Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can My Mom With Tracheostomy Have A Quality Of End Of Life?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
TRACHEOSTOMY IN KIDS (Part 1)
Over the last decade, tracheostomy has been increasingly performed in children, aligned with the improvements in neonatal and pediatric ICU care. Nowadays, the majority of children with tracheostomy represent a very complex cohort of patients with sustained reliance on tracheostomy and related medical technology for long-term survival.
WHAT IS A TRACHEOSTOMY?
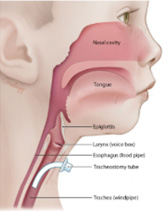
The term tracheostomy is used to describe a surgically created hole in the neck that extends to the trachea (windpipe) to allow for safe breathing. A tracheostomy tube is the plastic breathing tube that is placed into the hole.
WHY YOUR CHILD NEEDS A TRACHEOSTOMY?
Your child’s doctor will talk with you about why your child needs a tracheostomy. The length of time your child has a trach tube depends on the reason for the trach tube. The tube helps breathing and helps clear mucus from the airway.
The more common reasons for a tracheostomy are listed below.
- A blockage in the upper airway: if the upper airway is blocked, air cannot get into the lungs. The trach tube helps your child breathe.Paralyzed vocal cords may also block the upper airway. When the vocal cords do not open, air does not get through and the child cannot breathe. The trach tube lets the child breathe normally.Other conditions that may block the upper airway include polyps; narrowing of the trachea; or weak muscles in the trachea. When the muscles in the trachea are weak, the trachea closes and blocks airflow.
- Inability to clear mucus from the lungs and airway: lungs make mucus. Mucus cleans the lungs by picking up tiny bits of dirt and dust. Cilia, which line the lungs, help the mucus carry the dirt and dust out of the lungs. This protects the lungs from irritation and infection.Some children are not able to cough mucus out of the lungs and airways. If mucus stays in the lungs, the child is more likely to get infections. The trach tube provides a way to help clear mucus from the lungs.
- Long-term help with breathing: A trach tube is put in when a child has to be on a ventilator for a long time. Your child may have to use the ventilator at home after the trach is placed. There are many reasons why a child may need long-term help with breathing. You need to discuss this with your child’s doctor.
IS A TRACHEOSTOMY PERMANENT?
For most children the tracheostomy is not permanent. The length of time it stays in place depends on the individual patient and the reason it was initially placed.
Although some tracheostomy tubes stay in place for many months or years, many are temporary and can be removed after a shorter period of time.
After the tracheostomy tube is removed, the hole frequently closes by itself. If it does not close by itself, the hole can be surgically closed.
TRACHEOSTOMY PREOCEDURES IN PEDIATRIC POPULATION
Differences in Pediatric and Adult Upper Airway: Kids Are Not Small Adults
When planning the approach for tracheostomy placement in infants and children, it is important to first address the differences in adult and pediatric laryngeal anatomy. Both anatomic and physiologic characteristics of the infant trachea require special surgical techniques and adequate postoperative care.
Anatomy.
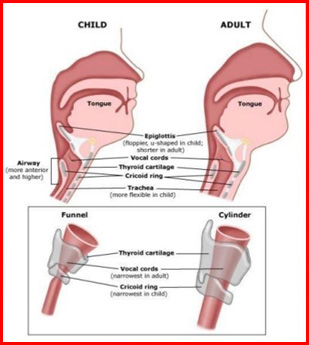 Infants have shorter and fatter necks than adults. The adult larynx is positioned at the sixth or seventh vertebra. The hyoid frequently overlies the thyroid cartilage notch, making palpation of anatomic landmarks difficult at times. The infant thyrohyoid membrane is also much shorter. The cricoid cartilage is the narrowest part of the airway in a child; in adults, it is the vocal cords.
Infants have shorter and fatter necks than adults. The adult larynx is positioned at the sixth or seventh vertebra. The hyoid frequently overlies the thyroid cartilage notch, making palpation of anatomic landmarks difficult at times. The infant thyrohyoid membrane is also much shorter. The cricoid cartilage is the narrowest part of the airway in a child; in adults, it is the vocal cords.
