What is BiPAP ventilation?
Bilevel positive airway pressure (BIPAP) is a continuous positive airway pressure (CPAP) mode used during Non- Invasive Ventilation(NIV)(positive pressure ventilation). It delivers a preset inspiratory(breathing in) positive airway pressure (IPAP) and expiratory(breathing out) positive airway pressure (EPAP). BIPAP can be described as a continuous positive airway pressure system with a time-cycled or flow-cycled change of the applied CPAP level. CPAP, BIPAP and other non-invasive ventilation modes have been shown to be effective management tools for chronic obstructive pulmonary disease(COPD) and acute respiratory failure.
The main purpose of BIPAP ventilation is to push air and oxygen into the lungs, whilst also keeping the lungs and the alveoli inflated, allowing more oxygen to enter the lungs. The main reason for using BIPAP is if your loved one is unable to breathe effectively and therefore is unable to inhale sufficient oxygen into the lungs. BIPAP is an alternative therapy to Intubation and mechanical ventilation. During BIPAP your loved one would get a few breaks to be put back on an oxygen mask, as BIPAP on the one hand can be extremely effective improving oxygenation, but on the other hand can be very tiring.
BIPAP is either used with a specific BIPAP machine or it can be applied using a mechanical ventilator(Ventilators (Breathing Machines). A BIPAP mask is fitted on to your loved ones face and attached to the ventilator with flexible circuits(tubing).
The main use of BIPAP is in Patients with
- Pneumonia
- COPD
- Acute Severe Asthma
- Cardiac failure
- after Extubation
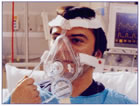 Example of a full face mask
Example of a full face mask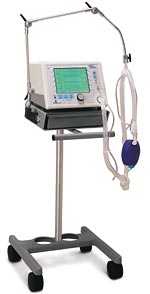 Example of a BIPAP Machine
Example of a BIPAP Machine
These images sourced through Google using ‘bipap’ as keyword
How Long is BiPAP therapy being Used?
BIPAP is often used before Intubation or after Extubation. In both cases, this can range from several hours to several days and sometimes several weeks.
If your loved one is requiring ongoing BIPAP or Non-invasive mask ventilation and wants to leave Intensive Care and/or Hospital, check out www.intensivecareathome.com for more information
Also, have a look here for home BIPAP/CPAP services
Are There Any Complications?
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE ARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- Be more selfish if your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 4 ways on how to be more persuasive if your loved one is critically ill in Intensive Care
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


