Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
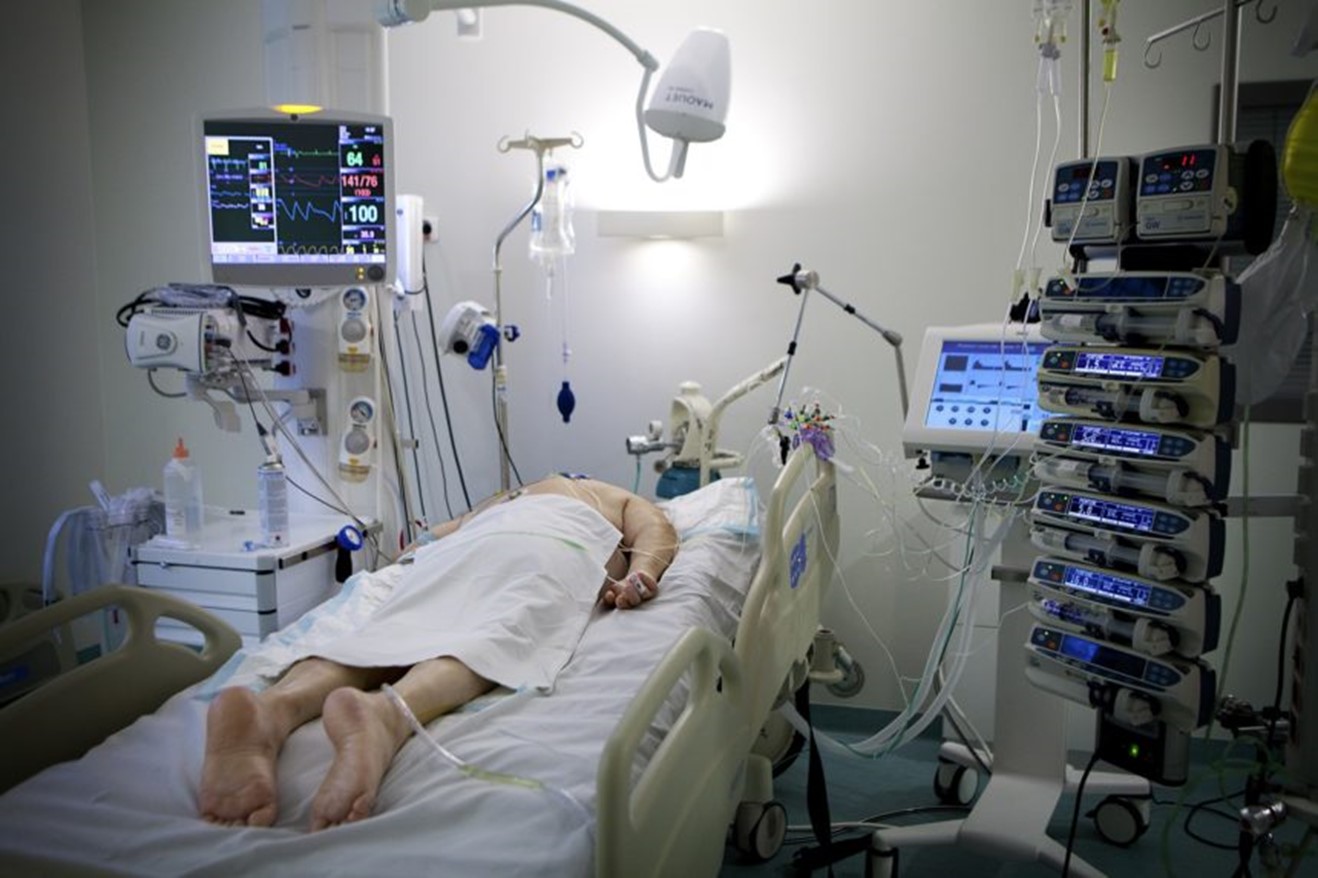
How Can Prone Positioning Help my Critically Ill Loved One with COVID/ARDS in ICU?
