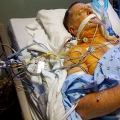
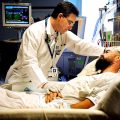
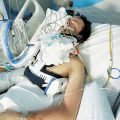
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why Is My Dad Still on Sedation and Why Are They Not Waking Him Up in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Richard, as part of my 1:1 consulting and advocacy service! Richard’s dad is with a breathing tube and on a ventilator in the ICU. Richard is asking what must the ICU team do in order for his dad to come off the ventilator in the ICU.
What Must the ICU Team Do in Order For My Dad to Come Off the Ventilator in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Richard here.”
Richard: Well, they calculated my dad with COPD (chronic obstructive pulmonary disease) like 5 years ago when he was in ICU, but he hasn’t been taking any medicine. He’s had no medicine in the last four years. He’s had all vitamins through the PEG tube. The only medicine he took was ARVs (antiretroviral) because he ended up with some skin thing on his nose and he got off that, that’s when he had some back rash or something, so I don’t know if that’s what created the whole sepsis thing or not, but he doesn’t take any medication for COPD. When he got out of ICU, he had a little oxygen and he hasn’t been on it.
Patrik: Right.
Richard: Like I said, the only thing he has is a feeding tube for the last 4 years, and that’s it, so I’m not sure if he has it because of the scenario he was in, but he doesn’t take anything for it. He doesn’t have asthma. They don’t give him nothing. In the last 4 years, he’s been fine. He breathes on his own, no issue. He just had some skin issue and that’s it.
Patrik: That was the other thing. Why does he have a PEG tube?
Richard: Because the last time he went to the ICU, four years ago at a different location, he ended up getting sick and they had to intubate him. They restarted his heart and they pushed the PEG tube. I hate the PEG tube. I’ve kind of got accustomed to it, but they pushed the PEG tube, this doctor pushed it, to say, “Well, to feed him, that’s what we needed.” Because it was in his nose too long and for them to push the PEG tube, and that’s when the PEG tube showed up.
Patrik: Right, and he’s been having..
Richard: And he’s been doing the PEG tube at night and during the day he’ll eat.
RECOMMENDED:
Patrik: Right. Wow. Okay. Okay, fair enough. Okay, and when did they last talk about the tracheostomy? What did they say last time about the tracheostomy?
Richard: They threw it on me. It was on day 7 and they mentioned about a trach, and they said that normally when they do a trach, that they would have to do it on the 14-day mark, and I think it was last Saturday, and I said, ” Okay, well then I guess we’ll give him time until Tuesday.” And then the doctor said, “Fine.” and then we can go back over the trach, but they didn’t really… I mean, I asked, “What are the pros and cons of it?” Of course, I wasn’t really in detail of understanding all at the same time compared to where I’m at now, because after that I started doing a lot of research, but I haven’t heard anything about it since then.
Recommended links:
Patrik: Right. Okay.
Richard: And his primary hasn’t called me and then now, suddenly she’s calling me, so the last time we spoke, I was a little concerned about the situation, because last time when he met her, they gave him Vancomycin, and this time when this situation happened, they just gave him Erythromycin and I kind of said something to her about, ” My dad, we met in the ICU and I thought, maybe you would’ve gave him Vancomycin and now he’s on a ventilator.” So I was a little upset and that’s all I said and then she just kind of like went off and said, “I need to take care of your dad right now.” And then she hung up on me and that’s the last time I spoke to her, so now she’s calling back probably to try to push whatever.
Patrik: Right. I would argue that with the ventilator settings, as they are, and especially if they’re not lowering sedation, for whatever reason, I would say that a tracheostomy might be on the cards now, just looking at the ventilator settings, but I would really want to find out from her, why are they not lowering sedation? What stops them from doing what they’re doing? What’s..