Physiology.
The cartilages of the infant larynx are softer and more pliable than in adults, with a tendency to collapse if pressure is placed on them. The mucosa of the supraglottis and subglottis are lax in infants and thus more prone to edema when inflamed or injured.
Indication.
It is important to be aware of the indication for placing the tracheostomy in a child. If a tracheostomy is being placed for upper-airway obstruction secondary to abnormal anatomy, such as subglottic stenosis or complete tracheal rings, entry into the airway may be difficult, with risk of damage to the posterior tracheal wall.
HOW IS A TRACHEOSTOMY PERFORMED?
The tracheostomy procedure is performed in the operating room under general anesthesia. A small incision is made in the skin overlying the trachea in the middle of the neck. The surgeon exposes the airway and makes a small incision into the trachea. The tracheostomy tube is placed in the hole, and secured to the neck.
WHAT ARE THE EFFECTS OF TRACHEOSTOMY?
The specific effects of the tracheostomy tube will depend on the age of the child, the reason the tracheostomy tube was placed, and the need for long-term ventilation. It is important that you discuss your child’s tracheostomy and the effects of the procedure with your child’s surgeon.
When a tracheostomy is present, care must be taken to prevent water or sand from getting into the tracheostomy tube (no swimming.) As a general rule, the tracheostomy tube will not keep your child from being able to eat normally or use their voice, although some children may not be able to eat orally or speak for other reasons. Many children with a tracheostomy tube are able to lead happy lives.
WHAT ARE THE COMPLICATIONS OF TRACHEOSTOMY IN CHILDREN?
To ensure adequate function of the tracheostomy, and to minimize potential complications from the tracheostomy, proper care and maintenance is important.
Adverse related tracheostomy events can be divided into those occurring “early” (including the perioperative and immediate postoperative period) and “delayed”. It is important that adverse events be quickly recognized and addressed to prevent devastating consequences.
EARLY COMPLICATIONS:
- Air leak
- Pneumothorax, pneumomediastinum, or subcutaneous emphysema. These complications are most often caused by technical errors during surgery. Despite all precautions to prevent these complications, they still may inadvertently occur. A chest radiograph should be routinely performed when the child returns to the ICU following tracheostomy to check the status of the chest.
- Injury to surrounding structures. The cricoid cartilage and tracheal landmarks need to be clearly identified before making an incision in the trachea, to prevent inadvertent incision into the cricoid cartilage, which could result in subglottic stenosis. Injury to both the esophagus and recurrent laryngeal nerves has also been reported and can be prevented by careful surgical technique. Esophageal injury is also more likely to occur if there is a nasogastric tube in the esophagus, with the esophagus being accidentally mistaken for the trachea.
- A false passage may be easily created upon initial insertion of the tracheostomy tube. Especially if the incision in the trachea is too small or the tube is aggressively pushed against resistance. Posterior tracheal lacerations may be caused by a similar method. If the tracheostomy tube is the incorrect size and is too large, it may cannulate a main bronchus. It is important to always assess the position of the tube in relation to the carina with a flexible tracheoscopy immediately after it is placed.
- Airway obstruction
- Mucus plugging. Can be prevented by adequate humidification, tracheostomy cares with routine suctioning. Constant supervision of a child with a tracheostomy tube is required to prevent plugging.
DELAYED COMPLICATIONS:
- Accidental decannulation. Can occur in the immediate postoperative period, and the consequences may be tragic. It can commonly occur as the patient is being moved from bed to bed to travel to the ICU. The presence of stay sutures, especially in a very small infant, will help with replacing the tube through the fresh stoma. Accidental decannulation can be prevented by correct tracheostomy tube selection and placement, ensuring that the tube is adequately secured, and by stable patient positioning.