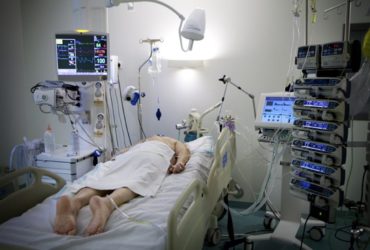
SARS-CoV-2 virus causes pneumonia that was identified through fever, dyspnea, and acute respiratory symptoms and named COVID-19. This disease exacerbates in a number of patients and causes pulmonary edema, multi-organ failure, and acute respiratory distress syndrome (ARDS).
ARDS was first introduced in 1968 with clinical presentations such as acute hypoxemia, non-cardiac pulmonary edema, decrease in pulmonary compliance, and increase in work of breathing. Among the introduced treatment methods for management of ARDS patients, prone position can be used as an adjuvant therapy for improving ventilation in these patients. It should be prescribed along with low tidal volume (6 cc per kg body weight) and infusion of neuromuscular blockers (cisatracurium for 48 hours). These 3 treatment strategies together, lead to improvement in oxygenation and survival of ARDS patients. [3]
What is Proning?
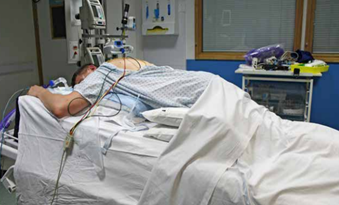
Prone position is the medical term for lying flat on your stomach. Lying flat on your back is referred to as the supine position.
Prone positioning (also known as ‘proning’, ‘prone manoeuvre’, or ‘prone ventilation’) refers to mechanical ventilation with patients positioned in prone position in contrast of standard supine (flat or semi-recumbent) position.
The use of the prone positioning was proposed over 30 years ago as a means to improve arterial oxygenation in patients with acute respiratory distress syndrome (ARDS)?. Since then, extensive physiological research has been conducted to explore the possible mechanisms underlying the observed improvement in gas exchange, which involve changes in the distribution of both ventilation and pulmonary blood flow. Furthermore, it has been shown that, independently of gas exchange, prone positioning may reduce the harm of mechanical ventilation which is known to adversely impact patient survival.
How does proning help?
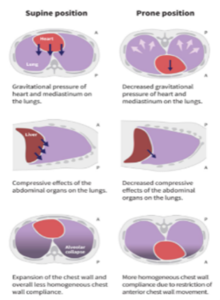
In the supine position, the lungs are compressed by gravity and other forces — including the internal organs. This position can cause hyperinflation of alveoli in the ventral lung while causing alveolar collapse (atelectasis) in the dorsal part of the lung. Gravity complicates things by pushing blood downward toward the poorly oxygenated alveoli in the posterior lung, creating a ventilation/perfusion mismatch. This mismatch is thought to drive rapid deterioration of patients with conditions that compromise breathing. Furthermore, the longer patients are mechanically ventilated, the greater the risk that prolonged immobility will lead to delirium and generalized weakness.
Proning relieves some of the pressure on the heart and lungs that occurs when lying on the back, and it can help clear respiratory secretions. It also plays a significant role in reducing the effects of prolonged immobility and can even reduce the time spent on mechanical ventilation by improving strength and endurance.
How does proning help your loved one with COVID-19/ARDS?
Research has found that when proning is used in patients with severe ARDS and hypoxemia not improved by other means, it has the benefit of:
- better ventilation of the dorsal lung regions threatened by alveolar collapse;
- improvement in ventilation/perfusion matching; and
- potentially an improvement in mortality.
These benefits are the result of a more even distribution of ventilator volumes and pressures throughout the lung, which is thought to reduce the incidence and severity of ventilator-induced lung injury.
Patients who are put in the prone position are carefully monitored. Medical staff will place them in the prone position for a set number of hours before transitioning them back to the supine position for a few hours. The process might be repeated over the course of several days if the person is breathing better and can tolerate the treatment. In some cases, this has helped people avoid being intubated and placed on ventilators in the ICU.
How often and how long is your loved one proned?
Prone positioning is an important non-pharmacologic strategy with lifesaving potential that should be considered for all invasively ventilated patients with moderate to severe ARDS.