Richard: They say when they lower the sedation that he starts breathing heavy, but they’ve lowered it several times and they keep saying he breathes fast, so maybe it’s still the infection, the lungs, because they haven’t given him the proper fungal medication versus just some strong antibiotics. Something that’s particular or that’s not resistant to certain type of whatever infection he has, so that was my thing and that was my thing about why I asked you about why did they wait 14 days to do a bronchoscopy to find out exactly what infection he had, to give him the proper medication, because I know that with MRSA (Methicillin Resistant Staphylococcus Aureus) that you can only give certain medications that actually help with that type of infection, so that’s my thing, why did they wait 14 days to give him? Is it normal to wait that long to get a bronchoscopy? Or is it because they did that medication and it worked, their white cell count went lower and they took it off. The chest x-ray looked good and then it spiked up again.
Suggested links:
Patrik: The bronchoscopy is often a very situational treatment option, so what that means is, for example, if someone deteriorates quickly, if you need to increase FiO2 (fraction of inspired oxygen), if you need to increase PEEP (Positive End Expiratory Pressure), suddenly you do an x-ray and the x-ray shows what’s considered a white-out. And then you do often a bronchoscopy, so it’s a very sort of situational approach. If that makes sense.
Richard: So 14 days is actually okay then?
Patrik: I wouldn’t say it’s okay, there are some patients that come into ICU and that have a complete white-out on the chest X-ray, and you ventilate them with 100% of FiO2 and then you do it then. Probably what we need to find out is what led them to that decision to do a bronchoscopy. I think that’s what we need to find out.
Richard: Okay, so my thing is if we try to lower the sedation and breathing goes back, what are the options, what do we do? What haven’t they done? Type of thing.
Patrik: Correct.
Richard: And that’s where we’re right now.
Patrik: Very much so, and again, do you know that, for example, it depends on how much fentanyl he’s been on. Fentanyl, for example, is an opiate that’s addictive, so depending on how much fentanyl he had over the last couple of weeks, when they’re trying to reduce the fentanyl, he could potentially be going through withdrawal.
Richard: And it’s just anxiety or withdrawal, and it’s not really the lung issue?
Suggested links:
Patrik: It could be, and that’s the sort of thing we need to find out. He might have been on minimal doses of fentanyl, but we wouldn’t know.
Richard: I know because I’ve written them all down. I have a little chart.
Patrik: Okay.
Richard: Every time I called them, I pretty much written them down. It was pretty much 100 or 70, 60, 50 each time, so I have a little charts that I keep together.
Patrik: For the last couple of weeks?
Richard: Yeah.
Patrik: Well, I think that’s enough to go through some withdrawal, if they reduce it. I think that would be enough.
Richard: What kind of medication should they be giving him if he goes through a withdrawal?
Patrik: Yeah, if he goes through withdrawal, the Dexmedetomidine might be the right approach, from my experience. The alternative to Dexmedetomidine, if someone is going through withdrawal is Clonidine, but there’s Clonidine in Dexmedetomidine, so again, those are the questions we can ask. What’s your dad’s weight approximately?
Richard: Approximately, I overhear it’s about 135.
Patrik: That’s pounds. Is it?
Richard: Yep.
Patrik: Just give me a second. I’m a metric person. Just give me one second. I just need to get that kilo. Just give me a second. Just typing it into my calculator, so 61 kilo, so that’s a lightweight. That also means that the doses of fentanyl, when you say 50 to 100 mcg per hour, that’s a fair bid for someone with 135 pounds, so a lot of it depends on people’s weight as well. That also puts in perspective, 70 mg of propofol an hour, generally speaking is not a lot. However, given that your dad is 135 pounds, it’s an average dose. When you..
Richard: Yeah, he’s usually at 135 to 140.
Patrik: Right, so when you talk to him on Face Time, is he doing anything for you? Do you think he’s responding?
Richard: No, he’s not, no.
Patrik: Right.
Richard: After that last ICU, he doesn’t really talk or do much, but if you touch him and everything he does… Rub his hair, he does kind of moves and doesn’t really like that too much and stuff like that.
