premature to say we’re pulling the plug, for lack of a better word.
Ariel: But I wouldn’t put her on the ventilator to begin with, but that’s a different story. It’s a steady decline and this belief that if her pancreas is better, but it isn’t producing insulin and it’s necrotic. They think that that will magically make all the other organ systems be fine. And we know that to be not true.
Patrik: No, I think if anything, it’ll make the other organs fail.
Ariel: So, I’m in a bad position because I’m the only one with the truth or some amount of truth. There are other people in the family, but everybody’s scared to say anything. One of her daughter is onboard. I don’t know, do you really think it’s premature to say it. This is making me nauseous. Yeah. Okay.
Patrik: Look, I’ll tell you what a tracheostomy will do. It’ll buy your sister time to either improve or not. She needs to have a tracheostomy if she wants to live even if it’s for another two weeks, the tracheostomy is inevitable.
Ariel: But she’s not awake. They put her in the-
Patrik: That’s exactly the point why she needs the tracheostomy. That’s exactly the point.
Ariel: Regarding the coma thing, she’s not in an induced coma anymore. She’s just not awake.
Patrik: Yeah, sure. How many days ventilation?
Ariel: Maybe 10. I don’t know.
Patrik: Yeah. So she’s at the point now sort of 10 to 14 days. You got to look at the trach or no trach.
Ariel: So you’re used to knowing another way, right? You’re used to fighting for people to be able to have these treatments?
Patrik: I am surprised what I’m hearing from you in terms of what the doctors are telling you. Nine times out of 10, the doctors are the ones pushing for end of life.
Ariel: Really?
Patrik: I’m surprised what I’m hearing from you.
Ariel: To be honest with you, I haven’t heard that myself, it’s not in their reports. It’s what the kids are saying. We had one family meeting and they refused to give odds. They did what you said, the 50-50 chance of her living or dying. But I don’t even think it’s that much chance. And it’s a recurring thing too.
Patrik: Look, normally we are a professional advocacy company, really. If anything, we are advocating, but we can also advocate for end of life, if that’s how you feel but most of the time we are advocating pro-life.
Recommended:
Ariel: I thought so. Do you think I’m awful? I think it’s just that because-
Patrik: No, no, I don’t think you’re awful.
Ariel: I just know where it’s going, I just know. Have you seen in this description of illness that acute pancreatitis and that much progression anybody really recover? That’s the kind of questions they’re asking.
Patrik: I don’t like when I hear necrotic pancreas. That’s confirmed?
Ariel: Yeah.
Patrik: Right. Necrotic pancreas is something that I would argue from experience, there’s definitely a higher mortality with that compared to other… You’re talking in your email ARDS. ARDS has a high mortality rate but I wouldn’t… Necrotic pancreas from experience has a higher mortality rate than ARDS.
Ariel: And then the compartment syndrome and then the kidneys and then she’s got lung issues now and she’s in atrial fibrillation and it just continues. Her blood pressure, three different blood pressures, that’s new for me to know. She really got hit with it. And then complex brief on top. Of course I’m a spirit person, so I don’t know. What I would be asking is for you to explain to them with your credentials that this is what the likely outcomes are from each of the different conditions. They’re hearing me but… Then these doctors are pissing me off. They’re like, “Oh, there’s hope.” One of her tests, let’s say which isn’t really cheap, but it comes back a little bit better. They’re like, “Oh look, this is great.”
Patrik: Their hope would be based on getting her out of ICU alive without looking at what does it look like down the line. That stats are 90% of ICU patients survive so the odds just on the survival level are in a patient’s favor. But again, it’s not talking about quality of life, it doesn’t talk about what it looks like. It’s just looking at can we get a patient out of intensive care alive?
Recommended:
Ariel: Okay. I don’t know if it’s true because I didn’t hear it, they said, “What are the odds of her walking out of here?” I’m like, “She’s not walking out of the ICU.”
Patrik: She’s not walking out of ICU.
Ariel: She’s not equipped to fight this battle either. They’re looking at it like a freaking football game. So you think maybe I just got to give them more time, but my take on it is that she’s clearly feeling things and suffering and she’s in deep sacrifice, and now they cut her throat out. For what? And that is where the burden of treatment versus quality of life.
Patrik: I guess because you are saying you are a spiritual person and I believe I’m a spiritual person too, you could take the argument and that can be important for some families, not for all families. Does she need to live for another few weeks to have more time with you that you and your family can come to terms? I don’t know. I can’t answer that question for you.