The position of patients placed in prone position should be changed every 2 hours and sides should be switched. At least 3 to 5 individuals should participate to correctly put intubated patients in prone position, which is a serious limitation for keeping the patient in this position for a long time.
Overall, it seems that studies on the effectiveness of prone position in ARDS patients clearly point out that correct patient selection, timely initiation and duration of patient’s placement in this position can all affect the effectiveness of this treatment method. Available meta-analyses show that prone position can decrease mortality in ARDS patients when performed in the initial hours of disease manifestation, in patients with severe impaired oxygenation and for a long time [7]. The minimum suggested duration of prone position is 12 hours a day.
What are the side effects of proning?
In addition to the effectiveness of this treatment method, caretaking aspects and the side effects of this position on ARDS patients should also be considered. Patients that undergo ventilation with ventilator in prone position face risks such as:
- accidental removal of the endotracheal tube
- limited access to the venous route
- bending or pulling of the catheters and chest tube
- pressure wound
- bruising around the mouth due to presence of the tracheal tube
- edema around the eyes and facial edema
- gastroesophageal reflux
- hyper-salivation
- skin injuries
- hypotension (low blood pressure)
- arrhythmias (irregular heartbeat/rate)
In prone position, the patient should face the ventilator and in patients with tracheostomy, a roll of fabric or pillow should be placed under the shoulders to prevent airway obstruction, these patients should receive muscle and nerve relaxant medications and high-dose sedation as infusion, eye pads should be used for closing the patients’ eyes to prevent corneal ulcers.
Considering the condition of these patients and presence of pressure on their stomach, the probability of reflux after gavage is very high, so they must be closely monitored regarding aspiration of gastric contents.
Many patients with coronavirus disease (COVID-19) will develop acute respiratory distress syndrome (ARDS). Prone positioning is an important non-pharmacologic strategy that should be considered for all invasively ventilated patients with moderate to severe ARDS (including those with COVID-19). Prone positioning offers several physiologic and clinical benefits, including improving hypoxemia, matching ventilation with perfusion, reducing regional hyperinflation, and improving survival.
Prone positioning is a lifesaving non-pharmacologic strategy that should be part of the toolbox in every ICU that manages patients with ARDS. The use of prone positioning requires an understanding of indications and risks, along with appropriate health system planning through development of protocols and procedures as well as simulation and practice to gain competence and expertise.
Additionally, if proning has not been effective along with conventional therapy, then ECMO can be initiated which is the final step in the algorithm for managing life-threatening lung failure due to COVID in advanced ICUs.
REFERENCES:
- Prone Positioning in COVID-19-Related ARDS: An Overview and Clinician Opinion.
https://www.pulmonologyadvisor.com/home/topics/critical-care/prone-positioning-in-covid-19-related-ards-an-overview-and-clinician-opinion/
- Prone positioning benefits for the COVID-19 patient
https://www.medline.com/coronavirus/prone-positioning-benefits-covid-19-patient/
- Prone position in ARDS patients: why, when, how and for whom
https://link.springer.com/article/10.1007/s00134-020-06306-w
- Prone Position in Management of COVID-19 Patients; a Commentary
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7158870/
- Understanding How Prone Position Is Used in Medical Settings
https://www.healthline.com/health/lung-cancer/prone-position
- Proning During COVID-19
https://www.pennmedicine.org/updates/blogs/penn-physician-blog/2020/may/proning-during-covid19
- Prone positioning for ARDS patients—tips for preparation and use during the COVID-19 pandemic
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7759020/
- Prone positioning in the ICU
https://oxfordmedicine.com/view/10.1093/med/9780199600830.001.0001/med-9780199600830-chapter-99
- Image credit to: Prone Positioning in COVID-19-Related ARDS: An Overview and Clinician Opinion
https://www.pulmonologyadvisor.com/home/topics/critical-care/prone-positioning-in-covid-19-related-ards-an-overview-and-clinician-opinion/
- Image credit to: Guidance For: Prone Positioning in Adult Critical Care
https://static1.squarespace.com/static/5e6613a1dc75b87df82b78e1/t/5e72187c06c2956228316545/1584535679039/FICM-ICS-Prone-Position-Adult-Full.pdf
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!