Recommended:
Patrik: Right.
Richard: But yeah, after his last ICU, he doesn’t really talk at all.
Patrik: Right.
Richard: But he will move, if he doesn’t like something he will and kind move like that.
Patrik: Sure.
Richard: But yeah. I touched him and everything, he didn’t do nothing.
Patrik: Right. And have you witnessed the breathing rapidly yourself when they lower sedation? Have you witnessed that yourself?
Richard: No.
Patrik: Right. So this is..
Richard: When I was there, I asked them and then they said that they just did it the day before, and so they couldn’t really do it, and they would ask the doctor, and then when I came in at the next visit from 4 to 8, the doctor just told me all this stuff and then about his heart stuff, and all that and yeah. But no, I have not witnessed it, because I ask her like, “Since I’m here, why can’t we do it? Because maybe if he’s a little fearful, he wakes up, he’s a little scared I could talk to him or rub him and that might help him because last time at the ICU, that’s kind of like what I did.”
Patrik: Yeah, just remind me again, how old is your dad? Did you say 75?
Richard: Yeah, 75.
Patrik: Yeah. Okay, and prior to..
Richard: He had some psych issues back in the day and they had on a lot of psych medicines and I finally got him off of it, and I think the last 5 years, he hasn’t been on hardly any, maybe like 5 mg of some. I have to go look, so many medicines through my head right now, I can’t even remember, but yeah, he hasn’t been really on anything, so I don’t know, maybe that’s gotten kind of clear information or something.
Recommended links:
Patrik: Yeah. You’ve also had the question in your email about ECMO or Extracorporeal membrane oxygenation. ECMO is an option, but it’s often only an option for patients below the age of 65. Now don’t get me wrong, I argue that everything in life is negotiable. However, ECMO is in very high demand now during COVID. It has been in high demand before COVID, it’s in even higher demand at the moment because of COVID, and as I said, the cut-off generally speaking for ECMO is 65, and I would argue that at the moment, it might even be lower because of COVID.
Richard: So what are the options with the issue on getting off the ventilator? What options are there?
Patrik: Yes, so the first thing that needs to happen is lowering sedation. He won’t be able to get off the ventilator without lowering sedation.
Richard: And when they lower it and the breathing goes high?
Patrik: Well, that’s where I think the Dexmedetomidine might come into play. They probably need to try it. Your dad’s brain is intact, never had a stroke. His brain is intact before this all happened.
Richard: Well, he had a stroke in his last ICU.
Patrik: Well, that’s a while ago.
Richard: 5-6 years ago.
Patrik: Did he recover from that?
Richard: He recovered, but like I said, he didn’t talk, he’s pretty much bedbound, he refuses to do any type of physical therapy. In fact my dad couldn’t move. The right side doesn’t move the left side he can move well. He moves his arms and everything. When I play with his feet, because I do that sometimes, his feet move, but no he doesn’t walk. He stays in the bed, but like I said, if he wants to, he moves his whole left arm and everything and when they try to change him and do all that, he would make noises and stuff like that.
Suggested links:
Richard: Yeah, but he did have a stroke they said, when all that happened, but they think that he couldn’t move and then all of a sudden, one day they were trying to move him out of the bed and he kind of push back on them. It’s not that he can’t move. I think he just refuses to, before that happened at the other facility, he tell me he kind of wanted to not do all that stuff and a lot of other things was going on and he was saying things, and so yeah.
Patrik: Right, but normally he is mobile? He does get out of bed?
Richard: No, he does not. No, he does not get out of bed. He doesn’t do physical therapy, he is bedbound.
Patrik: I see.
Richard: But he moves his left side.
Patrik: Yeah, sure.
Richard: He moves his arm, everything and all that. The right side, he does not move.
Patrik: Yeah. Yeah.
Richard: Yeah.