Ariel: Got it. Yeah. She’s not communicating. So is it true that people can communicate when they’re on the tracheostomy better than with the-
Patrik: Better than with a breathing tube, if they are awake?
Recommended:
Ariel: Yeah. She was on the breathing tube for one day and awake and writing on a whiteboard. And then the next day they had her in the induced coma. I’m not sure what happened, but it happened.
Patrik: Look, it would also be nice probably to get your sister to a point where she might be more awake and where you can ask her the questions that you’re asking me now. That could be the best.
Ariel: She’s in terrible pain. I guess it’s one of the most painful thing. Then they just… I said, gutted her, I shouldn’t say. They just cut her open and then sealed it up with some kind of, I don’t know what it is.
Patrik: Probably.
Ariel: To drain the fluid. She gained 25 pounds in two days.
Patrik: Oh my goodness. So she’s got an open tummy with a dressing on it?
Ariel: It was open and now they have closed it. They put some, I think mesh in there and a drain. It’s hard to get info out of the doctors. They want consent for things, but they talk to… I pushed them, you probably figured that out by now and I’m reading the records, but they talk to them in layman’s terms, which I guess they should. But maybe understanding it better would help them too, but they’re really saying she’s going to be alive. You’re right, that’s a good point. She’s going to be alive, but she’s not going to be who she was. I keep trying to say that nicely but it’s hard.
Patrik: Is your sister or your sister’s children, religious?
Ariel: No.
Patrik: Because Catholic families, for them, life is sacred and they would do whatever.
Ariel: Yeah. Life is sacred, I know that the spirit lives on, but I think people are looking at it, they want that back and I understand, I’m very compassionate. I’m not talking like this to them, but again, what would she want is more important to me at this time. It’s been really awful.
Patrik: I can imagine. I was just about to ask, have you or your family ever seen anything similar with families, friends before?
Ariel: I have. Their father just died more than a year ago, in a different situation, but he had been in the ICU, but they were sheltered from that. Yeah. I’m the person that holds people’s hand as they die. It’s sad that I do, but not a lot. I’ve seen it, but not like this. She walked in and now, boom. And of course I’m used to it. And again, I’ve had these conversations with her and the husband so…
Patrik: Yeah. Look, from my perspective, and again, having done this for a long time, you do what you can, you try. If it succeeds, great. If it fails, it fails. I guess that’s probably where the 50-50 odds come in. But again, if you succeed in keeping someone alive, ICU’s are very poor at predicting what does it look like six months down the line if people survive? They have no idea.
Ariel: Yeah. We can’t tell. But science tells. I’m looking at the research. I don’t know if this is true, tracheostomy. In her age group, and there’s not great records either, but with this acute necrotizing pancreatitis, it’s not a good situation.
Patrik: With ARDS, she doesn’t have COVID. Does she?
Recommended links:
Ariel: No, she had just interestingly gotten this shot about a week and a half before.
Patrik: Oh my goodness.
Ariel: She didn’t have COVID. They test her all the time, but she didn’t have it. It’s so weird. It mirrors it though the way that this has gone. And it was just big as.. I’ve been so close to her my whole life, but especially since her husband died, I’m the one that’s been talking to her every night. And so she just cycled through. We talked about ventilators for like, I don’t know, almost two months.
Patrik: Really? Conscious of the time, what I can definitely offer you is to get on a call with you and your nieces and with the doctors and find out a little bit more, what is exactly happening? I can definitely offer you that.
Ariel: Okay. I told them I was going to contact you and meet with you. And they were like, “Yeah, okay.” I’m like, “Who’s paying for it?” She has the money, I think. Brenda can get at it. But my only concern is you are in Australia and thank you for saying that. And also, as I watch your videos, I respect what you do, but it’s actually the opposite of probably what we need.
RECOMMENDED:
Patrik: The opposite of what you probably want. And I can accept that. I can advocate for you one way or another. If you feel like she’s suffering, she doesn’t want to live. And especially if there is an advanced care directive, then the advanced care directive needs to be followed. In terms of, just very briefly, I’m talking to people from different parts of the world.
Ariel: And you could go over the conditions with them and not have to deal with it later. I don’t want them to hate me because I’m telling them what’s real. Doctors are not doing that.
Patrik: No, they’re not.
Ariel: It’s unfortunate. And if they are, I don’t know about it. So let me talk to the girls, especially the one that’s the proxy and I will email you and I appreciate your time.
Patrik: Please.
Ariel: Yeah. Thank you, Patrik.
Patrik: Okay. You’re welcome. All the best for now. Thanks Ariel. Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!