- Stomal Problems
- Granulation Tissue. Develops secondary to the friction and movement of the tracheostomy tube or chronic inflammation. It usually responds to local wound care and more frequent tracheostomy tube and dressing changes. Treatment is topical antibiotic, and steroid ointment is sometimes required. Occasionally, silver nitrate cautery is required to control granulation tissue
- Tracheocutaneous Fistula. A tracheocutaneous fistula may develop when a tracheostomy orifice epithelializes during a prolonged course of healing or undernutrition.
- Tracheal Lesions. Suprastomal Granuloma, suprastomal collapse, subglottic stenosis
- Hemorrhage. Perioperative hemorrhage may be prevented by meticulous attention to hemostasis throughout the procedure. Bleeding often stops spontaneously but can occasionally persist, and it is important to address it with cautery before the tracheostomy tube is placed. Coagulation abnormalities should be ruled out in any child undergoing tracheostomy, especially those with chronic liver disease and thrombocytopenia secondary to sepsis, and abnormalities should be corrected before surgery if possible.
- Tracheoesophageal Fistula. The TEF is another complication among patients with tracheostomy tube. This complication is due to high cuff pressure or direct mechanical trauma. TEF is very rare; its rate of incidence is about 0.5%.
- Swallowing Problems.
NEWLY FORMED SURGICAL TRACHEOSTOMIES
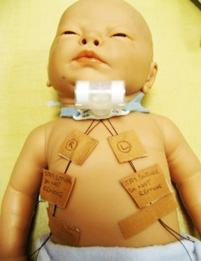 Stay sutures are placed in all surgical tracheostomies. They are placed through the tracheal wall on either side of the midline and left long, secured to the child’s chest and labelled Left (L) and Right (R) with DO NOT REMOVE or STAY SUTURES and are to remain in situ until after the first tracheostomy tube change (day 5-7).
Stay sutures are placed in all surgical tracheostomies. They are placed through the tracheal wall on either side of the midline and left long, secured to the child’s chest and labelled Left (L) and Right (R) with DO NOT REMOVE or STAY SUTURES and are to remain in situ until after the first tracheostomy tube change (day 5-7).
In the event of an emergency tube change during this period, traction is applied to the sutures (upward & outward) to hold the stoma open to facilitate the insertion of a new tracheostomy tube or endotracheal tube.
PLACEMENT OF CHILDREN WITH TRACHEOSTOMIES
Children normally recover from the operation quickly. Your child will need to stay in an intensive care unit to make sure the first tube can be safely changed (normally between five and seven days after surgery). Once the tube has been changed without any complications, your child will be transferred to a ward.
But there are cases that children will need to stay in the ICU indefinitely because of critical airways.
Your child with tracheostomy can actually go home with services like intensive care at home where they will be looked after 24/7 by a team of highly skilled, highly experienced intensive care nurses, cut the cost of an ICU bed by 50% and provide your child and families with better quality of life and provide a win-win situation.
Now, patients and families, couldn’t be happier to finally leave in a burdensome stay in intensive care and go back to their lives at home with 24-hour specialized intensive nursing care at home. Our clients, whether they’d be children or adults can actually go back to school, can go back to kindergarten, whatever their normal life activities are because they’ve got the specialists care around the clock, and that doesn’t stop them from going back to their lives and to the things they want to do.
**Tracheostomy in Kids (Part 2) will continue in next week’s episode.
REFERENCES:
-
Tracheostomy (Tracheotomy)
https://www.stanfordchildrens.org/en/service/ear-nose-throat/conditions/tracheostomy
-
Tracheostomy in Infants and Children
-
Tracheostomy Care for Children
https://www.drugs.com/cg/tracheostomy-care-for-children.html
-
Tracheostomy Management
https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/Tracheostomy_Management_Guidelines/
-
Tracheostomy: What It Is and When It Is Needed
-
Tracheostomy management for an infant, child or young person
https://www.starship.org.nz/guidelines/tracheostomy-management-for-an-infant-child-or-young-person/
-
IS IT TRUE THAT SUPPORT WORKERS CAN’T HANDLE SAFELY VENTILATED PATIENTS WITH TRACHEOSTOMIES AT HOME?
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!