Patrik: And the left side he moves on purpose? That’s purposely movement? Yeah, yeah.
Richard: Yeah. He moves his arm and he’ll scratch his nose all the time or rub the top of his head and yeah.
Patrik: Yeah. Okay.
Richard: And he’s right-handed, so.
Patrik: Yeah. Okay. Well what he needs to do in order to get off that ventilator, he needs to follow commands. He needs to have a good cough and once that’s been achieved, obviously he needs to breathe at least on pressure support/CPAP (Continuous positive airway pressure), and again, this is something we need to ask the doctor, how they want to move him towards that, because the fentanyl and the propofol won’t help him achieve that.
Richard: So is that just a trach that would help him achieve that?
Patrik: At the moment? I would say yes.
Richard: Or maybe a psych medicine.
Patrik: Maybe, yes. The other thing on that note is, so FiO2 (fraction of inspired oxygen) is at 60, PEEP (Positive End Expiratory Pressure) is at 14. They might say it’s too risky to do a trach at the moment. They might say that.
Richard: And you know what? The FiO2 was higher yesterday too. It was 80 something, so it’s come down.
Patrik: I heard that. Yeah. I heard that from him, but the PEEP being at 14 is very high, which means I would argue the PEEP needs to be less than 10 for them to do a tracheostomy. They might deem that as too risky. Have you heard of PEEP?
Richard: Yeah. Yeah. I’ve seen it on there. Yeah.
Patrik: Right. It’s basically the pressure that maintains the lungs open, that’s the PEEP simplified and yeah, PEEP above 10 is not very conducive to a trach at the moment.
Richard: Is there a medicine you can use to lower the PEEP?
Patrik: Not really. The PEEP is probably a result of pneumonia/ARDS or Acute respiratory distress syndrome. We don’t know which one it is. Again, it probably comes down to what he has been diagnosed with, if he has been diagnosed with ARDS, I would argue the steroids are not everything he needs. That’s where I keep coming back to maybe nitric oxide, maybe the Flolan, and maybe the Sildenafil/Viagra. Do you know whether he’s got pulmonary hypertension? Have you heard of that?
Richard: Yeah, I’ve heard of that, but he has just blood pressure medicine and yeah, he probably has some of that too. You said nitric oxide, the Flolan and what was the other one?
Patrik: So Viagra is a common drug being used for pulmonary hypertension, if he has that, and some patients that have ARDS automatically have pulmonary hypertension, but again, that’s where it comes back to what has he exactly been diagnosed with?
RECOMMENDED:
Richard: And then should they be using the steroids daily? Like they said, they haven’t done it today.
Patrik: Right. Steroids is something that should be used temporarily, and once they decided to stop it, it’s a gradual reduction. It’s not that you’re giving steroids and then you stop them. You wean it off gradually, so if he’s had 40 of methyl prednisolone, for example, they would wean that down. Next day 30, next day 20, next day 10, maybe then down to 5 and then stop it. That’s usually how they wean.
Richard: I think it was Solu-Medrol.
Patrik: Or Solu-Medrol, whatever it is. It’s a gradual approach. It’s not as simple as just stopping it.
Richard: Okay.
Patrik: So let’s talk to the doctor as the next step, I would think, and see what he recommends.
Richard: Yes and the fact that they barely started giving him yeast antibiotics when it’s the yeast thing.
Patrik: Oh, absolutely. If they found yeast, it makes sense to give fluconazole. It makes sense.
Richard: And they just started that the other day. I mean, you never know, a couple days it might clear up and the lungs might be able to breathe.
Patrik: That’s right. It might clear up, so, again, they have to give this for a few days similar to a course of antibiotics and then reassess what the next steps are.
Richard: Okay. I’ll call her and then she’ll let me know.
Patrik: Please, get back to me.
Richard: And we’ll set up time.
Patrik: Yeah. Okay. Thank you.
Richard: Thank you.
Patrik: Thank you. Bye.
Richard: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!